


24 November 2025

Welcome back to our Winder Memory Care and Assisted Living blog! We’ve got a heartfelt Holiday tip for all of you wondering what to do for that special loved one residing either at home with you or with us here at Gateway Gardens. The answer is simple: plan to spend quality time doing the things you’ve always enjoyed together. Sounds simple, right?
The key word is plan. Even the best intentions can slip away during the busy Holiday season unless we intentionally schedule time. You know how quickly obligations pile up—shopping lists, events, errands, and responsibilities. And while our loving, professional staff here at Gateway Gardens Assisted Living and Memory Care in Winder, GA provides daily compassionate support, we can never replace you.
So, please consider this a warm and sincere invitation to spend a little extra special time with your loved ones this Holiday season. And by extension, you’ll be spending time with us too—we’re honored to be part of their lives every day, and we’d love to catch up with you.
From all of us here, Happy Thanksgiving!
If you have questions about Independent Living, Assisted Living, or Memory Care services in Winder, GA, don’t hesitate to call anytime.
17 November 2025

Welcome back to our Winder-area assisted living and memory care blog. We are professional assisted living care providers as well as professional memory care providers here for those living in and around Winder. A caveat right up front here: your first and most trusted source for consultation regarding you or your loved one’s perceived memory care concerns is your trusted team of medical professionals.
We take great pride in sharing our knowledge, professional education, and professional experience to help you along your journey. We hope that the efforts in publishing today’s blog post answer questions and give you comfort—but most importantly, we hope articles like this help you prepare for and benefit most from future discussions with your medical doctors.
Dementia is a progressive brain disorder that affects memory, thinking and behavior. Understanding the stages of dementia is crucial for providing effective care and support to individuals diagnosed with the condition. Each stage presents unique challenges, and the care needs of individuals evolve as the condition progresses. Early recognition and planning can help improve quality of life for both the person with dementia and their caregivers. This blog outlines the seven stages of dementia, including what to expect at each stage and the importance of tailored care.
Dementia is an umbrella term for various brain disorders that impair cognitive functions—including memory, reasoning, and the ability to perform daily tasks. Alzheimer’s disease and vascular dementia are two of the most common types, but there are many others, including Lewy body dementia.
Dementia progresses through several stages, each characterized by worsening symptoms and increasing dependence on caregivers. These stages are often categorized using the Global Deterioration Scale (GDS), also known as the Reisberg Scale, which helps track cognitive decline.
At this stage, there’s no impairment or noticeable symptoms. Individuals are fully functional and show no signs of memory loss or confusion. Even though dementia may be present in the brain, it has not yet impacted daily activities.
This is the ideal time for proactive planning, as seniors can still participate in discussions about future care, including exploring Life Plan Communities like Gateway Gardens Assisted Living and Memory Care in Winder. Engaging in these discussions ensures that both the individual and their family are prepared for the challenges ahead.
In Stage 2, individuals may experience slight forgetfulness or very mild cognitive symptoms, such as occasionally misplacing objects or forgetting names. These signs are often mistaken for normal aging but can be early indicators of dementia.
Despite these symptoms, individuals can still handle daily tasks and maintain their social and work life. However, it is important to begin monitoring changes in memory and cognitive function, as early detection allows for more effective management.
Stage 3 marks the point where cognitive decline becomes more apparent, and diagnosis often occurs. Common symptoms include:
At this stage, dementia-related anxiety may start to affect both the individual and their family. It is crucial to establish a care plan to slow the progression of dementia and provide support for daily tasks. The services offered here at Gateway Gardens Assisted Living and Memory Care deliver positive, life-changing effects for both the affected and their families.
Stage 4 involves moderate cognitive decline, where the effects of dementia extend beyond memory loss. Individuals may have difficulty with language, organization and problem-solving. They may struggle with daily activities such as managing finances, cooking or making decisions. Other common symptoms include:
Families often notice significant behavioral changes during this stage. While seniors can still perform some daily tasks, it may be time to consider professional Memory Care to ensure their safety and well-being.
In Stage 5, individuals begin to require more assistance with daily tasks. At this stage, they experience moderately severe dementia. There is a noticeable decline in cognitive abilities, including difficulty recognizing close family members or friends. Some key changes include:
Due to this decline, expert Memory Care becomes essential. Our highly trained staff provides compassionate, round-the-clock care tailored to each resident’s unique needs.
Stage 6 brings significant cognitive and physical challenges. The individual may lose the ability to communicate effectively, struggle to use the bathroom, and require assistance with eating. Additional symptoms include:
Caregivers at this stage must provide uninterrupted hands-on support, allowing individuals to live with compassion and dignity as they navigate late-stage dementia.
The final stage of dementia results in a loss of the ability to respond to their environment. As the brain’s connection to the body deteriorates, individuals may lose mobility and require assistance with all daily activities. At this stage, individuals may:
The goal at this stage is to ensure comfort and quality of life. Families take comfort knowing their loved ones are receiving compassionate, skilled care tailored to their needs.
Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we lovingly deliver personalized, compassionate care through every stage of dementia. We understand the unique challenges dementia presents and are committed to helping residents maintain dignity and comfort. Our approach focuses on truly knowing each resident, providing tailored support, and creating meaningful moments with family involvement.
Contact us today to learn how we can help you and your loved ones navigate the journey through dementia with care, compassion, and support.
10 November 2025

In last week’s assisted living and memory care blog post, we mentioned that we’d return once more to the subject of Thanksgiving safety for all of you at-home assisted living or memory care support providers. We realize that safety isn’t the most festive topic to discuss this time of year—but it’s certainly one of the most important. So, we’ll keep this brief but meaningful.
Fires aren’t the only unexpected hazards that can arise on Thanksgiving Day. People with food allergies, for instance, should take extra care. If you didn’t prepare the meal yourself, be sure to find out exactly what’s in it. And while it may seem simple, remember to give your full attention to tasks like chopping vegetables and carving the turkey—many holiday injuries happen when we rush or get distracted.
Thanksgiving also calls for special caution in the kitchen to prevent food poisoning. The American College of Emergency Physicians (ACEP) offers these helpful reminders:
The Centers for Disease Control and Prevention (CDC) also recommends that oven temperatures be set no lower than 325°F. And even though it’s tempting to relax on the couch after that last slice of pumpkin pie, remember to refrigerate leftovers within two hours to keep everyone safe.
Choking incidents are surprisingly common on Thanksgiving, especially when people are laughing, talking, or taking overly large bites of food. The ACEP advises everyone to chew slowly and cut food into small pieces. And make sure at least one person at your gathering knows how to perform the Heimlich maneuver.
If food does get stuck, try to stay calm. Take a sip of water if you can, or make noise to alert others if you’re unable to breathe. Someone should immediately call 911, while another person—preferably trained in first aid—attempts to help.
Finally, a friendly reminder from all of us here at Gateway Gardens Assisted Living and Memory Care in Winder: if alcoholic beverages are part of your celebration, practice moderation and keep a watchful eye on loved ones. Your care and attentiveness could truly save lives this Thanksgiving.
3 November 2025

Welcome back to our assisted living and memory care blog! We’re always grateful for your feedback—especially your appreciation for our safety-focused posts. Many of you have shared how helpful these insights are for home-based assisted living and memory care providers.
We know that some of you care daily for loved ones who are still—perhaps just barely—able to live independently. Yet, you may be noticing signs that raise concerns about how much longer that independence can safely continue. That’s an age-old family dilemma, one that calls for careful reflection. While we’re here to educate and support through this Winder-area assisted living and memory care blog, the ultimate decision depends on your family’s unique circumstances and resources.
Now, back to safety. Did you know that Thanksgiving Day ranks No. 1 for kitchen fires in the United States? If your independent-living mom insists on helping with the upcoming Thanksgiving dinner, here are some practical kitchen safety tips—useful not just for seniors, but for everyone in the family.
Fires aren’t the only unexpected hazards we might face during Thanksgiving. We’ll be back next week with more safety reminders to help you prepare for a worry-free holiday.
Finally, from all your friends here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we encourage you to get outside and enjoy the crisp, moderate fall weather—before Mother Nature reminds us that winter is just around the corner.
27 October 2025

Welcome back to our Winder-area assisted living and memory care blog!
We were recently asked to revisit a previous post related to memory care and the Halloween holiday. While we’re not sure if this is the exact one requested, upon review, it’s filled with helpful and thoughtful considerations for those of you caring for a memory care loved one.
At Gateway Gardens Assisted Living & Memory Care, we have a longstanding tradition of celebrating Halloween with both our assisted living and memory care residents. However, we do celebrate a bit differently within our two unique care communities. The scary and ghoulish themes that make Halloween fun for many can actually have a detrimental effect on memory care residents. So, for those of you caring for a loved one at home, we’d like to share a few important things to keep in mind as the holiday approaches.
Halloween is one of the most celebrated days on the American calendar—a day rich in history, excitement, and fun for children who love to dress up in costumes and fill their bags with candy.
However, the scary costumes, eerie decorations, and sudden sounds that define the season can be quite frightening for individuals living with Alzheimer’s or other forms of dementia. It’s important to create a version of Halloween that allows your loved one to feel safe, included, and loved.
Below are a few tips to help make Halloween both happy and safe for everyone:
Maintain Minimal Decorations
Halloween wouldn’t be complete without a few decorations—but too many, or the wrong kind, can lead to confusion or anxiety for those with Alzheimer’s. Keeping decorations simple and familiar helps your loved one enjoy the holiday without feeling overwhelmed.
Here are a few quick guidelines:
A few festive but gentle touches—like pumpkins, fall leaves, or friendly ghosts—can still bring a seasonal feeling without distress.
Avoid Crowded or Public Celebrations
While children may love parades or neighborhood Halloween events, these busy, noisy, and costume-filled environments can be confusing or even frightening for someone with Alzheimer’s.
Instead, opt for smaller, quieter celebrations at home or within a familiar environment. This can help your loved one feel calm, safe, and included.
Keep the Candy in a Safe Place
Candy is a big part of Halloween fun—but sugary treats can pose health risks and temptations for seniors with Alzheimer’s. It’s best to monitor access to sweets or store candy safely out of reach.
Offer a few treats in moderation or provide healthier alternatives, such as fruit or sugar-free options, if appropriate.
Prepare Your Loved One in Advance
Before Halloween night, gently explain that there may be costumes, noises, or doorbell rings throughout the evening. While your loved one may not retain all the details, a calm explanation can reduce anxiety.
If trick-or-treaters are visiting, consider sitting together in a quiet area or turning off the porch light early if it becomes overwhelming. Distraction through conversation, music, or a favorite show can also help keep them relaxed.
Halloween can still be a fun, heartwarming time for everyone—even those living with memory challenges. With a few thoughtful adjustments, you can help your loved one feel secure, comfortable, and part of the celebration.
Just as we take safety measures to protect children during Halloween, it’s equally important to extend the same care and consideration to our elderly loved ones.
From all of us here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, we wish you and your family a joyful and safe Halloween celebration!
20 October 2025

Warm greetings once again from your Winder-area assisted living and memory care community here at Gateway Gardens!
Following last week’s post celebrating Mental Health Month, we’d also like to take a moment to recognize another special October observance — Pastor Appreciation Month.
This is a wonderful opportunity to express gratitude to the spiritual leaders who guide, inspire, and support us through life’s joys and challenges. Whether it’s your head pastor, assistant pastor, or other faith leaders, take a moment to reach out and let them know how much their care and dedication mean to you and your family. A simple note, call, or heartfelt “thank you” can go a long way in showing your appreciation.
As always, our warmest wishes to you and your loved ones — from all of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA!
13 October 2025

Welcome back to our Gateway Gardens Assisted Living and Memory Care blog—and Happy Mental Health Month!
Each October, people across the world come together to raise awareness and take action for mental health. Since 1992, Mental Health Month has been a time to recognize that mental well-being is just as important as physical health—and something that everyone should care about.
The movement began with the World Federation for Mental Health, an organization with more than 70 years of advocacy in over 90 countries. Their mission continues today through global events, educational campaigns, and meaningful conversations that help us better understand mental health, seek help when needed, and support others with compassion.
You don’t need to be a mental health expert to make a difference. Here are five simple ways to get involved during World Mental Health Month 2025:
1. Start a Conversation
One of the most powerful ways to fight stigma is to talk openly about mental health. Check in with friends, family, or neighbors. Ask how they’re doing—and truly listen. If you feel comfortable, share your own experiences. Your openness might help someone feel less alone.
2. Share Awareness on Social Media
Social media connects us all. Share posts, infographics, or personal stories around this year’s theme: “Mental Health is a Universal Human Right.” Use hashtags like #WorldMentalHealthDay and #MentalHealthIsAHumanRight to join the global conversation. The World Health Organization (WHO) and other mental health groups offer free shareable resources to help spread the word.
3. Organize or Attend a Community Event
Look for mental health activities happening right here at our Gateway Gardens Assisted Living and Memory Care community. If nothing fits your schedule, consider hosting something small—like a wellness walk, yoga session, or even a virtual coffee chat to talk about mental well-being.
4. Prioritize Your Own Mental Health
Leading by example is a wonderful way to inspire others. Take time this month to nurture your own well-being—practice mindfulness, get outdoors, enjoy your favorite hobby, or spend time with loved ones. When you care for yourself, you show others that mental health matters.
5. Support a Mental Health Organization
Consider donating to or volunteering with organizations that provide mental health services. Groups like the National Alliance on Mental Illness (NAMI), Mind, and the World Federation for Mental Health depend on community support to continue their vital work.
At Gateway Gardens Assisted Living & Memory Care in Winder, GA, we believe that socialization and connection play a vital role in preventing isolation and loneliness—especially among seniors. We love seeing our residents and their families engage, participate, and build lasting friendships within our community.
If you or your loved one is looking for a compassionate, engaging environment where wellness and connection are priorities, we’d love to meet you.
29 September 2025

Welcome back to our blog page for our Gateway Gardens Assisted Living and Gateway Gardens Memory Care community! One of the most common questions we receive this time of year is:
“What ideas do you have to make this Halloween holiday special for my memory care loved one?”
Well, we thought we’d share another special edition blog post on the subject in hopes that it provides some ideas you can put into action.
Halloween’s main purpose is to create joy and fun while reveling in a bit of spookiness. However, for those who suffer from dementia or Alzheimer’s, Halloween can bring a different set of experiences — sometimes including triggers, anxiety, or agitation.
It’s important to be aware of potential challenges the holiday may pose. For example, scary decorations, flashing lights, or spooky costumes can cause confusion and distress. The good news is that with a little planning, you can create a festive, safe, and enjoyable Halloween experience for your loved one.
Here are a few dementia-friendly Halloween activities to try this year:
Painting has been shown to have therapeutic effects for individuals with Alzheimer’s or dementia. It helps engage attention, encourage creativity, and promote social interaction.
Make it festive by painting pumpkins instead of carving them! This is a fun, inexpensive activity that can be done with family members of all ages. You can find small pumpkins at your local grocery store or pumpkin patch — just grab some paints, brushes, and let the creativity flow. It’s a wonderful way to start a new, dementia-safe Halloween tradition.
Charades are a lighthearted and social way to celebrate Halloween together. They encourage laughter, movement, and participation — all while being gentle and non-threatening for your loved one.
Keep it simple with Halloween-themed prompts such as “witch,” “black cat,” or “pumpkin.” This is a great way to get everyone into the spirit while keeping things fun and interactive.
Slime isn’t just for kids! It’s a fun, tactile activity that provides sensory stimulation — something that can be especially beneficial for seniors with Alzheimer’s or dementia.
Making slime is easy, safe, and engaging. You can even add festive touches like orange or purple coloring, or small Halloween-themed trinkets. It’s a hands-on activity that can bring smiles and keep your loved one engaged for hours.
We hope you’re enjoying this beautiful Fall season and looking forward to one of the most fun holidays of the year.
Of course, you’re warmly invited to join us for our Halloween celebration here at both our Gateway Gardens Assisted Living and Memory Care communities. But if you’re celebrating at home, we hope these ideas help make your loved one’s Halloween both joyful and stress-free.
Happy Halloween from all of us at Gateway Gardens!
22 September 2025

As you know, we manage our assisted living and memory care blog as a public service and with the intent to positively change the lives of those in and around our community. It is a simple fact of human life that we don’t enter this world living independently, and we’re not meant to leave it that way either.
We base that claim on the recurring testimonials of our dear assisted living and memory care residents alike: “Where would I be without the support, love, and care provided by all of you who surround me?” We hear variations of this sentiment often, and it stands as one of the greatest rewards of choosing this profession.
Independence and freedom are values we all cherish. Yet, whether prompted by a major life change or simply the desire for a new environment, many of us feel curiosity about the benefits of community living. Here are five ways that community living can enrich life for you or a loved one:
Strong social connections are one of our greatest strengths as humans. They allow us to live more joyfully and accomplish more than we could alone. The opposite is also true—social isolation can harm mental health and even worsen conditions such as Alzheimer’s and dementia. Studies show that maintaining close connections with family and friends can improve mental resilience and help ward off illness.
Staying physically active is important at every age. But as energy levels naturally decline, it can be harder to find motivation. Community living changes this. Having friends to walk with, exercise alongside, or simply chat with during activities makes movement more enjoyable and more consistent—helping maintain strength, mobility, and self-esteem.
When people dine with friends or loved ones, they tend to eat more regularly and more nutritiously. This is especially critical for seniors, as hunger and thirst cues can diminish over time. Shared mealtimes are not only uplifting social events but also opportunities to keep nutrition levels strong and health on track.
At home, even small accidents can become serious if help is not immediately available. In a caring assisted living community like Gateway Gardens, residents enjoy peace of mind knowing they are surrounded by friends, staff, and healthcare professionals who understand their needs and are ready to step in when necessary. This strong safety net provides both reassurance and real protection.
Beyond the health and safety benefits, community living offers something just as important—it’s fun! From watching shows together to going for walks or joining in community activities, opportunities for friendship and laughter are everywhere. These bonds often become some of the most rewarding aspects of community life.
You can see these life-enhancing benefits in action right here at Gateway Gardens Assisted Living and Memory Care in Winder, GA. Better said… we WANT you to come experience our bright, dynamic, and rewarding community firsthand. It’s not just a place to live—it’s a place that will change your life.
15 September 2025

Welcome back! Our blog is designed to serve our dear residents and their families residing within our Gateway Gardens Assisted Living and Gateway Gardens Memory Care communities. Of course, we also strive to support the broader local public as a community service.
Most of you know that we manage this assisted living and memory care blog on behalf of our cherished residents, their families, and all of you home care heroes caring for your loved ones. Today, we’ll discuss a concern that many of you have questions about but may be uncomfortable addressing directly: dementia assessment.
Are you (or a loved one) forgetting where you put your car keys? Struggling to remember the name of an old friend at the supermarket? Is a memory lapse a sign of dementia—or just a normal part of aging? The truth is, it is normal to forget things occasionally as we age. But serious memory problems that interfere with everyday tasks—like driving, using the phone, or finding your way home—may be cause for concern.
Some older adults have a condition called mild cognitive impairment (MCI). This means they have more memory or other thinking problems than other people their age. People with MCI can usually take care of themselves and continue their normal activities. MCI may be an early sign of Alzheimer’s disease, but not everyone with MCI will develop Alzheimer’s.
Signs of MCI include:
Dementia is not a normal part of aging. It involves a loss of cognitive functioning—thinking, remembering, learning, reasoning—and behavioral abilities to the extent that it interferes with a person’s quality of life and daily activities.
In addition to memory loss, dementia may also include problems with language, visual perception, attention, or personality changes. While there are different forms of dementia, Alzheimer’s disease is the most common type in people over age 65.
Normal Aging
Alzheimer’s Disease
The good news is that support is available. Medicare covers services for individuals living with dementia and their caregivers. These services can include assessments performed at home, in person, or via TeleHealth.
You’ll be paired with a trained personal dementia coach and a nurse practitioner who will assess your situation and create a customized care plan tailored to your needs. Your dementia coach will guide you through a comprehensive assessment, identify areas of concern or stress, and connect you with resources and education. Based on these findings, a nurse practitioner will review and finalize your personalized care plan.
If you or your loved one is worried about cognitive decline, now is the time to reach out for help. Whether you know us already or are new to us, we can help. Contact us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
8 September 2025

With the crisp fall air upon us, it’s the perfect time to get outside and enjoy seasonal activities with friends and family. For some of our cherished residents in assisted living or memory care, cooler weather may feel like an excuse to stay inside, curl up with a blanket, and enjoy a favorite book or movie. While relaxing indoors is enjoyable, too much sedentary time during the cooler months can contribute to both physical and cognitive decline.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we provide an active and engaging alternative. Our community offers a variety of indoor and outdoor amenities designed to keep residents moving, social, and thriving—not just passing time. These amenities are more than conveniences; they are purposeful tools to enhance quality of life. And what better time to enjoy them than fall—complete with football, food, tailgating, and festive gatherings?
Remaining physically and socially active during the cooler months is vital for seniors’ overall health. Colder weather often brings unique challenges, from brittle bones to fewer opportunities to enjoy the outdoors. That’s why our team at Gateway Gardens focuses on providing safe, fun, and meaningful ways for residents to stay engaged both inside and outside.
Grilling Outside
Nothing brings people together like food. From hamburgers to hotdogs, grilling outdoors is a great way to combine fellowship, laughter, and delicious meals. Whether it’s during a big football weekend or a casual afternoon, our residents and families can share in the joy of cooking and dining together.
Outdoor Games
From cornhole and bocce ball to horseshoes, there’s no shortage of fun when it comes to outdoor games. These simple yet engaging activities help foster social connections while encouraging gentle movement. Even classic card games can be taken outdoors when the weather allows, giving everyone a chance to enjoy fresh air and sunshine.
Take a Walk
Movement is medicine at any age, and walking is one of the simplest yet most effective ways to support health. For seniors, regular walks help improve circulation, strengthen bones, and boost mood. Our community provides safe, well-designed spaces for residents to stroll, explore, and connect with nature—all while bundled up for the season.
When the weather turns chilly, we know it’s not always safe or comfortable for everyone to spend time outdoors. That’s why our indoor amenities are available year-round, offering opportunities to stay active, social, and engaged without stepping outside. Purpose-driven amenities are essential to keeping residents not only occupied but thriving in mind, body, and spirit.
We invite you to see for yourself how Gateway Gardens Assisted Living and Memory Care in Winder, GA creates a welcoming, enriching environment where seniors and families come together to celebrate life—even in the cooler seasons.
1 September 2025

Welcome back to our Winder Assisted Living and Memory Care blog! Last week, we shared five signs that may indicate you’re experiencing caregiver burnout. It’s only fitting that we now follow up with some practical tips for managing it.
Let’s face it—caregiving is exhausting. For some, it’s physical fatigue. For others, it’s emotional or mental exhaustion—or even all three. Wherever you find yourself on that spectrum, consider the following strategies to protect your well-being and recharge your spirit.
Take intentional breaks with healthy distractions. Make time to see friends, attend that potluck dinner, or simply enjoy an evening walk with a buddy. Social connections can help lighten your emotional load and restore your energy.
You don’t have to do it all on your own. While you may prefer to personally handle important tasks like medications or personal care, there are plenty of ways others can step in—whether it’s running errands, picking up groceries, or handling small chores. Let people help, and don’t hesitate to ask family members for support.
Sometimes the best comfort comes from people who truly understand what you’re going through. Support groups provide a safe space to share your experiences, listen to others, and gain valuable advice from those who’ve walked in your shoes. And remember—our team here at Gateway Gardens Assisted Living and Memory Care is always part of your support network.
Superheroes may exist in movies, but in real life, you’re just one person. Be kind to yourself by setting realistic, achievable goals. Don’t overschedule your days so tightly that you leave no time for joy, rest, or personal fulfillment.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we know how deeply you care—and we see it every time you visit your loved ones. We honor your devotion and are here to support you. When the time comes to explore transitioning your loved one into a compassionate, uplifting assisted living or memory care community, know that we’re ready to walk that journey with you.
25 August 2025

Like you, all of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA celebrate our mothers, fathers, and grandparents who were always there for us. Life often calls upon us to accept a role reversal—where we become the caregivers for the very people who once cared for us.
The truth is, caregiver burnout can happen to anyone who spends significant time caring for a loved one. It affects people physically, emotionally, and mentally. Burnout can creep in slowly or arrive suddenly, and because caregivers often give freely of themselves—sometimes at the expense of their own well-being—they are especially at risk.
So, are you approaching caregiver burnout? Let’s reflect together.
1. Withdrawal
Many caregivers find themselves slowly withdrawing from friends, hobbies, and social activities without even realizing it. Maybe you’ve been turning down dinner with friends, skipping outings with coworkers, or passing on family gatherings you used to enjoy. This gradual pull away from your own life is a major sign of burnout.
2. Changes in Weight or Appetite
Caregivers often skip meals, eat on the go, or turn to unhealthy options because of time constraints. Some lose weight from not eating enough, while others gain weight from stress-related eating. Both are signs of imbalance linked to burnout.
3. Physical Exhaustion
Caring for someone you love is demanding, and when burnout sets in, you may feel constantly drained. Frequent yawning, forgetfulness, aches, and even nodding off during the day can all signal caregiving-related exhaustion.
4. Frequent Sickness
Lack of sleep, stress, and physical fatigue can weaken your immune system. If you find yourself getting sick more often, or struggling to bounce back from minor illnesses, caregiver stress may be taking its toll on your health.
5. Depression
Caregiver burnout and depression can overlap. Caregivers often wrestle with guilt, even when they are doing everything right. If you’re feeling anxious, losing interest in activities you once enjoyed, experiencing mood swings, or struggling with sleep and appetite changes, it may be time to speak with your doctor.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we see and honor the love you give your family. Every visit, every hug, and every moment you share with our cherished residents reminds us of your selfless devotion.
But when caregiving becomes overwhelming, remember—you don’t have to do it alone. Sometimes the best care for your loved one is shared care, where a team of professionals can step in to support both them and you.
Come visit us. It would be our honor to become part of your caregiving team.
18 August 2025

Disease and aging can be frightening. But when we embrace them instead of fearing them, each new day becomes a celebration rather than a burden. At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we walk alongside our dear residents living with Parkinson’s—not by shielding them from the realities of the disease, but by facing it together. We help them, and they help us, celebrate each sunrise as the gift it truly is.
Parkinson’s disease is often misunderstood as simply a “tremor disease” or a condition that only slows movement. In reality, it can present in many different ways. Knowing the range of symptoms helps families better understand the care their loved one needs, both now and as the disease progresses.
Tremors – Often beginning in the hands and arms, tremors may appear as spasms, jerks, or tics. They usually occur when the body is at rest and may lessen with movement.
Trouble moving or walking – Slowness of movement (bradykinesia) affects the arms, legs, and body. Many patients lose the natural arm swing when walking. Rigidity, or stiffness in the limbs, causes pain and contributes to stooping or hunching over.
Sleep difficulties – Falling asleep, staying asleep, and achieving restful sleep are common struggles. REM Sleep Behavior Disorder may cause kicking, punching, or shouting during sleep.
Pain – Up to 85% of patients experience some form of pain. This may include:
Constipation and gastrointestinal issues – Slow digestion may lead to constipation, bloating, gas, heartburn, chest pain, or shortness of breath.
Other symptoms – Reduced facial expression, loss of smell, softer voice, handwriting changes, dizziness, fainting, and apathy.
Parkinson’s affects every individual differently, and often requires a care team that may include primary care physicians, neurologists, pain specialists, orthopedic surgeons, and therapists. At Gateway Gardens, we consider ourselves an extension of that care team—providing daily support, encouragement, and skilled assistance.
Early treatment is critical to address dropping dopamine levels caused by nerve cell damage. While medications can help manage dopamine levels, lifestyle and therapy interventions also play a key role.
While the exact cause of Parkinson’s remains unclear, certain factors increase risk:
If you’ve read this far, you are already taking an important step—seeking knowledge, investing in care, and making the most of life despite the challenges Parkinson’s brings.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we’re here to support you through every stage of the journey. Whether you have questions about assisted living or memory care, or simply need encouragement, know that you are not alone. We live this every day—with love, skill, and hope.
4 August 2025

As the August sun blazes and temperatures soar, all of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA want to remind you to pay special attention to the health and well-being of our senior loved ones. Dehydration can lead to a range of serious health concerns for older adults. Ensuring they get enough fluids, however, can be trickier than it sounds.
Yes! If you’re caring for a senior—whether at home or in a professional setting—hydration should be a top priority. Consider these eye-opening facts:
Clearly, maintaining healthy fluid intake isn’t just about comfort—it’s about survival.
Several factors make older adults more vulnerable:
By the time your loved one feels thirsty, they may already be experiencing dehydration. Proper hydration helps reduce UTIs, improve mental clarity, boost energy, and stabilize blood pressure—benefits that are crucial for overall well-being.
While “structured drinking” might sound rigid, our experience at Gateway Gardens show that creating a routine makes hydration effortless and effective—especially in memory care settings. And remember: hydration isn’t just about plain water. Herbal teas, infused waters, fruit juices, broths, and water-rich foods like melons and cucumbers can all count toward daily fluid intake.
| Time | Hydration Goal |
|---|---|
| 7:30 AM | 1 glass of water upon waking (room temperature or warm) |
| 9:00 AM | Herbal tea or infused water with breakfast |
| 11:00 AM | Small glass of water or diluted juice |
| 12:30 PM | Water or broth-based soup with lunch |
| 2:30 PM | Hydrating snack (watermelon, cucumber slices, orange) |
| 4:00 PM | Small glass of water or herbal tea |
| 6:00 PM | Water with dinner |
| 8:00 PM | Final small glass of water or warm caffeine-free tea |
Caregiver Tip: Flavor variety helps. Offering lemon water in the morning, berry-infused water at midday, and herbal tea in the evening makes the routine more enjoyable.
All the best to you from your professional caregiving friends here at Winder Assisted Living and Winder Memory Care. If you’d like more tips on senior health and wellness—or to learn how we ensure hydration for our residents—contact us today.
28 July 2025

Some of the happiest and most active residents in our assisted living community here at Gateway Gardens are those who planned ahead—well before any calendar date dictated the change. These residents thoughtfully considered their options, weighing the pros and cons of moving to assisted living before their independence waned.
What they discovered? A new level of comfort, community, and quality of life that made the transition not only easier—but something to look forward to.
There’s something unmistakable about those who prepare for their golden years versus those who don’t. Understanding the five emotional stages of retirement can help you anticipate the journey ahead and embrace the many opportunities this new chapter can bring.
Nearly every senior goes through these stages, and knowing what to expect can make the transition smoother. More importantly, being part of a senior living community can provide support, structure, and joy during each step of the way.
This is the stage of anticipation. You're still working, but your thoughts are increasingly turning toward the future—your savings, lifestyle goals, hobbies, travel plans, and even where you might want to live.
This stage is exciting but can feel overwhelming. Good planning is key—financially, emotionally, and socially. It helps build the roadmap to a secure and satisfying retirement.
Once retirement begins, many experience a “honeymoon phase.” There’s newfound freedom, time to travel, relax, reconnect with hobbies—or try new ones entirely.
You may feel invigorated and energized during this period. Some retirees use this time to join clubs, pursue part-time passions, or simply savor the break from decades of schedules and deadlines.
After the initial excitement, a slower pace of life may lead to feelings of boredom, loneliness, or even a lack of purpose. This is a common and completely natural stage.
But the key difference between those who flourish and those who flounder is preparation. Smart planners understand this phase may come—and they proactively seek out environments that offer support and engagement.
At Gateway Gardens, our community model is built to counteract disenchantment through active programming, shared experiences, and purposeful living.
This is the turning point—where you begin reshaping your life on your terms. New routines emerge. You find purpose in volunteering, socializing, creative pursuits, or perhaps something totally unexpected.
It’s a time to rediscover your passions and redefine your identity in this next phase of life. And here at Gateway Gardens, our daily calendar of enriching events, wellness activities, and interest-based groups makes this exploration easy and enjoyable.
By this stage, you’ve found your rhythm. You feel confident, connected, and content. The routines you’ve built support your lifestyle, and the community around you uplifts your spirit.
You’ve adapted to retirement—and are thriving in it. It’s no longer about “what you gave up” but about how much you’ve gained.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we’re committed to supporting each resident’s journey toward this stage of joyful stability—with a structured, secure, and welcoming environment that feels like home.
Understanding the emotional stages of retirement can help make your transition smoother, more positive, and more empowering. Each phase offers opportunities for growth and connection—and you don’t have to go through them alone.
When prospective residents tour Gateway Gardens, they often say the same thing: “This just feels right.”
We invite you to experience it for yourself. Visit us here in Winder and discover the comfort, community, and care that define our difference.
21 July 2025

Greetings once again from your senior living experts here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
Every so often, we receive heartfelt words from the families of our residents—messages telling us that they’ve never seen their loved one so happy, so socially engaged, and with such a positive outlook on life. Those moments affirm everything we strive to do at Gateway Gardens. They remind us why we do what we do.
Socialization is not just a luxury—it’s a biological need. As far back as the 1940s, psychologist Abraham Maslow recognized “belonging” as one of the most essential human needs in his famous Hierarchy of Needs. We all need acceptance and connection—not just from family, but from a broader community.
At Gateway Gardens, creating opportunities for connection is one of our primary goals. From our thoughtfully designed community spaces to our enriching programs and services, we foster a supportive environment that brings people together—especially vital as seniors face physical limitations or see long-time social circles change.
We follow a multi-dimensional wellness philosophy that emphasizes physical, mental, emotional, and cognitive health—all of which are strengthened by social interaction.
Our community actively integrates residents’ past vocations, passions, and interests into clubs and initiatives they help shape. Why? Because socializing is a full-body exercise for the mind. It’s about memory recall, conversation, emotional connection, shared interests, and joy.
Whether it’s a group art class, a gentle yoga session, or just a chat on the patio, social engagement works wonders for our residents:
Research shows that maintaining a strong social life as we age can result in:
“Feeling socially isolated can be as toxic to your health as smoking.”
— Research on senior wellness and cognitive health
One of the best ways to benefit from all these advantages is to move into a senior living community before health or mobility becomes a concern. Early transitions allow residents to build friendships, participate in programs, and feel fully connected from day one.
Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we are committed to providing uninterrupted opportunities for engagement, activity, and purpose.
If you’re considering senior living for yourself or a loved one, contact us today to learn how we support thriving, connected lifestyles at every stage.
14 July 2025

Welcome back to the Gateway Gardens Assisted Living and Memory Care blog. We’re always grateful for your feedback—it’s clear that our shared experiences are making a real difference in the lives of caregivers and families like yours.
One of our most-requested topics is summer safety—especially as it relates to hydration and heat management for seniors with memory challenges. A thoughtful reader recently told us that focusing on hydration made a noticeable improvement in her mother’s energy and mental clarity. Inspired by that feedback, we’re revisiting this important topic with a broader five-step plan to help you care for your loved one during the hottest months of the year.
This is the most important step on our list. If your loved one is mobile and tends to move around independently, they could accidentally venture outside during peak heat—putting them at risk of heat stroke or overexposure.
What You Can Do:
The sun is strongest between 11 AM and 3 PM, making it the most dangerous window for sun exposure.
Tips to Help:
Seniors—especially those with memory loss—can forget to drink water, which leads to dehydration before symptoms even appear.
Ways to Encourage More Drinking:
Technology can give you peace of mind. Many devices now allow you to set up “safe zones” and receive alerts if your loved one moves beyond them.
Popular Tools:
Managing the temperature inside and ensuring proper clothing choices can make a big difference.
Stay Cool Strategies:
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, our mission goes beyond professional care—we see ourselves as an extension of your family. Your trust in us inspires everything we do, and it warms our hearts to know that our blog continues to support your caregiving journey.
Let’s keep our loved ones safe, comfortable, and thriving this summer—together.
30 June 2025

At Gateway Gardens Assisted Living & Memory Care in Winder, GA, what makes our memory care team so exceptional is a heartfelt combination of learned skills and innate compassion. This profession draws those with a natural love and kindness for our memory-challenged seniors, and federal holidays like the Fourth of July offer a special opportunity to lift their spirits and create cherished moments together.
Here are some simple and meaningful ways to celebrate Independence Day with your loved one:
Fire up the grill, set the picnic table, and enjoy a traditional Fourth of July celebration. Keep it classic with hot dogs, brats, and burgers, or spice it up with BBQ chicken or steak kebabs. Consider organizing a potluck to ease the workload. Don’t forget festive favorites like lemonade, watermelon, and a few sparklers to cap off the evening.
Gather friends and family in the community’s outdoor space for fun, low-impact games. Try classics like:
If it’s a warm day, a water balloon toss can bring some refreshing fun. Want to get creative? Mix corn syrup and dish soap to blow giant bubbles using a wire coat hanger shaped into a wand—guaranteed smiles all around!
If your loved one prefers a quieter day, unfold a lounge chair and dive into a favorite book. Our local library or community book clubs can recommend summer reads for every interest. Reading outdoors offers a peaceful and rejuvenating way to enjoy the holiday.
A gentle walk in nature does wonders for both physical and mental well-being. Take your loved one to a nearby park—especially one they haven’t visited in a while—for a change of scenery and a breath of fresh air. It’s a simple yet meaningful way to spend quality time together.
Many local events include live music, food, and, of course, fireworks! Check out what our Winder community has planned and bring your loved one to enjoy the patriotic sparkle in the sky. Bring a blanket, some snacks, and make it a memorable evening.
Here at Gateway Gardens, we deeply value the bond we share with the families of our residents. That mutual love and commitment to our seniors is what makes our community so special. We look forward to seeing you waving your flags, smiling wide, and enjoying this day of celebration with those who matter most.
23 June 2025

Welcome back to the final installment of our June series for Alzheimer’s & Brain Awareness Month, brought to you by your friends at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
Over the past few weeks, we’ve been honored to share tips and insights aimed at empowering families, caregivers, and loved ones impacted by Alzheimer’s disease. As we wrap up this series, we offer five final—but powerful—tips that anyone can use to support brain health and memory care efforts.
11 – Learn About the Disease
Knowledge is empowering. Read books, attend support group meetings, explore online resources, and talk with healthcare professionals to better understand Alzheimer’s disease. The more you know, the better you can respond with compassion and confidence.
12 – Promote Communication with Doctors
Be an active participant in your loved one’s medical care. Ask questions, voice your concerns, and stay informed about the progression of the disease and care options available.
13 – Kindness, Humor, and Creativity are Essential in Providing Care
Physical touch—like hugs or hand massages—can speak louder than words. Light moments of humor and creative activities can strengthen your bond and bring emotional comfort to both you and your loved one.
14 – Discuss the Situation with Your Family and Friends
Don’t carry the burden alone. Keeping an open line of communication with your support system is vital. Share responsibilities and engage in cognitive activities such as listening to music, playing memory games, or doing puzzles together.
15 – Adopt a Positive Attitude
While Alzheimer’s may change your relationship, it doesn’t eliminate the opportunity for connection. Celebrate the strengths your loved one still has. Cherish the shared moments and focus on joy where you can find it.
As June comes to a close, we want to thank you for joining us in this important awareness effort. Our mission at Gateway Gardens Assisted Living and Memory Care is to deliver peace, comfort, and the highest possible quality of life to all our residents, especially those living with memory care needs. For us, this is not just a service—it’s who we are.
16 June 2025

As we shared with you last week, here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we’re continuing our pledge to double down on raising awareness and encouraging early recognition of Alzheimer’s symptoms. June is Alzheimer’s & Brain Awareness Month, a time to highlight how we can all take better care of our cognitive health—today and in the years ahead.
No matter your age, there are simple, powerful steps you can take to protect your brain. Picking up where we left off last week, here are five more tips for boosting brain power and promoting long-term mental wellness:
6. Protect Your Head
Traumatic brain injuries can increase the risk of cognitive decline and dementia. Always wear a helmet during activities like biking or contact sports.
Prevention matters—protecting your head today safeguards your brain tomorrow.
7. Improve Your Heart Health
Chronic conditions like high blood pressure, obesity, and diabetes can negatively affect your brain. What’s good for your heart is good for your brain!
A healthy circulatory system fuels both the heart and mind.
8. Challenge Your Mind
Keep your brain sharp by solving puzzles, learning a new skill, or playing strategy games.
Mental stimulation strengthens neural pathways and enhances cognitive function.
9. Stay Socially Engaged
Isolation can lead to cognitive decline. Stay connected with family, friends, or your community.
Meaningful interactions stimulate the brain and improve emotional health.
10. Exercise Regularly
Regular aerobic and strength-training exercises improve circulation and may reduce the risk of dementia.
A strong body supports a strong mind—movement matters!
At Gateway Gardens, we are privileged to serve those with memory care needs by providing a supportive, enriching, and loving environment. Sharing tips like these is part of our mission to help every individual—not just our residents—live with better brain health and a higher quality of life.
Stay tuned for Week 4 as we continue to share ways to protect your brain and care for those affected by Alzheimer’s.
9 June 2025

As we shared last week, all of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA are committed to raising awareness and encouraging early recognition of Alzheimer’s during Alzheimer’s & Brain Awareness Month.
June is a time to focus on protecting and strengthening our brain health—because no matter your age, there are simple, daily habits that can support your memory and mental sharpness for years to come.
Here are five powerful tips to boost brain health today:
1 – Prioritize Sleep
Lack of sleep can interfere with memory and thinking skills. Quality sleep is essential for brain function, especially for memory consolidation. Aim for 7–9 hours of restful sleep each night.
2 – Eat a Brain-Healthy Diet
A balanced diet rich in fruits, vegetables, whole grains, and healthy fats supports overall brain health. The nutrients in these foods fuel cognitive function and may lower your risk of decline.
3 – Keep Learning
Lifelong learning helps build cognitive reserve and strengthen neural pathways. Whether it’s taking a class, picking up a new hobby, or reading daily, keep your brain engaged and curious.
4 – Quit Smoking
Smoking reduces blood flow to the brain and significantly increases the risk of cognitive decline. Quitting today improves your long-term brain and lung health.
5 – Support Your Mental Wellbeing
Mental health matters. Depression, anxiety, and chronic stress can negatively affect your brain. Don’t hesitate to seek help—taking care of your emotional wellbeing supports your cognitive health too.
At Gateway Gardens, we are proud to offer support, resources, and expert care throughout every stage of cognitive health. For those facing memory-related conditions, it is our honor to provide the highest level of peace, comfort, and quality of life.
This is what we do. This is who we are.
2 June 2025

June is Alzheimer’s and Memory Care Awareness Month, a time dedicated to increasing understanding, compassion, and support for individuals and families affected by Alzheimer’s disease and other forms of dementia. Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we’re committed to doubling our efforts this month to raise awareness and encourage early recognition of the signs of Alzheimer’s. Early diagnosis and treatment can significantly improve quality of life—for both those living with the disease and their caregivers.
We encourage you to take this time to:
Alzheimer’s is a progressive, irreversible brain disorder that gradually impairs memory, reasoning, and the ability to perform daily tasks. Over time, it leads to the need for full-time care.
Although the exact causes of Alzheimer’s remain unclear, research points to a combination of genetic, environmental, and lifestyle factors. While risk factors like age, family history, and heredity cannot be changed, emerging studies suggest that others—such as diet, exercise, and mental engagement—may be within our control.
Today, an estimated 6.5 million Americans of all ages live with Alzheimer’s.
We know it can be uncomfortable to talk about Alzheimer's disease—but starting the conversation early is one of the best things you can do. The disease progresses over time, which means the challenges will increase. Our goal is to help you prepare—emotionally, physically, and mentally—so both you and your loved one can maintain the highest possible quality of life throughout the journey.
Whether you’re part of our Winder community, a loved one’s family member, or a dedicated at-home caregiver, we consider you family. We're honored to support you with the same compassion, skill, and dedication we would give our own loved ones.
Together, let’s raise awareness, spread understanding, and provide loving, informed care for those affected by Alzheimer’s and other dementias.
26 May 2025

Hello everyone from your friends and neighbors at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
If it hasn’t already happened, chances are it will one day: your loved one with memory loss will ask you to do something that simply isn’t possible. They may ask you to “go get my husband,” even though he passed away many years ago. Or they might say, “I’m ready to go home. Take me home,” even though they are already at home with you—or here with us.
These moments can be emotionally difficult. Today, we want to offer you some helpful things to consider when they arise.
For someone living with dementia, “home” often means more than just a physical place. It can represent a time or feeling of comfort, familiarity, or safety. They may be thinking of a childhood home, a house from many years ago, or even an idealized place that never physically existed.
Instead of correcting or reasoning with them, try to understand and validate the emotions behind their words. You might gently ask, “Tell me about your home—what did you love about it?” This can open the door to a comforting conversation that helps them feel seen and heard.
If you found yourself in a strange or unfamiliar place, wouldn’t you want to go “home” too?
Let your loved one know they are safe and cared for. A gentle touch, like holding their hand or placing your hand on their arm, can be very reassuring if it feels appropriate. Words like, “You’re safe here. I’m with you,” can help soothe their anxiety.
Wanting to “go home” can sometimes stem from deeper emotions—fear, sadness, loneliness, or confusion.
Ask yourself: Is this happening more often when they’re alone or not receiving visitors? Are there signs they’re not adjusting well? Talk to staff members—they might notice patterns or know if something has changed in their routine or mood. Sometimes, just knowing someone is paying attention to their feelings can be a comfort.
Sometimes a kind distraction can help. Keep a photo album handy—whether it’s a printed book or a gallery on your phone or tablet. Reminiscing about familiar people and places may calm their anxiety and bring joy. You might also suggest a walk, a snack, or their favorite activity.
If your loved one frequently asks to go home, note the time of day or circumstances when it happens. Is it around mealtime? When the environment is loud or overstimulating? Do they ask more often when it’s quiet or when fewer people are around?
Noticing patterns can help you—and the care team—better manage these moments and perhaps prevent them altogether.
At Gateway Gardens Assisted Living and Memory Care, we understand the challenges, emotions, and beautiful moments that come with caring for someone with memory loss. You are not alone on this journey. We’re honored to support you and your loved one every step of the way.
May strength, patience, and moments of peace and joy find you often.
Warmly,
Your Friends at Gateway Gardens Assisted Living and Memory Care
19 May 2025

Welcome back to our Assisted Living and Memory Care blog!
As we age, it’s not uncommon to experience a diminished sense of purpose or increased feelings of loneliness, depression, or anxiety. However, engaging in volunteer work or participating in community activities can provide tremendous emotional and psychological benefits. Volunteering not only helps others—it can bring seniors joy, fulfillment, and a renewed sense of self-worth. Here are some of the many ways volunteerism can positively impact mental well-being:
Life transitions such as retirement can sometimes leave us feeling uncertain or disconnected. Volunteering allows seniors to reestablish a sense of purpose by making meaningful contributions to their communities. The act of helping others fosters a deep sense of accomplishment and reminds us that we still have so much to offer.
Volunteering creates opportunities to meet like-minded individuals who share similar passions. These interactions often blossom into meaningful friendships and support networks that help combat feelings of isolation. Staying socially engaged is a vital part of maintaining emotional health and overall happiness.
That warm, uplifting feeling after helping someone? It’s more than just a mood boost. Volunteering stimulates the release of "feel-good" hormones like dopamine and oxytocin, which contribute to a greater sense of happiness and emotional satisfaction.
Many volunteer roles involve learning new skills, problem-solving, or engaging in creative thinking—all of which help keep the brain sharp. Regular mental stimulation can reduce the risk of cognitive decline and support overall brain health.
Focusing on helping others allows seniors to shift their attention away from personal stressors. Volunteering cultivates a sense of calm, reduces anxiety, and boosts self-esteem by creating a sense of achievement and purpose.
To experience the full mental health benefits of volunteering, it’s important to choose opportunities that align with one’s interests, abilities, and schedule. Whether it’s mentoring children, helping at a local shelter, or contributing to causes within their own community, seniors can make a meaningful impact in countless ways.
Join Us in Living a Fulfilling Life
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we believe that aging should be vibrant, purposeful, and joyful. Our programs are designed to support not just physical health, but also emotional and mental well-being. We encourage residents to stay actively engaged and connected through volunteer opportunities and community involvement.
If you or a loved one are ready to embrace a secure and enriching retirement lifestyle, we invite you to reach out to our caring team in the Winder area. Together, we can make a positive difference in our community—and in each other’s lives.
12 May 2025

Greetings once again to our cherished residents and family members of Gateway Gardens Assisted Living, Memory Care, and Respite Care communities.
While many come to appreciate the simplicity that comes with downsizing, the transition can be an emotional or logistical challenge for others. Today, we’d like to share some thoughtful strategies to help you manage your lifestyle more comfortably and joyfully within a smaller footprint.
Creating more usable space starts with letting go of what no longer serves you. It’s easy to develop sentimental attachments to belongings, but too much “stuff” can quickly make a smaller space feel cramped. Focus on keeping items with true sentimental or functional value. Consider donating or selling the rest.
Make it a habit to declutter every few months. If you haven’t used something since your last decluttering, ask yourself if it’s truly essential.
After decluttering, be selective about what you bring into your home. Each new item should have a clear purpose or bring you joy. If you’re thinking about buying a new gadget or piece of furniture, take a few days to reflect before purchasing. Ask yourself:
Furniture size and functionality make a big difference in small spaces. Oversized pieces can overwhelm a room, so aim for a balance between comfort and scale.
Consider:
Every item in a smaller home should earn its keep. Look for furniture that offers multiple uses:
These clever options add functionality without adding clutter.
When closet and cabinet space is limited, think creatively:
Once you’ve found your storage spots, keep them tidy and efficient:
Well-organized storage not only saves space but also makes everyday life easier.
Finally, always consider how your layout affects your ability to move comfortably through your home. Clear walkways and wide paths around furniture make a space feel more open—and safer.
Try different arrangements until you find one that allows you to move freely while still enjoying your furniture’s function.
While adjusting to a smaller living space may seem daunting at first, many find it refreshingly liberating over time. With a little creativity and planning, your new space can be just as cozy, functional, and beautiful as any larger home.
To learn more about the rewarding lifestyle here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we invite you to reach out anytime. We’re here to support you every step of the way.
5 May 2025

Welcome back to the Gateway Gardens Assisted Living and Memory Care blog! Every member of our team is devoted to enhancing the quality of life for the residents of our assisted living and memory care communities—as well as supporting their families and friends.
While your loved one is never alone here at Gateway Gardens, we understand that many at-home caregivers face the emotional and physical challenges of providing care. This post is here to remind you just how valuable your presence is to the health and happiness of your loved one—and how that simple presence can even help reduce their risk of dementia.
Dementia is a broad term used to describe a range of symptoms affecting memory, thinking, and social abilities. According to the World Health Organization (WHO), someone in the world develops dementia every three seconds. While not all causes of dementia are known, researchers continue to study contributing factors and potential preventative measures.
Some risk factors for dementia—such as age, genetics, or pre-existing conditions—are beyond our control. However, other factors can be influenced by lifestyle and environment. One growing area of research is the link between loneliness and cognitive decline.
In a recent study, researchers surveyed 12,000 individuals, tracking their levels of loneliness, social isolation, behaviors, and genetic predispositions. Loneliness was defined as "a feeling that you do not fit in or do not belong with the people around you.” Over a ten-year period, the researchers monitored participants for signs of dementia.
The results, published in The Journals of Gerontology, showed a striking finding: individuals who were socially isolated were significantly more likely to develop dementia. In fact, loneliness was associated with up to a 40% increase in dementia risk.
This isn’t the only study to report such a link. A separate review published in Aging Research Reviews also found that low social participation and infrequent social contact are associated with a higher risk of dementia.
If you've noticed your aging loved one becoming more socially withdrawn or isolated, don’t hesitate to reach out. Sometimes, simply talking about feelings of loneliness can be a powerful first step. You might also consider these questions:
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, we foster a warm, inclusive environment that promotes engagement and connection. Through structured activities, shared meals, and compassionate care, we create opportunities for our residents to stay active and socially connected—an important step in maintaining cognitive health at every stage of life.
If you're concerned about your loved one’s isolation or are simply exploring the best ways to support their health and happiness, we’re here for you. Reach out to learn more about how Gateway Gardens can make a difference.
28 April 2025

As a caregiver, being responsible for the well-being and happiness of your loved one can come with a wide range of emotions. Most certainly in many, many ways it is a deeply rewarding role. However, we know with certainty that caring for your Winder-area memory care loved one comes with challenge and cost to your mental and physical wellbeing.
If you’re the primary caregiver of a family member, you’ve given much of your time and effort toward making sure that your loved one can enjoy the highest quality of life possible. But what happens when you’re no longer able to provide senior care at an acceptable cost to your own health and wellness? We want you to think about this very important question: How do you start the conversation with family members and openly discuss the next steps of finding the right level of care for your loved one?
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, our assisted living community and our memory care community provide home-like living that deliver professional assisted living support services that will return you to the quality of life that both you and your loved one deserve. Let us be clear. We know you are doing your absolute best. However, the simple truth is assisted living and memory care needs will (not if) arise to where a team of professionals are required to step in for the health and wellness’ sake of all.
Accept and Acknowledge Your Feelings
Many caregivers reach a breaking point after serving as the primary caregiver for a family member. This is nothing to be ashamed of, but it can bring up a myriad of challenging emotions and feelings.
Whether you’ve neglected self-care and are facing caregiver burnout, stress, or guilt, or you’re simply unable to balance a demanding career or personal life along with your caregiving responsibilities, it’s essential to be kind to yourself as you begin to acknowledge your reasonings for being unable to provide senior care.
By being honest with yourself about your limits and abilities, you’re allowing your family members to find the level of care they deserve and need to thrive and live happily.
Maintain a Positive Mindset
Caregiving creates strong bonds between the person providing and receiving care, especially if it’s your parent or a close relative. As mentioned previously, this can lead to feelings of guilt when you’re no longer able to provide senior care.
Perhaps your family member has reached a point where they require additional assistance that you aren’t qualified to provide, or you simply don’t have the extra time to offer the full spectrum of care that they need for them to live comfortably and joyfully.
It’s important to note that by researching professional care services, you’ll quickly find that deciding you’re unable to continue providing senior care is the best possible option for your loved one’s health and well-being. When you reframe your thoughts and maintain a positive mindset, you can better understand how this decision will benefit your family members in the long run.
Start the Conversation
Once you’ve come to terms with your decision, it’s time to start the conversation with other family members. This might bring about some complex family dynamics, and you might already be anticipating feelings of resentment or disappointment from certain members of your family.
However, it’s crucial to avoid bringing up past issues or arguments during this time and avoid both making or responding directly to personal remarks that could be hurtful.
Stand firmly in your decision and remind yourself and your family members that this is the best possible option for yourself and for your loved one’s health, safety, and well-being.
If the conversation begins to take a negative turn, ask your loved ones to place themselves in your shoes for a moment. Make sure they ultimately understand that your loved one should not receive senior care from someone who doesn’t have the ability or time to provide the support they deserve.
Discuss Options
At Gateway Gardens Assisted Living and Memory Care here in Winder, professional care for your loved one means living joyfully and fulfilled in enabling of a lifestyle that every individual involved desire and deserves. Our community stands out from the rest in the variety of services, engagement, and fulfillment that our team provides for residents every day.
To learn more about our assisted living community and our memory care community in Winder, contact any member of our Gateway Gardens team.
21 April 2025

It’s not surprising that those who are caregivers for aging parents experience extensive stress. From supervision to running errands to even making sure their parents are taking their medication; caregiving is both emotionally and physically exhausting. This is why those who care for senior parents at home are more prone to depression than those who aren’t.
There are several contributing factors, and one of the main issues is that caregivers frequently put their own needs on hold. Caregiving consumes so much time and effort that there is little left over for self-care. This is one reason that assisted living communities like ours have become such an important option to help relieve caregiver stress.
This means that every time you put off taking that time for a walk around the neighborhood, coffee with a friend, or even getting a good night’s sleep, you’re depriving yourself—and others–of the care needed.
Did you know that May is Mental Health Month? Throughout May we will examine how professional assisted living can be a viable solution for both dependent and care providers alike.
Caregiver Depression by the Numbers
The Family Caregiver Alliance cites these facts:
It’s important to note that caregiving itself doesn’t cause depression, and depression may be the result of several factors.
Sometimes, feelings of anger, anxiety and isolation can be contributed to the elements. Often, depression can be caused by brain chemistry, which is why it’s important to talk to a counselor or health care professional if you are experiencing the signs of depression.
What Are the Signs of Depression?
If you suspect (or even question) whether you may be suffering from depression, you should immediately speak with your health care professional. Here are just some of the signs:
Methods to Cope with Caregiver Depression
There’s not any one method that works for everyone, so a part of your journey to wellness begins with exploring what is appropriate for you. However, in general:
How Can Professional Assisted Living Help Caregivers
Caregiving is an all-encompassing and often frustrating job. Professional assisted living is a wonderful solution because we can provide your loved one with assistance with medication management, bathing and other activities of daily living. However, we always support your loved one’s independence and enable them to live independently as long as safely possible.
Those in assisted living do not need 24/7 medical supervision. Of course some people do require 24/7 care services and that is why you can turn to professional memory care options like ours for those who have Alzheimer’s or other dementias.
The big takeaway here: The option of professional assisted living services here in Winder or our professional memory care services in Winder means that you can step back into your role as son, daughter or spouse and allow us to care for your loved one with the dignity and care they deserve.
Contact us to schedule a tour today!
14 April 2025

Regardless of the religious beliefs of you or your loved one within their assisted living community or their memory care community, Easter is a good opportunity to welcome the spring season and engage in Easter-related activities. We hope that you’re planning a get-together this upcoming Easter weekend. If you’re looking for a few fun ways to put a smile on your senior’s face, here’s some simple things to consider.
Prep time
If you’re hosting the shindig, invite your elderly family members or friends over to help decorate, prepare place settings for guests or put the finishing touches on food offerings or dessert. They’ll appreciate the gesture and be pleased they get to lend a hand in planning something for the family.
Get crafty
Dyeing eggs and decorating Easter baskets is a fun pastime for many families. These are great, hands-on craft projects for seniors to partake in because there are no sharp tools involved and they are simple and easy. Helping organize an Easter egg hunt for the younger family members is another way seniors can contribute to the party. It also allows them to spend quality time with grandchildren, who they might not have the chance to see often.
Go to church
Many seniors may be interested in going to a local church service. If you’re not able to attend a church service, see if there are any senior services or music at a local community senior center. A day of singing and music can make the holiday special for your elderly loved one.
We Hope to See You This Weekend
Even if you can’t visit your elderly loved one in person, make it a point this Easter holiday to give them a call to catch up or pop a nice card in the mail to let them know they’re in your thoughts.
For those of you with a senior loved one residing within our Gateway Gardens assisted living community or our Gateway Gardens memory care community in Winder, GA, you can rest assured that they will experience a special Easter celebration this upcoming weekend. But nothing beats family, and they (and we) hope to share the celebration alongside you. If you can’t visit your elderly loved one in person, make it a point this Easter holiday to give them a call to catch up or pop a nice card in the mail to let them know they’re in your thoughts.
7 April 2025

Welcome back to our Gateway Gardens assisted living and memory care blog where we strive to enlighten those of you who on subjects vital to those who provide senior assisted living services or memory care services to your loved one.
Regarding the subject of taxation, well, this is going to be a fun read, right? You might rather hear fingernails on a blackboard than discuss the subject of taxation. We get it. But tax season is here, and this time of year can be stressful for anyone, but it can be even more stressful for seniors who are trying to navigate tax preparation. If you are a senior, or you are a family member of a senior, you may need help filing taxes.
Here are just a few tips to help seniors during tax season:
1. Beware of Scammers
Tax season is the perfect time for scammers to try to take advantage of the elderly. Too often con artists will make unsolicited contact via text, email, or phone to try to obtain personal information. They are sometimes threatening or intimidating by claiming to be a higher authority. Remember that the IRS will not make unsolicited calls, nor will they ask for personal information, including your social security number, over the phone. Never wire money over the phone and never buy prepaid cards or gift cards to pay for “dues” they say you owe.
2. Calculate Your Social Security
Social security benefits alone can be confusing. But trying to figure out the taxable amount of those benefits can be overwhelming. If you are a senior preparing your own taxes, it is imperative to CAREFULLY complete the Social Security benefits worksheet. Tax season is the perfect time for scammers to try to take advantage of the elderly. Too often con artists will make unsolicited contact via text, email, or phone to try to obtain personal information.
3. Know What You’re Entitled To
As a taxpayer of age 65 or older, you can qualify for extra tax breaks. For example, you can get a bigger standard deduction, a higher tax-filing threshold, property tax breaks, a tax credit if you also have low income, and best of all…free tax help! Be sure to check your resources for additional tax benefits.
4. Get Free Tax Help
The Tax Counseling for the Elderly (TCE) program provides free tax assistance for taxpayers aged 60 years or older. IRS-certified volunteers, who are knowledgeable about tax issues relevant to seniors, will review your taxes and assist with basic tax preparation and electronic filing. You can locate the nearest TCE representative near you on the IRS website.
5. Get Ready for Next Year
Now is the time to get organized for next year. Ensure your electronic records and paper documents are easily accessible. This will make it less stressful during next year’s tax season.
Rest Easy at Gateway Gardens
If your senior loved one is an existing member of our Gateway Gardens assisted living community or our Gateway Gardens memory care community in Winder, GA, you can rest assured that your loved one’s best interest are why we choose this profession. Whether it medication, nutrition, physical safety, positive mental health, socialization, love and understanding, and yes, taxes….we endeavor to positively each daily, and on an improving daily basis. Just like you do.
31 March 2025

When you are looking for memory care services for a loved one, you might hope to find a single-source FAQ page that answers all your questions. Unfortunately, the range of questions that you seek answers for are wide and numerous. So today, we thought we’d start out by addressing five of the most common questions regarding memory care that we answer routinely. We hope this helps.
1. What is Memory Care?
Although its structure within a senior living model can differ amongst communities, what memory care offers can be easily explained. Memory care services are specially designed for people with Alzheimer’s disease or other forms of dementia.
Communities with memory care services provide seniors with a structured environment, including set routines tailored to the individual resident’s needs and preferences, and safe environments to help residents feel secure. Memory care services include more security measures compared to standard assisted living communities, helping prevent residents from wandering too far away from home.
Seniors who need memory care enjoy specially trained staff to help with all their needs, including personal care tasks.
2. What’s the Difference Between Assisted Living and Memory Care?
There are many overlaps between professional memory care services and professional assisted living services. We provide both services and understand that people get confused when it comes to the relationship between the two.
Assisted living and memory care both provide residents with help with daily tasks like:
In addition to typical assisted living care, memory care residents get that extra level of supervision that helps them feel safe, and that reassures their loved ones. Memory care offers programming specifically designed to retain residents’ cognitive function. Communities also make sure that memory care residents can stay connected to loved ones while receiving the care they need.
3. Does Memory Care change as My Loved One Ages?
As assisted living residents age, their services often increase to include memory care. That’s why it’s smart, when looking at assisted living and memory care communities, to make sure the community you choose is prepared to provide both assisted living and memory care so that your loved one’s age in place. Studies reveal that comfort and stability is vitally important to every memory care patient.
When touring memory care communities, ask about how they’ll handle your loved one’s needs as they progress, and how that will impact the monthly costs of memory care. Ask specific questions about the availability of:
4. Do Memory Care Programs Ensure My Loved One is Engaged and Social?
Memory care programs should fill your loved one’s life with meaningful experiences that meet their needs. This helps to improve the quality of your loved one’s life, and it makes family visits and interactions more meaningful.
Quality senior living includes trained memory care specialists (like ours) who will talk to you and your loved one to assess their needs and strengths. This will help the community experts develop a structured experience that keeps your loved one’s interests and passions alive.
The best memory care programs will not just look at needs. They will also focus on your loved one’s existing abilities to maximize their strengths, rather than focusing on what they can no longer do. Top-tier memory care is all about making the most of what we have, and paving the way to an easier, brighter future.
If you’re touring a memory care community and the memory care services don’t seem to differ much from assisted living, keep touring different communities until you feel comfortable with the level of attention your loved one will receive. We’re confident to that end, all roads will lead you here to Gateway Gardens Assisted Living and Memory Care in Winder, GA! The right memory care program should know how to best communicate with your loved one, and it can provide meaningful therapeutic experiences including music, art, off-site outings, and more.
5. Does Memory Care Cost the Same as Assisted Living?
Professional care services, by nature, are more demanding upon staff, programs, and facilities than professional assisted living. Not surprisingly, memory care is more expensive than assisted living, but there is good news here, too. We have a tremendous track record for helping our resident family members successfully negotiate the fiscal transition to memory care. Time and time again our resident family members set aside their fear that memory care is simply unaffordable. Since your loved on is our loved on also, you will be amazed at the positive synergistic effect when determined family and professional care givers team to discover solutions that they can celebrate.
Call to Learn More
If you’d like to discuss these issues in more detail or work deeper into your personal FAQ list regarding Gateway Gardens assisted living or Gateway Gardens memory care services, we are ready to help. Call us today!
17 March 2025

Welcome back to our Gateway Gardens assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home whether you provide senior assisted living services or memory care services to your loved one.
First, a caveat. When it comes to financing managed care for you or your loved one, we are not your subject matter experts. A professional financial advisor is the one for you to take all accounts into consideration and to build a plan that is right for you. Yes, we are versed in the various ways that our cherished residents manage their managed care fiscal affairs, but the variety of ways that it is accomplished is precisely why we feel comfortable only providing general knowledge and ideas that you can get educated upon and take forward to your trusted financial advisors.
There are short-term financing options available for your long-term plan. If you are waiting for a house to sell, benefits to arrive, or simply want to explore additional funding options to pay for your care and service. You may want to consider:
Bridge Loans
Are you challenged with paying for senior living while waiting for your home to sell, Veterans or insurance benefits to begin or another financial event to occur? Or maybe the timing isn’t right to sell an investment, or for tax purposes it’s better to borrow. A Bridge Loan may provide peace of mind by “bridging your family’s funding gap”:
Real Estate Program
We understand life changes and a time comes when you may be looking to downsize, move into a retirement community, assisted living community, or in with a family or a friend. Where do you start and how do you assist a family member who is three blocks or three states away?
You may want to consider working with a realtor who is certified with an expertise in working with seniors; a Senior Real Estate Specialist or SRES. Their knowledge of your local market can assist you every step of the way. Other services that may be available to you include:
Insurance
You have paid premiums over the years to provide protection and security for yourself and your family. Now that you are considering senior living, you may decide to access your policies to pay for care.
Long-Term Care Insurance Claims Assistance
Many families are unaware of the complexities and time involved in preparing and filing Long Term Care insurance claims. Additionally, most owners of Long-Term Care policies do not realize the ongoing tasks required to properly manage an ongoing claim process. Often, policies have an elimination period or waiting period that ranges from 90 to 180 days where no insurance funds are paid. You may want to consider speaking with a specialist for help in reviewing your current policy. If you need access to funds during this elimination period, a Bridge Loan could assist in paying for care until your policy kicks in.
Life Insurance
In many cases, if you own a life insurance policy, there may be an alternative way to use your policy. Depending on your situation and policy, you may be able to sell or borrow against a life insurance policy to pay for senior housing and/or care expenses. With some programs, you can potentially preserve a portion of the insurance benefit for your designated beneficiaries and still obtain proceeds today.
Community Entrance Fee
Perhaps you need help moving to assisted living Life Care Retirement Community (LCRC) before your home has sold, without being required to liquidate assets. A personal consultation with a CCRC Sales Specialist might help in determining the most appropriate options available to you.
Wealth Preservation
For families that have assets or equity in a home, you may want to consider speaking with a specialist to arrange a consultation with a partner who offers a monthly income product that may cover ongoing expenses. This product may help cover the costs of private pay care without spending all of one’s wealth. This income can be used for anything, including paying for living, medical or care expenses.
Please know that we stand ready to help you navigate this critically important research. Please contact us anytime here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
10 March 2025

Welcome back to our Gateway Gardens assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home whether you provide senior assisted living services or memory care services to your loved one. Today’s blog topic is a focus upon those of you lovingly caring for a loved one recently diagnosed with Alzheimer’s or other dementia-related condition.
When a loved one is diagnosed with dementia or Alzheimer’s disease, there is a wave of emotions they experience, but grief is often front and center. Grief for the life they may have lived without the disease, anticipatory grief, sadness, anxiety and much more. Regardless of your role in the caregiving journey, your loved one can use support and guidance through these feelings, and there are many ways you can help.
One of the initial reactions of any caregiver is questioning what to do after a dementia diagnosis. To be sure, a diagnosis of dementia or Alzheimer’s is serious, and your loved one may experience a full range of emotions. If your loved one is early in their journey, grief is a common reaction. Plus, there may be anxiety and distress with the acknowledgment of symptoms, learning of the disease progression, and anticipating what may happen to them in the future (known as anticipatory grief) is common.
As early as possible after diagnosis, have open and honest conversations with your loved one about their emotions and how they can affect their mental and physical health. The most important thing to emphasize with your loved one is that these are normal feelings and very common. It’s vital to validate their feelings and affirm they are not alone.
First, always remember that your loved one is a person – the person you know and love. But now, they are a person living with dementia or Alzheimer’s and one who needs a caring advocate.
As such, talking with your loved one’s healthcare team, if they’re open to including you, can help lay a foundation for truly understanding the disease and its diagnosis. Finding reputable sources to learn about the stages of Alzheimer’s and dementia also can help reduce early anxiety and depression.
Education goes a long way in breaking the stigma around dementia and Alzheimer’s diagnoses. For example, people with a diagnosis of Alzheimer’s or dementia may see their friends and family members withdraw due to their own misunderstanding of the conditions and out of fear of the changes they may see. When loved ones have the facts, assumptions and unfounded fears may lessen.
In addition to being there to support your loved ones through every part of their journey, work with them to find communities and support groups to help provide encouragement and comfort. In fact, these communities can be excellent support for dementia caregivers as well.
When you’re familiar with the stages of dementia and Alzheimer’s, it can be easier for you and your loved one to recognize changes and address them early with medical and support teams. After a diagnosis of dementia, plan to assist your loved one as they progress. From simple steps like setting up automatic bill pay to more involved processes such as putting financial and legal affairs in order, lower stress by preparing and planning.
If your loved one’s condition progresses to the point where they need elevated levels of professional care such as administration of medication, various therapies, wound care and assistance eating or drinking, consider your professional memory care options like ours here at Gateway Gardens.
While your role as a caregiver is vital, it’s also crucial that you care for yourself, helping to prevent burnout and overwhelming emotional stress. Just as your loved one should rely on resources such as support groups to find supportive communities, you should consider those tools for yourself as well.
If providing day-to-day care, know the types of resources available to help keep your loved one safe while giving you a break – meal delivery, visiting nurses and more. If providing care for your loved one is resulting in you neglecting your own basic health, don’t be embarrassed to ask for help. Eating nourishing foods, getting daily exercise, and finding some time for yourself are basic needs and caregiver respite is imperative.
Wherever you and your loved one are on the journey from dementia or Alzheimer’s diagnosis through the progression of the condition, stay educated, do your best to provide care and support for your loved one and never forget to care for yourself. Contact us for more information.
If you are a full-time home caregiver for your loved one, we want you to know that help for you is just around the corner, and we invite you to reach out to us anytime. If your senior loved one is receiving care in our Gateway Gardens Assisted Living and Memory Care community in Winder, GA, you already know that we are professionally trained and lovingly apply a wide range of proven techniques that maximize comfort to your memory challenged loved one. You can learn a lot from us….and we from you. May peace and strength be with you all.
3 March 2025

Well, National Napping Day is not until March 10th, but we thought we’d inform you well in advance of that.
All kidding aside, the purpose of this blog post is to rob you of excuses for seemingly having nothing to say right now to your loved one(s) residing within Gateway Gardens assisted living community or Gateway Gardens memory care community. Pick up the phone and simply say “Happy National Napping Day, Mom”! Who knows where the discussion will go from there!
Below is your guide for the entire month of March. Pick your date then pick up the phone. And have a warm and rewarding conversation.
PS: For heaven’s sake, don’t forget to call her on the 31’st for “National Tater Day”.
This loving advice is offered to you from your trusted, caring, and fun-loving professional caregivers at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
24 February 2025

Welcome back to our blog page for our Gateway Gardens Assisted Living and our Gateway Gardens Memory Care community. Today, we want to educate you about chiropractic care, a surgical and drug-free method of potential pain management and quality of life enhancement. Before going further, it goes without saying that your medical team is your first contact for all things related to health and wellness. With that said, today we simply want to introduce a health and wellness modality that is working for seniors across the country and could possibly work for you too.
As we age, our bodies naturally experience changes. From joint stiffness to decreased flexibility and strength, these changes can limit our mobility and overall quality of life. Chiropractic care offers a non-invasive, drug-free approach to addressing these issues. By aligning the spine and optimizing the nervous system, chiropractic adjustments can help seniors feel better and live healthier lives.
Here’s how chiropractic care can enhance longevity and promote a 100-year lifestyle:
1. Anti-Aging Benefits
Chiropractic care isn’t just for pain relief—it’s also a powerful tool for anti-aging. Regular adjustments help maintain proper spinal alignment, improve posture, and reduce the stress on joints and muscles. This can lead to increased flexibility, better balance, and greater mobility, all important factors in staying active as you age. By preventing stiffness and promoting joint health, chiropractic care helps you feel younger and more energetic.
2. Maintaining Mobility
As we age, our bodies can lose some of the mobility we once took for granted. Chiropractic care is designed to keep your spine and joints functioning at their best, helping you maintain the mobility necessary for daily tasks and physical activity. Whether it’s taking a walk, gardening, or playing with your grandchildren, maintaining your flexibility and strength is key to staying independent and active.
3. Pain Relief
Chronic pain, whether from arthritis, sciatica, or old injuries negatively impact quality of life. Chiropractic adjustments can relieve pain by reducing nerve interference and improving joint function. This can help reduce the need for medications and allow seniors to live with less discomfort, leading to a more enjoyable lifestyle.
4. A 100-Year Lifestyle
A 100-year lifestyle is all about optimizing your health, mindset, and overall well-being to live a full, vibrant life into your 90s, 100s, and beyond. Chiropractic care supports this lifestyle by keeping your body in top condition as you age. With regular chiropractic adjustments, you can improve your posture, enhance your balance, and maintain a healthy spine—contributing to a more independent, active, and healthier life.
5. Enhancing Quality of Life for Centenarians
Many centenarians—people who live to be 100 years old—attribute their longevity to maintaining an active lifestyle and prioritizing health. Chiropractic care is a key component of a healthy aging strategy, helping seniors stay active and pain-free for many years. By incorporating chiropractic adjustments into your routine, you’re investing in your health for the long haul, improving your chances of living a long, independent life.
For all of our dear residents and family within Gateway Gardens Assisted Living community and Gateway Gardens Memory Care community, we exist to enhance your quality of life. Chiropractic care is something you might be hearing about for the first time here in this blog post. If you’ve never enquired about it with your medical team, give it some thought. It could change you or you loved one’s life for the better.
17 February 2025

Welcome back to our Winder-area assisted living and memory care blog where we lovingly share our professional advice and offer our heartfelt support to all you home-based caregivers. Today, let’s talk about shoes. With apology in advance, we’re not going to discuss the latest in senior shoe fashion. We’re going to cover a much more important subject, shoe safety.
Balance in all aspects of life is a good thing. We work hard but make time for fun, love our children while setting boundaries, and eat healthy to enjoy a sundae on Friday night. But mental equilibrium isn't the only kind of balance that's important in life. Good physical balance can help seniors avoid the debilitating and potentially life-threatening complications of a fall.
Falls are the leading cause of fatal and non-fatal injuries among older people, according to the Centers for Disease Control and Prevention. A recent study calculated that annually, over two million fall injuries sent seniors to emergency rooms and over 600,000 required hospitalizations.
Reducing the fall risk of our senior loved ones must be a top health priority. Fall risk management is a core tenant of Gateway Gardens Assisted Living and Memory Care in Winder, GA, but fall risk management needs to be an active component of your home health care service to your senior loved ones.
Choosing safe shoes for your assisted living or memory care loved one is just one of the countless considerations and challenges that you face daily. Please know this. If caring for your senior loved one at home starts to feel overwhelming, know that you are not alone. Call us! Sometimes just sharing your questions and concerns with a trusted voice of experience….is all you need in that moment.
10 February 2025

Welcome back to all of you who benefit and enjoy our weekly assisted living and memory care related blog posts. Sometimes the answer to the question, “Are my Parents still self-Sufficient at home?” is answered by way of a phone call. A call like one of our associates recently received:
“Ma’am, this is police officer Jones. Your mother is fine, but I just pulled her over for driving 10 MPH in a 45 MPH zone. It took her a while to notice me and my flashing lights behind her, and then it took her some time to understand that I needed her to pull over. Again, she’s OK, but she’s lost, confused, and scared, and does not know her way home. We need you and another to come and get her and her car”.
As you age, watching your parents become less competent with their everyday tasks can be difficult. The warning signs might not be as obvious as that described above, but there are signs to the observant that indicate the need for more care to help them live at home safely and comfortably.
Here are some signs your loved one might need assistance.
Below are just two examples relating to the benefits provided by professional managed care like ours here at Gateway Gardens:
Senior isolation is a major factor in feelings of depression and loneliness. But that doesn’t have to be the case if your loved one lives at assisted living. Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, our residents enjoy socializing during lunch, dinner, fitness class, Bible study, game nights, and so much more.
Seniors often lack the energy or resources to grocery shop, which can lead them to losing access to proper nutrition. It is common for seniors as they age or when loved ones lose their motivation and interest in cooking for one person. This causes a negative impact on senior health such as weight gain and muscle loss.
All of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA carry our deepest respect and best wishes for all of you providing your loved ones with assisted living and/or memory care services there at home. We manage this assisted living and memory care blog in the trust that is serves all of you at-home caregivers to provide efficient and improved care services while simultaneously lowering the known burden that comes with your selfless care endeavors.
3 February 2025

Transitioning from professional assisted living to professional memory care here in Winder is blessedly comfortable for our residents and their families. Familiarity and trust, often the most difficult challenges associated with this life change are baked into the transition process. So, this memory care blog post is more for those of you out there who are not currently engaged within professional assisted living or memory care services.
Roughly one in every seven seniors in America is affected by some form of dementia. For many of these older adults, memory care is the best option for a safe living environment that preserves their dignity. However, the transition into a memory care community even as professional managed as ours can be tricky to manage. Fortunately, you can do things to simplify and smooth out this process. As assisted living and memory care professionals, we recommend that you follow a few tips to better support your loved one.
Effective planning is typically crucial when it comes to easing the move into a memory care program. Aspects of a solid plan include:
When talking about memory care, you may want to follow an agreed-upon script instead of speaking spontaneously. This step can help you comfort your loved one and avoid any misunderstandings. The same holds true when it comes to helping your loved one pack up their treasured belongings and creating a new environment that mirrors aspects of what they already know.
The things you do on moving day can pay big dividends for you and your loved one. There’s a good chance that the day will be stressful and highly emotional. It’s important that you acknowledge these feelings. Ask your loved one how they’re doing. Regardless of how they respond, try your best to remain supportive and empathetic.
We recommend that you do a few other things. First, you can help your loved one get familiar with our staff. In addition, you can help them start the process of socializing with their new neighbors. It’s also important for you to talk to the staff yourself. This will allow you to establish solid channels for ongoing communication in the future.
The question of how to most comfortable transition an Alzheimer’s patient into memory care remains relevant after moving day. For some it takes a considerable amount of time to fully adjust to their new living environment. Awareness of this fact will help you temper your expectations.
Visits to your loved one can be vital for them, as well as for you. However, you need to exercise caution when making these visits. Why? Unless you’re careful, you may add to your loved one’s feelings of dislocation and distress. Specific steps you can take to limit this possibility include:
Why visit in the morning? Seniors with dementia are typically more alert at that time of day. By participating in an activity with your loved one, you help fit your visit into their daily routine. In turn, this step can help make the visit less disruptive or distressing.
Want more information on smooth transitioning to memory care? Gateway Gardens Assisted Living and Memory Care in Winder, GA are standing by. We have extensive experience supporting seniors and their families at this crucial time. No matter the questions you have, we can answer them.
27 January 2025

Welcome back to our blog page for our Gateway Gardens assisted living and our Gateway Gardens memory care community. We often choose our blog topics based upon frequently asked questions regarding the services offered here at Gateway Gardens. Questions like “What exactly is assisted living” and “How do I know when assisted living is now in my mom’s best interest”?
Well, guess what? Many of us here on staff are children of aging parents just like you. We ask ourselves the exact same questions. A major difference between them and you, however, is we get to witness first-hand the amazingly positive effects of assisted living. And we get to personally here our family members testify why they are so grateful for making the hard decisions that have elevated the health and wellness of their loved one.
So, let’s get to some of the basics that hopefully you will find both informative and actionable.
Assisted living, a term often associated with senior care, refers to a residential option designed for individuals who require assistance with daily activities but do not need the extensive medical care provided in a nursing home. This form of care, commonly referred to as “assist live”, combines personal care services, supervision, and in some cases, healthcare, in a way that promotes maximum independence for residents.
Assisted living communities like ours play a pivotal role in the long-term care spectrum. They offer a middle ground between independent living, where seniors live autonomously with minimal assistance, and nursing homes (nurse home), which are designed for those requiring continuous skilled nursing care (skilled nurse care). Assisted living thus caters to those who fall in between these two extremes, offering a balance of support and autonomy.
The primary difference lies in the level of care and support provided. Independent living is geared towards seniors who are largely self-sufficient but enjoy community living. Nursing homes, conversely, are for those who need 24-hour medical attention and assistance. Assisted living, meanwhile, is tailored for individuals who need help with activities of daily living like bathing, dressing, or medication management but do not require intensive medical supervision.
Assisted living becomes a viable option when the tasks of daily life become challenging, and the safety and well-being of the individual can no longer be assured at home. This need may arise due to age-related conditions, mobility issues, or cognitive impairment.
Recognizing these needs early is vital. Warning signs include difficulties in managing activities of daily living, noticeable decline in hygiene, unexplained injuries, or forgetfulness in taking medication. These indicators suggest that an assisted living community could provide the necessary support and care.
You simply need to visit all the communities you might consider entrusting your loved one to. We know that you will (and should) have a long list of questions. Often, However, decisions become surprisingly easy. Your eyes, ears, nose, and heart will largely be your guide when touring our Gateway Gardens assisted living community in Winder, GA. Allow us the privilege to share the entirety of our community with you via guided tour. Our experience is that most of your questions will be answered that very day.
20 January 2025
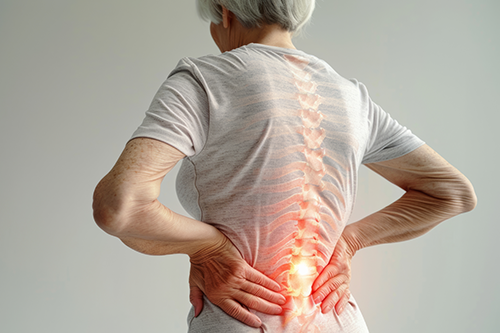
Today’s assisted living and memory care blog post is focused upon Osteoporosis prevention. This blog post is targeted for all of you at-home care givers who lovingly take care of your assisted living and/or memory care loved ones. The guidance we provide to you today comes from decades of professional knowledge and experience supporting both our assisted living and memory care communities.
Osteoporosis prevention is important for everyone but is essential for our seniors. The disease affects around 54 million in the United States alone. It is often referred to as a “silent disease” because it may not come with any symptoms. Many people do not know that they have it until they break a bone.
Having no symptoms doesn’t mean that osteoporosis is harmless. As it progresses, it can be very painful and debilitating. It causes bones to become fragile, making them more likely to break. This can cause mobility issues, deformities, and reduced height. It leads to an overall lower quality of life.
In some cases, fractures caused by osteoporosis can even lead to death due to complications from the injury. Elderly people require more time to heal and have a higher risk of complications that can lead to diminished health or even death.
Senior health and wellness is our top priority here at Gateway Gardens Assisted Living and Memory Care in Winder, GA! We want our residents to thrive and enjoy the highest quality of life possible. That’s why, whether you are a dear resident of ours or not, that it is important for all adults to understand what osteoporosis is and how to prevent it.
Anyone can develop osteoporosis, but some groups are at a higher risk. The biggest factor is gender. While osteoporosis affects around one in 20 men, it affects around one in five women. White and Asian women have an even higher risk.
Women’s elevated risk stems from hormonal changes that occur during menopause. These changes affect bone density. Oestrogen is needed to build strong bones. This hormone decreases after menopause, reducing bone density. Men also have a larger skeleton, which helps them avoid breaks.
Even if you don’t fall into the female demographic, you can still end up with osteoporosis. Your risk may be increased if you:
Our risk increases as we get older. Women will see an increase in loss of bone mass for several years after menopause. By the age of 65 or 70, bone mass loss occurs at around the same rate for both men and women.
Seniors may have osteoporosis and not know it. Many older adults have no idea they have the disease until they have a fall or bump that causes a bone to break. You don’t have to wait until you are injured to check for osteoporosis. The U.S. Prevention Services Task Force recommends that women over age 65 as well as those who have an elevated risk schedule a screening for the disease.
Testing is done using a scan to measure bone density. The patient’s results, which are called a T-score, are compared to those of a healthy young adult. A patient who has low bone density but not low enough to be considered osteoporosis may instead be diagnosed with osteopenia. It is not as serious but should be considered a strong indicator that the patient needs to take steps to prevent osteoporosis.
Having an osteopenia diagnosis doesn’t guarantee that you will get osteoporosis, but it can go that way without making healthy changes.
If you experience a bone break, especially one that seems like the injury shouldn’t have been that bad, speak with your doctor immediately.
Not everyone will have to deal with osteoporosis in their lifetime. There are many factors that you can control, which can help you prevent the disease. You can’t stop aging, but you can live a healthy, active lifestyle. Seniors who want to protect themselves from bone loss should try the following.
Eat Bone-Nourishing Foods
Prevention of many health conditions starts with a healthy diet. Making sure your body has what it needs will help it perform better. Calcium, vitamin D, and protein are essential for your bones.
Women under age 50 should get 1,000 mg of calcium daily. Those over age 51 should increase to 1,200 mg. Adult men should have 1,000 mgs in their daily diet, increasing to 1,200 mg after age 70.
Live an Active Lifestyle
Exercise and diet are equally important for senior wellness. Being active also helps keep bone density high. Find a workout regimen that is ideal for you and suitable based on your mobility and health status.
Remember to consult your doctor before changing your activity levels. They can recommend how to do so safely, and so you get maximum results. Seniors who have trouble with balance or mobility should consider seated exercises.
Maintain an Ideal Body Weight
Keep your body weight at an ideal number based on your height and build. If you aren’t sure where you should be, ask your doctor. Everyone is built differently so one number may work for one person but not for another.
Being underweight can indicate that a person’s nutrition is lacking. They may not be getting the vitamins and minerals they need, like vitamin D and calcium. Those who are overweight can also have problems due to the mechanical load on the skeletal system.
Stop or Avoid Smoking
If you are a smoker, this is the time to stop. If you don’t smoke, make sure you never start. Tobacco use comes with increased health risks – including osteoporosis. Stopping the habit will bring many health benefits. Smoking reduces calcium absorption and lowers vitamin D levels. It can cause hormone changes and lowers body mass. Researchers have also found a connection between smoking and a higher risk of bone fractures and slower healing.
There is no cure for osteoporosis. However, there are things seniors can do to prevent it or slow it if they already have it. The main goal is to live a healthy lifestyle that includes a balanced diet and exercise. Those that already have an osteoporosis diagnosis may be advised to make lifestyle changes to reduce their risk of a bone fracture. They may be prescribed medications that help slow bone loss like calcitonin, bisphosphonates, estrogen, or RANKL blockers. They may also be given drugs that rebuild bone like synthetic parathyroid hormone.
Professional care communities like ours here at Gateway Gardens Assisted Living and Memory Care in Winder, GA help seniors stay healthy by giving them the resources they need to take control of their health and well-being. Stop in anytime. We’d love to discuss this and any other concern you might have for caring for your beloved assisted living or memory care loved one.
13 January 2025

Are you exploring options for memory care communities here in Winder? Establishing a routine is crucial in dementia care, providing stability and comfort for individuals facing cognitive challenges. Routine activities can help navigate dementia symptoms by offering predictability and structure, which are essential in managing daily life effectively.
Navigating dementia requires thoughtful planning and consistency. Establishing a regular schedule for meals, medication, and activities can reduce confusion and anxiety, promoting a sense of security for patients. Memory care facilities often emphasize the importance of routine to enhance the quality of life for residents, fostering a supportive environment where individuals can thrive.
In addition to establishing a regular schedule, providing familiar surroundings and minimizing changes in the environment can significantly help individuals with dementia. We strategically design our spaces to be easy to navigate, with clear signage and familiar objects, which can reduce disorientation and improve comfort.
Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, maintaining a routine helps in managing behavioral symptoms such as agitation and sundowning. Consistent daily patterns can regulate sleep-wake cycles and improve overall well-being. Our caregivers play a crucial role in implementing and maintaining these routines, ensuring that each day follows a familiar and comforting rhythm for their loved ones.
When considering dementia care communities here in Winder, look for those (like ours) that integrate personalized routines into their care plans. Facilities that tailor activities and schedules to meet individual needs can better support residents in maintaining cognitive function and emotional stability. This approach enhances the effectiveness of treatment and promotes a higher quality of life for seniors living with dementia.
Contact us today to discover how our personalized approach can enhance your loved one’s well-being and provide the support they need to thrive.
6 January 2025

Happy New Year and welcome back to our Winder assisted living community blog and our Winder memory care blog. A new year’s resolution to improve physical fitness initiatives is not just for the young. For those dealing with Alzheimer’s, integrating physical activity into daily routines can provide significant advantages. Here’s how regular exercise positively impacts seniors with Alzheimer’s:
Incorporating physical activities into the daily schedule is an integral part of care plans. These activities are tailored to individual needs, ensuring that each resident benefits from a program suited to their abilities and interests.
We understand the profound impact of physical activity on your loved one. Rest assured that an active lifestyle within our Gateway Gardens memory care community is something to not only expect, but to cherish.
Happy New Year to you all. We look forward to bringing you regular recurring topics here that you can both enjoy and put to active use in furthering the loving care of your assisted living and/or memory care loved ones!!!!
2 December 2024

Very warm Holiday greetings from all of us at Gateway Gardens Assisted Living & Memory Care in Winder, GA. To all of our residents within both our senior assisted living community and our memory care community, we trust you’re feeling the love that arrives with the Holiday season. For the non-resident community reading this today, we offer you the same warm Holiday greetings as well.
Tis the season to sit with family and enjoy good wholesome Holiday movies, memories, and other electronic-based love and fellowship. The gentle glow of a screen may seem harmless, but it can deeply affect your loved ones’ sleep. Excessive screen time, especially in the evening, may interfere with seniors’ sleep quality by disrupting the body’s circadian rhythm. This rhythm, which regulates when the body feels awake or sleepy, is essential for quality rest.
For those in their golden years, restful sleep can often become more elusive, and screens—whether television, computer, or smartphone—may contribute to this challenge. The reason lies in blue light, a high-energy light emitted by screens that can delay the release of melatonin, the hormone that signals to the body it is time to sleep.
Blue light exposure before bedtime is known to interfere with melatonin production. Melatonin helps to set the body’s internal clock, signaling it to wind down as evening approaches. Blue light tricks the brain into thinking it is still daytime, leading to delayed sleep onset or more restless nights.
While individuals of all ages can experience this disruption, the impact on those in later years may be more significant, as natural melatonin levels gradually decline with age. This makes quality sleep hygiene all the more crucial, and reducing screen time before bed becomes an effective, simple way to support better sleep.
Creating an evening routine that does not involve screens can make a big difference in supporting sleep quality. A “screen curfew” an hour before bed allows the body’s natural melatonin production to take effect. During this time, try a few calming activities that not only encourage relaxation but also bring enjoyment. Traditional paperbacks, listening to soft music, or spending time with a crossword puzzle are screen-free options that keep the mind active in a soothing way. For those who enjoy community events, a late afternoon walk, or time at a local library, these gentle routines can be a rewarding alternative to evening screen time.
It may take some time to adjust away from screens, but the reward of better rest is worth the transition. Activities like reading a novel, working on a craft, or enjoying a cup of herbal tea while looking through a favorite photo album help signal to the body that it is time to relax. These activities not only support better rest but also offer opportunities for creativity and reflection. Additionally, puzzles, light stretching, or simply gazing at evening views around a well-chosen community can bring both peace and fulfillment. A routine like this makes winding down both enjoyable and beneficial for sleep.
Quality sleep is foundational to a vibrant life and can contribute to improved mood, alertness, and energy throughout the day. Practicing good sleep hygiene by reducing screen time naturally leads to these benefits. With restful sleep, individuals often feel more connected to daily routines, have more energy for activities, and find a deeper sense of calm. For your loved ones, adopting these sleep-enhancing habits is a small change with a large impact, supporting both physical and mental health.
We know how much of a difference a good night’s sleep can make in your loved one’s day. That’s why we focus on creating an environment that encourages relaxation and supports healthy routines. Imagine your loved ones enjoying quiet, screen-free activities like reading a favorite book, solving puzzles, or sipping herbal tea in a calm and inviting space. These simple yet meaningful moments help prepare the mind and body for restful sleep.
At our senior living and memory care community here in Winder, we offer more than just a place to live—we provide a space where well-being is part of daily life. Our team is here to help your loved ones discover enjoyable ways to wind down in the evenings, with activities and surroundings that make rest feel natural and refreshing.
25 November 2024

By now we trust that all of you realize that here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, we invest in managing this senior living and memory care blog as a service to our cherished residents, their families, and to the countless angels out there who lovingly provide self-help at-home senior care services. We feel a heartfelt responsibility to freely share our professional knowledge regarding professional assisted living and memory care support. We are fully aware of the vast weight of the labor of love that all of you bear regardless of the level of professional support that you currently secure.
While this Thanksgiving-related blog post is heavily focused on those of you who care for a loved one with memory care issues, so much of this messaging can be directly applicable to those providing senior assisted living support to someone without memory issues.
Thanksgiving is a time for family and friends to gather to give thanks, catch up and share a special meal together. However, when a family member is diagnosed with dementia, such as Alzheimer’s disease, the family dynamic changes dramatically. Nowhere is this more evident than at holiday gatherings. The hustle and bustle of a typical family Thanksgiving can cause extreme levels of anxiety for someone with dementia, turning a wonderful day into a confusing and agonizing ordeal. Consequently, for the family caregiver, it can become a day full of tension as they watch over their loved one with anxious eyes. It doesn’t have to be that way. With advance planning and preparation, Thanksgiving can still be enjoyed by everyone, even the family members with dementia. To be successful, however, you do need to plan and structure the day for the best possible outcome.
Here are some tips we’ve gathered, contributed by individuals with dementia, families and caregivers:
If your loved one is one of our cherished memory care residents here at Gateway Gardens, you know there is an open invitation to bring your Thanksgiving cheer here to them. For some, especially your and our memory care loved ones, this can be an advantage over disrupting their routine by transporting them to your gathering.
For more information about senior living or memory care services here in Gateway Gardens, contact us anytime.
18 November 2024

Thanksgiving is once again just around the corner. Can you believe it? This is a wonderful time of the year, but as you all know, it tends to be that period in the year when it sometimes feels like life’s task list grows and maybe sometimes, we come to realize that our focus has strayed away from what it most important. Well, our focus is on our beloved residents within our assisted living community and within our memory care community here at Gateway Gardens. Today’s blog is an attempt to offer ideas during these busy times to retain focus on what’s most important to all of us, our family.
The Thanksgiving holiday conjures an assortment of emotions within all of us. For some, this is a time to reflect on loved ones, the living and passed. And, yet, regardless of where Thanksgiving finds each of us this year, it brings an opportunity to pause and give thanks for the simple things we often take for granted. Things like the love of family, food on the table, and even for life itself.
Take due time in advance of the Thanksgiving holiday to reflect upon the things that enrich your soul. Make a list because you might find that your list of things is long. Some things will be obvious. Others, maybe not so much. Strongly consider committing yourself to sharing these thoughts with your loved ones. This is a wonderful time of year to express gratitude to those people in your life who make it so special.
If you are reading this list today as a resident here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, a family member of the same, or simply a member of the public seeking ideas regarding how to make Thanksgiving for your senior or memory care loved ones, know that you already exist within our list of people to be thankful for.
4 November 2024

Let’s be real dear readers of our Gateway Gardens Assisted Living and Memory Care blog. Half of you is going to be disappointed in the results of this year’s presidential election. The other half, likely some cross between relief and celebration. Whichever camp you reside within, you (and your assisted living and/or memory care loved ones) will be deeply rewarded by laughing it off. As it turns out, Reader’s Digest has been right all these years: Laughter is the best medicine!
There are many benefits of laughter on mental and physical health, but here are five we think are most important:
Boosts Mood: Laughter triggers the release of endorphins, the body’s natural feel-good chemicals, which can promote an overall sense of well-being.
Reduces Stress: Laughter decreases the production of stress hormones like cortisol and adrenaline, helping to relax the body and alleviate tension in both the muscles and the mind.
Strengthens Immune System: Regular laughter can increase the production of immune cells and antibodies, thus improving the body’s ability to fight off infections and illnesses.
Improves Cardiovascular Health: Laughter has been shown to improve blood flow and circulation, which can lower blood pressure and reduce the risk of heart disease and stroke.
Boosts Cognitive Function: Laughter can increase oxygen flow to the brain, promoting mental clarity, creativity, and problem-solving abilities.
Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we laugh with our beloved residents every day. Everyone here unanimously agrees that laughter and love is simply the single best unpaid benefit of serving here. Laughter fills our communal spaces, and it is impossible to tell who is doing it for who.
28 October 2024

Welcome back to our Gateway Gardens Assisted Living and Memory Care blog! Every single one of us here at Gateway Gardens exist to enhance the quality of life of the dear residents of our Gateway Gardens assisted living community, our memory care community, their families, and their friends.
Caring for aging parents can be stressful, especially when you include siblings in the mix—the people you’ve grown up with, played with, fought with, and reconciled with. It can be difficult to remember that you’re all adults now with your own thoughts and perspectives, and it often leads to tension.
So, what’s the best way to work together to care for your parents and avoid as much stress as you can?
Working with your siblings to take care of an aging parent is just that: working together. It’s important to be understanding and respectful of each other, to listen to what each person has to say and what they feel and keep everyone up to date about changes in your parents’ lives. It can help to determine a primary caretaker to make important decisions.
If your parents are here with us at Gateway Gardens, it certainly can be therapeutic for everyone to schedule a group visit and spend quality family time together. By focusing on the good things and letting go of more stressful situations, you can help us, help yourselves, and most importantly, help your parents enjoy the very best of their golden years. Being surrounded by direct family and a team of caring individuals like those here at Gateway Gardens Assisted Living and Memory Care means that, with 100% assurance, every moment of your life you can know that your loved one(s) enjoy the loving support they need for a comfortable and fulfilling life.
21 October 2024

Welcome back to our blog page for our Gateway Gardens assisted living and our Gateway Gardens memory care community. As is always the case, one of the most common frequently asked questions this time of year is “what ideas do you have to make this Halloween holiday special for my memory care loved one”? Well, we thought we’d break out another special edition blog post on the subject in hopes that it provides some ideas that you can put into action.
Pumpkins are a staple at Halloween, but instead of carving them we can just decorate the pumpkin and avoid issues with sharp knives. There are so many ways to decorate – painting, using stick-on pieces, wrapping with materials, tights, lace etc., adding features like tinsel hair, drawing on eyes and a mouth etc., or using household items like tin foil to create a personalized pumpkin etc.
Why not make your own trick-or-treat bags and fill them. You can have a lot of fun making them, cheekily sampling the products! Just be careful if your loved one has swallowing/choking issues.
Making your own Halloween decorations can help save money, engage your loved ones, and remove any fear they may have of them. You could even start a conveyor belt for creating decorations where one person takes control of making part of it – like drawing out the shapes, cutting the card, coloring etc. You can make bunting in Halloween colors, paper chains, Halloween cards or simply helping blow up balloons? Whatever your loved one would enjoy!
Take a shot at Halloween themed crafts like pipe stick figures or paintings of pumpkins, using autumn leaves as stencils or creating a collage etc. These can all help those with dementia, seniors, and the elderly activate their brains, help with hand and eye coordination and connect with tactile materials. Why not try getting the paints out, glitter, and tactile materials to make your own Halloween posters together. Or you can simply print off free Halloween coloring pages to color in together.
If your loved one can’t be with you and you want to keep them reassured. Get together on a zoom, facetime, duo, or echo show party and share tales of your past Halloweens or what you used to do as kids. If they are wearing headphones it could help drown out the sounds outside the home. If you don’t want your loved one to be disturbed at home, then you can print out these no trick or treat poster and stick it up on the front door or window.
Get out of the house – go for a walk, collect falling leaves, small branches, anything to target and put your minds to. Just getting out can help and you’ll have collected things u can use to make things later.
We hope you all are enjoying this Fall season and are looking forward to one of the most fun holidays of the year. Of course, you all are invited to come celebrate your loved one’s Halloween celebration here at both our Gateway Gardens assisted living community and our Gateway Gardens Memory Care community. If we don’t see you here, have a great time celebrating at home!
14 October 2024

Our team of professional memory care and assisted living care providers here at Gateway Gardens are there for all of you, young and seasoned alike. Your memory care loved one may periodically (or often) exhibit bouts of sudden and inexplicable anger. Today’s blog offers “food for thought” regarding proven helpful ways that you can react to situations.
If your loved one gets angry or exhibits aggressive behavior, try to de-escalate the situation as much as possible. You can do this in a few ways.
Is your loved one hungry or in pain? Is she confused or in a strange environment? Try to identify what might be causing the outburst and rectify it. Offer a snack or a drink. Take her away from the noise and into a calm room. This can help calm her down and alleviate some of the anger she is feeling.
Just because rational thinking is lost over time for someone with dementia, this does not mean intuitive thinking is lost. Intuitive thinking includes the five senses, core feelings like joy and love, observing others’ feelings and enjoying beauty. Trying to rationalize your loved one out of his anger or frustration will likely lead to further anger or frustration. Instead, focus on the thinking skills they do have. What do they see, taste and smell? How are they feeling? How do they think you’re feeling? This will help them feel competent and capable, rather than confused or embarrassed because they are unable to use rational thinking.
Thoughts for dealing with a loved one’s anger and aggression:
If your loved one is having regular or intense outbursts of anger or aggression, be sure to talk to your healthcare provider. They can provide insight on what to do, if medication is the culprit or other providers who may be able to help.
Anger and aggression can be difficult (seemingly, or impossible) to deal with. We want you to know that loving, effective, and comforting response to dementia-related emotions resides within the core of our professional education and decades of experience. Loving memory care is what we do here at Gateway Gardens Assisted Living and Memory Care. You are never alone.
7 October 2024

Welcome back to Gateway Gardens assisted living blog and our memory care community’s blog. Most of you know that we manage this blog on behalf of our cherished residents, their families, and of course for all homecare heroes taking care of your assisted living and/or memory care loved ones. Today, we’ll discuss a real concern that many of you might not be familiar with: Powers of Attorney.
As a senior, you may at some point be faced with situations when you need assistance with handling your affairs. If you are hospitalized or incapacitated, who will pay your bills and manage your finances? Who will make your healthcare decisions if you can’t? Having a Power of Attorney allows you to make these choices, so it’s important for seniors to include it in the estate planning process.
A Power of Attorney (POA) is a legal document that designates someone to act as an agent to make financial or medical decisions if you are unable to do so. A general POA covers financial and legal decisions, including paying bills, entering contracts, or buying and selling property. A durable POA includes a clause that allows the document to remain active if you become incapacitated. A limited POA limits the agent’s powers to one-time events, such as purchasing a home. A medical POA provides authorization for an agent to make decisions about your healthcare if you can’t do so.
An estate planning attorney can help you create a POA that will protect your interests when you need it most.
It lets you choose who will handle your financial matters.
A durable POA specifies who will handle your financial affairs if you are not able to do so. With a POA, you can choose a close family member or other trusted person to represent your interests. It prevents the need for a guardianship or conservatorship. If you don’t have a POA, a judge will appoint a guardian or conservator to handle your affairs for you, and that person may not make the choices you would prefer. Without a POA, you will have no input in who will fill this role.
It allows you to choose someone to handle your healthcare.
If you are unable to make decisions about your medical care, a medical POA will allow your agent to do so for you. If you don’t have one and there is an emergency that leaves you unable to make those decisions, a stranger may make those decisions for you.
It ensures that your wishes are followed.
The trusted agent you choose with a POA knows what your wishes are and can make sure those wishes are followed. A court-appointed guardian or conservator may not know how you would like certain financial or medical matters handled.
The major drawback of not having a POA is that you won’t have any control over your affairs if you are unable to manage them. This means your court-appointed guardian or conservator could make decisions with which you wouldn’t agree.
Having a POA is an important step in the estate planning process for seniors since it allows you to choose someone to be your voice and make sure your financial and medical affairs are handled according to your wishes.
We hope you found this information helpful. When it is time for you to seek professional assisted living or memory care here in Winder, we’ll help you cover all the bases.
30 September 2024

We want you all to know that our primary mission is to provide a loving, safe, and life-enhancing living experience within our assisted living community and our memory care community. For you at-home dementia and other assisted living care providers, we sincerely hope to assist you via this assisted living and memory care blog. Today, we’re going to offer some ideas regarding useful items that are known to support loving people like you to help others.
“Dementia products” are intended to make life easier for a person with dementia and their loved ones. Some of these products can indeed be helpful. However, often they go unused or hold interest only briefly. Before you jump in and try or buy something, do a little advance thinking. Here are some suggestions to guide you:
Many care partners have found that the following items offer contentment, comfort and/or human connection – all critical needs for individuals living dementia! Many of these you can find in your home, or do not cost a lot to buy.
Photo Albums/Loose photos
If you have more than one photo album, place them in different rooms. A loved one might enjoy looking at or “organizing” loose photos. Looking at photos is a wonderful way to connect with a loved one with dementia. However, try not to quiz your loved one as you look at photos, as that could cause frustration. Instead, simply point out what you see and reminisce.
Scrapbooks of memories or interests
Let’s say the person with dementia used to work in construction, they might enjoy a scrapbook with photos—cut out from magazines or catalogues or downloaded from the Internet—of heavy equipment.
Magazines with subject matter of interest
For example, a car enthusiast might enjoy an auto magazine. See if your neighbors or friends can pass along their magazines when they are finished with them to keep a fresh assortment.
Pieces and parts of a hobby
A former quilter might really enjoy handling a variety of fabric scraps. Or, a loved one who loved to cook might enjoy looking at cookbooks or making a grocery list. The woodworker or tradesman might like to handle or “organize” nuts and bolts into a plastic bin.
Radio or other source of music/entertainment
Because long-term memory persists longer than short-term recall for those with dementia, experiment with music from their childhood, adolescence or young adulthood. If your loved one was a sports enthusiast, they might enjoy listening to a game. If they grew up in an era of radio shows, you can find many of those classics on YouTube.
“Laundry” for folding or housework
If a person is no longer able to fold actual laundry, use old towels or t-shirts. This can be especially useful for someone who kept house or was very organized.
Housework-type items
Items like feather dusters; placemats/napkins on the dining room for setting the table; plastic (non-breakable) dishes in the sink for washing may engage someone with dementia and help them stay involved in day-to-day tasks.
Bird feeders
If you have a bit of yard and a window with a view, a bird feeder might provide entertainment and could be soothing (for you as well!).
Personal care items
There are simple ways to have a positive, sensory and even loving connection with your loved one. Lotion for hand and arm massages; a brush for gently brushing hair; hair elastics/barrettes for hair styling; and nail polish and make-up for nails and face are all items to have on hand that could bring comfort and pleasure – to both of you.
Hopefully, you will find helpful items – from this list or that you have come up with on your own — for comfort, contentment, and connection. Be sure to share your ideas with other care partners! Here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, we encourage everyone to remember to take care of yourselves, which is a foundational requirement for you to be able to take care of others.
23 September 2024

Welcome back to our Gateway Gardens senior assisted living and memory care blog!
Have you ever found yourself worried about the driving abilities of a senior in your life? Maybe they have been caught in too many close calls or minor accidents. Maybe they refuse to give up the independence that comes with driving, even when it’s no longer safe for them to drive.
It can be a tough and uncomfortable conversation to tell a loved one they may not be able to drive anymore. However, if your friend or loved one is putting themselves and others in danger, it’s an important conversation to have.
Below are some warning signs that likely signal that a senior is no longer a safe driver.
History of accidents
First, look at their driving history. Have they recently been in a car accident? Look at their car and check for damage. Are there new dents or large scratches? Ask your loved one about what happened and try to be objective in deciding who was likely at fault.
Slow reaction times are more common in older drivers. If a person can’t remember a driving incident, that can be another indication their cognitive abilities may be hindering their driving.
Attitude shift
Has the senior in your life become reluctant to get behind the wheel? Are they nervous because of a negative experience in the past? If a senior becomes uncomfortable with driving, they may be recognizing their limits or feel like they are at risk when they drive.
Dangerous behaviors
Have they recently received a ticket for a traffic violation? Maybe they were driving too slow or too fast for traffic. Maybe they couldn’t stay in their lane, were distracted by their phone or lost focus. Dangerous behaviors signal that a senior may no longer be a safe driver.
Health problems
As we age, our health issues can start to interfere with our driving ability, as can our medications. Being a safe driver requires adequate vision and hearing, as well as range of motion, flexibility and good reflexes. When considering the safety of a senior driver, ask yourself:
Perhaps the senior in your life lacks one of these qualifications, or they have admitted to you that they do. If that’s the case, they need to be able to address their health concerns before continuing to drive.
If you want to check whether an aging loved one is safe to be on the road, you likely have several options. Keep in mind, however, that every state is different when it comes to laws about elderly drivers.
A quick solution may be to take a ride with the senior and see for yourself how they drive. Take note of whether they follow the rules of the road or not, and whether you feel safe with their driving. You could also encourage them to make a self-assessment of their driving skills.
Offer to tag along the next time the senior in your life needs to visit the doctor. Tell their doctor or physician your concerns and ask whether they need a vision or hearing check. In fact, many states already have additional requirements for adults aged 65 and older to renew their license, including retaking vision and driving tests.
Visiting a doctor is especially important for those who may be experiencing memory loss. A person with Alzheimer’s disease or dementia should not be driving. If cognitive impairment may be present, the driver should stay off the road until they have been seen by a doctor.
If you feel like you need the help of a driving expert, consider hiring someone to do a driving evaluation. This could be a certified driver rehabilitation specialist (CDRS), who is usually a qualified driving instructor or an occupational therapist. These instructors will do a thorough evaluation to determine if the senior you may be worried about is a safe driver. After the evaluation, the instructor will inform you if the senior should not drive anymore or can still drive, perhaps with modifications.
Check out our Gateway Gardens assisted living community or memory care community to determine if we may be a good fit for your loved one. You can also contact us here at Manor Lake or request more information.
16 September 2024

Welcome back to our blog page for our Gateway Gardens assisted living and our Gateway Gardens memory care community. You know that all of us here at Gateway Gardens are professional caregivers, but we don’t expect our blog readers to think much about the fact that many of us are just like you, supporting our aging parents at home. We are blessed to be surrounded by a volume of those not only in the same boat, and by professional association, are card-carrying members of the “at home senior care fraternity”. We hope you find today’s blog post to be both informative and actionable guidance for your senior care journey.
Every person has different concerns as they age, and as an adult child of an aging parent, you want your loved one to enjoy a good quality of life—no matter the situation. Even if your parent still lives independently, it’s never too early to make a plan to support your aging parent.
Many adult children and older parents wait until an emergency or crisis happens before they talk about support needs. But the small, early signs that your loved one needs additional support may already be there. Take note of changes in health, ability to do daily tasks, feelings of isolation, or differences in behavior. It’s important to stay tuned in to any changes that merit more support.
To help you feel more prepared, use these steps to address the big concerns and make a plan together for long-term care and well-being.
As providers of professional assisted living services or professional memory care services, we are your biggest fans. We know your challenges, your frustrations, and of course the comfort and rewards for the loving care that you provide. May strength, patience, and happiness find you all!
9 September 2024

We have not authored a “fall focused” senior living and memory care blog post since September of 2022. The risk of injury to our assisted living and memory care seniors increases in the fall and winter season. So, let’s revisit the topic in the interest of getting everyone focused upon the safety and welfare of our loved ones. Before we go on, realize that for any assisted living or memory care-related question, know that we offer both senior assisted living services, memory care support services, and that we gladly share our wealth of experience and advice to all of you reading this. OK, now on to senior fall risks and how to prevent them.
According to the CDC, 33% of adults age 65 or older will experience a fall this year. For older adults, falls can cause very serious injuries like head trauma, internal bleeding, or hip fractures. These slips or tumbles are the leading cause for fatal and nonfatal injuries in older adults. Even though a third of older adults experience a fall, less than half of those people will consult their primary care provider about it.
There are a few ways to minimize the risk of falls and fall-related injuries. What is most important is talking to your primary care provider to review your current medications as well as health conditions that may be affecting your balance or coordination.
Wear shoes that are comfortable as well as easy to walk in. They should be the proper size for your feet and should include non-slip tread on the bottom. High heels, loose sandals, or shoes with little or no tread are dangerous footwear options. Shoes that are laced up with nonskid soles are recommended to avoid falling.
Exercising regularly will help sustain and improve reflexes and balance. Swimming or walking in a pool is another activity that is easy on the joints but also helps improve leg strength.
Some ear and eye conditions can increase the possibility of a person experiencing a fall. Make note of any dizziness or pain you feel when you are walking as well as any numbness or shortness of breath. These details will help you and your doctor create a plan of prevention.
Since most falls occur at home, preventing in home falls is one of the most crucial parts of fall prevention. Hazardous furniture, rugs or other items around your home can cause a trip or fall. Be sure to remove or properly secure objects such as boxes, space rugs, electrical cords, and phone cords from high traffic areas. Furniture that is close to the ground such as coffee tables, nightstands, or plant stands can cause one to fall. Your bathroom should utilize assistance devices such as hand bars in the shower or tub as well as a seat with arm rests on the toilet. This will make getting in and out of the bathroom much easier. Putting a properly secured bathroom tile rug as well as a bathmat within the tub or shower is critically important.
Make sure that your bed is not too low or too high on the ground to avoid falling out of bed or experiencing trouble getting up. Couches and lounge chairs should also not be too close to the ground, as this may be a hazard when you get up. Install handrails for both sides of the staircase in your home, if needed, and keep your staircase illuminated at night.
At Gateway Gardens Assisted Living & Memory Care in Winder, GA, we know caring for a senior loved one brings joys and challenges. Our mission is to change the way the world ages. We provide seniors with quality care that enables them to live happier and healthier lives. Our services are distinguished by the caliber of our caregivers, the responsiveness of our staff and our expertise in Live-In care. We embrace a positive, balanced approach to aging centered on the evolving needs of older adults. For more information, contact us here at Gateway Gardens anytime!
26 August 2024

Hello and welcome back to our Gateway Gardens Assisted Living & Memory Care blog. Today we turn our focus to the upcoming Labor Day weekend and how all of you providing assisted living care and/or memory care support services to a loved one.
We take this moment to remind all you at-home caregivers that if you're going to be an effective caregiver. taking care of yourself is not a luxury. It is an absolute necessity. Did you know that the original intent behind creating this federal holiday was to honor the contributions that workers have made to the strength, prosperity, laws, and well-being of the country. And who are the often-overlooked workers that need to be included in the celebrations this year? Caregivers of aging parents.
As someone caring for elderly parents, you can’t ever really take a day off...or can you? Here are some reasons why you should consider taking a break this Labor Day:
When you are caring for elderly parents on a regular basis, you run the risk of developing caregiver burnout if you don’t take time to recharge your batteries from time to time. Burnout can manifest itself in different ways, according to WebMd, including:
Caregiver burnout affects both your physical and emotional health and can even lead to strained relationships with a spouse or close friends. But there is hope: caregiver burnout can be prevented by creating boundaries and carving out more time for yourself.
Self-care for caregivers is so important for your ability to care for aging parents over an extended period of time. Indulging in some “me-time,” whether that’s a long weekend at a bed and breakfast, a quiet hour to read a book, a commitment to exercising regularly or even just a warm bath at the end of a long day can help preserve your mental and emotional health when caring for elderly parents.
All of us here at Gateway Gardens Assisted Living & Memory Care in Winder, GA do everything we can to make sure all seniors and their families feel comfortable, happy, and at ease as a cherished member of our community.
12 August 2024

Welcome back to our Gateway Gardens assisted living and memory care blog! We exist to enhance the quality of life of our assisted living residents, our memory care residents, their families, and their friends.
In an era marked by the swift evolution of technology, voice technology shines brightly as a beacon of accessibility and convenience, particularly for seniors. As traditional interfaces become increasingly complex and daunting, voice-enabled devices offer a refreshing alternative, eliminating barriers to engagement and empowering seniors to navigate the digital landscape with ease. Today, our goal is to help you learn more about voice technology, dissecting the top devices and how they benefit seniors.
Voice technology revolutionizes the way we interact with our digital environment, offering a hands-free and intuitive experience that transcends traditional interfaces. From virtual assistants such as Amazon Alexa and Google Assistant, which have become household staples, to specialized devices meticulously crafted to meet the unique needs of seniors, the spectrum of voice-enabled solutions is as vast as it is versatile. Whether it's facilitating everyday tasks, fostering social connectivity, or enhancing accessibility, voice technology caters to a diverse range of needs and preferences, empowering individuals to navigate their digital world with unparalleled ease and efficiency.
Promotes Independence
Voice-enabled devices empower seniors to perform daily tasks independently, enhancing their sense of autonomy and self-confidence. Whether it’s setting medication reminders or accessing relevant information, voice technology eliminates barriers and fosters self-reliance.
Enhances Social Connectivity
For seniors, social isolation can pose significant challenges to their well-being. Voice technology serves as a conduit for connection, enabling seamless communication with loved ones and fellow residents. Through virtual chats, interactive games, and shared experiences, seniors can cultivate meaningful relationships and combat feelings of loneliness.
Improves Safety and Security
With features like voice-activated emergency alerts and home monitoring, voice technology prioritizes seniors' safety and peace of mind. In the event of a fall or medical emergency, prompt assistance is just a voice command away, ensuring timely intervention and support.
Stimulates Cognitive Function
Engaging with voice-enabled devices stimulates cognitive function and mental acuity among seniors. From trivia games to brain teasers, interactive content promotes brain health and enhances memory retention.
Facilitates Access to Information
Voice technology serves as a gateway to a wealth of information, empowering seniors to stay informed and engaged. Whether it’s checking the weather forecast or listening to audiobooks, voice-activated assistants provide instant access to relevant content, keeping seniors abreast of current events and trends.
Amazon Echo: As a pioneer in voice technology, Amazon Echo stands out for its versatility and user-friendly interface. With simple voice commands, seniors can play music, set reminders, control smart home devices, and even make hands-free calls.
Google Nest Hub: Google Nest Hub combines the functionality of a smart speaker with a vibrant touchscreen display, making it an ideal companion for seniors. From viewing family photos to accessing step-by-step recipes, the visual interface enhances the user experience, catering to individuals with varying levels of tech proficiency.
GrandPad: Designed specifically for seniors, GrandPad offers a simplified interface tailored to their needs. With large icons and intuitive navigation, seniors can easily make video calls, send voice emails, and browse curated content without the complexities of traditional devices.
Once your senior loved one gets tuned into voice technology, they’ll soon be able to teach you a thing or two about it. Wouldn’t that be something to celebrate?
All the best from the loving staff here at Gateway Gardens Assisted Living, and our Memory Care Community!
5 August 2024

Many people erroneously believe that assisted living communities are living options only for those who have reached the point where they physical or medical support to lead a healthy life. While this is true, many other benefits come with moving into an assisted living home. Let’s review three lesser-known benefits.
One of the most significant benefits of assisted living is that they tend to have much more free time to pursue hobbies and recreational activities or spend time with friends and family. This is because many of their daily tasks and chores are taken care of by our staff here at Gateway Gardens. Tedious chores like cooking and housework become a thing of the past. Our residents enjoy plenty of time to get back to old hobbies that they may not have had the time or energy to pursue or discover new passions they’ve always wanted to try but never been able to.
Another excellent way that assisted living communities can improve residents’ quality of life is the increased opportunities to socialize. Many seniors only see their medical caregivers and family when they have a few moments to stop by. In Gateway Gardens Assisted Living & Memory Care in Winder, GA, there is always something going on or someone to visit with, so residents feel less lonely and can make new friends during their golden years.
We provide varied, nutritious meals that ensure our residents remain healthy and happy. While this may seem like a more medical advantage, the mental and spiritual boost that comes with eating good food (especially when you don’t have to prepare it!) cannot be denied.
If you’d like to learn more about Gateway Gardens assisted living or Gateway Gardens Memory Care services, we are ready to help. Call us today!
31 July 2024

Welcome back to our Gateway Gardens senior assisted living and memory care blog! Our goal today is to have every reader reconsider the effects of extreme weather upon our Winder area memory care loved ones. August is here, and extreme heat is a real threat to all of us.
Changes in the weather can greatly impact someone living with dementia. The elderly become vulnerable when it comes to extreme weather changes. Brain function can slow down, and it becomes difficult to regulate body temperature. In this blog, we want to help make you aware of how individuals living with dementia may feel when it comes to warm or cold weather!
A person with dementia may not understand how to dress for weather changes. There are effects of hot weather on people with dementia that they may not understand. Deaths of the elderly during heat waves have been caused by heart failure.
Dehydration can occur in dementia patients because they may not be able to recognize when they're thirsty. They don't remember they need to drink more fluids to prevent dehydration. If dehydration does occur, it can leave toxins in the bloodstream. This causes the kidneys and liver to work overtime. When these organs work overtime, it can cause the urinary tract to become exposed to infections.
Heatstroke can happen if the senior has problems with their circulation and takes medications. This combination can cause the person to not being able to sweat so the body can cool itself off. If the body can't cool itself, then heatstroke can occur.
To prevent overexposure to heat, make sure your loved ones are drinking plenty of fluids to stay hydrated. Avoid drinks with caffeine or sugar, these only lead to even more dehydration and more frequent urination.
Proper ventilation is also going to be a key part of keeping the elderly cool. Make sure air conditioners are working properly before the heat comes. Be sure to check on individuals with dementia to make sure they aren’t showing signs of heatstroke. A few symptoms could be nausea, headache, dizziness, or disorientation. If signs of heatstroke are present be sure to try putting a wet cloth on the back of a person’s neck will help to regulate body temperature. Also, a lukewarm shower or bath will help to lower body temperature.
File this away for a few weeks from now, but important considerations right now none the less. Cold weather can cause a person with dementia to become agitated, depressed, or distressed. If the person has sundowners, the new lack of sunlight can exacerbate it. Sundowning occurs at the end of the day and shows in acts of anger, irradiation, and aggression when the sun starts to set. With the long nights of winter, the behavior of a person with sundowners can become more difficult to deal with.
A person with dementia can start to have sleep disturbances. This happens because dementia interferes with the part of the brain which controls the internal body clock. When it starts to get dark early, it can cause confusion. They may want to go to bed at 5 pm but then will be awake during the middle of the night.
Because dementia can cause visuospatial problems, shadows, and dim lights can cause even more confusion and disorientation. A person with dementia may think they see a person or object which isn’t there. This can cause the person to become even more agitated.
A person with dementia should go outside, under supervision, whenever possible in the natural light. It will boost their mood and help reduce tension and stress. Plus, as the natural light fades, be sure the rooms in the house are brightly lit to control shadows and reflections.
Whatever room the person spends the most time in, keep it calm and relaxing during the late afternoon and into the early evening. Try to keep the evenings soothing and low-key.
Being a caregiver to a loved one with dementia is a full-time job. If you need assistance, Gateway Gardens can be the perfect place to call home. Contact us, anytime, for any reason!
24 July 2024

Greetings once again to our dear residents and family members of our Gateway Gardens assisted living community and our Gateway Gardens memory care community. Let’s get the obvious out of the way right up front. It is a primary goal of every employee of Gateway Gardens to be viewed by our residents as their “extended family”. We long to be viewed and accepted as loving, caring, and skilled friends that can never approximate the blessings of true family. We humbly submit that we are quite successful in that endeavor. With that said, today’s blog post is focused upon the importance of you, the blood relative, to the health and wellness of your (and our) beloved senior and memory care residents.
The bonds of family can be strong and enduring. For seniors and memory care loved ones, these connections serve as lifelines providing comfort, companionship, and an invaluable sense of belonging as they navigate the golden years of their lives. As society progresses and modern lifestyles lead to geographic dispersion and busy schedules, it's crucial to recognize and cherish the significance of family ties, particularly for our aging loved ones.
From infancy to old age, human beings crave connection. For seniors who may grapple with feelings of loneliness or isolation due to factors such as retirement, loss of a spouse, cognitive changes, or physical limitations, the presence of family members can be a powerful source of emotional support. Studies consistently highlight the correlation between strong family relationships and improved mental health outcomes for older adults. In instances where blood family is few and/or far away, the importance of loving professional like us here at Gateway Gardens Assisted Living & Memory Care in Winder, GA deliver play a vital role in overall health and wellness.
The simple act of spending time together—whether sharing meals, engaging in conversation, or participating in leisure activities—can uplift spirits and foster a sense of fulfillment. Knowing that loved ones are there to listen, empathize, and offer encouragement can mitigate feelings of depression and anxiety, promoting overall well-being.
The family bond provides support, comfort, and connection for seniors navigating this new chapter of life. Family members play a pivotal role in enhancing their senior’s quality of life by fostering emotional support, advocating for them, enriching their social connections, and preserving family traditions.
As we recognize the importance of family bonds for seniors, it's essential to cultivate collaborative partnerships between families, seniors, and the loving staff here at Gateway Gardens. By working together to create a nurturing and inclusive environment that honors the unique needs and preferences of each individual, we ensure that seniors thrive and flourish, surrounded by the love and support of their families.
To learn more about the beauty of assisted living and memory care live here in Winder, contact us anytime!
10 July 2024

Although professional assisted living is often a great choice for aging adults who need some help day-to-day, professional memory care is more suited for those with a diagnosis of Alzheimer’s disease or dementia. This is because they provide a more structured environment as well as specially trained staff and engaging activities tailored specifically to meet the needs of those living with the condition.
When your loved one receives a diagnosis of dementia, you’re faced with a lot of questions and considerations. Know that you are not alone, and neither is your loved one. In fact, more than six million adults are currently living with the disease. And that figure doesn’t include individuals living with other types of dementia, or their affected family members.
All types of dementia cause some challenges for the person living with the condition as well as their loved ones. One challenge to be aware of with dementia is its unpredictability. Dementia is a progressive condition, so day-to-day capabilities will constantly shift, which can make it difficult for family members to help. Once a loved one thinks they’ve reached a “new normal,” things shift again.
This inevitability means that future planning is especially crucial for maintaining their well-being and safety. You want to have steps in place for keeping your loved one safe regardless of their condition’s status or progress.
Specialized memory care communities like ours here at Gateway Gardens Assisted Living and Memory Care deliver comforting reassurance for family members, along with personalized assistance that keeps parents or loved ones healthy and independent. An early transition to memory care can decrease the risk of transfer trauma and make the overall experience much more therapeutic for your loved one.
If you are new to our senior living space, you might assume that all communities offer dementia assistance. Although seniors with dementia are often represented in assisted living, it’s important to make sure the community you choose provides skilled memory care like ours, if that’s what your loved one requires.
We offer various levels of care, from those who need very little assistance day-to-day to those who require regular help with activities of daily living (ADLs), such as grooming or dressing. Their programming is typically more general than the tailored care plans and events offered at our memory care community.
On the other hand, our memory care community is specially designed to provide the best environment, care, and interactions for those living with dementia. Although assisted living is an excellent solution for residents who need some assistance with daily tasks, memory care increases the quality of care for these residents through:
These three essential elements of community living are what make Gateway Gardens Memory Care an unmatched option for those with dementia. Here’s why:
Structured Environment
Our memory care community is equipped to ensure resident safety while still giving easy access to the outdoors and community spaces. Because wandering—or walking without a purpose or destination—is a common side effect of dementia, we have open spaces where residents can stroll, but they also have secured entrances and exits, ensuring residents are adequately supervised. Those within our assisted living community are afforded more independence when it comes to solo travel.
Beyond safety, the most important aspect of our memory care community is that it is designed to feel just like home. It’s common to see residents interacting in our shared living spaces, including the activity room and family-style dining room. Hallways are well-lit to decrease the risk of falling. And like home, residents also enjoy easy access to outdoor areas like our courtyard.
Specially Trained Staff Members
Living in a community that offers memory care also provides access to specialized teams of caregivers and other staff. Our memory care community employ caregivers and other team members who are specially trained in dementia conditions and processes. They are equipped with the professional know-how to create personalized interventions that build trust as well as meaningful moments.
Engaging Activities
Another important part of living within our memory care community is attention to engagement. We feature a robust calendar of events, activities, and trips that are designed to increase overall wellness—and offer some well-deserved fun.
Seniors with dementia who live at home alone or with a caregiver are at an increased risk of isolation. Not having that element of engaging in social support can lead to a variety of health concerns, including more rapid cognitive decline. We deliver hubs of activity, making connecting with staff members or fellow residents as easy as stepping out into the hallway or attending the next social event.
Finally, in between group activities, residents living in our memory care community enjoy the opportunity to take part in activities that match their daily routine or rhythm. It’s not unusual to see a resident chatting with a caregiver while folding towels in the living room or a resident helping to set the table. These daily rhythm tasks help to maintain healthy sleep patterns, decrease anxiety caused by confusion, and increase feelings of belonging.
If your parent or loved one has been diagnosed with Alzheimer’s Disease or dementia, a memory care community like ours here at Gateway Gardens offers the support and stability they need to lead a pleasant and productive lifestyle. In contrast, our assisted living community is better suited for those who may need help with some ADLs, but are otherwise safe to go about their days unsupervised.
We’d be honored to discuss things in detail with you. Contact us anytime!
26 June 2024

We pride ourselves here at Gateway Gardens Assisted Living & Memory Care in Winder, GA for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Winder who lovingly provide at-home assisted living care and/or memory care support to your loved ones. Today we’re going to discuss a very important topic related to the extreme heat that is currently blanketing our nation.
Older Adults are more vulnerable to heat stress because they do not adjust as well as younger people to sudden changes in temperature. They are more likely to have a chronic medical condition that changes normal body responses to heat or to be taking prescription medicines that affect the body’s ability to control its temperature or sweat.
Exposure to high temperatures can increase the risk of dehydration, heat exhaustion, and heat stroke. These heat-related illnesses can be dangerous or life-threatening. We offer some basic things to seriously consider regarding the safety of your assisted living and/or memory care for loved ones at home.
Keep an eye on weather forecasts and heat advisories so you know when extreme heat is coming and how long it will last. Drink more water than usual throughout the day and wear loose-fitting, lightweight clothing.
Heat exhaustion signs include heavy sweating, weakness, dizziness, nausea, and headache. Heat stroke symptoms include a fever of 103 degrees F or higher, confusion, and loss of consciousness. If you are suffering from heat stroke, seek medical attention immediately.
Let’s take care of each other and keep each other safe. Make sure to have access to a working phone – a landline can be helpful during a power outage – and keep an emergency contract list close by.
Know where your local cooling center is located and where to find transportation. Set your A/C to 75—80 degrees F. If air conditioning isn’t available, visit spaces with air-conditioning, like a cooling center, library, community center or shopping center.
Talk to your healthcare provider or pharmacist to see if any of your medications affect your body’s ability to regulate temperature.
Avoid being outside in the direct heat for a long time, especially when the sun’s rays are the strongest (between 10:00am and 4pm). Avoid alcohol and caffeine as those beverages can dehydrate you further.
If you’re unable to travel to or find an air-conditioned space, consider the following at home:
All of us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA carry our deepest respect and best wishes for all of you providing your loved ones with assisted living and/or memory care services there at home. We manage this assisted living and memory care blog in the trust that is serves all of you at-home caregivers to provide efficient and improved care services while simultaneously lowering the known burden that comes with your selfless care endeavors.
19 June 2024

By now, most of you know that our sole reason for existence here at Gateway Gardens Assisted Living and Memory Care in Winder, GA is to provide a loving, safe, and life-enhancing living experience to our assisted living community and our memory care community. Through our assisted living and memory care blog, we also seek to support and educate at-home care providers and the general public. Today, let talk about the very real scourge of elder abuse.
Did you know that each year thousands of individuals aged 60+ experience abuse? If you find yourself shaking your head, you are not alone. Many Americans simply have no idea as to the extent of elder abuse occurring on a day-to-day basis.
Here at Gateway Gardens, we are keenly in tune with the importance of keeping our elderly population safe. We believe that protecting our elders, especially those who are cognitively impaired, require an educated American culture that recognizes the signs of elder abuse and are willing to act upon their observation. So, what do you need to know?
First, it is important to understand that elder abuse is not always physical. The National Institute on Aging identifies several ways in which an older individual’s wellbeing can be compromised:
As hard as it is to learn about these horrific abuses, it is important to be aware of them. Most of us have an older relative or know someone who is reliant upon others for assistance and guidance. And we, too, may eventually have the same needs.
If you witness physical elder abuse, call 911. If you have a suspicion of abuse, you should report it to the National Center on Elderly Abuse. The generations of amazing individuals who have come before us deserve respect and dignity. They raised families, had skills and interests, and worked hard to make the world a better place for their children and grandchildren.
So, in addition to celebrating their lives we owe it to them to keep them safe and protected and to help ensure that they can continue to live their best lives, full of peace and joy.
Here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, we encourage everyone to keep their eyes and ears open to the signs of elder abuse and have the courage to report any observed or suspicion that you might have. Our beloved seniors deserve nothing less.
12 June 2024

The golden years are a time for seniors to enjoy life to the fullest. These years should be relaxing and hassle-free, with more time to explore new passions and make new friendships. To achieve this, it’s important to prioritize mental and emotional wellness. Staying healthy – physically, mentally, and emotionally – will help make your golden years truly glow.
At Gateway Gardens Assisted Living and Memory Care in Winder, GA, the premier choice for assisted living and memory care services, we empower residents to embark on a new stage of life. We offer state-of-the-art care services and with luxurious, resort-style amenities to ensure that our residents lead fulfilling and vibrant lives.
In this latest contribution within our assisted living and memory care blog, we’ll explore tips to prioritize mental and emotional wellness and how our community fosters well-being among our seniors.
Remaining social helps combat isolation and loneliness, as well as exercises the brain and contributes to higher self-esteem. Maintain close relationships with family and friends by inviting them to visit your senior living community and introduce yourself to your new neighbors.
Our social activities and group outings make it easy to make new friends. We offer a variety of community events, both on and off-site, to keep our residents engaged and allow them to pursue cherished hobbies and explore new passions.
Physical activity is essential for mental and emotional well-being. Engage in gentle exercises like walking, yoga, or tai chi to improve mood and reduce stress. Yoga and tai chi are especially helpful for practicing mindfulness and meditation, which can reduce stress and anxiety.
Fuel your body, fuel your mind. Maintaining a nutritionally balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help prevent a number of health complications as well as make you feel energized and alert. Within both our senior living and memory care communities, residents receive three strategic nutritionally-balanced meals per day. Our dining options are inspired by registered dieticians to ensure that meals are not only nutritious, but delicious.
Establishing a bedtime routine can promote better quality sleep, leaving you feeling clearer, more focused, and more engaged throughout the day. Settle down with a relaxing and screen-free activity, such as reading a book or listening to music, and aim for seven to nine hours of sleep per night.
Making sure you have a warm and inviting environment is a key part of getting restful sleep. We offer several floorplan options to suit your needs with plenty of room in each to get comfortable.
Continue to stimulate the mind through lifelong learning. Read consistently, take up a new hobby, or explore courses that interest you. We provide a number of educational opportunities for residents to explore interests and test new skills.
We are dedicated to prioritizing the mental and emotional wellness of our seniors. Come and experience the Gateway Gardens Assisted Living and Memory Care difference – where every day is an opportunity for seniors to glow and thrive.
5 June 2024

Welcome back to our Gateway Gardens senior living and memory care blog. At first, someone with Alzheimer's disease may notice mild confusion and difficulty remembering. Eventually, people with the disease may even forget important people in their lives and undergo dramatic personality changes.
Alzheimer's disease is the most common cause of dementia — a group of brain disorders that cause the loss of intellectual and social skills. In Alzheimer's disease, the brain cells degenerate and die, causing a steady decline in memory and mental function.
Current Alzheimer's disease medications and management strategies may temporarily improve symptoms. This can sometimes help people with Alzheimer's disease maximize function and maintain independence for a little while longer. But because there's no cure for Alzheimer's disease, it's important to seek supportive services and tap into your support network as early as possible.
Gateway Gardens Assisted Living and Memory Care in Winder, GA is here to help families with caregiving for loved ones living with Alzheimer’s disease or dementia. To learn about our memory care services here in Gateway Gardens, browse our website, take a drive through our senior living and memory care blog, and know we celebrate your reaching out to us to learn more!
29 May 2024

One of the greatest benefits of an assisted living community is right there in its name – a community. However, the perks of living in Gateway Gardens assisted living community or Gateway Gardens memory care community go far beyond the welcoming, social aspects. Convenience, compassion, and connection are just some of the benefits you’ll enjoy when making the move. Here are four benefits that are real & significant when making the move to assisted living.
As we age, the responsibilities of homeownership tend to become even more difficult and demanding, to the point where your life can feel like one big chore. At a senior living community like ours here in Gateway Gardens Assisted Living and Memory Care in Winder, GA, you’ll enjoy all the benefits of independence, like a private apartment home and your own schedule, without drawbacks like deep cleaning and landscaping. You won’t even have to cook for yourself!
Living alone as an older adult can worry your loved ones, and even if you aren’t suffering from any significant health risks, sudden illness or injury can strike at any time. If your family members live far away or lead busy lives, it can be difficult to find a supportive caregiver in these instances. When you choose an assisted living community like ours, you and your loved ones can rest easy knowing that you’ll be surrounded by staff trained to deal with health problems, accidents, and other unforeseen incidents.
Post-retirement living can present several challenges to older adults, especially those living alone. One of these is plain and simple – loneliness. An assisted living community provides a veritable neighborhood full of like-minded individuals to spend time with as well as friendly staff and various social activities, such as movie nights, musical entertainment, guest speakers, book and card clubs, and travel outings to local fun spots.
Our assisted living community features excellent dining programs headed by professional culinary team, offering strategically healthy and enjoyable dining experience. It’s hard to beat such an impeccably crafted balanced diet, especially when you’re cooking for yourself every day.
We could go on but thought we’d keep things short today. With that said, if you’d like to drop in (or call) for a much longer discussion of the topic, we stand ready, able, and in fact excited at the notion. Contact us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, anytime!
15 May 2024

Welcome back to our Gateway Gardens senior assisted living and memory care blog! According to the Centers for Disease Control and Prevention (CDC), loneliness and isolation are connected to low levels of activity. And here’s the thing to know about inactivity. The hardest part is…..simply getting started. Sir Isaac Newton nailed it when he discovered that “an object at rest tends to stay at rest”. So, let’s get moving…. it’s summer!
We all love the sunshine and the carefree feeling that summer brings. It’s always a great time to get together and celebrate life’s special moments, whether it be Father’s Day (just a few weeks away!), the Fourth of July, or just a simple weekend cookout.
For some, however, the summer can pose challenges, as the heat and humidity make it difficult to enjoy time outside and may even pose a health risk to some vulnerable groups. For that reason, some people find it difficult to enjoy the activities that they love once the hot weather sets in. But fear not! There are plenty of ways for seniors to stay active and social without spending too much time in the heat. Keep reading to learn more about the activities you can do this summer!
Here at Gateway Gardens Assisted Living and Memory Care in Winder, GA, we’re always looking to find ways for our residents to express their creativity, and arts and crafts classes prove to be the perfect place to do it. Whether it’s knitting or making a holiday-themed trinket, there’s always an arts and crafts activity going on at our community! These social crafts take place in a social setting where seniors can make friends and share tips with one another, learning new ways to express themselves. It’s a great way to come together over a common interest, forming new bonds along the way!
Some folks just love competition, and within both our Gateway Gardens assisted living community and our Gateway Gardens memory care community, we’re all for that! That’s why we’ve created ways in which our residents can let that competitive spirit show while having fun in the process. By playing indoor games, residents can enjoy the thrill of competition while making new friends and memories, all while staying cool. We encourage game play for everyone, no matter their skill level or activity level. It’s our goal to create an inclusive, vibrant environment that everyone can enjoy!
Socialization is the key to preventing isolation and loneliness in senior citizens. Here at Gateway Gardens Assisted Living & Memory Care in Winder, GA, we encourage all our dear residents to actively socialize. It warms us all to witness how active our residents’ families are in helping their loved ones adapt and meet new people. We’d love to meet you. Stop in anytime!
8 May 2024

Welcome back to our Gateway Gardens assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home whether you provide senior assisted living services or memory care services to your loved one. Today’s blog topic is a focus upon those of you lovingly caring for your loved one with memory issues.
Communicating with a loved one who has memory loss can be challenging in several ways. Those with memory loss often ask questions that are difficult to answer. Certain sights, sounds, and smells can trigger memories, and they may ask about people or events that have long passed. According to a report by the Mental Health Foundation, those with dementia may ask these questions because they are experiencing time-shifts, delusions, and even hallucinations. When your loved one asks difficult-to-answer questions, consider using some of the following tips to be clear and comforting in your response.
Your loved-one’s nonverbal cues can deliver insight into how to respond most appropriately. If your loved one is clearly agitated or upset when they ask a question, a gentle, comforting touch, and a pause before you respond can often bring them back to a comforted state. If the questioner is smiling and seems wistful, a knowing smile back can make them feel validated even if they aren’t making much sense. Your loved one will remember your own non-verbal cues better than your words.
Most experts agree that when someone with memory loss asks a question where the answer could cause distress, honest answers may not be the way to go. If your loved one asks when their spouse will arrive, and you respond that their spouse is dead, they can experience the pain of loss as if it had just happened. Often these kinds of questions come up repeatedly and so the pain of hearing the truth is frequent. If telling a lie is uncomfortable to you, try skirting the issue instead. “Dad isn’t coming today, mom,” may be all that needs to be said.
Since everyone’s personality is different, and everyone’s memory loss experience is different, you may need to try different tactics to see which one works best for your loved one. Changing the subject outright might be annoying or insulting to one person and a perfect solution for another. The most important thing to do when confronted with difficult and awkward questions from your loved one with dementia is to remain calm and show empathy.
If your senior loved one is receiving care in our Gateway Gardens memory care community, you already know that we are professionally trained and lovingly apply a wide range of proven techniques that maximize comfort to your memory challenged loved one. It’s a critically important benefit that professional memory care experts deliver to you and your challenged loved ones.
24 April 2024

Although moving yourself or a loved one from your home into an assisted living community or a memory care community can be an emotional and overwhelming life change, it is also a chance for a new start. This is your chance to create a warm, welcoming environment that feels like home.
Your new senior living space should reflect your (or your loved one’s) personality. It should offer comfort and provide a sense of familiarity. With a few thoughtful touches and creativity, you can transform your senior living apartment into a place you love.
Retirement is the perfect time to try something new, whether it’s the latest design trend or something you’ve always wanted to try but couldn’t. When raising a family, we tend to decorate for function and sensibility to accommodate growing kids and busy lifestyles. Shy of bringing a drum set into your new apartment, you should take control of how you use your space. Have fun!
When moving into a new space, bringing along your most loved and treasured belongings is essential for creating a sense of comfort and familiarity. Surrounding yourself with cherished items such as family photographs, favorite artwork, family heirlooms, and antiques will help you acclimate to your new surroundings.
These personal items will infuse your senior living apartment with special memories and make it feel more like home.
A well-organized living space promotes efficiency and creates a calming and comfortable home. Donate, throw away, or pass down unwanted items to family and friends. Take only the things you truly need and love.
Invest in innovative storage solutions such as bins, baskets, shelves, and tables with hidden storage space to keep your belongings organized and easily accessible. You'll create a more peaceful and functional living space by eliminating clutter and having a designated area for everything.
Comfort is critical when making a senior living apartment feel like home. Seek out comfortable furniture, soft, luxe bedding, cozy throws, plush towels, and beautiful rugs. Enhance the ambiance with soft lighting, scented candles, essential oils, and soft music to create a soothing and relaxing atmosphere.
A comfortable and cozy living space will help you settle in and truly enjoy your new home.
Turn your senior living apartment into a tranquil oasis with beautiful plants or greenery. A couple of lush green plants will add beauty and freshness to indoor and outdoor living spaces. In addition, plants and greenery reduce stress, relax the mind, improve air quality and overall well-being.
Moving into a senior living apartment doesn’t mean giving up the feeling of home. With these tips, you can transform your living space into a place that reflects your personality, provides comfort, and a sense of familiarity. Embrace the opportunity to create a space that brings you joy and supports your well-being, making it a home where you can thrive and enjoy this new chapter of your life.
If you have questions about assisted living or memory care services here in Winder, GA, contact us anytime!
17 April 2024

Greetings once again from your Gateway Gardens Assisted Living and Memory Care community here in Winder, GA. We manage our assisted living and memory care blog as a labor of love for all those who care for our local seniors and memory care dependents. Yes, we are in the business to provide safe and nurturing professional care services, but we celebrate all of you who care for loved ones at home. We know you and your struggles better than you might think. By helping you with our blog production, we hope to improve your quality of life while simultaneously demonstrating our care, knowledge, and professionalism. We want to make a difference for you now when you might not need us full-time. We know, we’ll make a difference when the time comes to transition to full-time professional assisted living and/or memory care.
It’s essential to build your support network early in your caregiving role. Look for support groups offered through local hospitals, libraries, area agencies on aging, senior centers, and mental health advocacy organizations. Through these groups, you will find helpful resources, guidance for dealing with difficult situations, and the invaluable insights of those who have already navigated caregiving challenges.
Knowing where to find, and having access to support is not the same as asking for help. If you are overwhelmed, showing signs of caregiver stress (see below), then you must put ego aside and ask for the help you need. Your loved one’s medical provider or patient advocate from a local hospital or support group is a good place to start.
Mindfulness is not only for people who meditate. You can learn to bring mindfulness strategies into daily life—from folding laundry to walking the dog. You can also cultivate a formal mindfulness practice, which has been shown to significantly reduce stress, chronic pain, and symptoms of depression and anxiety. Many community programs such as yoga studios, parks and recreation, YMCA/YWCA offer mindfulness groups or look for a mindfulness-based stress reduction program for caregivers offered through a local hospital or medical arts organization.
There are three things caregivers can focus on to maintain their own wellbeing: sleep, balanced nourishment, and daily physical movement. Sleep is essential to overall health and wellbeing. During sleep, the body recovers, heals, and develops innate resources to support how we live, work and play during waking hours. One sure sign that you are getting sufficient sleep is waking up feeling refreshed and restored. If you don’t wake up most mornings feeling this way, then you may want to create a sleep routine. A healthy sleep routine includes going to bed and waking at the same time each day; using room darkening curtains; lowering the room temperature; and not using digital devices in the bedroom with the hour before going to sleep.
Balanced nourishment means including a variety of real, whole foods in your diet—and enjoying sweets and treats in moderation If you eat mostly packaged and boxed foods, your body is not taking in the vitamins and minerals and fuel nutrients (carbs, protein, healthy fats) that it needs for optimal function. Without a balanced diet, you will feel the effects of stress more sharply and you are likely to throw-off your sleep routine, which compounds stress. If you need some guidance on healthy eating to support your caregiver role, local hospitals and wellness centers usually offer nutrition workshops.
Physical Movement – While vigorous physical activity a few times a week is ideal, it may not be realistic for you as a caregiver to get 3 or 4 workouts in a week. Instead, aim for daily physical movement that gets your heart rate up for 30 minutes. This can be a walk, bike ride, working in a garden, yoga, taking a fitness class, or turning on music and dancing in your living room. Movement releases hormones that help support a positive mood, strengthens, and tones the body, and helps relieve stress. Find something you enjoy and move every day!
The stress of caregiving puts the caregiver at risk for health problems such as burnout, anxiety, depression, chronic fatigue, headache, sleep disturbances, and relationship tension. If you are experiencing symptoms such as these, it is imperative to seek support and medical guidance so that you can recover your wellbeing and continue to be of support to your loved one.
You have access to premier quality assisted living and memory care services right here at Gateway Gardens Assisted Living and Memory Care in Winder, GA. Come visit or send questions to us anytime!
3 April 2024

One of the most common questions from those new to us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA is: "How will I pay for it?" There are numerous ways to pay (fully or partially) for assisted living services and/or memory care services. Those ways include long-term care insurance, VA benefits, reverse mortgage, annuity, or a bridge loan. Let's take a closer look at each of these options.
Long-term care insurance is designed to help policyholders pay for the costs associated with long-term elder care services like assisted living. Long-term care insurance is private insurance. Monthly premiums for this type of insurance vary widely depending on the health, age, and amount of coverage.
If you're planning on using long-term care insurance to pay for assisted living, you must plan well in advance. The best time to purchase long-term care insurance is between the ages of 40 and 50.
You may be ineligible to purchase this type of insurance after a certain age or if you have certain major health conditions like Alzheimer's, cancer, heart disease, or multiple sclerosis. You may also be ineligible to purchase long-term care insurance if you have a criminal record or a history of substance abuse.
When purchasing a long-term care insurance policy, it is very important that you read all the fine print and fully understand the terms of your agreement. Working with an insurance or elder care attorney when purchasing a long-term care insurance policy can be beneficial.
If you have an active life insurance policy of $50,000 or more, you can convert that policy into a long-term care benefit plan account. Converting a life insurance policy to a long-term care benefit plan involves transferring ownership from you to an official benefits administrator.
The funds from your life insurance policy will then be put into an FDIC-insured benefit account, and automatic payments will be made to a designated care provider, like an assisted living facility.
The remaining account balance will be distributed to your family members or other beneficiaries after you pass away.
The Department of Veterans Affairs (VA) offers several programs to help veterans and their families pay for long-term care services, including assisted living. To be eligible for these benefits, you meet all the following criteria:
Generally, the VA does not pay for room & board at an assisted living facility but will pay for other basic services and healthcare expenses.
Certain veterans may also be eligible for the VA Aid & Attendance Pension, a version of the basic Veterans Pension specifically for veterans with limited income who cannot complete the activities of daily living without the assistance of another person.
These pension benefits will cover some of the daily living costs in an assisted living residence. The amount you can receive from the Aid & Attendance Pension is based on how many dependents you have and if you're married to another veteran who qualifies.
To learn more about accessing these services, call the VA's toll-free hotline at 877-222-8387, Monday through Friday, 8:00 a.m. to 8:00 p.m. ET.
A reverse mortgage is a loan that allows homeowners to tap into the equity in their homes and use it to pay for things like home repairs, medical expenses, or in this case, the cost of assisted living. The loan is repaid when the home is sold after the borrower dies or moves out permanently.
Generally, a reverse mortgage is only an option if a spouse or other co-borrower on the loan still lives in the home.
Contact a reverse mortgage specialist in your area for more information about how reverse mortgages work and whether or not you qualify for one.
An annuity is an insurance product that can be used as a source of income during retirement. Think of it as a contract between you and an insurance company in which the insurance company makes regular payments or a single large payout to you in the future. You can buy an annuity in one lump sum or overtime in a series of payments.
Annuities will grow over time and can provide income later in life when you need to pay for long-term care.
An annuity should be considered an investment, and like all investments, it carries a certain level of risk. Because purchasing an annuity can be complex, it's essential to work with a trusted financial advisor or attorney.
A bridge loan is a short-term loan that a senior takes out to fund their move to an assisted living facility while they wait for their house to sell. Taking out a bridge loan can be risky. Generally, this option should only be used if necessary. If your house doesn't sell as quickly as you thought it would, you will still be on the hook to begin loan repayment, which means you'll be paying for the loan, your home's mortgage, and the costs of assisted living. But for some, bridge loans pass the risk test.
There are many options available for financing assisted living costs, and seniors and their families often choose more than one way to pay these costs. It's just a matter of finding the ways that best suit your needs and budget.
Research each option and talk to friends and family members who have navigated paying for assisted living. Consider speaking to a trustworthy financial advisor or elder care attorney who can help you decide how best to use or invest your current assets for future long-term care needs.
Lastly, look into your state, regional, or local agencies and organizations on aging. They may have information on additional resources, offer benefits and financial counseling, and help walk you through government programs like Medicaid and Medicare.
When the time comes for you to seek a consult regarding caring for your loved one’s senior assisted living care needs, please know that Gateway Gardens Assisted Living & Memory Care in Winder, GA stands ready to help you every step of the way! And that includes doing everything we can to empower you to be fully informed regarding financial pathways.
27 March 2024

So, you’re planning what to do this Easter with your loved one and our cherished resident of here at Gateway Gardens Assisted Living & Memory Care in Winder, GA. You want so much to be uplifting, innovative, inspirational, but most of all, loving. But some of you are stressed about how to do this. We take great pride in helping not only our dear residents but all of you to enjoy life to the fullest. We have some simple things for you to consider.
Here are simple tips for visiting your loved one within either our assisted living community or our memory care community:
Please consider (but don’t worry) any of the things suggested above. Your loved one likely will be happy to simply go with the flow. So, Happy Easter to all from all of us here within our Gateway Gardens Assisted Living community and our Gateway Gardens Memory Care community! Enjoy your visit!
20 March 2024

Here’s an idea to make your senior family member or friend’s face light up. Regardless of the degree of your religious faith, chances are you senior loved one residing within our Gateway Gardens Assisted Living Community or our Gateway Gardens Memory Care Community are rooted in religious faith. Spirituality just might be your senior or memory care loved one’s most foundational joy. Come visit them and share your knowledge of “Palm Sunday” which arrives in just a few days.
Palm Sunday remembers and celebrates when Jesus rode into Jerusalem on a donkey, as foretold in a prophecy in the Old Testament in Isaiah and Zechariah. What Do Palm Branches Represent? Palm tree branches are a symbol of victory (Revelation 7:9). "Rising with slender stems 40 or 50, at times even 80, feet aloft, its only branches, the feathery, snow-like, pale-green fronds from 6 to 12 feet long, bending from its top, the palm attracts the eye wherever it is seen." The whole land of Palestine was called by the Greeks and Romans Phoenicia, i.e., "the land of palms."
The Jewish people wanted victory, victory over the Romans who had invaded their land. Jesus did come to enact a victory, but not quite the one they had in mind. When we use palm branches in our services, we can remember how Jesus conquered death for us to have a chance of salvation through Him.
Almost certainly, your discussion about Palm Sunday will give way to fond Easter memories (Easter Sunday follows Palm Sunday) and thus a warm and fulfilling visit will have taken place.
On behalf of our entire staff and your loved one under our care here at Gateway Gardens Assisted Living and Memory Care, thank you for stopping in and lifting the hearts of our dear residents. When their hearts are lifted, ours are as well.
13 March 2024

Many of you are already thinking of ways to make this Easter special for your loved one here within our Gateway Gardens senior living or memory care community. We’re here today to comfort you by suggesting that you don’t overthink this. Spending time with your loved ones is far and away the best gift that you can offer. the best part of celebrating the holidays and everyone appreciates feeling loved. Read on to learn more about how to celebrate this Easter with your senior assisted living or memory care loved one.
Easter is a holiday celebrated by many in various ways. People of all ages spend time with their families, engaging in festive activities such as having feasts, going on egg hunts, or making crafts. However, some of these activities are not suitable for certain family members – our aging parents. When planning such activities, we should always be mindful of their health and physical conditions, but this does not mean we have to compromise on the fun of the activities.
With Easter around the corner, we have put together this list of ideas for an enjoyable Easter celebration with aging parents.
What is Easter without decorated eggs? A common craft activity during the season, it is easy to do and older adults are sure to enjoy painting them. Prepare some hard-boiled eggs and art supplies such as watercolor paint, markers, stickers. You can even throw in a challenge and make it a competition amongst the family for the best design!
Let your loved one get creative by designing their own Easter cards. It may also give them a sense of purpose by bringing joy to friends and family through gifting their handmade cards this festive season. They will need colored paper, colored pencils, glitter, scissors, and other relevant materials. Once the cards are done, you can help mail them out to their recipients. Else, if your family is having an Easter family event, your loved one can pass it to the recipients personally.
Many older adults love playing bingo. Give it a twist with Easter or spring-themed bingo for your loved one. You can find such themed bingo boards online. Alternatively, you can let your loved one decorate plain bingo cards with Easter stickers and drawings as well as spring colors.
As people grow older, they tend to value and enjoy time with their loved ones more. Holidays are an excellent opportunity to get the family together. Organize a small Easter brunch or afternoon tea where family and friends can get together and bond over food and games. Your parents will enjoy the laughter and company.
If your parents are Christian, you can celebrate the occasion by going to church together with them. Easter Sunday and Good Friday services are usually offered several times throughout the day. Some seniors enjoy listening and singing to hymns and hearing the sermons. Sharing a spiritual moment with your parents is a good way to bond with them as well.
As many older adults suffer from a range of health conditions such as poor eyesight, shaky hands, or stiff joints, we are recommending the above activities that are deemed safe for people in that age group. However, as every person’s condition differs, it is imperative that for the craft activities, you monitor the situation closely or alter the activities accordingly as you deem fit. We hope that your loved ones will enjoy the activities and have a great Easter!
Gateway Gardens Assisted Living and Memory Care is a world-class living and care experience. You and your cherished family member will superb living, medical, and social opportunities. Rest assured your loved one will enjoy our community’s special focus on the Easter Holiday. But it’s not just Easter when our cherished residents wake up feeling excited for the new day. They take part in a full schedule of fun activities daily, whether it is Easter, St Patty’s Day, or just another Wednesday to celebrate life. Feel free to contact us for more information.
28 February 2024

Welcome back to our Gateway Gardens assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home whether you provide senior assisted living services or memory care services to your loved one.
We all know the importance of medication management. Here are a few medication management tips seniors should keep in mind to avoid any serious complications:
1) Create a list of all current medications. Keep an ongoing list of all prescription and over-the-counter medications that are taken daily. The list should include both the reason the medication is taken, along with the correct dosage, time of day to take it, and any other instructions, like taking it on a full stomach or with water. This list can then be discussed regularly with a doctor and updated accordingly.
2) Learn about possible medication side effects. Knowing common medication side effects can help you stay aware of any changes to your current health, especially when adding a new drug into the mix. If adverse side effects appear, they should be discussed with a doctor or pharmacist right away.
3) Set a medication schedule. If necessary, set reminders so you remember to take your medications at the right time of day every day. A medication dispenser can help keep your pills organized throughout the day. If you miss a medication, be aware of how to proceed- should you wait and take it at the next scheduled time, or take it as soon as you remember? Your doctor or pharmacist can help answer these questions.
4) Order refills in advance. Don’t wait until you’re down to one pill to order a refill of your prescription. Cutting it too close can cause you to miss medications, and in some cases, even skipping just one pill can cause problems in your treatment program.
5) Use the same pharmacy for all prescriptions. Pharmacists are extremely helpful in keeping tabs on your medications and can help eliminate any adverse side effects or reactions to new drugs. Plus, you can streamline the process for refills and pick up all your prescriptions at the same time each month.
6) Properly store all medications. While it might seem easiest to store medications in the bathroom, this is not the best location for many drugs. Bathrooms get warm and damp, which can cause medications to break down faster. Some meds may even need to be refrigerated. Read all the labels carefully to ensure you’re storing medication in the right place.
If your senior loved one is an existing member of our Gateway Gardens assisted living community or our Gateway Gardens memory care community, then you can rest assured that your loved one’s medication safety is meticulously managed. If your senior loved one is under your care at home, then it is never too early to take renewed detailed focus upon medication management, to ask questions of your loved one and the care providers subscribing their medications. Medication management adjustments are routinely driven via at-home care giver’s testimonials to their loved one’s care teams. We are trained and experienced at this. It is our sincere wish that you at-home care providers prioritize skill development in this arena as well.
21 February 2024

Greetings once again to all our Gateway Gardens assisted living, Gateway Gardens memory care community, and Gateway Gardens respite care residents, family, neighbors, and friends. There are plenty of myths and non-truths out there regarding dementia, its causes, effects, and expectations. Today we’re going to discuss a common belief that sugar alone can be a principal cause of memory challenges. So, let’s get right to it.
A high sugar diet is not a cause of dementia, but it can increase the risk of developing this disease. Our conclusions here are largely guided by an informational resource that you should check out: Alzheimer’s UK.
While eating sugar doesn’t mean someone is guaranteed to develop dementia, too much sugar can increase the risk of developing this disease. Sugar increases the risk of type 2 diabetes, a risk factor for dementia. Research suggests that cutting down on fizzy drinks, sweets, cakes, and other sugars can help lower the risk of dementia. Additionally, eating a balanced and healthy diet can help reduce your risk. Other research suggests that excessive sugar can lead to poor cognitive function later in life. Another study found that adults with high sugar intake were 1.84 times more likely to develop dementia.
So, again, lots of sugar isn’t a cause of dementia, but it can increase the risk of developing this disease. Rest assured your loved ones here at Gateway Gardens Assisted Living and Memory Care in Winder, GA enjoy a healthy, highly enjoyable, and highly regimented as guided by resident family and medical teams.
14 February 2024

As you get older, you might notice you’re reaching for sweaters more often, shivering even when you think you should be warm, or maybe turning up the thermostat often. Is it really getting that much colder every year, or is it something else?
As we get older, we often feel colder at temperatures we were once comfortable with. There are a few causes of this, including thinning skin, slower blood circulation, or even side effects of medication. Age isn’t the only cause of feeling colder, though; it can also be related to several medical conditions such as anemia or even diabetes. It can even be your own residence, contributing to the problem. With the rising costs of heating and other bills, many seniors find they’d rather wear a sweater and be a little cold rather than turn the heat to a comfortable temperature. But this can risk hypothermia or other temperature-related issues and lead to other problems.
Assisted living is an option to consider if any of this sounds familiar. Being in a community like Gateway Gardens Assisted Living and Memory Care here in Winder, GA gives you the option of being surrounded by a caring team that can help with medical concerns and daily needs. And, you get to avoid most utility fees, so you can dial up that heat and be as comfortable as possible!
There are several common reasons that can make you feel cold as you get older. As we age, our skin naturally thins, along with the layer of fat underneath it, and we even lose muscle mass. By having less of a natural barrier against the air, it’s no surprise you might be feeling more of a chill.
Along with this natural thinning, our metabolism naturally changes as well. Metabolism breaks down nutrients from the food and drink we consume and breaks them down into energy, which helps the body regulate its own temperature. As the metabolism slows, your body receives less of the energy it needs to maintain its heat, which can contribute to the cold you might be feeling.
Another common cause of feeling cold so often is related to blood circulation. Problems with blood pressure and blood circulation are common as we age, and a decrease in either can lead to you feeling colder in your extremities as blood works harder to get to them.
If you’ve recently noticed you’re less physically active than before, this can be a contributing factor to feeling cold all the time. As we get older, it’s common to stop doing some of the more physical things we’ve done for most of our lives. But if you’ve recently slowed down your physical activities, this could be directly related. Since daily physical exercise helps build and maintain muscle mass and helps with blood circulation and blood pressure problems, it could take something as simple as moving around more often to help.
There are many medical conditions that can cause you to feel cold all the time. Some of the more common conditions known to cause this include:
While these aren’t the only causes, they are some of the more common ones. If you’ve recently noticed that you feel cold more often, or you’re struggling with any symptoms caused by this, it’s extremely important to speak with a doctor. If you’re on any medication to treat one of these conditions, it could be causing the unfortunate side effect of making you feel colder.
We are currently accepting new residents, so don’t hesitate to reach out if you need excellent care at our memory care or our assisted living community. We also manage this blog for a reason, and that is to assist you and/or your caregivers to lead a more fulfilling and safe life. Call us today to learn more and to schedule a tour of our Gateway Gardens memory care community and/or our Gateway Gardens assisted living community. Oh, by the way, we provide Respite Care Services here in Gateway Gardens as well!
7 February 2024

Welcome back to our Gateway Gardens assisted living community and our Gateway Gardens memory care community’s blog. Most of you know that we manage this blog on behalf of our cherished residents, their families, and of course for all of you homecare heroes taking care of your assisted living and/or memory care loved ones. Today, we’ll discuss a real concern that many of you might not be familiar with: Elder Self-Neglect.
Elder self-neglect is a huge concern for many seniors and their loved ones. Our memory care professionals here in Gateway Gardens have some helpful information regarding this topic, as well as some signs you should be aware of.
According to the National Institute of Health, elder self-neglect is best defined as “refusal or failure to provide oneself with care and protection in areas of food, water, clothing, hygiene, medication, living environments, and safety precautions.” This is typically seen as a person getting older and they struggle to complete the necessary, everyday tasks they need to stay healthy and functional. This can look like poor personal hygiene, missing medications, and doctor’s appointments, skipping meals, and even staying isolated in one place.
This is a growing problem, especially after the global pandemic, and individuals who suffer from underlying health conditions are at even higher risk. For example, if they have Alzheimer’s or dementia, or other chronic conditions, such as diabetes, this elevates the cause for concern. Elder self-neglect only serves to exacerbate mental and physical health issues as well.
According to census data, around 25% of adults aged 65 or older live alone. That comes out to around 14.3 million Americans. Each year, this number only increases as well. According to more data, older adults spend at least half of their waking hours alone, if not more.
Unfortunately, this provides plenty of time for health and well-being to deteriorate, even going unnoticed and flying under the radar. This time spent alone can lead to a downward spiral, especially for those with dementia or other memory loss related issues.
Whether you are the primary caregiver, or you simply have a senior in your life you love and are concerned about, we have some signs that you should keep an eye out for. Elder self-neglect may not be as easy to spot as you would initially think. Oftentimes, your senior may even try to brush it off or say that everything is fine, even when it’s not.
Here are some of the signs you be aware of and questions you should ask yourself:
While all of these are not exclusively signs of elder self-neglect, and your senior loved one doesn’t have to check every box, they are still a good baseline as to what to be aware of.
If you determine that your senior loved one may be experiencing elder self-neglect, it may be time to reach out for help. As a primary caregiver, it is normal to want to do everything alone and shoulder the responsibility yourself. However, it’s important to know that you don’t have to, and we are here to help. Contact us here at Gateway Gardens Assisted Living and Memory Care in Winder, GA!
31 January 2024

IF YOU’RE STRUGGLING over the decision to move into an assisted living community to begin the next chapter of your life, we’re here to help. Here are eight great benefits of embracing a loving living environment like ours here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
Seniors who live alone are at a higher risk for social isolation and feelings of loneliness and depression. In professional assisted living communities, seniors enjoy a community environment with friends and staff encouraging participation in social events. Our community offers a dynamic activity calendar and encourages maximum participation. Residents have opportunities to discover new hobbies, embrace fitness for life, an array of social communal interests, and so much more.
Some residents in our assisted living community need help with daily tasks such as dressing, bathing, hygiene, medication assistance, and more. Maybe such things are not part of your personal daily need. But when or if that time comes, we’ll be there for you. Every staff member is well-trained to provide the care residents need in a way that protects privacy and promotes dignity. No matter if it’s managing a complex medication schedule, attending a senior fitness session, your loving staff are excited to help.
Assisted living isn’t just about care services, it’s also about having the freedom to enjoy life. We make sure residents are doing what they can when they can. Think of our services as professional living care providers as enablers for your quality of life: we enable you to live more carefree, more confidently, and with more fun!
Many seniors can maintain a home but find it increasingly less desirable to do so. Whether the notion pertains to increasing physical challenges or simply a different view on how best to use time, many seniors no longer want to mow the lawn, sweep, dust, and vacuum. Residents in an assisted living community don’t have to worry about the cleaning, the cooking, the shoveling. It’s our pleasure to work for each of our residents, allowing them to catch up on a reading list, plan an exciting trip, find a new hobby, or invest more time into a lifelong interest. Making the move to assisted living means doing more of what you love.
Meals here in our Gateway Gardens assisted living community are specifically created to benefit senior health because healthy residents are happy residents. Cooking for yourself by yourself can grow challenging. With nutritious meals prepared by talented culinary experts, our dear residents enjoy delicious meals that are scripted for senior’s dietary needs. Quality dining is important, but equally important is the rewarding social nature of community dining.
When driving becomes unsafe or car ownership becomes too much of a hassle, we offer reliable transportation to local shopping, dining, events, and doctor appointments.
A move into assisted living is a move into a lifestyle that promotes healthy senior living and opens a variety of options for the future if needs should change over time. Each resident has an individualized, custom care plan that is regularly evaluated by a medical team, ensuring that any change in health is noticed as it happens, resulting in early diagnosis and, inevitably, better treatment options.
All of these benefits work together to create the ultimate benefit: peace of mind. Friends and family of residents rest easy, knowing their loved one is being well cared for in a home-like environment where their needs are seen. Seniors themselves rest easier too, with the knowledge that they have a family in their community who is there for them, cheering for them, and helping make the most of every day.
We are ready to help you take a great stride in quality of life here at Gateway Gardens Assisted Living and Memory Care in Winder, GA. Call us today to learn more and to schedule a tour of our memory care assisted living community.
17 January 2024

Welcome back to our Gateway Gardens Assisted Living and Memory Care blog! To start 2024, we began this mini-series addressing the basic difference between assisted living and memory care communities. Last week we covered “Do We Need Assisted Living or Memory Care”. We’re going to finish the series today providing you with tips for choosing your future assisted living or memory care community.
Once you’ve determined which service that most likely meets your needs, you should research assisted living and memory care communities within the Winder area. We strongly believe the more you know about your options, the more attractive you are going to discover us to be.
If you are already familiar with the area or are interested in sticking close to your current residence, it can be helpful to seek out recommendations from local personal physicians, financial planners, social workers, friends, and other relatives who may be familiar with our local communities. Additionally, it can be helpful to reach out to your local state health department for recommendations.
Once you’ve created an initial list of candidates, you can begin to narrow down the field by reviewing the specific services, location and price range that fits into your budget. From there, it’s important to take the first steps to reach out to the community administrators to schedule a tour of each community.
We trust this blog has served useful. Please know that we stand ready to invest all our energies to help you navigate this critically important research. Please contact us anytime here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
10 January 2024

Welcome back to our Gateway Gardens Assisted Living and Memory Care blog! Last week we started our mini-series addressing the basic difference between assisted living and memory care communities. The fastest way to decide what type of service would best support you or your loved one is to take an honest assessment of your personal situation.
In general, you’re likely well-suited for our Gateway Gardens assisted living community if:
You’re likely better suited to Gateway Gardens memory care community if:
Understanding that after reading the above that you may discover having more questions than before, know that you are on the right track. We can personally help you navigate this deeply complex and critically important investigation. We are prepared to invest every minute you need to become fully informed.
Tips for Choosing a Loving Assisted Living or Memory Care Community. Until then, feel free to contact us anytime here at Gateway Gardens Assisted Living and Memory Care in Winders, GA.
3 January 2024

Very warm 2024 greetings to you all from Gateway Gardens Assisted Living and Memory Care in Winder, GA! To start off the new year, we’re going to author a short series of posts here on our Gateway Gardens Assisted Living and Memory Care blog to address the numerous differences between the two in the attempt to answer common questions. We hope to walk away with a better understanding of the support and services offered in each, as well as providing tips on how to choose the right option for yourself or a family member.
Assisted living and memory care provide similar levels of support by helping residents with daily tasks like getting dressed and eating. However, memory care is different from assisted living because it provides specialized support for individuals with memory impairments such as Alzheimer’s disease.
So, let’s start the new year off with a tutorial summary of the basics: Assisted Living vs Memory Care.
Individuals within our Gateway Gardens assisted living community are largely independent but want or need some help in certain areas of their lives. They are generally healthy and active. Our assisted living service is a strategic comprehensive assortment of long-term wellness programs that include:
The most important aspect of assisted living is the help it provides with daily tasks. That might include helping move from one place to another or helping to get dressed in the morning. Assisted living helps in these areas so residents can spend less time on these tasks and instead focus on enjoying their freedom.
Depending on the needs of each resident, our assisted living community provide additional services, such as “housekeeping” support, transportation services, 24-hour safety and security, recreational activities, and other things that make life easier and more rewarding.
The biggest difference between our assisted living and our Gateway Gardens memory care community is the people we support. Unlike the residents within assisted living, those within our memory care community have long-term health needs, specifically memory impairments such as dementia, that are best met by a specially trained staff.
To provide adults with the support they need to live full lives, our memory care service strategy encompasses the same base services and amenities as our sister assisted living community. However, memory care services and amenities are tailored to meet the needs of individuals with memory impairments.
For example, our memory care community offers similar housing accommodations to that which our assisted living residents enjoy, however, our memory care resident’s accommodations incorporate additional safety measures to ensure that those prone to wandering are safe and happy. Our memory care residents benefit from a more structured lifestyle designed to facilitate a stress-free lifestyle.
Our memory care residents enjoy specialized programs that are designed to improve cognitive skills and slow the progression of memory loss. These programs, along with access to 24-hour medical care, make for a safe, fun, and interactive living environment.
How to know if you or a loved one needs assisted living or memory care. Until then, feel free to contact us anytime here at Gateway Gardens Assisted Living and Memory Care in Winder, GA.
11 December 2023

While the Holiday season is a time for celebration, joy, and time together here at Winder’s Gateway Gardens Assisted Living and Memory Care, it can also be a time of added stress for those of you providing at home care. This is true for those of you who deliver memory care support to your Winder loved one or assisted living support to your Winder loved one. As you continue to prepare for and enjoy all that the season has to offer, those of you caring for others often have an additional worry of how to maintain traditions and connectedness while managing the many changes that come with your loved one’s journey through aging and/or disease.
Be Prepared: Setting expectations and being prepared can help settle stress for both the person, their caregivers and family members.
Maintain Traditions: Maintaining traditions is a wonderful way to invoke positive memories for all! While modifications may need to be made, sharing holiday traditions creates wonderful connections.
Maybe the most important thing you can do for your loved one is to remember to take care of yourself, manage your own expectations and know that all the time spent with your loved ones is a memory worth making!
All here at Winder’s Gateway Gardens Assisted Living and Memory Care wish everyone a wonderful Holiday Season!
4 December 2023
Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. Not much introduction to the linked video below is required. What is required is the due credit to the Chevrolet Motor Company for producing a heartwarming Holiday season video reminder that the joy and happiness within your memory care loved ones lies within, and just around the corner as you will soon learn.
This five-minute video depicts how a simple act of love from a family member returns visible joy to their memory care matriarch. If you have already seen this short video, then you know that it’s worth watching again, and likely has moved you to fetch some tissue in advance. For those of you who haven’t seen this video, go grab some. You’re going to need it.
For your assisted living and memory care loved ones, make this Holiday season one to remember. Warm Holiday greetings and wishes to you all from your friends here at Winder’s Gateway Gardens Assisted Living and Memory Care.
27 November 2023

Greetings once again to all our Winder-area assisted living and our Winder memory care community residents, family, neighbors, and friends. Physical activity is important at any age, but it’s essential for seniors. The CDC recommends that people 65 and older devote at least 150 minutes a week to exercise to maintain muscle mass, flexibility, balance, and strength. Staying active also has a positive impact on emotional well-being.
You and your senior loved ones can do plenty of indoor activities and exercises when it’s cold outside! Have a look through some of our suggestions below to get started, but remember that you should have your primary care provider approve any exercise routine before starting it.
If you haven’t exercised in a while or if you struggle with mobility, we recommend starting small. A simple activity is to go from sitting to standing and walking around your home. Just ensure your floors are clear of impediments so you don’t trip or fall. If you have stairs and can walk up and down them safely with a railing, this would also be a great addition to your exercise regimen.
Exercise doesn’t have to be grueling! Sporadic movement throughout the day is better than nothing. Be gentle with your body, but make sure you move throughout the day, even if it’s just from one room to another. If you have mobility issues that limit you, turn to your primary care provider for recommendations on exercises you can do while sitting or lying down, such as chair yoga or other gentle exercises. And if you have trouble remembering to move, consider leaving reminders out for yourself. A sticky note on your bedside table, end table, mirror, or refrigerator might do the trick.
You can tailor your exercise to your interests! Make it fun by playing your favorite music or watching an exercise video you enjoy. Better yet, invite a friend or family member to join you, or join an online exercise class. Activities with others can make anything more enjoyable.
We will enjoy comfortable and sunny days during the winter. If there’s no precipitation and the sidewalks are clear, put on your most supportive and stable footwear and head outside for a walk. Remember to take it slow. And, as always, adjust your plans accordingly if you have mobility issues.
Here at Gateway Gardens, we have a professionally trained staff to help our dear residents stay active while keeping them safe. We also have a full calendar of activities each month tailored to the season and weather. Want to learn more about life at Winder’s Gateway Gardens Assisted Living and Memory Care? Schedule a tour and know that we truly look forward to meeting you!
13 November 2023

Welcome back to our Winder-area assisted living and memory care blog here at Gateway Gardens. There is so much to celebrate as a resident or family member here. Today, we’re going to focus upon a benefit here that our residents and resident family alike don’t truly appreciate until sometime after moving in. We facilitate an active and vibrant social environment worthy of celebration.
An active social life isn’t just for young people. It can be argued that seniors benefit more from active social lives as do younger people.
Human beings are social creatures. Socialization is vital to survival. Life’s demands upon the young adults drive them naturally (willingly or unwillingly) into active social lives. Professional lives and raising children often produce plenty of social integration. But when seniors have moved on from employment and raising children, continued social interaction is key to both physical and mental wellbeing.
As we age, we tend to experience more life changes. One of the biggest is the loss of those around us. Physical limitations can make it difficult to expand our social circle. While loved ones grow older and pass away, many seniors find it challenging to meet new people and remain socially active.
If you or someone you love is a senior, it’s important to be proactive about being social. Find opportunities to meet people and connect with friends. Whether it’s in person or online, interactions can help us live happier, longer lives.
Why is an active social life an essential part of healthy aging? Social Seniors Tend to Be Mentally Healthier.
One of the many benefits of moving into our Winder assisted living community and our Winder memory care community is our committed focus upon encouraging and enabling a robust social environment. We strongly believe that seniors have earned the right to relax and share and celebrate their golden years within a loving community of their peers.
Come visit us here at Winder’s Gateway Gardens Assisted Living and Memory Care and personally experience our active and loving social environment.
HIR6 November 2023

Hello and welcome back to our Gateway Gardens Assisted Living & Memory Care blog. Today we turn our focus to the upcoming Labor Day weekend and how all of you providing assisted living care and/or memory care support services to a loved one.
While Veterans Day is celebrated every year, many people often mistake its meaning for Memorial Day. Memorial Day is dedicated to remembering those that have died in battle or as a result of their wounds. Veterans Day is a day to think about all veterans, both those living and those that have passed. It is a time to thank them for their service and the sacrifices they have made for our nation. If it were not for the bravery and dedication displayed by the members of our military, we would not be able to enjoy the freedoms that we have. And for that, we say thank you.
Please make every effort to share time, appreciation, and love for every person whose selflessly served our country. Here at Winder’s Gateway Gardens Assisted Living & Memory Care we celebrate every veteran’s unique sacrifice and contribution to our country and wish all of you a warm and blessed Veteran’s Day holiday!
30 October 2023

Getting the news that your parent, in-law, spouse, or other loved one has dementia is devastating. There’s no other way to put it. Here at Gateway Gardens Assisted Living and Memory Care here in Winder, we will be honored to help you every step along the way. Whether that help to you is direct in the form of you and your loved one joining our memory care community or by simply offering free education via this memory care blog, rest assured our hearts go out to you because very few can directly relate to what you are going through.
So, for those of you researching what construes the dementia journey, we hope to help you out here today. Dementia is a general term for a group of complex diseases that affect memory, thinking, and behavior. Alzheimer’s disease is the most common form of dementia and affects older adults.
Dementia begins with mild changes in mental function and slowly worsens to severe impairments in cognition. If you have a loved one with dementia, knowing these changes can help you plan for their care.
Dementia is more common with age, one-third of people over 85 may have some form of dementia, but it’s not a normal part of aging. There are different types of dementia, many causes of cognitive function, and varying symptoms depending on the type and stage.
Risk factors for dementia include the following:
Dementias are progressive diseases, and changes in functional ability continue to occur. Three stages of dementia include early or mild, middle or moderate, and late or severe. Early onset/mild cognitive impairment refers to Alzheimer’s disease diagnosed at a younger age.
Early or Mild Stages of Dementia
In early or mild dementia, people aren’t always aware they have the disease. However, some people may notice slight changes that something is wrong with their thinking but can still function independently with little help.
Changes can include memory lapses and forgetting things that can affect daily life. Signs and symptoms of early or mild stage dementia include:
Middle or Moderate Stage of Dementia
In the middle or moderate stage of dementia, people need more help with everyday activities and self-care as memory and thinking ability continue to deteriorate. At this stage, more people are aware of the condition.
Signs and symptoms of middle/moderate stage dementia include:
At this stage, making life easier for a loved one with dementia can include speaking to their doctor about care, treatment options, and support services.
Late or Severe Stage of Dementia
In late or severe dementia, the disease progresses to a point where it affects functioning and physical capabilities. Care needs are high and may require continued support 24 hours/day to ensure the highest quality of life.
Signs and symptoms of late or severe stage dementia include:
There is no cure for dementia, but an early diagnosis can help families plan for the future and consider different care options. Doctors can address family history and underlying conditions related to cognitive decline with treatment.
Other methods and tests used to diagnose dementia include:
At Gateway Gardens Assisted Living & Memory Care, we offer premier home environment care in a loving family atmosphere for your loved one. We facilitate the ability of your loved one to continue living with dignity, respect, freedom, and choice. Our home environment enables seniors with Alzheimer’s, Dementia, and other memory impairments to maintain the highest quality of life while providing peace of mind to their family and friends.
16 October 2023

We have a longstanding tradition here at Gateway Gardens Assisted Living & Memory Care here in Winder to celebrate Halloween with both our assisted living and our memory care residents. We do, however, celebrate a bit differently within our two unique care communities. The scary and ghoulish themes of Halloween can serve a detrimental effect on memory care patients. So, for you at-home memory care providers, we have some things for you to consider in advance of the upcoming holiday.
Halloween is one of the most celebrated days in the American calendar. It is a day rich in history that everyone should celebrate. For decades now, it’s been known to be a favorite day for the kids who would feel their pockets or even bags with candy, fully dressed in a ghoulish costume.
Halloween is characterized by scary costumes and decors which can greatly frighten individuals with Alzheimer’s. It is therefore important to organize Halloween parties that suite people with Alzheimer’s for them to feel loved an included. How can we organize Halloween for seniors? Here are few tips to make this Halloween happy and safe for everyone:
Halloween is all about decorations and costumes. Halloween wouldn’t be the same without them. But extreme decorations don’t go well with people who suffer from Alzheimer’s. Keep decorations to a minimum. Even though it may not guarantee that the patient will not get confused or stressed, maintaining the outlook of the house by decorating minimally celebrates the holiday without causing too much confusion or disorientation. To accomplish this, there are some things that one should do or avoid.
It’s always fun for kids to watch ghosts and goblins at the park during Halloween festival. The same cannot be said about people with Alzheimer’s. This might cause the patient to avoid the place again due to scary memories. The best thing is to take them to a less public and elaborate celebrations.
There is no Halloween without candy. In the culture of celebrating Halloween, most families, if not all share candy with other kids. It is therefore difficult to keep candy away. Nutritionally, sugary foods have been known to heighten the condition. Many patients won’t control themselves from taking candy. It is therefore important to monitor them or even keep the candy away in a safe place.
Although this may prove to be a hard option, it is important to try and explain to your loved one that there will be some commotion around. If you are someone who has stayed with the patient for a long time, you will have a good chance of getting them to understand. Even so, this won’t guarantee you success because patients with Alzheimer’s lose memory very quickly. Therefore, try to create distractions and carefully and patiently explain any questions that they may have.
Halloween can be a fun filled time for everyone. Just as we take safety measures to protect children during the holiday, we can provide the same precautions for our elderly and those who may suffer from memory conditions.
All of us here at Gateway Gardens Assisted Living & Memory Care wish you the very best for a joyful Halloween celebration.
9 October 2023

Welcome back to our Winder-area assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home whether you provide senior assisted living services or memory care services to your loved one.
One of the things that matters most to you is the health of your senior loved one. Anemia can cause loss of physical abilities, functional deterioration, and hospitalization, so it’s crucial to be alert for its warning signs. There are symptoms you may look out for and ways to help your loved one treat anemia. Here’s an overview of anemia in seniors, and how professional senior living care can help manage their condition.
When the red blood cell count drops below normal, anemia can develop. Anemia is frequently brought on by blood loss, a decline in the production of red blood cells, or the destruction of red blood cells. Anemia can have a negative effect on one’s health because hemoglobin in red blood cells plays an important role in transporting oxygen to human tissues.
Anemia can have a negative effect on one’s health because hemoglobin in red blood cells plays an important role in transporting oxygen to human tissues. Some common symptoms of anemia include:
Any of these symptoms should be taken seriously, even if they only “seem like what happens as you age.” If a member of your family displays these signs, call their doctor right away because anemia is treatable.
If your senior loved one is receiving care in our assisted living community, you know that we monitor for these symptoms. Our training has us all on extreme high alert anytime our dear resident’s medications are changed. It’s just one of the countless benefits of professional managed care.
25 September 2023

Hello to all our blog fans here at Gateway Gardens Assisted Living & Memory Care here in Winder. Today we return to the daily subject of inquiry from seniors and their caregivers alike: What are the critical indicators that it is time to pursue professional assisted living services? We answer many frequently asked questions that orbit around defining the turning point when a loved one no longer is best served by loved one’s at home. The bottom-line truth is everyone is different and warning signs are rarely absolute or all-encompassing.
Here are a few more behaviors and habits that can suggest it’s time to explore assisted living. Here are seven things to consider:
While there are certainly other considerations to weigh, the sum of these factors can be indicative. If you are observing patterns of injury, forgetfulness, negligence, or isolation, it’s wise to seek out professional counsel. Talk to your loved one’s primary care doctor to get at the root of these patterns and how you should respond.
Gateway Gardens Assisted Living and Memory Care is Winder’s most celebrated community that serves both the assisted living and memory care needs of area residents. Stop in anytime as we’ll be glad to show you why.
18 September 2023

Most of you are aware that our team of professional memory care and assisted living care providers here at Winder’s Gateway Gardens Assisted Living & Memory Care are there for all of you, young and seasoned alike. Whether you are a cherished resident, a family member, or someone caring for a loved one suffering for dementia, we hope you find our blogging efforts informative, a source of actionable ideas for you to provide better care, and a source for peace in your own lives.
Today’s blog post is intended to help you advise others who want to communicate with your loved one but might be intimidated to do that. This is a very common concern and maybe you yourself might be somewhat at a loss to offer them consultation. We find that how a person interacts and understands someone who has Dementia is so important. Recognizing different ways you can connect and communicate may help the relationship.
Consider these suggestions on different ways and opportunities to interact.
Respect. We all want respect and those with Alzheimer’s or Dementia are no different. They want and deserve respect so be thoughtful of how you speak and try to avoid phrases that could be patronizing, demeaning and/or condescending.
Speak clear and calm. Remember to refer to people by their names and refrain from using “he”, “she” or “they” as that can be hard.
It is okay to use touch. A reassuring hug or hand on someone’s shoulder can show affection without using words. Often some of our seniors with dementia miss the physical attention and can really benefit from feeling “loved”.
Keep the conversation simple. Try to talk about one thing at a time. If the conversation has multiple subjects, it can be confusing. Also, try to ask more simple questions that have the opportunity for one or two answers. This can make the conversation feel less frustrating.
Listen. Be sure to spend time listening and not always being the one to talk. If you do not understand something, it is okay to ask them to repeat it or say, “I am sorry, I do not understand”.
Talk about something they are interested in or about their past. Someone with Dementia may be able to remember his or her childhood but have a hard time remembering something that happened earlier that day.
Patience is so important. Give them some time to explain and talk. Try not to interrupt and if you ask a question, just pause and give them time to respond.
We pride ourselves for being readily available to all of you and to apply our vast array of skill sets to help in any way we can. If you are considering a senior living community for yourself or a loved here in Winder, we invite you to come visit and see the thriving senior assisted living community here at Gateway Gardens in Winder and/or our loving memory care community here in Winder as well!
4 September 2023

Greetings once again from your Winder-area assisted living and Winder memory care community here at Gateway Gardens. Today’s blog post is for all of you at-home memory care support providers who might be stressing about periodically (or maybe even often) misplacing your keys, your cell phone, your TV remote, or other commonly used items. Maybe some of you are even moving beyond stress and into fear that you, yourself, are beginning to suffer the same disease as the cherished loved one that you care for. Well friends, while only a professional can diagnose your concern with certainty, what we (non-clinical professionals) can tell you is that the frustrations listed above are more often simply commonalities of normal, fully functional aging adults.
Aging is a natural process, and as we grow older, parts of our brain and body are gradually altered. Some of the changes affect our physical abilities, and others affect us mentally. Everyone ages differently. We all experience changes eventually, and there’s no exact timeline for when these changes will occur.
We can all expect to experience some memory loss at some point, but how do we know the difference between normal aging and a condition that affects cognitive functions, like dementia or Alzheimer’s disease? When is it time to speak to our family doctor about additional support services or memory care?
Dementia and memory loss have similar symptoms but are significantly different from each other. How do we distinguish between forgetfulness and a need for memory care? Memory loss occurs as part of the normal aging process, resulting from a natural decline or slowing of the body. Although the brain begins to slow, a person’s intelligence continues to function as usual.
Natural memory loss will not:
Dementia is a progressive condition resulting from a breakdown of cognitive function. This condition can cause frequently disruptive mental and physical symptoms that gradually worsen.
Symptoms of dementia effect:
If you are losing sleep or constantly worry about your memory issues possibly being related to early dementia, speak to a medical professional. More likely than not, your mind will be put at ease making you more happy, positive, and a better care provider for your loved one. Of course, when it becomes time to put your loved one into the loving care of memory care professionals here in Winder, contact us anytime.
28 August 2023

Welcome back to our Winder-area assisted living and memory care blog! A healthy heart is conducive to brain health which helps mitigate the chances of cognitive decline and impairment. While the exact risk factors for dementia are not set in stone, certain lifestyle changes do seem to have a significant impact on the body and brain and reduce the chances of certain types of dementia, like Vascular Dementia.
Studies show that heart health is linked to brain health. This might be cited as the fact that your heart pumps blood to different parts of the body, including the brain. Therefore, any damage to the vessels through which blood is supplied will lead to a host of serious health conditions like heart disease as well as dementia.
Vascular dementia is commonly caused by a stroke, which is a kind of brain attack. This happens when plaque or a clot blocks a blood vessel, limiting the supply of blood to the brain. It also happens when a blood vessel bursts in the brain. Due to this, the brain tissue dies, increasing the chances of memory loss.
Vascular Dementia is caused by a string of these strokes, which lead to impaired memory and other problems. Therefore, it is safe to say that brain health is related to and, at times, dependent on heart health.
Taking care of your heart can significantly reduce the chances of heart disease as well as memory loss. This guide will talk about some of the ways you can take care of your heart to avoid losing memory at an early age.
High blood pressure or hypertension is a precursor to heart disease. During high blood pressure, too much pressure is exerted on the blood vessels, which incurs the risk of heart disease. High blood pressure is often called a silent killer as its symptoms tend to go ignored.
High blood pressure also increases the chances of dementia later in life. To prevent this, monitor your blood pressure and work closely with a doctor to avoid experiencing dementia.
To ensure heart health, you need to take care of what you feed your body. There are certain foods that are conducive to sound heart health. You should try to incorporate fruits, vegetables, whole grains, and omega-3 fatty acids into your diet. If you have a history of heart disease in your family, you should limit your intake of alcohol and foods that have high sugar content and saturated fats.
Staying active is another way to ensure your heart is healthy and reduce the chance of vascular dementia. A sedentary lifestyle increases the chances of high blood pressure and obesity, another contributing factor to heart disease. Experts recommend at least 150 minutes of moderate intensity exercise a week.
Sound heart health is imperative for brain health, which in turn helps to prevent cognitive impairment conditions like dementia. Follow the tips above to enjoy a healthy heart and brain and do your part in keeping dementia at bay.
At Winder’s Gateway Gardens Assisted Living and Memory Care, we are here to help. We want families to make the best decision for their situation. Furthermore, the staff at both our Winder memory care community and our Winder senior assisted living community are proactive. That means we are not waiting for a problem to arise. Instead, we are actively engaged with every resident. We warmly extend our invitation to come see it all for yourself. We are confident you’ll find it to be a warm experience!
21 August 2023

Welcome back to our Winder-area assisted living community and our Winder memory care community’s blog. We manage this blog on behalf of our cherished residents, their families, and of course for you Winder-area homecare heroes taking care of your assisted living and/or memory care loved ones. Today, we hope you might benefit from learning how music can be used as therapy for your memory care loved one.
Music is a powerful art form. Melodies and rhythms can resonate with us on profound levels. That’s because music operates on a subconscious level, gently stroking our emotions as we listen.
Because certain tunes and beats can have an undeniable influence on our feelings, music therapy can be used to help us connect with our emotions and engage with the world around us.
Music therapy can be particularly beneficial for older adults living with dementia.
The magic of music lies in the way it boosts our brain’s neuroplasticity, which is what allows it to change and grow.
The benefits of music therapy and dementia are well researched. Experts tell us that music is processed in several areas of the brain — and by using different pathways to transfer and store information, the memories it conjures are vivid and clear. This positive experience can help ease worry, calm anxiety, and even improve communication.
Memory is like a file cabinet where information is organized and stored for later reference or use. That information includes sights, sounds, tastes, and smells, and those senses play a significant role in our ability to recall specific memories.
Within that ‘file cabinet’, music stimulates the brain’s reward system, releasing healthy doses of “feel-good” chemicals such as dopamine, serotonin, and oxytocin. This can make the retrieval of older memories an easier task for someone with Dementia by stimulating the mind in ways that improve cognitive function, including memory recall.
Consistent stimulation like this means that the benefits can extend beyond the confines of treatment plans and become ingrained in daily life.
Music therapy is all about jumpstarting the brain. For example, rousing music that features fast-paced, immersive beats engages the mind in a way that increases awareness.
But not everyone responds to music the exact same way, and there are different ways to kick the mind into high gear. Some are participatory while others are passive — it’s all about finding what works best for each individual.
Here are three types of music therapy for dementia that work well within a memory care community.
Group Singing
Singing — or Vocal Intonation Therapy (VIT) — uses the power of language and speech to foster orientation. It grounds the participant and gives them a sense of stability in a world that can often feel off-kilter. In addition, group singing (or circle choir) challenges the mind to recall words, phrases, and rhythms in a way that also encourages community and collaboration.
Ensemble Instrumentation
Playing a musical instrument can release stress, and each instrument seems to have its own unique additional benefits. Some are soothing, while others energize the musician. Drumming, in particular, can help patients release anger and frustration in a way that’s healthy and safe for others.
Live Musical Performances
Research shows that musical activities of all varieties (including listening) can influence older adults’ perceptions about the quality of their lives. Simply sitting back and listening to music engages the brain and can reduce anxiety, blood pressure, and pain — as well as improve sleep quality, mood, mental alertness, and memory.
Some of the most effective therapies are simple to accomplish. Give music therapy a try because you both will be rewarded by so doing. As always, remember that when it comes time to enjoy the life changing benefits of professional assisted living services or professional memory care services, we’re here for you.
14 August 2023

Welcome back to our Winder senior assisted living and memory care blog!
According to the Centers for Disease Control and Prevention (CDC), loneliness and isolation are connected to serious health problems. A national Academies of Sciences, Engineering, and Medicine report found that nearly one-fourth of people over age 65 are socially isolated.
The risk increases the older we get because elderly people are more likely to experience chronic health conditions, hearing loss, and the loss of loved ones. All these factors impact socialization.
Seniors who are isolated or lonely have a significantly increased risk of premature death. They are also more likely to suffer from anxiety and depression. Suicide rates are higher in this demographic as well.
Heart failure patients who are experiencing loneliness are nearly four times more likely to pass away and have a 68% increased risk of hospitalization. They are also 57% more likely to need to visit the emergency room.
The best way to combat these concerning issues is to build a thriving social circle and stay active. Gateway Gardens Assisted Living and Memory Care here in Winder welcomes new residents with many opportunities to meet new people. What can a senior who just moved into assisted living do to start building their social circle?
Be Friendly and Approachable
If you want to welcome new people into your life, you must give them an open door to enter through. That means being friendly and approachable.
Moving into assisted living can lift many of the burdens that come with aging and independent living. Some seniors have been dealing with their own struggles for a long time, so it can be difficult to adopt a more positive mindset.
If you struggle with this, it may be helpful to schedule time with a therapist. They can help you adapt to assisted living and find ways to be more approachable. Not only will it help you connect with more people, but it can also guide you toward a happier, more fulfilling lifestyle.
Get to Know the Staff
Getting to know the staff will make it easier to go to them when you need help or have questions. The staff may also be able to direct you to social opportunities or introduce you to other residents who share your interests or experiences.
Mingle in Common Areas
Our residents enjoy numerous common areas where fellow resident friends share fellowship. Join in a game of cards, watch a movie, enjoy the sunshine and wildlife, or simply breathe the fresh air.
Check Out the Events Calendar
Our community publishes a calendar of events. Find something that you enjoy and join in. Our Winder assisted living community provides many opportunities for fun and engagement among residents.
Try Something New or Learn a Skill
New things seem scary sometimes, but they can push us to learn more about ourselves. Being open to new experiences also helps us reach out to more people. Try a new activity or learn a new skill to enrich yourself and extend your social circle. Many colleges offer perks for senior citizens. In some cases, you could get free tuition. Check out local schools or look for online classes.
Even if you attend class remotely, learning something new could help you connect with the people you see in person. You may convince a neighbor to enroll in a class with you, so you can learn together.
Eat Meals with Your Neighbors
Human beings have used meals as a reason to socialize for thousands of years – and it still works well today! That’s why you should make a point to join your neighbors for mealtimes as often as you can. Being able to eat together is one of the social benefits of living here in our assisted living community.
Plan a Housewarming Party
Organize a gathering in your new home. This is also one way loved ones can help seniors build their social circle. Plan a housewarming party and invite your closest neighbors. It doesn’t have to be an elaborate affair. Create a place where you and your fellow residents can gather and get to know one another.
You can also look for icebreaker games that will help you ease into conversation and find common interests.
Connect with Other New Residents
Find other new residents and get to know them. You will already have some common ground being new arrivals. You can learn and explore our community together, and possibly bond over these shared experiences. As you become more acquainted with your community, your staff, and amenities, you can use this knowledge to help seniors who move in after you. You may not be the newest person anymore, but you can help support others and make new friends in the process. This can also help you feel a sense of purpose, which is an essential component of good mental health.
Be Patient with Yourself and Others
Remember to be patient with yourself and others. Building a strong social circle isn’t something that happens overnight. It takes time to find compatible people and form a bond of friendship. Moving into assisted living may seem overwhelming at first, so be patient with yourself. Give yourself time to adapt and be open to making friends, but don’t rush it.
Socialization is the key to preventing isolation and loneliness in senior citizens. Here at Winder’s Gateway Gardens Assisted Living & Memory Care, we encourage all our dear residents to actively socialize. It warms us all to witness how active our residents’ families are in helping their loved ones adapt and meet new people. We’d love to meet you. Stop in anytime!
7 August 2023

Greetings and welcome back to our Winder senior living and memory care blog. When an elderly parent or family member is living independently, there will come a day when you can’t escape the reality that their well-being is at risk. As time goes on, your loved one may require additional help for their health and safety. However, trying to decide whether it is time to transition to assisted living is not always easy.
As a trusted provider of assisted living in Winder, today we will discuss three of the most common signs indicating the need for assisted living:
Declining Health
According to the National Council on Aging, about 80% of older adults have at least one chronic condition, with nearly 70% of them having two or more. The presence of a chronic illness can cause your loved one’s health to deteriorate as they get older. Instead of trying to manage your loved one’s condition on your own, it may be time to escalate their needs with an elderly care provider.
Changes in Personal Hygiene
A decline in hygiene could be due to self-neglect but may also be caused by the inability to perform essential self-care tasks. Signs of poor hygiene include unkempt hair, stains on clothes, or unpleasant body odor. Additionally, other signs of self-neglect include unsanitary living conditions, weight loss, and poor medication management.
Social Isolation
Social isolation in seniors poses serious health risks. This includes heart diseases, high blood pressure, and cognitive decline. With assisted living, seniors gain regular opportunities for social interaction to enrich their lives.
Gateway Gardens Assisted Living & Memory Care is the place to go for those who need high-quality support from compassionate, qualified specialists. To provide comprehensive support, we offer personalized care that includes memory care services here in Winder as well.
Stop by and let’s talk about your concerns for your loved one and how professional assisted living services can serve both you AND your loved one. It very likely will give you peace.
31 July 2023

It is never easy to make the decision to transition a loved one into an Alzheimer's care community. You'll be forced to grapple with tough questions like, "Is it the best decision for my loved one?" and "Will the quality of care be worth the cost?" Once you have a clearer idea of the broader picture, you'll be able to make a more informed decision on Alzheimer's care.
To help you make the wisest decision for your loved one's future, we've rounded up some of the top benefits you and your loved one gain from a Winder memory care community like ours.
Here are a few of the top ways that your loved one benefits from residential memory care services.
Improved Quality of Life
You know exactly the kind of toll that Alzheimer's has had on your loved one. You've witnessed the decline of their cognitive abilities and how their life has changed. Fortunately, a memory care home can significantly improve their quality of life.
Within their community, your loved one will receive personalized care services to benefit their everyday life. Not only will they receive the nurturing benefit of one-on-one care, but they'll also experience fewer injuries, participate in more engaging activities, and feel more connected with the community around them.
Independence In a Safe Environment
Our memory care community goes to great lengths to achieve a delicate balance between resident safety and independence. Your loved one deserves to have the freedom to go about their days how they see fit without sacrificing their own security.
For that reason, our community leverages innovative security features to monitor resident safety while simultaneously allowing them plenty of freedom. For instance, here at Gateway Gardens Assisted Living and Memory Care in Winder, our community is outfitted with monitored exits and a secure backyard. Our residents are also free to go about their days at their own pace. Throughout any given day, residents can bake some goodies in the kitchen, relax in the living room with their favorite film.
Greater Socialization
One of the biggest concerns for older adults experiencing Alzheimer's or dementia is increased isolation. Loneliness may worsen their disease and contribute to the development of other serious conditions, such as depression. Fortunately, that's not the case in our memory care community!
Within these communities, there are plenty of opportunities for social interaction. These may include:
That daily socialization can make a significant difference for your loved one.
Specialized Support for Behavioral Issues
As experts at the Alzheimer's Association note, Alzheimer's disease and dementia can lead to a number of behavioral issues. These may include behaviors like:
We understand these are difficult and frightening subjects to consider. With that said, here at Winder’s Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
24 July 2023

Greetings once again to all our Winder-area assisted living and our Winder memory care community residents, family, neighbors, and friends. Today we’re going to share with you a few fun ways to stimulate cognitive health and have a lot of fun while doing it. Cognitive decline is a natural part of aging, but you can likely stave off and reduce some of the effects. Staying as sharp as a tack may be as simple as enjoying some games. Whether you play with fellow community residents, family, or online, brain games hold many benefits.
Since its invention, chess has been associated with brilliance and quick thinking, so it’s no surprise playing it helps support cognitive function. To win at a strategy game like chess, you have to compute many scenarios and recognize patterns in the gameplay. It’s likely that forcing your brain to practice in-depth computations and memory tasks like pattern recognition help stave off cognitive decline. Some studies even appear to show a correlation between playing chess and dementia prevention, but more research is needed to prove that connection.
With mobile chess apps, you can find opponents from around the world. You’re automatically paired with people of a similar skill level, so you’ll get the perfect balance of challenging but fun games.
Sudoku is all about analyzing. Trying to find the next number is like trying to find a four-leaf clover, and that concentration practice is generally considered good for mental function. Doing a sudoku puzzle is very similar to meditation. You sit quietly and focus on one thing for a duration, which is almost the definition of meditation. So analytical games like sudoku have many of the mental benefits of meditation.
There’s more and more scientific evidence being found that shows a correlation between the meditative state and slowing down the aging process in the brain. Specifically, meditators tend to have less grey matter loss than non-meditators. This could mean that solving meditation-inducing puzzles helps keep your brain sharper and younger.
Crossword puzzles generally deal with the cognitive function of recall. Since most crosswords have answers from many different categories, you must recall a large variety of information and experiences to solve them. This can help support memory and recall because it helps make new associations and pathways. And since crosswords require a limited answer that must fit into the puzzle, you don’t just have to recall an answer to the clue, you must recall all the answers to the clue until you find the one that fits. Crossword puzzles are the inspiration for many modern brain training games.
Also known as combination cubes, Rubik’s cubes are a fun brain game for people who like something more physical. They’re compact, so they make great traveling puzzles, and you can get a mental workout wherever you go. If you get bored of the classic 3x3, you can always challenge yourself by leveling up to larger cubes.
They likely help support cognitive function by helping your brain practice creating new neural networks. This happens because each time you try a new action to try to solve the puzzle, your brain has to keep track of what that action did. Playing around with these kinds of puzzles generally activates parts of the brain associated with this process, giving them a good workout.
A book of logic puzzles is a good place to stick your nose if you're looking for a mental challenge. Whereas most other brain game activities help support cognitive function by strengthening your brain, logic puzzles are about cultivating a learned way of thinking. These puzzles are usually some kind of riddle that requires you to think of a problem from a different angle. The skill of "thinking outside the box" is called lateral thinking, and learning it can make you feel like a genius. Lateral thinking teaches you to throw out unconventional solutions if they aren’t working and find more elegant ways to solve problems.
A study found that dementia was 15% less prevalent in seniors who reported regularly playing board games, but the reason for this might not be what you expect. The researchers think the correlation between playing board games and decreased mental decline is due to the smaller number of depression cases among board game players. So basically, they think board games make you happier and that helps support your cognitive function.
Board games generally aren’t as mentally taxing as games like chess, but they can still benefit your mental wellbeing and brain function. The fun and social experience of a board game connects you with others, which has shown to help decrease the risk of mental illness.
Recently, there has been an influx of brain training apps that generally compile many brain games into one place. They usually incorporate different types of cognitive skills and will "test" your acuity in each. The games they provide are fun and may help increase mental sharpness, but the apps often make a lot of unsubstantiated claims. It’s important to remember that these apps are not necessarily scientific and approach them with skepticism.
Gateway Gardens Assisted Living & Memory Care here in Winder is a vibrant, compassionate, and cheerful assisted living and memory care community. Come see us, anytime!
17 July 2023

Today five million people in the U.S. are living with Alzheimer’s disease and related memory loss, and as our population ages, that number will increase. Professional memory care support services such as those provided to our cherished residents here at Winder’s Gateway Gardens Assisted Living and Memory Care empower them to make the most of their remaining abilities. At the center of our professional caring hearts is the notion that every resident is who they are, and always have been. Like you, us, and all others, they’ve just moved on to another place, another chapter in life. And we cherish being part of their journey.
Studies reveal that people with dementia often feel excluded from everyday life, and this is largely due to the unfortunate stigma associated with the disease. Sadly, some people avoid a friend who’s been diagnosed with Alzheimer’s. Family, too, can experience the effects of this prejudice. “Friends and even some family members avoided me, and didn’t want to talk about my husband’s condition,” reported one wife. “It was just when we could have most used their support.”
This stigma is based on ignorance. Studies disprove so many myths about Alzheimer’s disease. For example, many people assume that people with dementia are miserable. Yet studies show many people with early-stage Alzheimer’s report having an improved outlook on life! While depression, denial, and despair might come with the diagnosis, many people studied expressed an appreciation and acceptance of life, lessened concern about failure, and strengthened relationships.
It’s important to fight this stigma, as we would any prejudice. Negative attitudes harm the quality of life and even stand in the way of a prompt diagnosis, and the best advance planning.
Change is possible. People with dementia and their allies are working to improve the attitudes of the public. More public programs and resources seek to support and meet the needs of people with dementia, and to create appropriate opportunities for people with and without memory loss to interact in ways that break down barriers.
A group of people in the Alzheimer’s Association National Early-Stage Advisory Group offered these suggestions about how people with memory loss can help combat the stigma:
Family and allies are also vital to fighting this prejudice! They can focus on their loved one’s remaining abilities and advocate for them with information, the best way to dispel prejudice. Here at Gateway Gardens Assisted Living & Memory Care, we attest that each resident is a unique individual. The goal of our community is to allow each resident to feel valued, safe, successful, peaceful, cared for, healthy, energetic, and loved.
10 July 2023

What makes our memory care team at Winder’s Gateway Gardens Assisted Living & Memory Care so good at their beloved profession is a both an innate and learned powerful shift in perspective. Our staff is innate in their perspective because this profession draws a loving and kind heart for our challenged seniors. Our staff also is empowered by a learned perspective where we work hard to see our resident from a different perspective than some family’s.
Some family perspectives are both predictable and understandable. Some see their cherished loved one as someone who is less than they once were. We view every single resident as a whole person with much to offer. It takes patience and compassion, but if you meet them on their level, and listen to what they are telling you, and accept them in that moment, then you will get so much more from them in return.
It can be very frustrating for family members, because they want so badly for their loved one to remember and to be like they were. We show family members how to let go of that kind of thinking, how to meet the person where they are today, which reduces anxiety and helps the person be all that they can be, today.
Helping families in their struggle with Alzheimer’s is a component of providing care to those living with dementia and related forms of the disease. Showing family members how to successfully redirect their loved one is another valuable tool shared by Isaac and her team.
For instance, if a resident tells us, ‘I need to go home, my husband or children are waiting for me,’ our staff is trained to never correct their perceived reality. Our loving approach is to reply in some form of, “Oh, I’d love to hear about your husband or your children, tell me about them”.
Another successful tactic is to get the person engaged in their favorite pastime, craft, or job-related skill that they performed fluently at some point in their life. Asking a man who worked as a contractor in his professional life for help with a simple mechanical task affords a sense of accomplishment and importance.
Of course, ours is a complicated profession. But it is simple at its core. We familiarize ourselves in depth regarding who our residents were. We accept and celebrate the person as they are now. And we seek to bridge their two worlds into a reality that inspires happiness.
Our mutual love and admiration for our seniors here at Winder’s Gateway Gardens Assisted Living and Memory Care binds you and us as a team.
26 June 2023

We’re glad to have you here on our assisted living and memory care blog and hope you find it useful. Through the kind feedback from you, our blog readers, we know we’re making a difference with our efforts. We received feedback about a blog post we did way back when regarding the importance of hydration, especially for seniors. We were asked by a kind lady if we might re-post it because she firmly believes that her newfound focus upon keeping Mom hydrated made a lasting difference in her energy and overall mental outlook. So, here’s a re-look at the important considerations regarding hydration.
With steadily rising outdoor temperatures, we thought it smart to cover the VERY important topic of hydration. Every bit of advice listed below should be considered advice for both you and your senior loved one. So here you go, seven tips to stay hydrated this summer:
Bonus for parents of young children out there
Our bodies are comprised of nearly 60% of water and kids are an even greater percentage. Every cell, tissue and organ in our body relies on water. For example, our bodies rely on water to regulate temperature, remove toxins, and keep our joints lubricated. When we talk about hydration, it means keeping the water levels in our bodies in a healthy range so we can function at our best.
You should drink half your body weight in ounces of water each day. (Ex: If you weigh 120lbs, you should drink 60 ounces of water each day.). One of the simplest ways to know if you’re drinking enough water is the color of your urine. In most cases, a well-hydrated person will have colorless or light-yellow urine. If it is dark yellow or amber, it may be a sign of dehydration. Another telltale sign you’re dehydrated. You’re thirsty. If you’re thirsty, you’re already dehydrated, and you need to pick it up!
Here at Winder’s Gateway Gardens Assisted Living and Memory Care, we take great pride in our holistic approach to managed care. We invest heartfelt time and energy managing this senior care blog for the purpose of assisting those of you at-home senior care providers to help you deliver the best care possible. We want all of you to consider us a ready resource for information and advice that is intended to help improve your quality of life as well.
We’re glad to have you here on our assisted living and memory care blog and hope you find it useful.
19 June 2023

Transitioning into an assisted living community like ours here in Winder can (and should) be a welcome and exciting chapter in life. Your new community will be filled with newfound freedom and the luxury of time. But for some, this transition can also bring an unexpected sense of loneliness and isolation, especially for those living alone. Thankfully, a retirement community can be the antidote, offering an engaging social environment, meaningful connections, and a host of activities to keep your days filled with joy and camaraderie during retirement.
One of the greatest benefits of living in either our Winder senior assisted living community or our Winder memory care community is the sense of just that, the community it fosters. Here, you are part of a family of like-minded individuals who share similar life experiences. From friendly neighbors to compassionate team members, you’ll be surrounded by people who genuinely care about your well-being.
Regular community gatherings, such as seasonal celebrations, local heritage celebrations, holiday celebrations, and birthday parties offer plenty of opportunities to mingle and form lasting friendships. This sense of belonging can significantly alleviate feelings of loneliness and contribute to your overall happiness.
Boredom can often lead to feelings of isolation, but in a vibrant assisted living community there’s always something exciting happening! We understand that everyone has unique interests and hobbies, which is why we offer a diverse array of senior living activities to cater to different tastes.
Whether it’s joining a book club, taking up a painting class, or participating in fitness activities, you’ll find plenty of options to engage both your mind and body. These activities not only keep you active but also provide a great platform to interact and connect with others.
While nothing can replace the warmth of a face-to-face conversation, technology can bridge the gap when physical presence is not possible. We offer tech-support to help residents stay connected with their loved ones. This could be through teaching you how to use video calling apps, or arranging virtual family meet-ups. Through technology, you can share your experiences with family and friends, no matter the distance.
Perhaps one of the most comforting aspects of living in an assisted living community is the availability of support when you need it. Whether you need help with a health issue or just need someone to talk to, the community team members are there to assist. We offer counseling and mental health support, understanding the importance of emotional wellbeing in preventing social isolation.
Finally, a senior assisted living community offers the freedom to be yourself. Here, you can pursue your passions, engage in your favorite pastimes, and enjoy your retirement exactly as you see fit. By providing an environment that encourages individuality and personal growth, a retirement community can ensure that your golden years are truly fulfilling and far from lonely.
Gateway Gardens Assisted Living and Memory Care here in Winder delivers a profound positive living and quality of life enhancing experience. Come see it for yourself!
12 June 2023

We pride ourselves here at Gateway Gardens Assisted Living & Memory Care (Winder) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Winder who lovingly provide at-home assisted living care and/or memory care support to your loved ones. Today we’re going to discuss ways to celebrate our fathers in advance of the Father’s Day weekend. Some families have traditions on this day. Others love variety from year to year. No matter what you do to celebrate Father’s Day, the most important aspects for most are to honor your dad and spend quality time with him.
Here are some innovative ways to connect with your father this year.
Above all else, if at all possible, just physically be there with him. For the vast majority, you really need not worry about any of the things suggested above. He’ll be happy to simply “wing it” with you. Happy Father’s Day, to all our dear dad’s here at Gateway Gardens Assisted Living community and our Gateway Gardens Memory Care community!
5 June 2023

One of the truly rewarding aspects of serving our senior assisted living community and our memory care community is chatting with visiting family, friends, clergy, and all other kind souls that visit us on a daily basis. Those engagements are rewarding to us personally, but more importantly, they are teaching moments about what might be top-of-mind thoughts within the minds of our cherished residents. Those insights help us to connect with your loved ones in a deep and more meaningful way.
So, on behalf of our entire staff and your loved one under our care here at Winder’s Gateway Gardens Assisted Living and Memory Care, thank you for spending time with us and sharing our stories.
29 May 2023

Our focus for today’s senior assisted living and memory blog post is for you, the friends and relatives of our cherished memory care residents here at Winder’s Gateway Gardens Assisted Living and Memory Care.
If you are hesitant to visit a friend or relative with significant memory care issues because you’re intimidated about what to say or how to act, listen, you are more the norm than the exception. We routinely address these concerns with our visitors here and thought to put the recurring suggestions down on paper as food-for-thought prior to your visit. If you read no further than this paragraph, our advice is simply walk in and take earned reward for prioritizing time for those you love.
Some things will come easy and naturally. Possibly, things could get uncomfortable. Whatever happens, consider the following in advance:
Understand that you likely will not be able to have the same kind of conversations with the person as you did in the past. If they forget something you just told them, avoid correcting them or saying things like, “We talked about that just a few minutes ago. Don’t you remember?” Chances are they genuinely don’t.
A better response is to acknowledge what they’ve said and then casually change the topic. Let go of the desire to correct them. It’s not going to help them, and it’s likely only going to frustrate you. The sooner you recognize that expecting them to behave “normally” is an unproductive exercise, the more likely you’ll have a successful visit.
OK, if you disagree with this outright, we totally get it. But these are the rare circumstances where, in our opinion, that it’s perfectly okay not to tell the truth, particularly when the truth is destined to be upsetting. It’s best to say things that comfort rather than distress the person, even if it means telling little white lies.
A common question you might be asked relates to when their deceased spouse is “coming home”. Expect hard questions like that in advance and develop a philosophy about how you will react. “He went out for lunch. I’m not sure when he’ll be back”. Now your friend is picturing her husband at a restaurant and not in a casket. Isn’t the former a more productive and loving approach?
People with dementia are often at their best from mid-morning to early or mid-afternoon. After that, they may be prone to restlessness and confusion, a phenomenon known as sundowning. Not everyone follows the same pattern, though. Keep in mind that most individuals with dementia tend to get tired later in the day, so dropping in for supper may not be the best option.
If your experience confirms that sitting and talking is difficult, spend time doing an activity together when you visit. Bring a book, pictures, or music you know that she enjoyed once upon a time. All of these things can be triggers for happy and rewarding experience.
If your visit doesn’t go well, don’t be discouraged. Just because the person gets agitated or restless does not mean the visit is counterproductive. Take it as a learning lesson regarding what not to say or do. Simultaneously, take note of what words and behaviors triggered positivity. Over time, the positive and rewarding minutes will far outpace the uncomfortable minutes.
Here at Gateway Gardens Assisted Living and Memory Care, we provide support for people with dementia and their families every day. We embrace the days (for us, always good) with our residents. Like you, we take notes, we learn, and our memory care residents’ days get consistently better. Even if they don’t recognize it.
22 May 2023

Are you or a loved one considering professional assisted living services or professional memory care services here in Winder? While there are many factors to consider when making this decision, one that can't be overlooked is the proximity of family and friends. Being close to loved ones can provide emotional support, socialization, and a sense of familiarity with the local community. Plus, it makes visits and outings much easier and more convenient. In this article, we'll explore the benefits of being close to family and friends who reside within managed care communities.
Benefits of being close to family and friends in our assisted living or memory care community here in Winder NC:
Choosing an assisted living facility near family and friends is a smart choice for seniors. It offers emotional support, socialization, and familiarity with the local community, which can lead to a happier and healthier life. Moreover, the proximity of the facility to medical centers and emergency services, as well as the affordability and cost of living in the area, are also important factors to consider. Gateway Gardens Assisted Living and Memory Care is excellent option for seniors who require specialized care for memory impairments. Our community provides a safe and comfortable environment, with personalized care plans and round-the-clock assistance from trained staff. Its convenient location and accessibility to medical facilities and transportation options make it an ideal choice for families seeking quality care for their loved ones.
Contact us today!
15 May 2023

Memorial Day weekend is just around the corner. While Memorial Day signifies the start of summer to many, to those who have served our country or have a loved one that fought and did not come home, Memorial Day is a sacred day of remembrance.
Here at Gateway Gardens Senior Assisted Living and Memory Care, we have accomplished veterans living among us who have fought heroically for the freedom we enjoy and often take for granted. Individuals from the Greatest Generation and those that followed, who have endured many hardships with astonishing resilience.
Please remember to take time to honor and remember those who have faced the ravages of war and sacrificed their own lives for our country. Realize that the living senior veterans within your life and those around you very likely suffered the combat loss of good friends and fellow combatants. Remember that Memorial Day is tough for so many of those that served. Memorial Day can (and should) be a day when we are there for them. They certainly were for us.
With heartfelt thanks, our Gateway Gardens senior assisted living staff and our memory care community staff here in Winder remembers all the men and women who have bravely served our country.
8 May 2023

Many older adults plan to age independently but are ultimately forced to make decisions about their care as their health and physical independence decline. According to the Pew Research Center, nearly 12 million Americans over the age of 65 live alone. At some point, together with their aging parents, adult children must decide whether to bring in outside care, rely on a family member or investigate assisted living. Our senior assisted living community is designed for older adults who need additional support in their day-to-day lives. This often includes bathing, housekeeping, preparing meals, managing medications, and assistance with transportation and medical appointments. For many adult children, assisted living placement can evoke feelings of shame, apprehension, and guilt. However, these feelings are common and can be dealt with in positive ways.
Choosing to move your loved one into an assisted living community can be one of the hardest decisions to make for your parents. Whether you’re a caregiver who needs additional support, lives long-distance, or is an adult child managing your own life, choosing an assisted living community does not equate to failure. Many family members may experience feelings of guilt and sadness, but also a relief. Working through these feelings can help you feel more confident about the decision and focus on your loved one’s care without feeling guilty. Here are a few ways to cope with this unfounded guilt:
Understand you did not cause the illness. If your loved one is dealing with a progressive condition such as Alzheimer’s disease or Parkinson’s or is declining physically, they would still have to deal with their declining health even if you were able to care for them at home. Moving your loved one into our memory care community doesn’t mean you’ve failed to take care of them. It means they’re getting the care they need to live a life of dignity while receiving high-quality health care in a safe environment.
Acknowledge your efforts. Being a primary caregiver for a parent is a huge undertaking. Making decisions in situations you’ve never encountered before can make you feel like every decision made is a bad one. However, it’s important to acknowledge your efforts and understand you’re doing the best you can in a difficult and emotional situation.
Assess your options. Most older adults are resistant to the idea of transitioning into assisted living communities. However, assisted living offers high-quality support to both older adults and their family members. Doing your research, touring facilities, and asking important questions can leave you feeling more confident about the facility you’ve chosen. This is important and we point this out in confidence that the more you learn about your options, the more you’ll come to value our service offerings here at Gateway Gardens Assisted Living and Memory Care.
17 April 2023

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. Most older adults know the day will come when it’s time to downsize. But no matter how realistic you are about the necessity of downsizing — or rightsizing, as it’s sometimes called — you probably also realize that the process will be an emotional one. To help you get through the transition without feeling overwhelmed, here are some suggestions for dealing with the emotions of downsizing:
Moving out of your home is stressful — and daunting. But it will be even more overwhelming if you don’t acknowledge the emotional toll the process can take. Give yourself time to pause and experience the emotions that come up. Cry if you feel like it. And allow time to reflect on any memories that arise as you sort through your belongings. Consider reaching out to friends and loved ones to reminisce or talk about some of the memories that are surfacing.
Just as you need to acknowledge your feelings of grief and nostalgia, it’s also important to keep in mind the good reasons you have for downsizing. Your next home may be smaller, but it will be better suited to your lifestyle and future needs. The vast majority of older adults who move to a senior living community like ours are happy they made the transition. Our dear residents have none of the responsibilities of homeownership but enjoy countless opportunities to make new friends, explore new activities and enjoy fresh adventures.
You’ll have a greater sense of control — and less anxiety — if you have a plan. Make a list of tasks you need to accomplish and then grab your calendar and start working out a plan of action. Be sure to give yourself plenty of time. It’s best to start months ahead of your move date to avoid the stress of having to rush through the project. As your plan takes shape, include goals for each day so you can keep the project moving forward. Also let friends and family know when you’ll be needing their help, so they can arrange to be available.
It can be tempting to dive into the most challenging rooms first, but you’ll gain confidence and momentum if you start with an easy space like the laundry room or linen closet. As you progress, you’ll develop a system of sorting and packing, so you’ll be more prepared for the rooms that are filled with old memories or sentimental favorites.
Self-discipline is necessary and admirable, but when you’re tackling emotionally difficult tasks it’s important to be kind to yourself, too. Give yourself treats — a cup of tea or a phone call with a friend — after you’ve finished a particularly onerous duty. Invite friends and family to participate in the project. You’ll benefit from the companionship. Plus, sharing stories as you sort through belongings can help you process your feelings and remind you that you have support when you need it.
As you consider which items to bring with you, give yourself only two options: yes or no. If you allow yourself to set items aside with a “maybe,” you’re only postponing the decision. To help you decide, ask yourself if the item is necessary or if it makes you happy. Your bowling trophies, for example, probably aren’t necessary, and they may stir feelings of nostalgia without making you joyful. In such cases, taking a photo can make it easier to rehome once-cherished items.
In dealing with the emotions of downsizing, it can be helpful to remind yourself why you’re making this change. Downsizing your home is a way to right size your life. Here you’ll have the comforts of home, a community of new friends, and the services and amenities that support a flourishing lifestyle. Contact us to find out more about senior assisted living services and memory care services here at Gateway Gardens.
12 April 2023

Our senior living and memory care blog team considered changing the title of this blog post to: “Legal Documents Every Adult Should Have”. The focus of this blog clearly is not limited to our beloved Winder senior living community and our Winder memory care community, however, on average, the urgency for senior and their families to heed the advice here is heightened. So, let’s get right to it.
One of the most challenging times for a family is when a loved one transitions from this life. Heightened emotions from grief can often bring the best and the worst out in others close to you. Knowing in advance what your loved one wants regarding funeral arrangements, finances, medical wishes, and how to distribute any assets and personal or sentimental items is a blessing and gift to those you love. There are legal documents that can help make wishes known and every senior should have in place. Having them in order will help give your loved one the confidence that their wishes will be honored, help alleviate stress and unnecessary family arguments, and ultimately save time and money.
We list five documents below that every senior should have. One of the highest value services you might enjoy (if you haven’t already) is to secure the services of an elder care lawyer who will work to protect both the senior and their family from legal perils. Whereas we don’t promote any lawyer or lawyer group, online search for such services should produce several resources for you to consider.
Here are the basic documents you should familiarize with and strongly consider establishing:
So, to be clear, we offer this with the goal to get you thinking about important elder legal care responsibilities. Please, if ever there was a need to seek the consult of knowledgeable professionals, in our professional opinion, senior legal consultation ranks right up there.
For more information, we openly invite you to contact us anytime here at Winder’s Gateway Gardens Assisted Living & Memory Care.
3 April 2023
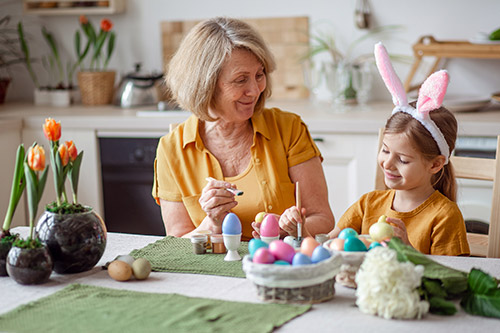
With the sun out shining bright and winter starting to loosen its grip, it’s the best time to celebrate spring and Easter! Just like any other special occasion and holiday, it is possible to keep up your favorite Easter traditions here in our Winder senior living and memory care community. If you have a loved one who lives in a retirement community, remember to extend the special traditions to include them as well. Spending time with your loved ones is the best part of celebrating the holidays and everyone appreciates feeling loved. Read on to learn more about how to celebrate this Easter with your senior assisted living or memory care loved one.
Our community does a fantastic job of planning holiday events and activities for our residents. Check with our activity director to see what activities are available. Invite your family or friends to share in the event or have a meal together.
Maybe you used to color Easter eggs, bake cookies, or volunteer at a local charity every year. There is no reason why you can’t continue these old traditions. Keep up the treasured tradition so you can feel at home.
A new living situation is a perfect opportunity to create new Easter traditions with your neighbors, friends, and loved ones. You can come up with some easy and fun activities to do together such as dyeing Easter eggs or decorating Easter baskets. Gather to share memories while making new ones.
Take the opportunity to get outdoors for a nice walk. Go for a stroll with a family member or friend and enjoy the beautiful weather and promise of the new season.
For many people of faith, Easter is one of the most important holidays of the year. Take your senior loved on with you to Easter service. This can in fact be a huge gesture to them.
Manor Lake Assisted Living and Memory Care is a world-class living and care experience. You and your cherished family member will superb living, medical, and social opportunities. Our residents wake up feeling excited for the new day. They can take part in a full schedule of fun activities, and they also get to use the excellent amenities. Here is where you can live a fulfilling lifestyle. Feel free to contact us for more information.
27 March 2023

Hello everyone from your friends and neighbors here at Winder’s Gateway Gardens Assisted Living and Memory Care. If you’re struggling with aging parents who refuse your best efforts to help, you’re far from alone: A whopping 77% of adult children believe their parents are stubborn about taking their advice or getting help with daily tasks.
None of the things we offer here will be viewed as earth-shattering new discovery, but sometimes we all need a gentle reminder of smart habits that can get clouded in the storm of frustration.
As providers of professional assisted living services or professional memory care services, we are your biggest fans. We know your challenges, your frustrations, and of course the comfort and rewards for the loving care that you provide. May strength, patience, and happiness find you all!
20 March 2023

Hello to all our blog fans here at Gateway Gardens Assisted Living & Memory Care here in Winder. Today we return to a FAQ, a subject that we’ve covered before, and a topic that is understandably stressful for both our seniors and their families. Transitioning to managed care means saying goodbye to a home that’s comfortable, familiar, but may no longer be safe. A high percentage of new residents and their family members here within our senior assisted living community contemplated moving for months. They did this for good reasons. Transitioning from independent living is without doubt one of the most difficult decisions anyone will ever make.
Our advice is to acknowledge these feelings but to also focus on the positive aspects of moving. It’s also important to seriously evaluate and consider your current and future needs. Some reasons why considering a move might be the right choice include:
15 March 2023

Welcome back to our blog page associated with our Winder-area assisted living and our Winder memory care community. We’re also here for you Winder-area homecare heroes taking care of your assisted living and/or memory care loved ones. If you looking for ideas on how to celebrate St. Patty’s day with your loved one, we have some ideas for you!
St. Patrick’s Day is the traditional holiday that we will celebrate on Friday, March 17, in honor of St. Patrick, the patron saint of Ireland. While it’s an Irish celebration, it’s a huge occasion in many cities and towns all over the world. While some of these parties tend to get a bit rowdy, there are lots of ways for seniors to get involved in the festivities and have fun with friends and family.
One of the best ways to celebrate the day in a family-friendly way is to enjoy some classic Irish cuisine. Gather a small group of friends and family or organize a big potluck-style dinner and have everyone prepare an Irish-themed dish. Make the party extra festive and decorate with lots of green – napkins, placemats, and centerpieces. (It wouldn’t hurt to add some gold in there too!)
Create a menu with Irish themed appetizers, drinks, and dinner. Need some ideas? A few classic Irish dishes to try include soda bread, corned beef, Irish stew, and colcannon. (Or you can also just stick to food with lots of green!) Be sure to include some green drinks and desserts for an extra festive touch!
Whether you decide to have a few friends over or throw a big dinner party, some fun St. Patrick’s Day decorations are always a good call. (This is a great way to get kids involved too!) Get in the spirit by creating some fun Irish themed decorations. Keep it simple and cut out some paper shamrocks to place around the room or make green paper shamrock crowns for everyone to wear. If you plan on having a party, you can create centerpieces for a snack table, or some cute shamrock pins for just a touch of green. Check out these St. Paddy’s craft ideas from Martha Stewart for some inspiration.
Some St. Patrick’s Day parades are known for getting a little wild, but there are plenty of family friendly celebrations around. Many communities have a traditional parade, which is a great way to immerse yourself in the fun of the day. There’s always something fun to watch, including plenty of music and dancing! Really get in the spirit and wear a fun, green-themed outfit to the festivities. (This is a good idea if you want to avoid a friendly pinch for not wearing green!)
Irish traditional dance is a big part of most St. Patrick’s Day celebrations. The lively and energetic steps are always exciting to watch, but they’re even more fun when you do them yourself! If you happen to know a skilled Irish dancer who can teach you some steps, that’s always a bonus. However, you don’t really need lessons in order to do a jig. Simply put on some traditional Irish music and get moving. Dancing is a proven mood booster, and it’s a great way to get some exercise while having a blast.
Add a fun twist and change up your regular game night. For large groups, Lucky Bingo is a great way to add some St. Patrick’s Day fun into the mix. It’s easy – take a classic bingo card and replace the top letters with L-U-C-K-Y. Use green bingo dabbers for an extra festive touch and decorate the cards with stickers. It’s sure to be an exciting game with the luck O’ the Irish on your side.
Celebrating St. Patty’s Day with your senior loved one need not be complicated or stressful. There’s real simplicity in all the ideas presented above. As always, remember that when it comes time to enjoy the life changing benefits of professional assisted living services or professional memory care services, we’re here for you.
8 March 2023

Welcome back to our assisted living and memory care blog here at Gateway Gardens. As we get older, we start reaching for sweaters more often, shivering (even when you think you should be warm), or maybe turning up the thermostat more often than not. Is it really getting that much colder every year, or is it something else?
As we get older, we often feel colder at temperatures we were once comfortable. There are a few causes of this, including thinning skin, slower blood circulation, or even side effects of medication. Age isn’t the only cause of feeling colder. It can also be related to several medical conditions such as anemia or even diabetes.
It can even be your own residence contributing to the problem. With the rising costs of heating and other bills, many seniors find they’d rather wear a sweater and be a little cold rather than turn up the heat to a comfortable temperature. But this can risk hypothermia or other temperature-related issues and lead to other problems.
Professional assisted living services is an option to consider if any of this sounds familiar. Being in a community like ours here at Gateway Gardens Assisted Living and Memory Care here in Winder gives you the option of being surrounded by a caring team that can help with medical concerns and daily needs. And, you get to avoid most utility fees, so you can dial up that heat and be as comfortable as desired! And we want you to feel comfortable calling us anytime for advice!
6 March 2023

Greetings once again from your Winder-area assisted living and Winder memory care community here at Gateway Gardens. Dementia changes lives and introduces new challenges seemingly on a daily basis. Dementia changes the way a person thinks and feels, and it changes the way a person makes even the smallest decision. Dementia has a major impact on how one lives, and can make many mundane activities surprisingly difficult. The same can be true for caregivers. If you are a caregiver for someone with dementia, just take it one day at a time.
Here are a few tips to make those daily tasks easier:
Sometimes a sensible schedule helps to minimize anxiety for a person with dementia. A schedule helps most people feel comfortable because there are certain things they can count on at certain times. You don’t have to schedule every little thing but learn what specific daily tasks are most important to schedule and try to do those tasks with your loved one at a time that works for them as well as for you. This could include bathing and other grooming activities as well as eating or going for walks.
A person with dementia may not be able to communicate with you the way they used to, but when you are spending time with your loved one, pay attention, offer them support, and patiently explain what you are doing and why. It will help eliminate anxiety for them and will also help you become a better caregiver.
Many caregivers make the mistake of depending too much on television or other distractions but people with dementia may benefit more from focusing their attention on you and the daily tasks you are doing together. Similarly, it might help to remove clutter from your house to make it a safer place for your loved one and to reduce the possibility of their getting anxious.
You have access to quality senior care communities like us here at Gateway Gardens Assisted Living and Memory Care. Send questions into us anytime!
27 February 2023

We hear horrible stories from at-home care providers concerning an elderly loved one who was short-changed or downright scammed, financially or otherwise. Our caring professionals here at Winder’s Gateway Gardens Assisted Living & Memory Care feel it is important to remind you that con-artists and scammers lurk, and you must be on guard. So, let's cover the basics of protecting your senior loved one from scams.
Con artists will charm elderly victims by phone with an affable “nice guy” approach. Deceptive and dishonest, this tele-trickster is the last person you would want to invite into your home! You’re right if you guessed… he’s a con artist! Americans lose an estimated $40 billion each year due to the unethical activities of fraudulent “salespeople.” Advise your senior, if they are called, emailed, or text for subjects they have not actively requested information on, then hang up on that caller.
Encourage your senior loved one, as a standard practice, do not reply to any email, voicemail, or text offers. Their standard practice should be to share those things with you first. If it is a voice call, their standard practice should be to either hang up or to direct them to call back when you (my daughter, son, etc) is going to be with you. Scammers won't make that call. Legitimate agencies will.
If you have any questions or concerns regarding how to provide fraud free loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Winder.
22 February 2023

Welcome back to our assisted living and memory care blog here at Gateway Gardens. As your parent or other loved one ages, you almost certainly have worries about their health and wellness. For many, conditions like Alzheimer’s disease, dementia, or other memory issues are a top concern because of how common they are in older adults. According to the World Health Organization (WHO), a new case of dementia is diagnosed every three seconds.
Dementia is a broad term that can include many changes to memory or the way the brain works. And, while we don’t know all causes of dementia, studies continue in an effort to find risk factors and ways to prevent it. These studies help show areas where your parent could reduce his or her chances of getting the disease.
Your parent can’t control some risk factors – such as age, another related condition, or genetics. However, you may find areas where you can help your aging parent make changes for the better. For example, a study recently showed loneliness linked to risk of dementia.
In the study, researchers surveyed 12,000 people about their loneliness, social isolation, behavior, and genetics. They defined loneliness as “a feeling that you do not fit in or do not belong with the people around you.” After collecting this initial data, they followed each person over 10 years for signs of dementia.
In 2018, The Journals of Gerontology published results from the study. Over the 10-year period, those who reported their current status made them feel socially isolated were much more likely to have developed the condition. Overall, the study concluded that loneliness increased the risk of dementia by as much as 40 percent.
This recent study isn’t the only one to find a link between dementia and feeling lonely. In 2015, another study published in Ageing Research Reviews found a link between dementia and factors like low social participation or less frequent social contact.
If you’ve noticed signs that your mom or dad is more socially isolated, don’t be afraid to offer support. By talking about feelings of loneliness, you can help avoid its health effects.
When it comes to fighting loneliness, consider how your aging parent’s location affects social interaction. How far is mom or dad from others at a similar life stage? Are there activities nearby for seniors? If you’re aging parent can’t drive, does this cause a problem?
Often, when your parent lives in a location that provides ample social events, it helps to reduce isolation. Our assisted living community and our memory care community offer a wide array of activities for our residents. Research and our entire team of professional care providers here at Gateway Gardens Assisted Living and Memory Care can’t emphasize enough the importance of daily contact with peers.
13 February 2023

Well, it’s “all hands on deck” time for your Winder senior assisted living blog team as well as your Winder memory care blog team here at Gateway Gardens. We’ve left our computers and are now busying about to brighten our communities in preparation for Valentine’s Day. Our beloved seniors and memory care are going to be pampered and enjoy the special love that defines what Valentine’s Day is all about.
You may associate Valentine's Day with young love - after all, most films and books are full of stories about young couples finding their happily ever after. However, there's a whole lot to be said for spending Valentine's Day with seniors! A day spent with your grandparents or elderly friends can do wonders for both the heart and soul. It's important to involve seniors in the celebration and show them that they are still important and loved.
So, if you are traveling here to spend Valentine’s Day with your loved one(s) here at Winder’s Gateway Gardens Assisted Living and Memory Care, we can’t wait to see you! If you are celebrating the holiday at home, then we celebrate the special time, thought, and energy that you plan to deliver to the seniors of your life. They certainly deserve it.
8 February 2023

Greetings once again from your Winder-area assisted living and Winder memory care community here at Gateway Gardens. As we age, our joints lose fluid and our muscles lose elasticity, leading to a natural decrease in flexibility. Seniors who lose flexibility find it hard to complete normal daily tasks like getting up from chairs or walking up and down stairs, let alone more complicated chores like cooking and cleaning.
The CDC recommends that adults 65 and older get at least 150 minutes of moderate activity each week to help with strength and balance. More specifically, routine range of motion exercises can strengthen muscles and maintain flexibility. At Gateway Gardens Assisted Living and Memory Care, we work with residents to ensure they remain flexible to avoid issues with tight muscles and injuries.
Our cherished residents here at Gateway Gardens thrive with help from our experienced nursing staff whose care services involve encouraging strength, balance, and range of motion exercises. We understand how these exercises can benefit our aging community members. Consider a few of the benefits:
Our assisted living services and our memory care services here at Gateway Gardens assess and address physical and cognitive limitations. We help our residents to thrive with research-proven care services as well as events to stimulate residents on an intellectual and emotional level. Our routine exercise programs give our residents the physical strength and dexterity they need to enjoy the many other programs we have to offer.
The residents of Gateway Gardens Assisted Living and Memory Care enjoy all that this beautiful location has to offer along with everything they need to live a safe, independent life, including chef-prepared meals, comfortable accommodations, entertainment and activities, and compassionate nursing staff.
We are currently accepting new residents, so don’t hesitate to reach out if you need excellent care at our memory care or our assisted living community. Call us today to learn more and to schedule a tour of our memory care assisted living community.
6 February 2023

Greetings once again from your Winder-area assisted living and Winder memory care community here at Gateway Gardens. Everyone ages differently and will have a specific set of physical and emotional needs. For many, mobility issues make it difficult to do things like pick up groceries and attend medical appointments, or they may have trouble with cooking and cleaning or basic tasks like bathing and taking medications. Even if a senior is physically healthy, memory issues like dementia or Alzheimer’s can create another set of challenges.
Whether your aging loved one needs a little bit of help to live with dignity or they’re struggling with everyday tasks due to memory loss, assisted living may be the answer. Take a look below at some of the main reasons people turn to our assisted living community and memory care community for the support they need to keep their loved ones safe.
Professional assisted living and memory care services provide a stable environment where your loved one can relax in familiar surroundings with a soothing routine. Routines are essential when it comes to Alzheimer’s care and dementia care in general, and we provide the memory care services needed to keep seniors with these conditions at peace. Furthermore, assisted living facilities are designed to allow seniors to be as mobile as possible while remaining safe, with single floor living and wide doorways. Features like handrails and accessible bathrooms help seniors avoid dangerous falls while allowing them to maintain as much independence as possible.
Our memory care assisted living community provides 24/7 care. Compassionate and experienced, our staff members can respond to emergencies at a moment’s notice.
Nothing is more important to us than the safety of our residents. We utilize internal and external safety protocols including a secure building access system, video surveillance, patient monitoring, and more.
Gateway Gardens Assisted Living and Memory care here in Winder is dedicated to providing a memory care assisted living community where residents and their families feel safe. Learn more about our commitment to safety and our advanced memory care services. Contact us today.
30 January 2023

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. We take great reward in the form of personal feedback from our blog readers that we inspire you with our efforts here. But we humbly submit that it is YOU who inspire us! In today’s blog post, together, let’s briefly ponder the benefits of our online relationship with each other.
Today’s senior has evolved away from the one-size-fits-all model. Savvy older adults are wanting more control over their lives and are demanding convenience and choice. That’s why the Gateway Gardens Assisted Living and Memory Care philosophy is to create a lifestyle completely customized to each individual’s needs.
It starts by asking a lot of questions when residents first move to one of our communities. We then aim to suit each individual’s style and needs and encourage aspirations. Resident needs are at the heart of whatever we do.
Once you move into one of our communities, we’ll ask plenty of questions to get to know you so we can make your life right for you in every way.
Think of it as a senior needs assessment – only more personal. It’s customized with details that pertain only to you. This collection of facts, preferences and stories about your life will form both the basis of our friendship with you and your lifestyle plan. This information is then used to create a uniquely relevant experience for you, where your needs are met in a style that suits you.
You want to eat lunch in your room instead of the dining room? Done. Would you like to invite a friend for tea and cookies in the lobby? Will that be hot tea or iced? Do you want your haircut appointment to be every other Wednesday or every single Thursday?
Our staff within both our assisted living community and our memory care community is skilled at learning what you like and then creating a lifestyle customized to your needs.
What are some of the desires we hear from residents? Seniors want to feel connected to others and experience social engagement. A survey from the National Council on Aging supports this need. The survey discovered that seniors have a real need for connectedness. More than half of seniors nationally – 53 % – indicate that being close to friends and family is important. Only 15 % felt occasional feelings of isolation. Relationships with friends and family even outweighed financial concerns for older adults.
Research about happiness and aging may surprise you. According to an AARP survey, although many younger Americans have a negative perception about aging, most older Americans feel good about their lives. The national study surveyed 2,601 American adults. It reported 67% of people age 60-plus are “satisfied” or “very satisfied” with their lives versus 61% of people age 18-39 and 60% of those respondents age 40-59. While about half of the survey respondents age 18-39 believe it’s “normal to be depressed when you are old,” just 10% of those over age 60 feel old age is a depressing life stage.
What can you look forward to every day with the lifestyles we’ve meticulously designed? You can look forward to something uniquely different – something inspired by you. For certain there will be the same smiles and friendly conversations that everyone in our communities shares. But there will also be the opportunities for you to take off for your morning walk while your neighbor settles in to put together a puzzle. You can come back for coffee (with cream, please) and your book club while the choir strikes up in an adjoining room. You get the picture. Your lifestyle will be anything but cookie cutter.
So very simply stated, thank you for your feedback and to our cherished residents and resident family, thank you for enriching our professional lives with the privilege of both caring and growing with you!
25 January 2023

Heart disease is a significant threat to our cherished seniors, and we need you to understand that we take senior heart health seriously. The following items are primary goals of our assisted living community and our memory care community in an effort to reduce the risk of our senior residents developing heart illnesses.
Keeping seniors active and relaxed improves heart health. Workout programs that range from low to moderate impact exercises are managed based on fitness levels and health status. Regular exercise helps lower stress levels and improve quality of sleep. When these two vital factors are achieved and stabilized, a healthier heart is guaranteed.
Assisted living communities pay close attention to the nutrition and diet of their senior residents. They make sure that the food served to senior residents are both appetizing and healthy to improve food intake and facilitates consumption of important nutrients that can strengthen the heart. Also, taking note of food that must be taken moderately. Low-salt, low-fat, low-sugar diet are usually the dietary recommendation for these people.
We know for a fact that a smoker has a higher risk of developing chronic heart disorders including atherosclerosis and coronary heart disease. Gateway Gardens Assisted Living & Memory Care offers a designated outdoor area for smokers separated from non-smokers so that non-smokers will not be exposed to smoke-filled air. This is also a way to encourage current smokers to break the habit. Medical advises are also given to those smokers to support them to give up smoking.
For more information about assisted living and memory care services in and around Winder, contact Gateway Gardens today!
18 January 2023

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community.
In our previous blog post, we presented some facts about Alzheimer’s disease that hopefully helped you feel a bit better about your ongoing journey as a home care provider. Today, we offer some tips on transitioning your Alzheimer’s loved one to professional memory care like ours here at Winder’s Gateway Gardens Assisted Living and Memory Care.
The transition period can be difficult for everyone, especially an Alzheimer’s patient. Even though every situation is unique, these tips can provide some guidance on how to transition an Alzheimer’s patient to memory care:
A loved one with Alzheimer’s may feel confused, sad, or apprehensive. Address their fears, questions, or concerns with understanding and be sensitive to their emotions.
If they are still able to communicate, involve them in the conversation. Assure your loved one that the memory care community is a safe place where they will be cared for while doing the things they love.
Take a tour of our memory care community and see for yourself the loving professionalism and care being provided here. Feel free to visit as many times as you like before moving so your loved one can get familiar with the new environment, staff, and amenities.
To avoid stressing and overwhelming your loved one, pack their belongings. Take care of donating or selling unwanted items and arrange to have their belongings in their new place of residence.
Having their most valued possessions, such as photos or a favorite piece of furniture, will create familiarity and feelings of home, comfort, and safety.
Take the day off on moving day and have someone with you for support. Schedule the move at a time that your loved one is most comfortable.
Speak to staff in advance to share information about your loved one’s needs and preferences and maybe even coping strategies. Avoid rushing the process. Allow your loved one time to settle.
Despite all your efforts to make the transition easy, there can still be challenges. Speak to the memory support staff about your loved one’s progress and what you can do to help.
Your loved one may complain and ask to go home. It’s natural to feel anger, frustration, or sadness in the first few weeks when adjusting. Reassure them how much you care.
Visit often and try to understand some of their concerns. When they become agitated, redirect them to something positive and partake in activities with them.
Sometimes visits can trigger negative emotions. In this case, you can ask the staff for advice on how often to visit. Visits and calls from other family members or friends can help in these instances, keep them connected, and not feel forgotten.
We hope you benefit, are encouraged, educated, and enjoy our blogging efforts. When the time comes for you to seek a consult regarding caring for your loved one’s professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care in Winder stands ready to improve the quality of both you and your loved one’s lives. Call us!
16 January 2023

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community.
Alzheimer’s is a progressive disease that can seriously affect a person’s ability to carry out daily activities. And at the later stages of the disease, an Alzheimer’s patient will require more care than what is available at home.
Mild memory loss is typically the first sign of this disease. As a caregiver, deciding whether a loved one with Alzheimer’s should go to a memory care facility can be difficult. While there are some benefits to keeping them at home, professional memory care support providers are highly trained and highly effective in delivering quality of life support to people living with dementia.
Consider the following that represents just a sub-set of the amenities that we offer:
In our next blog post, we’ll discuss exactly why transitioning to professionally managed Alzheimer’s care need not be a daunting task. Until then, know that if caring for your senior loved one at home feels overwhelming, whether you are an at-home senior assisted living support provider or an at-home memory care support provider, we can help. Our mutual love and admiration for our seniors binds you and us as a team.
11 January 2023

Welcome back to our Winder-area assisted living and memory care blog where we strive to pass along our love and professional knowledge to all of you caring for special needs loved ones at home. In last week’s blog post we covered “Ways to Make Your Assisted Living or Dementia Loved One Smile”. To our great reward, a reader reached out and shared her story about how she employs the magic of music in the daily care of her Alzheimer’s mom. She suggested we follow last week’s post with one focused on how music can be a tremendous therapy for our assisted living and memory care loved ones. We will do just that.
The following are the scientifically-proven ways that music can improve the quality of life for those dealing with Alzheimer’s.
People of all ages and stages of life can relate to hearing a song from a different time in life and being taken right back in time. Songs can ignite a sense of nostalgia unlike any other mechanism.
Additionally, music (whether new or familiar) evokes emotion. Listening to a particular song can bring up memories of a spouse, children, grandchildren, or even a well-loved hobby or career.
When coupled with activities of daily living (ADLs), music can help to trigger memories associated with each activity. After some time, listening to the same song during the same activity can help bolster your loved one’s cognitive abilities throughout each activity.
Agitation, anger, and delusions can become a daily occurrence for those dealing with Alzheimer’s. Listening to music or playing a musical instrument has been shown to increase levels of endorphins that help elevate overall mood and even improve sleep. Music can become a powerful tool for calming your loved one and turning around a foul mood quickly.
Seniors diagnosed with Alzheimer’s disease can experience ever-increasing stress levels, which can cause isolation, boredom, and depression. Stress is also a strong contributor to agitation and anger. Turning on your loved one’s favorite tunes has been proven to lower stress levels and brighten moods while helping them feel more relaxed and at ease.
One of the common side effects of Alzheimer’s is the inability to sleep for longer periods of time, leading to interrupted sleep patterns and a disrupted circadian rhythm. Due to music’s calming effect, it has been proven to improve sleep for seniors living with Alzheimer’s. Thanks to the release of endorphins that are released when your loved one listens to their favorite songs, their body will produce more melatonin and help them get a better night’s rest.
It’s important to note that many other complications can arise for seniors that aren’t getting enough sleep, so prioritizing rest is very important.
Seniors with Alzheimer’s should be engaging their brain in stimulating activity on a daily basis. Studies show that listening to music activates a large portion of the brain, surprisingly, not just the area responsible for music and singing. In fact, listening to music seems to activate the right side of the brain and even spark activity in the left side of the brain, as well.
With this added stimulation, many seniors with Alzheimer’s find that they can think more clearly than usual while listening to music.
We said it last week and we’ll say it again. All of us at Winder’s assisted living community and our Winder Memory Care community are your biggest fans and wish you nothing but happiness and true reward for your selfless support of others.
9 January 2023

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. Last week’s assisted living and memory care blog post focused upon ideas how you can engage your support group for strength, insight, and reward for your journey as a assisted living or memory caregiver. Today’s focus returns to the loved ones you care for. We offer simple ways to make your assisted living or memory loved one smile. When you do that, of course, you smile along with them.
OK, here’s the big secret: Engage in activities they enjoy! Everyone has different hobbies and interests. If you know what the individual with dementia enjoys, try doing that activity with them. For example, if they enjoy music, try singing or listening to music together.
Share old memories: Reminiscing about past experiences and memories can be a great way to bring joy and connection to individuals with dementia.
Play with pets: Many people find interacting with animals to be calming and uplifting. Consider bringing in a therapy animal or showing the individual pictures of pets.
Use humor: Humor can be a powerful way to bring joy and connection to any situation. Try telling jokes, sharing funny stories, or playing word games.
Offer physical touch: Sometimes, a simple hug or holding hands can bring comfort and joy.
It's important to remember that each assisted living or person with dementia is unique and may respond differently to different activities. It may be helpful to try a variety of approaches and see what brings the most joy and connection.
As always, all of us at Winder’s assisted living community and our Winder Memory Care community are your biggest fans and wish you nothing but happiness and true reward for your selfless support of others.
4 January 2023

Happy New Year and welcome back to our Winder-area assisted living and our Winder memory care community blog. Today’s message is very simple and something we hope each of your will act upon.
There is no doubt that all you special caregivers out there, selflessly tending to your assisted living and memory care loved ones, compiled an inventory of special warm moments over the Holidays with those you lovingly labor for. Our advice and hope are that you share the stories with your support group(s). When the labors of your love seemingly become daunting, purposeful reflection and sharing stories of those special moments is therapeutic. Therapeutic for not just you, but for all those on the receiving end of your message.
From all of us at Winder’s assisted living community and our Winder Memory Care community, we wish you renewed strength, patience, perseverance, and reward for all that you do for your loved ones in need.
12 December 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. A common discussion during the Holiday season is: “During the happiest time of the year, why do I sometimes feel down”? Well, sometimes it’s explainable because a particular Holiday, month, or day of the year triggers meaningful and reflective memories. But maybe it has nothing to do with the Holiday.
Today, we want to share with you the “Four Worst Habits for Good Cognitive Health”. These conclusions emerged out of the Mayo clinic, one of the most highly respective research institutes in America. Here are the main controllable threats to good cognitive health:
Sedentary Lifestyle. Having a sedentary lifestyle has been linked to mental health concerns like depression, anxiety, and chronic stress. So, sitting for more than eight hours a day can lead to decrease in motivation, contribute to fatigue and make it difficult to manage stress and anxiety. For those of us who move via wheelchair, then Mayo advises us to simply roll more.
Poor Sleep. Insufficient sleep can slow down your thinking, impairs your memory, concentration, judgement and decrease in your decision-making skills. This can also impede learning as well. Studies show that between 7-8 hours a day can be essential for stimulating brain growth.
Time in the Dark. Don’t spend too much time in the dark. A decrease in sunlight exposure can lead to problems like seasonal affective disorder, and even depression, so make sure you're opening those blinds, getting some sunlight every day and go outside from time to time.
Thinking Negatively. Don’t think negatively. When you're constantly stressed and anxious, it takes a toll on your mental health. This can lead to problems like depression, anxiety, and even dementia. Keep your brain healthy, make sure you're thinking positive thoughts.
From all of us at Winder’s assisted living community and our Winder Memory Care community, we wish you peace, happiness, and the blessing of the best cognitive health possible.
5 December 2022

Hello dear residents, resident’s family, and the entire local community who are soldiering through the dedicated and blessed love in providing in-home assisted living services or memory care services. Today we share a story from one of your fellow Winder-area Gateway Gardens Assisted Living and Memory Care blog readers about an interaction at church on Sunday with a memory-challenged person she’d never met before.
I sat next to this nice man who introduced me to his wife and aged mother. I am relatively new to the church and shortly after our introduction, service started. I made it a point after service to communicate how nice it was to meet them. I made a special effort to grab that senior’s hand, (shame on me for forgetting their names), bending down, looking into her eyes, and saying, “It was very nice to meet you”. Her response caught me off guard.
She responded, “It was very nice meeting you too, but I am sorry that I likely won’t remember you come next Sunday”. Momentarily at a loss for words, I simply offered this: “Well, I look forward to meeting you again next Sunday, for the first time”. She smiled an honest smile and offered: “Yes, I look forward to that”.
What a special moment and a special life-lesson from such a beautiful soul who knows exactly where she is….and where she isn’t. We remind you all that the blessings of your care to others is neither buried nor hard to find. There right there on the surface and we simply need to acknowledge them and celebrate them.
30 November 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. This blog is adapted from Martin J. Schreiber’s "My Two Elaines: Learning, Coping, and Surviving as an Alzheimer’s Caregiver". Full credit is offered here to Mr. Schreiber as the author and owner of the content that you are about to read.
If you are a caregiver, here are five things that I learned the hard way and share in my book My Two Elaines: Learning, Coping and Surviving as an Alzheimer’s Caregiver" to help other caregivers know they are not alone.
As a caregiver, you will do heroic work. You may be thinking, Me? A hero? I say, "Yes! A hero!" Even though your efforts won’t be enough to stop the disease from stealing your loved one, the deeds you will perform as you continue to care for and love your partner are heroic.
You can’t expect yourself to be perfect. Looking back at the past 18 years, I should have forgiven myself for not being perfect. I was doing the best I could in a difficult situation and so are you.
No matter how much you love your partner, you can’t take good care of him or her if you don’t first take good care of yourself. I didn’t realize how important that was until it was almost too late. I don’t want that to happen to you.
I should have started earlier to find an adult day care so that I could reclaim part of the day for myself, including time for exercise.
When your partner has Alzheimer’s, you can feel like that lone wolf, isolated from anyone who cares about your well-being. People don’t usually think of offering rides or meals or help with the yard work to an Alzheimer’s caregiver. They still love you, but they simply don’t know how to respond.
Feeling so lonesome was something I didn’t anticipate. Like other negative aspects of caregiving, it silently creeps in on you. Caregivers, here is your warning: loneliness is coming your way. You can’t just put on a brave face day after day. You need to reach out to others and teach them about Alzheimer’s. To survive, you can’t worry that you’re being a burden.
The toughest question a caregiver faces is moving their loved-one to a facility. Moving to a facility was never going to cure Elaine. I knew that. But I also recognized that Marty’s One-Man Nursing Home was no longer good enough either. That realization made it somewhat easier for me to accept the inevitable: Elaine should move.
You can’t expect yourself to be perfect. Looking back at the past 18 years, I should have forgiven myself for not being perfect. I was doing the best I could in a difficult situation and so are you.
Home, I’ve learned, isn’t a building. It’s a place inside you where you feel secure.
Even as I adjusted to the emptiness in my home and in my heart, there were two emotions dominating my thinking: relief that Elaine would be safe and hope that now I could focus on being a better father and grandfather.
Even though it broke my heart, I should have let go of my First Elaine sooner so I could love my Second Elaine where she is now.
I had lived such an active life with my First Elaine. With my Second Elaine, that was no more. Unfortunately, it took me too long a time to realize that I must choose to let go, to accept that hard truth.
I needed to meet my Elaine where she was and enter her world, something I call therapeutic fibbing. One time she asked about her parents, and I told her they were dead. After seeing the look of pain on her face, I vowed never to cause that pain again. Whenever she would ask about her parents, I would say they were great, and they loved her.
That’s my way of slaying the dragon of Alzheimer’s: choosing to see my wife as the person she was then. Helping her enjoy the person she was at that moment. Helping her sense that I was happy to be with her. You can slay the dragon as well, but you can’t do it alone.
Adapted from "My Two Elaines: Learning, Coping, and Surviving as an Alzheimer’s Caregiver," by Martin J. Schreiber and Cathy Breitenbucher. Copyright © 2022 by Martin J Schreiber.
28 November 2022

With Thanksgiving in the rear-view, early Merry Christmas, Happy Hanukkah, and other warm greetings assigned by your faith this Holiday season. Just so you know, we unapologetically say, “Merry Christmas” and “Happy Hanukkah” here at Winder's Gateway Gardens Assisted Living & Memory Care. We’ll offer “season’s greetings” as well, but just so you know, we unapologetically offer faith-based greetings. Allow us to tell you why.
Our dear assisted living residents and memory care residents here at Gateway Gardens span the gamut of religious faiths. We’ve queried our non-Christian residents about how some people today consider the term “Merry Christmas” as exclusive, and therefore offensive. Without exception, our dear residents, and staff (again, some of which are not Christian) are warmed (NOT offended) by people exchanging “Merry Christmas” in the heartfelt nature being offered.
We learn from you, our dear residents, every day. Maturity comes with age. So Merry Christmas, everyone, from all of us here at Manor Lake!
16 November 2022

Most of you are aware that our team of professional memory care and assisted living care providers here at Winder's Gateway Gardens Assisted Living & Memory Care are there for all of you, young and seasoned alike. Allow us to deviate here to pay tribute to all of you who help us deliver a celebrated standard of care excellence, something our dear residents so rightfully deserve.
Our path to personal and professional success is paved by (and with) the quality souls that we surround ourselves with. Since you’re reading this, consider yourself a member of our extremely valued fraternity of customers, venders, service providers, mentors, and other vital relationships. We know many of you feel the same toward us and we are humbled by it.
Today, we send this Thanksgiving note to communicate our heartfelt appreciation for all the things that you do to inspire continual process improvement, service quality, and passion for our business. We endeavor to only strengthening our bond throughout the rest of 2022 and well beyond.
With our blog team taking next week off for a well-earned Thanksgiving holiday, we extend our warmest Thanksgiving wishes to all of you, from all of us here at Gateway Gardens!
14 November 2022

Thanksgiving, 2022 is just a little more than a week away. We thought it would be appreciated to craft a Thanksgiving-focused blog reasonably in advance of the holiday to give all our readers time to reflect and hopefully act upon some of our notions.
The Thanksgiving holiday conjures an assortment of emotions within all of us. For some, this is a time to reflect on loved ones, living and passed. And, yet, regardless of where Thanksgiving finds each of us this year, it brings an opportunity to pause and give thanks for the simple things we often take for granted. Things like the love of family, food on the table, and even for life itself.
At both our assisted living community and within our memory care community here at Gateway Gardens, throughout the month of November we have been celebrating Thanksgiving with delicious dinners and special activities and events. We understand that it has been challenging for family members and for residents who, for whatever reasons, may not have been able to get together as often as they would like. Be warmed by the fact that, inside our doors, there is no shortage of celebration, laughter, and love. Our residents and staff members have been sharing special personal feelings of gratitude all month.
So, what are you thankful for this year? Have you shared your thankful thoughts with your loved ones? This is a wonderful time of year to express gratitude to those people in your life who make it so special.
Here at Winder's Gateway Gardens Assisted Living & Memory Care, we are thankful for the wonderful individuals who walk through the halls of our communities every day. Our residents and their families are a blessing as well as our dedicated, caring staff.
From all of us at Gateway Gardens, we offer you and your families a very special Thanksgiving. We hope to see you soon. If life prevents you from being here in person, know that we stand ready to assist you in any way possible to communicate your love and appreciation to your beloved family member, and our beloved resident.
9 November 2022

Very warm Veteran’s Day greetings from all of us at Gateway Gardens Assisted Living & Memory Care here in Winder. To all of our dear Veteran residents within both our senior assisted living community and our memory care community, we trust you’re feeling our love, admiration, and respect. For those non-resident veterans reading this today, we offer you the same notion of love admiration and respect.
Today we offer a brief Veteran’s Day history lesson as well as a couple of simple ways you can take proactive measure to honor veterans during this very special holiday.
A Bit About Veteran’s Day History and the Holiday
On November 11th 1918, the armistice was signed signally an end to the Great War or what would later become known as World War I. This was a monumental day in history and one that has been recognized every year since. The day was originally referred to by President Wilson as Armistice Day, and was created as a way to recognize and remember both those that survived the war and those that perished. In 1971, the day was officially renamed to Veterans Day.
While Veterans Day is celebrated every year, many people often mistake it’s meaning for Memorial Day. Memorial Day is dedicated to remembering those that have died in battle or as a result of their wounds. Veterans Day is a day to think about all veterans, both those living and those that have passed. It is a time to thank them for their service and the sacrifices they have made for our nation. If it were not for the bravery and dedication displayed by the members of our military, we would not be able to enjoy the freedoms that we do. And for that, we say thank you.
Simple Ways to Honor Our Vets
This year, we want to help give back by providing you with different ways you can say thanks to the veterans in your life. Whether it is directly or indirectly, everyone is connected in some way or another to a member of the military. By taking part in one of the activities listed below, you are not only recognizing military personnel for the sacrifices they make, but also saying thanks for everything that they do.
Wear a Poppy and Attend an Event
On November 11th communities across the country hold events to recognize and celebrate Veterans Day. By showing up and participating in these events, you are not only showing your support and saying thanks, you’re celebrating military personnel for the heroes that they are.
Sit Down and Talk with a Veteran
In order to truly appreciate the sacrifices a veteran makes, take some time to sit down and talk with one. Doing so will help you get a better understanding of what life in the military is like and it will allow you to better understand why we celebrate Veterans Day. Try to stay clear of questions about combat as this might be uncomfortable for them to talk about. Instead ask things like what motivated them to join the military. What is their proudest moment? What were some of their duties?
Visit The Grave of a Veteran You Have Lost
If there is a veteran in your life that has passed away, make sure to visit their grave and pay your respects. Lay some flowers, say a prayer, and pay your respects by visiting them and spending some time at their resting place.
Sharing laughter, joy, and praise of our veterans during this holiday is what it’s all about. Here at Winder's Gateway Gardens Assisted Living & Memory Care we celebrate every veteran’s unique sacrifice and contribution to our country and wish all of you a warm and blessed Veteran’s Day holiday!
7 November 2022

The holiday season is here, and we all look forward to spending quality time with our loved ones. While we will enjoy special meals and special events here at Winder's Gateway Gardens Assisted Living & Memory Care, for at-home caregivers the holidays can be stressful. For you loved ones, the holidays can heighten the feeling of isolation and sadness. Let’s address all this head-on.
Below are a few tips that should be on your holiday to-do list to check on the loved ones under your care and ensure they are all set for the holiday season:
Keep a Check on Their Well-Being
One of the most essential things is assessing your seniors’ health. Ensure they are taking their pills or medications regularly and on-time. Check if there is a need to refill their medicines. It will also be a good opportunity to talk to their doctors in person or over the phone.
Ask them how well they are doing and if there is anything that needs to be done soon. If you are going out for a while, leaving your old ones at home, you must obtain a full list of every prescription they take.
The list should also include their doctors' names and numbers, addresses, and email addresses. You must also have a plan in mind for any untoward event that may occur, and you must rush back to them.
Make a Pre-Vacation Checklist
If your elderly relatives are accompanying you on a trip, make sure you get their doctors' approval before leaving. Since it is mandatory to get country-specific vaccines if you are traveling abroad, check the country’s travel guidelines well in advance so you have enough time to get timely appointments for the inoculations.
Over and above that, carry their medication along with you in case of an emergency. Ensure that all their prescribed medicines and first-aid drugs, recommended for health conditions such as diarrhea, malaria, altitude sickness, etc., are part of your travel kit. It is also recommended to carry slightly more than the required dose to avoid running out if your trip gets extended for unforeseen reasons.
In addition to this, it is advisable to book assistance at the airport. Contact the airline and airport authorities to get assistant-manned wheelchairs and ride-on carts for your parents. Always remember to avail of these services wherever and whenever necessary to avoid over-exhaustion while traveling.
Look Closely
As your parents will always want you to believe that all is well, you do not always realize whether they need any extra care or not. Therefore, it is important to look deeper to truly see how well they are living and if something is missing, that needs to be done. For instance, it is recommended to inspect their bathrooms.
Are they clean? Do they have soap, shampoo, disinfectant, and clean towels? Check the refrigerator. Do they have a variety of foods and vegetables to provide them with enough nutrients? Is there any outdated food? See if they are taking out the garbage regularly or not.
Prepare the House for Eventful Days
As there are many festivals lined up back-to-back this holiday season, if your parents are planning to host a gathering or out-of-town guests, it will be very helpful if you take the initiative to clean and decorate the house and do everything that comes with preparing a house for hosting guests. Ensure they have everything they need to make these events joyful and stress-free.
Grocery Shopping and Meal Preparation
Grocery shopping and meal preparation during the holidays can be challenging for your loved ones, especially without any transport facility or if they have trouble lifting heavy items. Depending on mobility and agility, your parents may struggle to lift heavy pans in and out of the oven or prepare holiday dishes as quickly as they used to. Therefore, make sure they have everything they need in place.
Also, ensure they have a care provider who can assist your parents with tasks such as chopping vegetables, cleaning kitchen equipment and appliances, etc. so that their special family recipes and holiday meals for guests turn out just the way they want.
Ensure Home Safety
Your parents need to live in a safe home that prevents injuries, reduces fall risks, and ensures independence as they age. Therefore, without further ado, incorporate home safety tips into the house and follow a home safety checklist this holiday season.
Remove trip hazards, install non-slip flooring, cover all cords and wires, and install bathroom grab bars to ensure safety for your parents. Ensure a senior-friendly home by adding accessible seating as well. For instance, install a bench near the house's front door for putting on shoes, and put a stool in the bathroom and kitchen for your parents to perform the activities of daily living with ease.
Encourage Exercise
Physical activity is essential for your aged parents. But as soon as the holiday season kicks in, many of their daily routines go for a toss. With several other things in mind, your parents’ daily exercise routine may also take a back seat. Therefore, they should ensure they are keeping themselves physically active.
It will keep them fit, reduce their stress and tension, and help them burn off the extra calories they consume during the holidays. In addition, advise them to stay hydrated for their bodies to function at their best throughout the winter. Staying hydrated will help them feel more energized, boost their immune system, and increase their ability to deal with fatigue. It will also help them stay healthier and more active in all the planned holiday festivities.
Prevent Infections
Because the holiday season coincides with the arrival of winter, your parents are more susceptible to colds, flu, and other illnesses. Therefore, opting for influenza and pneumonia vaccinations is recommended to keep them safe. Also, as we have just come out of a deadly COVID-19 pandemic, ensure your aging parents are fully vaccinated, along with the booster shot.
In addition, you must help them follow healthy hygiene habits such as washing their hands, sanitizing surfaces, etc., to keep them from contracting infections. While getting immersed in the chaos and shuffle of family gatherings is good, make sure your loved ones are staying healthy and enjoying every planned holiday event by following a healthy lifestyle.
Encourage a Sleep Schedule
The holiday season is undoubtedly the time of the year when we all skip some of our essential needs, such as sleep. And your parents are no different. While it is fun to spend time celebrating and catching up with friends and relatives, a lack of sleep can harm your parents’ health. It may also affect their memory, communication ability, and overall health. Therefore, please encourage them to stick to a healthy sleep schedule as much as possible.
Provide Emotional Support & Companionship
You must provide emotional support and companionship for your parents as the holidays approach. It is common for seniors to experience loneliness and isolation. With age, they may not be able to get around on their own anymore, may have also lost their close ones, and therefore, spend a lot of time alone, which is not good. If you stay away from them, plan weekly or bimonthly visits.
Even if you don’t do much and just simply sit and have a cup of tea, it will be something for your aging parents to look forward to and cherish. Once in a while, you can take them to community functions or church services. Feeling like a part of a group positively affects overall mental well-being.
Conclusion
All in all, while you may have been able to gauge your senior loved ones' safety and well-being, it is sometimes necessary to personally look at their conditions. Make sure you engage with them more often. The absence of family or even someone to talk to impacts everyone, regardless of age. Moreover, as your parents’ needs are rapidly changing, it’s essential to talk with them, including other family members and caregivers.
If caring for your senior loved one at home feels overwhelming, whether you are an at-home senior assisted living support provider or an at-home memory care support provider, we can help. Our mutual love and admiration for our seniors binds you and us as a team.
31 October 2022

Greetings once again from your Winder-area assisted living and Winder memory care community here at Manor Lake. With apology in advance for being late serving notice here, but did you know that October is “Pastor Appreciation Month”? Even if you’re reading this blog post early in November, strongly consider reaching out to your pastor (assistant pastors, or whatever title you bestow upon your spiritual leaders) and wishing them a very happy Pastor Appreciation Month. Blame being a day late (or two) on us, but we promise that the communication will be rewarding to you both.
As always, all the best to you and your loved ones from all of us at Winder's Gateway Gardens Assisted Living and Memory Care!
24 October 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. One of the most common frequently asked questions this time of year is “what ideas do you have to make this Halloween holiday special for my memory care loved one”? Well, we thought we’d simply refer you back to the ideas we presented in last year’s blog post, “Halloween Home Care Considerations for Loved Ones with Alzheimer’s”.
We hope you all are enjoying this Fall season and are looking forward to one of the most fun holidays of the year. Of course, you all are invited to come celebrate your loved one’s Halloween celebration here at both our Winder assisted living community and our Winder Memory Care community. If we don’t see you here, have a great time celebrating at home!
19 October 2022

Welcome back to the third (and final) episode of our three-part blog mini-series covering the subject of “Caregiver Stress”. We looked back on the calendar year 2022 to date and discovered that issues related to caregiver stress was a regular and recurring subject that those self-managing assisted living services at home and also memory care services at home.
Below we link to the prior two blog posts on this subject. Here are the three different topics that we are covering:
If you are new here to our Gateway Gardens (Winder) Assisted Living and Memory Care Blog, you’ll soon discover our blog to be a fantastic free resource on ways to learn about assisted living care and memory care and help you both provide your loved one with quality care while helping maximize your quality of life along your loving journey.
So now, onto the ways to manage caregiver stress.
The feelings of tension you may feel as a caregiver can frustrate and exhaust you. Fortunately, there are plenty of helpful techniques you can use to manage your stress. We took to social media and got feedback from real caregivers on how they manage the pressure. Here are our favorite tips from fellow caregivers and thought leaders on how to deal with caregiver stress:
Complete Small Tasks to Regain Control
When dealing with another person’s fluctuating health, it’s totally normal to feel overwhelmed and out of control. If this describes you, try this caregiver’s simple, helpful tip.
1. Eat Right
What we put into our bodies is what we get out of them. Proper nutrition is crucial self-care that can be left to the wayside when under a lot of stress. However, stressful times are when your body needs healthy fuel the most. Avoid skipping meals, snacks or overindulging in alcohol. Instead, set aside regular times each day to enjoy a balanced breakfast, lunch, snack and dinner.
2. Get Enough Sleep
When your mind is racing around a track with a million things to do on it, it’s only natural that your sleep may suffer. But you can’t avoid it: your body and brain unquestionably need time to recharge. Amazing things happen when you sleep, like muscle relaxation, tissue growth and repair and energy restoration. How well you sleep affects nearly every aspect of what happens in your waking hours, so make sure to get those quality ZZZs. Aim for 7-9 hours each night, preferably at consistent times.
3. Exercise
If you are physically capable, getting your body moving and your blood pumping is an almost guaranteed way to relieve tension. Physical activity pumps up your “feel-good” endorphins and refocuses your mind on your body’s movements, releasing stress and improving your mood. Physically, exercise helps maintain a healthy weight and can even regulate your sleep cycle by making it easier to fall (and stay) asleep.
Virtually any physical activity works: walking, jogging, gardening, housecleaning, biking, swimming or anything else that gets you moving. Find time, even if it means asking someone else to provide care while you take a break.
4. Try Meditation
Meditation creates a sense of calm, peace and balance that benefits both mind and body, and it encourages the use of breathing to get through stress. You’ll focus your attention on the sensations you experience, squeezing out anxious thoughts. The best part? You can meditate almost anywhere, from a doctor’s office to a bus ride.
5. Do a Little Coloring (Really!)
Think coloring books are just for kids? Think again. Adult coloring books have become an increasingly popular way to decrease stress through mindfulness, the act of focusing on being in the present moment.
6. Have a Healthy Dose of Laughter
Did you know that laughter lightens your emotional load and actually causes physical changes in your body? Laughter enhances your oxygen intake, relieves mental stress and soothes physical tension. Try switching up the nightly news with a favorite comedian’s stand-up or a classic rom-com or call your funniest friend. And speaking of friends…
7. Get Social
Spending quality time with friends and family has long been a stress relief tactic used across many cultures and time periods. When you spend time with your social circle, you experience better mental health, a stronger immune system and can even lower your risk of dementia!
If you don’t have much time to meet up out of the house, or your friends and family are long-distance, don’t worry: video chatting and phone calls can provide many of the same positive effects as face-to-face socializing.
8. Start Journaling
Putting your thoughts and feelings into written words can be a good release for pent-up emotions. Writing often provides perspective that thinking, or even talking, cannot always give. In addition to venting out your worries, journaling is also a good place to list out all the positives in your life that you’re grateful for.
9. Don’t Go Through Your Health Journey Alone
You can stay connected to friends and family, plan and coordinate meals, and experience love from any distance.
10. Get a Pet
Therapy animals are around for a reason. Our favorite furry friends provide many stress-relieving benefits when they cuddle us, learn a new trick or simply just look adorable. Whether you prefer a dog, cat, parakeet or fish, owning and loving a pet can be enormously beneficial. And if you’re thinking that you can’t take care of yet another thing, not to fear: these low-maintenance pets might change your mind.
11. Just Say ‘No’
Yep, you read that right. You are more than allowed to turn requests down if you feel that you’re getting overwhelmed with responsibilities and places you just have to be. When you say ‘no’ to adding another “to-do” on your list, you’re opening up an opportunity to have very important time for yourself. You are a priority, too!
12. Reclaim Your Identity
Spending time on your passions will help remind you that you are more than a caregiver. Try to take time at least once a day to engage in an activity that makes you feel most like yourself outside of your caregiving role. It can feel like you don’t even have time to wash your face at the end of a long day, much less take 30 minutes to yourself. But there are opportunities to carve out you-time every single day. If you leave for work, use your lunch hour to go outside and read a book or magazine. If you stay home, take time to play your favorite music or make dinnertime exciting by cooking a fun, new recipe. It’s the little things that make us who we are and it’s important not to forget about them.
13. Prioritize Your Own Medical Needs
Caregivers still have regular checkups and dentist appointments, just like anyone else. It can be easy to get so caught up in the medical treatment of your loved one that you forget that you actually share some of the same needs. Take note of any appointments you’ve missed or may need in the next few months, and if necessary, start enlisting help so that you can make your appointments without a hitch.
Also, don’t forget about therapy. It might not be for everyone, but therapy is a tool that’s definitely worth considering. Many therapists specialize in the managing and relieving of stress through means such as Progressive Relaxation Training, mindfulness-based techniques and more. To find out about the different types of therapy and which one might be right for you, talk to your doctor about your symptoms and discuss getting a referral.
14. Ask for (and Accept) Help
It’s ironic that the people who spend so much of their time and energy helping others often find it incredibly difficult to accept help themselves. Here’s what a couple caregivers said helped them with this:
Some other ideas on this: Make a to-do list and recruit others to pitch in to help with meal planning, trips to the pharmacy, walking the dog, watering plants… everything that goes with your caregiver role.
Home care providers, we hope this mini-series proved to be helpful. Until next time, know that we are your biggest fans and stand ready to assist in any way we can. Very warm best wishes from all of us here at Gateway Gardens Assisted Living & Memory Care!
12 October 2022

Welcome back to the second of our three-part blog mini-series covering the subject of “Caregiver Stress”. We looked back on the calendar year 2022 to date and discovered that issues related to caregiver stress was a regular and recurring subject that those self-managing assisted living services at home and also memory care services at home.
Below we link to the first blog post on the subject. Here are the three different topics that we are covering:
If you are new here to our Gateway Gardens (Winder) Assisted Living and Memory Care Blog, you’ll soon discover our blog to be a fantastic free resource on ways to learn about assisted living care and memory care and help you both provide your loved one with quality care while helping maximize your quality of life along your loving journey.
So now, onto the causes of caregiver stress.
Common causes of stress include financial strain, relationship role changes and lack of rest for the caregiver.
The financial aspect of caring for your loved one can be one of the most troubling for caregivers. But we can help you manage that. Caregivers often spend less money on leisure activities as a result with nearly half reporting a decrease in going out to eat or taking vacations due to the costs of caregiving.
Another cause of stress is the emotional impact that comes from a reversal of caregiving roles. If caring for a parent or an older sibling it can be quite disorienting to start taking responsibility for someone who was previously responsible for you.
Finally, many caregivers neglect to give themselves the additional rest necessary for good health, since their primary focus is often on their loved one. Providing frequent support for another human is essentially doubling the work our bodies are designed to do. We all have a finite amount of energy – both mental and physical – and when we refrain from taking regular breaks, we run on fumes and aren’t giving our own bodies what we need.
Remember: giving your own body and mind the care they need is one of the most important components of being a good caregiver.
Next up, we’ll conclude the mini-series with a discussion about managing caregiver stress. Until then, our very warm best wishes from all of us here at Gateway Gardens Assisted Living & Memory Care!
10 October 2022

Welcome to the first edition of a three-part blog mini-series that will cover the subject of “Caregiver Stress”. We looked back on the calendar year 2022 to date and discovered that issues related to caregiver stress was a regular and recurring subject that those self-managing assisted living services at home and also memory care services at home.
Here are the three different topics that we will cover over the next three posts:
If you are new here to our Gateway Gardens (Winder) Assisted Living and Memory Care Blog, you’ll soon discover our blog to be a fantastic free resource on ways to learn about assisted living care and memory care and help you both provide your loved one with quality care while helping maximize your quality of life along your loving journey.
Caregiver stress is the physical and emotional strain that results from providing continuous care for another person. When this stress is prolonged, it can cause serious physical and mental health problems for those providing the care.
Caregiver stress may be the precursor to the more severe caregiver burnout, though many of the symptoms overlap.
As a family caregiver, it’s important to keep an eye out for any negative physical or emotional symptoms you experience, as these can lead to long-term damage. Physical signs that you might be experiencing caregiver stress include:
Emotional signs of caregiver stress include:
It’s known that the long-term effects of stress can be detrimental to health. Long-term symptoms can include:
If you or a loved one are exhibiting signs of caregiver stress, it’s important that you first talk to your doctor about ways to ease your symptoms. There are medications, holistic remedies, therapies and more that are designed to help.
Next up, we’ll discuss the causes of caregiver stress. Until then, our very warm best wishes from all of us here at Gateway Gardens Assisted Living & Memory Care!
3 October 2022

Our team of professional memory care and assisted living care providers here at Gateway Gardens in Winder are there for all of you, young and seasoned alike. Today’s blog offers “food for thought” pertaining to senior knee pain. Knee pain is so very common within the senior community. So, let’s talk about it.
There are a variety of activities that can contribute to knee pain as you get older. A lifetime of sports, injuries, running or arthritis are common culprits. Seniors with knee pain, in particular, know the years of wear and tear can take a toll and make mobility and flexibility more challenging.
Several conditions can also contribute to knee and joint issues for seniors:
While many of these ailments are relatively common, there isn’t always an easy solution. If you’re wondering how to take care of your knees as you age, there are ways to work your leg muscles to minimize knee and joint pain without surgery or medication.
It’s always important to meet with your medical provider before starting a new exercise plan, primarily because, in some cases, surgery is an essential option. If your physician clears you for exercise, you can begin working toward healthier habits by using the following tips for how to take care of your knees:
We pride ourselves for being readily available to all of you and to apply our vast array of skill sets to help in any way we can. If you are considering a senior living community for yourself or a loved here in Winder, we invite you to come visit and see the thriving senior assisted living community here at Gateway Gardens in Winder and/or our loving memory care community here in Winder as well!
28 September 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. We’re all feeling the pinch of rising costs due to inflation, but seniors are even more likely to worry about rising costs. Saving for retirement and closely managing your expenses are wise choices, but how do you ensure your money goes further when costs are at a 40-year high?
Experts recommend adjusting your budget, cutting back on unnecessary spending, and making changes to your investment strategy. Small changes can make a big difference. Consider driving less to save on gas, postponing a vacation, and making lifestyle changes to stretch your retirement dollar.
Does your current home need costly repairs or maintenance? Are food, gas, and health care costs becoming too much to manage?
You may also be thinking about the costs associated with updating your home to make it more accessible. As you age, it may be more challenging to get up and down those flights of stairs or get in and out of your existing tub or shower.
HomeAdvisor reports that you could expect to spend $10,000 – $15,000 on average to update a bathroom and up to $50,000 to update a large master bathroom. Now could be a great time to consider the value that senior living offers.
Forget about the costs of maintaining a home, updating it to fit your lifestyle, or making costly repairs. With stylish assisted living and memory care apartments, you pay one monthly rate—and your living expenses are included. From meals to housekeeping, activities, and even scheduled transportation, it’s all taken care of. Your senior living and memory care community comes complete with:
Fighting rising costs doesn’t have to be daunting for seniors. Making wise investments in your care and lifestyle can have huge benefits now and in the future. Choosing assisted living at Gateway Gardens or Memory Care living here at Gateway Gardens means putting your health, wellness, and lifestyle preferences first. It’s also a great way to save on home costs with one affordable monthly rate.
26 September 2022

Retirement can be a difficult time in life. You may find that you’re not as active or have health concerns, which means living on your own becomes harder. Daily tasks like cooking meals and doing laundry can become unwelcomed. Gateway Gardens Assisted Living and Memory Care (Winder) offers senior care and helps make the transition into older age less daunting.
As we age, it’s increasingly important to stay social and active. Unfortunately, nearly 25 percent of people over 65 experience loneliness and social isolation. This problem can lead to physical and mental issues like:
Even seniors receiving home care services or companion care may not receive as much socialization as they need. Twenty-four percent of seniors said they would have liked to participate in more social, recreational, or group activities. These findings emphasize the importance of frequent social participation in maintaining the quality of life.
We understand that staying active in retirement isn’t always easy.
Older adults can enjoy their golden years to the fullest by staying connected.
We manage accessible living spaces and amenities that reduce the risk of falls and accidents. Comforting features such as walk-in showers, grab bars, and maintenance service aid this benefit.
Assisted living apartments are perfect if you want the feel of community with the benefit of privacy and independence. Our assisted living community features beautiful outdoor spaces where our residents can enjoy time outside. Our memory care community is celebrated with our staff well trained in caring for Alzheimer’s and other memory impairment disorders. Our staff understand that the needs of each resident are as unique as the individual themselves.
The teams at our Winder Assisted Living Community and our Winder Memory Care community work with passion. We view our residents more as family than anything else. Come see for yourself what true senior and memory care compassion is about.
21 September 2022

We’d like to share some keen insight regarding the subject of napping and how some scientists conclude that napping can help boost cognition. It is a professional obligation for the staff here at Gateway Gardens Assisted Living & Memory Care (Winder) to exercise continuing education on the subjects of professional assisted living care services and professional memory care services, and continuing education for you at-home caregivers as well!
If you think naptime is for toddlers, think again. One study performed on a group of approximately 3,000 people ages 65 and older indicated that 60% of participants take a midday nap after lunch time. While in the past some scientists have advised against sleeping during the day, new research suggests napping can help boost our cognition. It turns out that a quick cat nap can benefit the brain, helping to improve learning and memory formation, regulate emotions and, finally, reduce grogginess.
But before you hit the hay during the day, there are a few things to consider. Not all naps are created equal, but there are ways you can help optimize your naptime.
A typical circadian rhythm is programmed to help us stay wakeful during the daylight hours and gradually become sleepy at night. But feeling tired during the day doesn’t necessarily mean that your circadian rhythm is off. In fact, it’s common to have a bout of sleepiness in the mid-afternoon.
How to conquer that midday hump? One study gave participants three options for soothing their daytime sleepiness: getting more sleep at night, using caffeine or taking a nap. The most effective solution was the nap.
A nap may help to reduce sleepiness and increase your brain function, but only if you do it right. You can help maximize your naptime by following these tips:
Keep Naps Brief
In one study, researchers found that older adults who napped for 30 to 90 minutes demonstrated more signs of good cognition, from better word recall to improved figure drawing. However, those who napped for longer than 90 minutes didn’t show the same benefits.
Sleeping for too long during the day can backfire, increasing grogginess rather than making you feel more rested. According to the Sleep Foundation, the optimum nap time is 10 to 20 minutes, although some scientists suggest that naps up to 40 minutes can be restorative. While everybody’s sleep needs are different, the principle remains the same: the ideal nap lasts just long enough for your brain to get quality rest, but is short enough to avoid deep sleep cycles that can make you feel more tired.
Nap Early
While a nap can be refreshing, it can also make it harder to fall asleep at night if taken too late in the day. According to the Mayo Clinic, napping before 3 p.m. may help prevent interference with your nighttime snooze.
Of course, everyone’s sleep schedules are different, and older adults in particular may go to bed earlier in the evening (that’s because our circadian rhythms change as we age). With that in mind, 3 p.m. may not be the ideal time for you. The Sleep Foundation recommends timing your nap around the halfway point between the time you wake up and the time you go to sleep.
Keep Your Nighttime Sleep Regular
Your nighttime sleep quality is an important factor in daytime naps. A regular sleep schedule at night can be balanced with short, refreshing naps during the day. But if you’re struggling with lengthy bouts of sleep during waking hours, naps may not be the best solution.
Consider why you’re napping. Is it because you’re not getting enough rest at night? Lengthy daytime naps may be an indicator of poor nighttime sleep, and in older adults, long naps have been linked with an increased risk for diabetes, heart disease and depression.
If difficulty sleeping through the night is the cause of your midday snooze, it may help to follow tips to get better nighttime sleep. And if you’re like many older adults who struggle with insomnia, you may want to avoid naps altogether, as they can interfere with nighttime sleep.
All of us share common goals here at Gateway Gardens Assisted Living and Memory Care. One of those goals is to continually educate the general public about a wide range of topics designed to enhance the quality of care provided to our local seniors. We hope today’s blog post on napping contributed to that.
19 September 2022

Today’s blog post is targeted for our entire assisted living and memory care blog-reading community. Whether you are a beloved senior assisted living resident here at Gateway Gardens, a loving family member of a memory care service resident, or one of the many providing loving care of a senior loved one within your own home, continuing public education on senior health care issues is a passion. Our love for our seniors is why we get out of bed every morning. We hope today’s topic regarding Osteoporosis resonates to the benefit of your senior loved ones!
There's more hope on the horizon for managing osteoporosis, a disease that can stop seniors in their tracks if they fracture a bone after falling. We’ve even heard of some extreme cases where seniors have broken their bones by sneezing or bumping into furniture!
Until recently, osteoporosis, a condition in which the bones become brittle and fragile from loss of tissue, was considered an inevitable part of the aging process. Thankfully, there are now some innovative therapies, some of which may further increase bone mass, thereby cutting down the fracture risk in older adults.
Current medications for osteoporosis either slow the loss of bone breakdown or increase the rate of new bone formation. But these treatments can have serious side effects, so it's worth putting effort into prevention of the disease.
More than 53 million Americans over age 50 in the United States have been diagnosed with osteoporosis or have low bone mass. It’s often called the “silent disease” because some people don’t know they have it until they break a bone. Even those who haven’t suffered a fracture may live in constant fear of breaking a bone because the consequences can be life altering—typically, half the patients who fracture their hip do not fully recover their independence.
Osteoporosis hits women harder than men. For women, the risk of breaking a hip due to osteoporosis is equal to their risk of breast cancer, uterine cancer and ovarian cancer combined. Women are in greater danger because they generally have a smaller bone mass than men—women with small frames are particularly at risk, as are older women given that bone loss occurs rapidly during menopause.
Older men too have a greater chance of developing osteoporosis than younger ones. In addition to age and sex, race plays a role, with Caucasians, Asians, and Latinos more at risk than other racial groups. As well, those with a family history of osteoporosis stand a greater likelihood of developing this disease, and those who have been taking steroid medication for a long time are at risk of developing rapid and severe bone loss.
Lifestyle can also make a difference. For instance, those who do not consume enough calcium through food or supplements increase their chance of developing osteoporosis. Inactivity can also increase the likelihood of developing this condition, as bones build up in response to weight bearing and strength training exercises.
Other lifestyle factors that put people at risk include smoking and drinking more than one alcoholic drink per day for women or two for men.
Although this may seem to paint a grim picture, please don’t waste time worrying about this disease—act instead. For starters, learn how you can prevent falls. If you're a woman over 65 or a man over 70, ask your doctor for a bone density test.
We also suggest that you look at improving your diet and upping your physical activity. Some factors, like your sex, age, or race—are not within your control. But your lifestyle choices certainly are.
As always, if you have any questions regarding professional senior assisted living or memory care services, contact us anytime.
12 September 2022

By now, most of you know that we manage our Gateway Gardens Assisted Living & Memory Care blog for the benefit of all of you at home in the Winder area caring for your loved one with senior assisted living needs and/or memory care challenges. We do this because you are neighbors and friends, but most importantly, because we view you as heroes. As professional care givers, we know the challenges that you face. And we want to do our part to help. Today we’re going to discuss how to welcome the changing of the season from Summer to Fall. We’ll give you all some Fall-season themed ideas to engage upon with your loved ones. We offer this while crediting dailycaring.com as the source for these ideas.
Coloring is an activity that everyone can enjoy, from the very young to the very old, as a solo activity or with others.
As an added bonus, psychologists say that coloring has stress-busting abilities similar to meditating.
There are hundreds of free, fall-themed coloring pages available online, here are some of our favorites:
Sitting at the table with a warm beverage and a festive puzzle is a great way to celebrate the season.
Here are some of our favorites:
Baking, mixing, and assembly are fun activities that many older adults will enjoy.
Mmmm! Try these delicious and easy-to-make treats:
Fall is a wonderful time to enjoy nature with your older adult.
Bundle up and breathe the fresh air, admire the beautiful colors on display, and hear the crunch of fallen leaves as you walk.
Be sure to wear face masks (unless it’s not safe for your older adult’s health conditions) and keep a safe distance from other people.
Adapt activities to suit different mobility levels:
Gateway Gardens Assisted Living & Memory Care here in Winder offers a wide range of care options that can help alleviate some of the stress, anxiety, and fatigue that come with caregiving on one’s own. We understand that taking care of aging loved ones can progress from slightly challenging to completely overwhelming in a matter of days, but we are here to support your family every step of the way. We offer senior assisted living and professional memory care services here in Winder and we will work with you to determine what is right for you and your loved ones. Now may be the time to have that discussion. Contact us today.
7 September 2022
Hello everyone from your friends and neighbors here at Winder's Gateway Gardens Assisted Living and Memory Care. Some of you might recall that in early August we produced an assisted living and memory care blog post focused on identifying the “national days” of August. We discussed the fact that many of you struggle to come up with new ideas on what to discuss and do with your assisted living loved ones or your memory care loved ones. We offered you a path to August’s “national days” for inspiration regarding how to plan quality time with your loved ones. We encourage you to revisit that post for new ideas this month.
Today we simply wish to refer you to “eventguide.com” where you can review the list of monthlong September observances. Take note that September 21 is “World Alzheimer’s Day” for those of you dealing with a loved one’s memory care struggles. Just so you know, our entire staff is fired up to learn that September is “National Shake Month”. Time to spend some precious moments with your loved ones at the local ice cream shop!
As always, if you ever have questions regarding professional assisted living services or professional memory care services, contact us anytime!
6 September 2022

Labor Day is behind us. That means that the “fall season” is in full swing. We’re not referring to one of the four calendar seasons of the year (the Fall season officially starts on Sept 22), we’re talking about senior fall risk. We’re talking today about the risk of falls to your senior loved one under your care at home. Before we go on, realize that for any senior care question that you might have, we offer senior assisted living services and memory care support services and are ready to take your call anytime. OK, now on to senior fall risks and how to prevent them.
A fall can be life-changing, especially for seniors. We think it won’t happen, but falls remain the leading cause of injury and death among adults over 65. Whether it’s broken bones or a fractured skull, seniors are at high risk for orthopedic injury.
For the elderly, a fall can be much more serious than when it happens to a younger person. A senior can break a hip or develop a brain bleed with one fall. In fact, falls are the most common cause of traumatic brain injury. Older adults are five times more likely to be hospitalized with a fall.
As we age, our skeletons change. Our bone quality and density begin to decrease. Starting as early as 24 years old, our reaction times also start to lengthen, meaning we can’t correct ourselves as quickly as we used to. Our sense of balance also fades with aging.
These changes caused by normal aging set up the perfect storm for injury.
How can one ensure the golden years remain golden when the risk for falling is high? If you or your loved ones are over 65, it’s time to consider “senior proofing” your home and theirs. Whether you are caring for a parent or trying to maintain your own independence, prevention is the key to keeping seniors safe. A few simple steps can help keep you and your loved ones safe.
Even with reasonable preventive measures, accidents can happen. If you are living at home alone or your partner can’t get to you quickly in an emergency, consider how you will be able to call 911 if you fall. Keeping a phone in your pocket or wearing an alarm device can be lifesaving.
If you fall, you will likely need to work with an orthopedic doctor and possibly a physical therapist. Together, they can help treat the injury and help you restore mobility.
At Gateway Gardens Assisted Living & Memory Care here in Winder, we know caring for an older adult brings joys and challenges. Our mission is to change the way the world ages. We provide seniors with quality care that enables them to live happier and healthier lives. Our services are distinguished by the caliber of our caregivers, the responsiveness of our staff and our expertise in Live-In care. We embrace a positive, balanced approach to aging centered on the evolving needs of older adults. For more information, contact us here at Gateway Gardens anytime!
31 August 2022

Hello and welcome back to our Gateway Gardens Assisted Living & Memory Care blog. Today we turn our focus to the upcoming Labor Day weekend and how all of you providing assisted living care and/or memory care support services to a loved one.
Labor Day is more than just an annual holiday that marks the end of summer. The original intent behind creating this federal holiday was to honor "the contributions that workers have made to the strength, prosperity, laws, and well-being of the country." And who are the often-overlooked workers that need to be included in the celebrations this year? Caregivers of aging parents.
Family caregivers are typically underappreciated and underpaid. In fact, according to data collected by the Family Caregiver Alliance, there are approximately 34.2 million people in America currently providing unpaid care to aging parents. The economic value of these services was found to total nearly $470 billion in 2013, and that number is expected to rise in coming years.
As someone caring for elderly parents, you can’t ever really take a day off...or can you? Here are some reasons why you should consider taking a break this Labor Day:
Caregiver Burnout Is Real
When you are caring for elderly parents on a regular basis, you run the risk of developing caregiver burnout if you don’t take time to recharge your batteries from time to time. Burnout can manifest itself in different ways, according to WebMd, including:
Caregiver burnout affects both your physical and emotional health, and can even lead to strained relationships with a spouse or close friends. But there is hope: caregiver burnout can be prevented by creating boundaries and carving out more time for yourself.
Practicing Self Care Can Help You Recharge
Self-care for caregivers is so important for your ability to care for aging parents over an extended period of time. Indulging in some “me-time,” whether that’s a long weekend at a bed and breakfast, a quiet hour to read a book, a commitment to exercising regularly or even just a warm bath at the end of a long day can help preserve your mental and emotional health when caring for elderly parents.
WebMd sums it up nicely, by reminding caregivers that “taking care of yourself is not a luxury; it is an absolute necessity if you're going to be an effective caregiver.”
All of us here at Gateway Gardens Assisted Living & Memory Care here in Winder do everything we can to make sure all seniors and their families feel comfortable, happy, and at ease as a cherished member of our community.
29 August 2022

Hello dear residents, resident’s family, and the entire local community who are struggling through providing in-home assisted living or memory care services. This goes out to you whether you are or are not actively searching for professional assisted living or memory care services in and around Winder. Those of you who follow our assisted living and memory care blog know that we invest in all of you by offering the lessons learned of our entire highly trained, skilled, and loving staff.
Everyone needs to be aware of the signs of stroke and know exactly what to do when these signs appear. Americans suffer strokes at a rate of one every 40 seconds, according to the Centers for Disease Control and Prevention. Nearly 75 percent of strokes occur in people aged 65 or older. However, age-related risk begins around age 55, and a stroke can happen at any age.
Strokes are categorized by their causes:
During a stroke, brain cells can quickly become damaged. This is due to a lack of oxygen. Symptoms may first develop in parts of the body which are controlled by those damaged areas.
One’s lifestyle choices, health conditions, and family history can increase a person’s risk of stroke. Although some of these risk factors may be outside of your control, the CDC estimates that up to 80 percent of strokes may be prevented through lifestyle changes alone.
Conditions such as heart disease, high blood pressure, high cholesterol, obesity, and diabetes may increase one’s risk of stroke. The chances of having a stroke are also higher for those who have already experienced a stroke or TIA.
Lifestyle and behavior factors that increase the risk of stroke are similar to those that increase one’s risk for heart disease. This includes physical inactivity, smoking tobacco, and drinking excessive amounts of alcohol. Nutritional factors are also a concern, as eating a diet high in cholesterol, sodium, and saturated fats can also increase a person’s risk of stroke.
A stroke can occur at any age. However, after age 55, a person’s chance of stroke doubles nearly every decade. Strokes occur more frequently in women than men, and race or ethnicity — especially for Black, Hispanic, American Indian, and Alaska Native individuals — may heighten stroke risk as well. One’s family stroke history and certain genetic disorders such as sickle cell disease may also increase risk. Knowing your family’s history of stroke may help you take preventative actions earlier on.
Become more familiar with these five common stroke indicators and empower yourself to save your own life – or the life of someone near you.
If you or someone near you experiences any of these signs, call 911 immediately. Medical professionals will need to make an assessment and begin treatment as needed.
Remember that fast, professional treatment is key for ensuring the best outcomes in the event of a stroke. Do not drive yourself or someone else to the hospital who may be experiencing a stroke. Your best course of action to treat yourself or the person with you is to dial 911 and request an ambulance.
Every minute counts when it comes to a stroke. This easy to remember assessment from the American Stroke Association can help you determine if you (or a person near you) is experiencing a stroke. Most successful stroke treatment occurs within the first three hours after symptom onset. Commit the stroke acronym F.A.S.T. to your memory. It could help save a life.
We hope you benefit, are encouraged, educated, and enjoy our blogging efforts. When the time comes for you to seek a consult regarding caring for your loved one’s professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care in Winders stands ready to improve the quality of both you and your loved one’s lives. Call us!
24 August 2022

Today five million people in the U.S. are living with Alzheimer’s disease and related memory loss. As our population ages, that number will increase. Appropriate support services and environments such as those that residents of Gateway Gardens Assisted Living and Memory Care here in Winder enjoy, help them make the most of their remaining abilities. We ensure each unique person participates in the community and thrive upon social interaction and engagement even as the disease progresses. “I’m still me!” we hear many people with memory loss say, even as their needs and abilities change.
Yet studies show that people with dementia often feel excluded from everyday life, and this is largely due to the unfortunate stigma associated with the disease. Sadly, some people avoid a friend who’s been diagnosed with Alzheimer’s. Family, too, can experience the effects of this prejudice. Friends and even some family members sometime avoided you and don’t want to talk about your loved one’s condition.
This stigma is based on ignorance. Studies disprove so many myths about Alzheimer’s disease. For example, many people assume that people with dementia are miserable. Yet studies show many people with early-stage Alzheimer’s report having an improved outlook on life! University of Kentucky researcher Dr. Gregory Jicha noted that while depression, denial, and despair might come with the diagnosis, many people he studied expressed an appreciation and acceptance of life, lessened concern about failure, and strengthened relationships.
It’s important to fight this stigma, as we would any prejudice. Negative attitudes harm the quality of life and even stand in the way of a prompt diagnosis, and the best advance planning.
Change is possible. People with dementia and their allies are working to improve the attitudes of the public. More public programs and resources seek to support and meet the needs of people with dementia, and to create appropriate opportunities for people with and without memory loss to interact in ways that break down barriers.
A group of people in the Alzheimer’s Association National Early-Stage Advisory Group offered these suggestions about how people with memory loss can help combat the stigma:
Family and allies are also vital to fighting this prejudice! They can focus on their loved one’s remaining abilities and advocate for them with information, the best way to dispel prejudice. At Gateway Gardens Assisted Living & Memory Care, we can attest that each resident is a unique individual. The goal of our community is to allow each resident to feel valued, successful, peaceful, cared for, and loved.
22 August 2022

As always, welcome back to our senior living & memory care blog where it is our passion to assist our assisted living residents and family, our memory care residents and family, and of course to all of you at-home caregivers as well.
Some of you at-home care givers simply need a break from caregiving and have a hard time both finding and building trust with prospective temporary care givers. While this blog post is primarily focused upon how to qualify professional care providers like us here at Winder's Gateway Gardens Assisted Living & Memory Care, many of the same considerations apply to you at-home care providers, and we hope this helps you as well.
“How do I qualify a professional care team to take care of my loved one?” This is a question we hear often when a person is searching for the best situation for their senior loved one’s care needs but are struggling with guilt and uncertainty.
When considering a move to assisted living or memory care, it is important to get to know the people caring for your loved one. Ask about team culture. Take the time to share a bit of yourself with the care team. You may find they become a valued friend to you and your family.
The caregivers who care for your loved one spend a lot of quality time with them, quickly becoming a care partner with them. However, for family members who do not have that same quality time, there are still ways to connect with care teams so that you can feel secure in the care decisions for your loved one.
The first part of feeling comfortable with making a care decision is in the tour process. You will have time to see how care teams engage with current residents. The following ideas may help you in your decision process as to whether the community you are touring is the right fit for your loved one:
How are the caregivers engaging with the residents? Do you see a friendly familiarity? Are they respectful?
Say hello to a caregiver and ask a question of them! When touring, if you see an opportune time, introduce yourself to a care team member, housekeeper, or server. Ask them about ways that they get to know their residents and how they personalize their care.
Discuss with the administrator what the company culture is like there at the community. A happy team is often a sign of an engaging community.
Once you have made the decision for a care community, you have several opportunities to connect with your loved one’s care partner. Some suggestions:
When you visit, check in to see which care members are caring for your loved one. Get to know them by name, talk to them about your loved one’s care, and take a little time to get to know them (as they are able, of course.)
Go to events! Join caregivers, residents, family members, and the rest of the staff at community activities and events. It is a great way to see the engagement and to get to know those who care for your loved one.
Take part in care meetings. Care meetings are your opportunity to truly create a partnership with the care team and overall care plan for your loved on.
We are so proud that our team of professionals at Gateway Gardens Assisted Living & Memory Care here in Winder goes the extra mile to make sure our seniors and memory care residents are safe, comfortable, and happy. Come see for yourself!
17 August 2022

When a parent or older loved one moves into an Assisted Living or Memory Care Community like ours here at Gateway Gardens, it is very important that family members and friends maintain the same level of connection with them that existed previously. Both our assisted living community and our memory care community are very supportive of this, as it plays a huge role in the overall well-being of their residents.
Let’s look at five great ways to stay physically and emotionally connected with your loved one here at Gateway Gardens.
To discuss this topic further or to discuss any question concern regarding assisted living or memory care services, contact us here at Gateway Gardens.
15 August 2022

Greetings once again to our faithful blog readers, cherished assisted living residents, memory care residents, and family members all! Over the past few weeks, we’ve had the privilege to consult a couple of callers concerned about their relatively young spouse exhibiting concerning cognizant behavior. One spouse was in his mid-40’s, the other mid 50’s. They both assumed away even a remote notion of Alzheimer’s setting in. They were completely uninformed about the subject of early onset Alzheimer’s. So today, we hope to get you all informed on this very subject.
Before diving into details regarding the later stages of early onset Alzheimer’s, let’s get clear on what the disease is. Early onset Alzheimer’s, also referred to as younger onset Alzheimer’s, affects individuals under age 65. Typically, these individuals are in their 40s and 50s. They often have careers, they may have children, and they may potentially be caregivers themselves.
Less common than late onset Alzheimer’s, early onset Alzheimer’s, according to the Alzheimer’s Association, currently affects 200,000 people in the United States.
As the Alzheimer’s Society describes, the earliest symptoms of early onset Alzheimer’s are linked to:
Although dementia is a progressive disease and worsens over time, the time it takes to progress varies depending on the individual. For some people, Alzheimer’s progresses rapidly, while it takes years to reach an advanced stage for others.
Now that you know, if you or a relatively young loved one displays such symptoms, talk to your doctor. Know that all of us here at Winder's Gateway Gardens Assisted Living & Memory Care are here for you.
10 August 2022

From all of us here at Winder's Gateway Gardens Assisted Living & Memory Care, we appreciate the positive feedback from our assisted living and memory care blog readers regarding the practical utility of our blog messaging. Many of our readers are at home taking care of their loved one’s Assisted Living support needs and/or their Memory Care support requirements. We are honored and humbled to lend a hand via our weekly blog posts. Today, let’s define for you who is a good candidate for professional assisted living support services.
Determining if assisted living is right for your loved ones can be an overwhelming decision, but we’re here to help make it as easy and clear as we can. A few questions you can ask are:
Depending on level of care needed, each assisted living resident has the ability to select specific services to help them day-to-day. When considering the future of long-term care for you or your loved one, our assisted living community here at Winder's Gateway Gardens Assisted Living and Memory Care is a great place to start. We deliver a solid foundation of care for assisted living residents allowing them to maintain maximum independence.
8 August 2022

We appreciate the positive feedback from all of us here at Winder's Gateway Gardens Assisted Living & Memory Care regarding the practical utility of our blog. It is now August, and the increasing heat index can be deadly for the young and senior alike. But summer danger is not restricted to the outside. While long days of sunlight are generally welcomed, there are reasons for at-home caregivers to be vigilant about summer safety for memory care loved ones inside the home.
The safety of our cherished residents in our top concern, and it should be for all of you at-home care givers as well. We feel a heartfelt responsibility to freely share our professional knowledge regarding professional assisted living and memory care support. So today, we’ll talk about the critical importance of proper lighting inside your home during both day and night.
There are several common problems experienced by those with dementia. We will discuss two:
Humans have a circadian rhythm, controlling when we sleep and when we are awake. This is mainly regulated by environmental factors such as the level of light that reaches the back of the eye, as well the times of mealtimes and level of activity during the day. Studies have shown a decrease of activity in the part of the brain that controls this rhythm in the elderly. As a result, they are less reactive to this process.
It has been found that persons with dementia spend as much as 40% of the night awake and a large portion of the day asleep. One of the negative results of this change of sleep patterns is the increased risk of falling, as these persons may get up during the night in low light conditions. It also leads to a reduced participation in physical, social and cognitive activities during waking hours.
There are many different theories as to why sundowning occurs. One of the reasons may be that less light reaches the back of the eye due to changes in the brain associated with dementia, causing the person to have a misinterpretation of shadows and objects around the home. This, coupled with the fact that many people with dementia develop tunnel vision, is a recipe for confusion. The changes in the brain can cause the person to interpret the change in light levels in the afternoon and early evening as a very sudden change in light levels. In rare cases, sundowning may also lead to aggression.
Proper light levels in the home help to address both of these conditions. Bright light exposure during the day has been shown to increase daytime wakefulness, improve night-time sleep and reduce evening agitation.
The general guidelines state that bright light (approximately 1000 lux, but no less than 600 lux) during the day stimulates the circadian rhythm. Natural light can contribute to orientate a person to the time of day.
It is especially important to ensure that corridors/hallways have proper lighting to reduce the risk of falls and to prevent shadows or dark spots that may be misinterpreted.
At night, it is recommended that night lights (if used) should not exceed 60 lux, as this can interrupt sleep. White light from screens or bright lights should be avoided at bedtime, as this disrupts the secretion of melatonin, the hormone that aides in sleep.
If you have any questions or concerns regarding how to provide both loving and safe care for your memory care loved one, contact Gateway Gardens Assisted Living and Memory Care here in Winder.
3 August 2022

Hello everyone from your friends and neighbors here at Winder's Gateway Gardens Assisted Living and Memory Care. We know that many of you struggle to come up with new ideas on what to discuss with your assisted living loved ones or your memory care loved ones. And we get it. Such “roadblocks” are not unique to our relationships with our elders. So, we have an idea for you to consider.
Visit and bookmark this link to NationalDayCalendar.com. Did you know that “National Chocolate Chip Cookie Day” is in this first week of August? Grab Mom, take here to the store, buy the necessary ingredients for the cookies (don’t forget the milk!), take her home, and make cookies together. If you are geographically separated from her, just call and say “Happy Chocolate Chip Cookie Day”. Let your lovely conversation with her go from there.
In the second week of August, we celebrate “National Family Day”. While we all may not need a reminder to focus on our family, sometimes we get caught up in the business of life. Perhaps there’s never time for the whole family to be together. Occasionally, we realize one family member, or another needs more attention. Time slips by, and we need to check in on a parent or an elderly relative.
There you go. Thirty-one days and countless ways to celebrate life with your loved ones. As always, if you ever have questions regarding professional assisted living services or professional memory care services, contact us anytime!
1 August 2022

If you have been diagnosed with memory impairment, stop and realize that you are not alone and that you are loved. Consider all of us here at Winder's Gateway Gardens Assisted Living & Memory Care to be a ready, empathetic, loving, and professionally experienced resource for you.
The level of grief associated with memory loss, both for the person with the impairment and for the caregivers, can be unexpected. These complicated feelings are valid and should be acknowledged to heal. Here are four strategies for coping with the grief associated with a memory impairment diagnosis:
The five stages of grief are denial, anger, bargaining, depression, and acceptance. Consider that you and your loved ones may be at different points in your grief journey and that acceptance may never fully happen. To ease the process, keep communication open and transparent with everyone involved. Compartmentalizing your emotions may also help you focus on the positive moments while you’re together, while carving out time for processing the loss after your visit.
When memory impairment begins to take its toll, grief and loss can feel overwhelming. Everyone copes with sadness in different ways, so it’s important to find the coping mechanisms that work best for caregivers and for a loved one experiencing memory loss. Acknowledge the stress and sadness that might be weighing you down, and focus on moving forward to enjoy time together. Start with identifying triggers that produce discomfort and implement habits to reduce stress levels.
Memory impairment can drastically change the parameters of a relationship, reversing the roles of who takes care of whom. Acclimating to a transition of power like this may take some time for everyone involved. Memory issues can also make you feel a loss of connection with your loved ones. Make time to vocalize the re-framing of your relationship and remain patient while you discover new connections.
There is a wealth of knowledge on the internet and in print material about dementia and Alzheimer’s disease. Our assisted living and memory care blog is a perfect example. People who experience memory impairment may process their grief and cope with their situation in different ways. Researching the science and psychology behind memory impairment will help caregivers understand and empathize with their loved one’s emotional reactions.
If you’re looking for professional assistance, our caregivers and staff are always happy to talk about the challenges you or your loved one are facing. Learning successful methods from experienced caregivers may provide families with the methods they need to keep loved ones comfortable.
Memory impairment brings with it a sea of new emotions and experiences for both caregivers and loved ones suffering from dementia or Alzheimer’s disease. Communicating and acknowledging your feelings of loss, being patient with yourself, and learning from a community of supporters are just four small ways to reduce stress as you move through the grief cycle.
If you are ready to speak to a professional, Gateway Gardens Assisted Living and Memory Care can help answer your questions and provide the resources you’re looking for.
27 July 2022

If you follow our blog, you know that we take great pride in helping you, our neighbors here in Winder who lovingly provide at-home assisted living care and/or memory care support to your loved ones. We know that along with your deep love for your memory care loved one, comes frustration in your unwavering commitment to their health and happiness. Today we’re going to focus on “single-minded tasks”, a process that you might try to help him or her achieve heightened levels of happiness.
Single-minded tasks are a great way to assist your loved one living with Alzheimer’s disease as they tackle day-to-day activities. Though the tasks may take longer to complete, your loved one may respond positively to having a sense of control in familiar situations. Take some time to adapt the activities they previously enjoyed, alone or with others, to their individual level of capacity.
You may have noticed your loved one now needs help with tasks that once were second nature to them. There is a lot that changes with Alzheimer’s or dementia, including memory loss, mood swings, social withdrawal, and more. It may be tempting to jump in and take over in the areas they are struggling with, but it is more important to maximize their independence, both for your relationship and for their self-esteem.
The repetitive nature of a routine provides a predictability that can be especially satisfying for people experiencing memory or cognitive issues. Single-minded, familiar tasks are easier to complete, bringing a sense of accomplishment and helping them connect with who they were before experiencing the challenges of memory loss.
Explore activities from your loved one’s past that they can accomplish on their own – washing dishes, organizing the mail, watering the plants – and establish a routine that allows them to have personal autonomy in those areas. When starting a new routine, utilize notes or lists to passively help your loved one remember what comes next.
Did you know multitasking makes your brain work harder, regardless of memory difficulties?
People with Alzheimer’s disease need more time to focus deeply on one thing without distraction before moving on to a second task. Asking them to complete two things at once can create confusion and agitation.
For example, if you ask your loved one to put on their coat, grab an umbrella, and turn off the light, they may get stuck on one request and forget the rest. Instead, ask them to put on their coat, wait for them to complete it, and then move on to the next request. Though it may take longer to get out the door, each task they complete is an exercise for their mind and body, and allows them to operate independently with minimal assistance.
Choosing the right environment for your loved one can make all the difference. Our memory care community is specially designed with residents’ safety in mind, while also promoting an appropriate level of independence. With the assistance of medical staff, memory care and assisted living facilities can provide your family with peace of mind and your loved one with the support they need.
If you are ready to speak to a professional, Gateway Gardens Assisted Living and Memory Care here in Winder can help answer your questions and provide the resources you’re looking for. Contact us anytime.
25 July 2022

If there’s one thing we’ve learned from professionally serving seniors, it’s that they are all unique. Here at Winder's Gateway Gardens Assisted Living and Memory Care, time has taught us to never underestimate the power of the individual.
Today’s senior has evolved away from the one-size-fits-all model. Savvy older adults are wanting more control over their lives and are demanding convenience and choice. That’s why the Manor Lake philosophy is to create a lifestyle completely customized to each individual’s needs.
It starts by asking a lot of questions when residents first move to one of our communities. We then aim to suit each individual’s style and needs and encourage aspirations. Resident needs are at the heart of whatever we do. We’re united for you – the individual – and your best interests.
Once you move into our community, we’ll ask plenty of questions to get to know you so we can make your life right for you in every way.
Think of it as a senior needs assessment – only more personal. It’s customized with details that pertain only to you. This collection of facts, preferences and stories about your life will form both the basis of our friendship with you and your lifestyle plan. This information is then used to create a uniquely relevant experience for you, where your needs are met in a style that suits you.
You want to eat lunch in your room instead of the dining room? Done. Would you like to invite a friend for tea and cookies in the lobby? Will that be hot tea or iced? Do you want your haircut appointment to be every other Wednesday or every single Thursday?
Learning more about your history, priorities and unmet needs helps us identify the programs, amenities and services that will best support your lifestyle. It also helps us enhance our assisted living active lifestyle offerings for every member of our community.
Whether your focus is upon assisted living support services or memory care support services, know that we are, and will always be, just a phone call away. Contact us anytime.
18 July 2022

Hello and welcome back to our Gateway Gardens Assisted Living & Memory Care blog. Today we turn our focus to all of you at-home care givers who looking for inspiration and strength to carry on in your assisted living care and/or your memory care support services. We’re here for you.
One of the most important things you can do as you walk this path is take care of YOU. Believe me, it’s easier said than done, but it really is important to stay healthy, that is mentally, physically, emotionally, and spiritually. As you watch your parent sink into the depths of dementia, it will consume you. You are fighting with the devil, and you will not enjoy many victories along the way. That said, what you can do, is stay alert, stay strong, stay healthy. Here are some at-home caregiver suggestions to keep you going:
All of us here at Gateway Gardens Assisted Living & Memory Care here in Winder do everything we can to make sure seniors and their families feel comfortable, happy, and at ease as a cherished member of our community. Give our team of senior care and memory care professionals a call today or schedule a tour anytime!
13 July 2022

Whether you are a faithful subscriber to our senior assisted living and memory care blog or have arrived us for the very first time, we are guessing your age is somewhere in your forties or older. People in their teens are locked down in their Twitter and Tic Toc accounts. People in their thirties and raising families and have relatively young parents. People in their forties have aging parents and they themselves might be starting to question their very own level of forgetfulness. Now, we don’t want to be Debbie Downers here today with you, but we do have some news that won’t settle well with any of you (and that includes yours truly, the author of this blog post). Some foods are particularly bad as they can contribute to forgetfulness regardless of your age. It’s all about Oxygen.
There are things that people put in their bodies that limit the amount of oxygen getting to the brain, causing it to operate at less than full capacity. Smoking has this effect and so does eating certain foods. Human body cells naturally lose their ability to carry oxygen as people age, which is why it’s important to choose foods that do not contribute to oxygen depletion.
So, here it is folks. The following foods use more oxygen than they provide:
To be clear, you senior assisted living care team and your memory care support team here at Gateway Gardens are not “outlawing” these food favorites. However, if you and/or your loved ones at home eat these foods regularly, should offset the ill effects by increasing your vegetable and fresh fruit daily. By default, if you do this, you’ll eat fewer hamburgers and pizza.
11 July 2022

If you are a subscriber or frequent viewer of our assisted living and memory care blog, you know that here at Winder's Gateway Gardens Assisted Living and Memory Care, we take great pride in our holistic approach to managed care. We invest heartfelt time and energy managing this senior care blog for the purpose of assisting those of you at-home senior care providers to help you deliver the best care possible. We want all of you to consider us a ready resource for information and advice that is intended to help improve your quality of life as well.
So, today let’s talk about the most common dietary deficiencies effecting today’s seniors who are not serviced by professional senior assisting living or memory care community living support. As our loved ones grow older, they start to expend less energy and require fewer calories as compared to the past. This means that eating foods that are healthy and nutritious are very important for the elderly as every calorie counts. However, it may be challenging to get enough nutrients to prevent dietary deficiencies like mineral or vitamin deficiencies. Read on to find out more about the most common dietary deficiencies!
There are several reasons to why mature adults are more prone to vitamin and mineral deficiency. Firstly, as people age, their bodies do not absorb nutrients as well as before, thus putting them at risk of nutrient deficiency. Furthermore, some medications that they are required to take end up interfering with the body’s capability to absorb vitamins and minerals.
With age, their teeth also become weaker, and some even lose their teeth. This makes it difficult for them to consume certain types of foods that are rich in nutrients, such as vegetables and fruits. Furthermore, as their mobility decreases, it may be hard for them to make grocery runs frequently to stock up on nutrient-dense foods.
Vitamin B12 Deficiency
Vitamin B12 is an important nutrient in our body and is needed for the body to construct the DNA in our cells. However, with age, vitamin B12 is absorbed less efficiently into the body. A deficiency of vitamin B12 in the body can lead to pernicious anemia. Some symptoms to look out for include vision that is blurred, breathlessness or dizziness, fatigue or weakness, issues with walking, an inflamed tongue, tingling sensations in the feet and the hands, mood swings, or changes in memory.
Calcium Deficiency
Calcium is another important nutrient in the body that is in charge of keeping the teeth and bones healthy and strong. Men over 70 years old and women over 50 years old are more prone to calcium deficiency as the body is less able to absorb calcium properly with age. This could also be linked to a lack of vitamin D. If the body is deficient in calcium, it will start absorbing calcium from the teeth and bones and could lead to osteoporosis and weak bones in the future.
Vitamin D Deficiency
To maintain a strong immune system, the body will need sufficient vitamin D to help the nerves and muscles in the body do their jobs. Vitamin D can also help the body have a more efficient absorption of calcium. A vitamin D deficiency is one of the most common vitamin deficiencies in America.
As people age, it is important to ensure the body remains healthy and strong by giving it the nutrients it needs. Feel free to contact us to find out more about our senior living and memory care communities!
6 July 2022

In our continuing effort to support those of you who lovingly support your senior loved ones, our team of Winder-area assisted living and Winder-area memory care professionals thought it would be wise to again share eight facts you should know about summer and senior care. We want all of you at-home care providers to fully understand that older adults are especially susceptible to heat-related injuries and heat stroke.
So, senior caregivers, please consider and take heed knowing that:
If you have any questions or concerns regarding how to provide both loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Winder.
29 June 2022

The 4th of July is a very special day on the American calendar. As such, there is no reason that anyone who wants to celebrate it should be prevented from doing so. Here at Winder's Gateway Gardens Assisted Living and Memory Care, we work hard to make sure that this extends to all our cherished residents. For you caregivers at home, sometimes figuring out how to make it fun for your assisted living or memory care loved one can be hard. Here we look at some ways of facilitating that.
There are two categories for holiday activities: a) those that take place outdoors and b) those that take place indoors.
For those who enjoy the outdoors, remember the following:
For those who would rather stay indoors, consider these activities:
We hope you enjoy a safe and fulfilling 4th of July celebration with your entire family. Seniors need and deserve your special attention, especially around holidays. By giving them special attention during this year’s fourth of July celebrations, you will be rewarded immensely as well. To learn about our approach to professional assisted living and professional memory care services, call us anytime!
27 June 2022

We wish to express thanks to those of you who provided such warm and welcome feedback on our recent five-part blog series focused on signs that transition to professional memory care is well advised. As you know we manage our Winder-area assisted living and our Winder memory care community blog for people like you doing your best to care for your loved one. Your feedback confirms that our blogging efforts do indeed provide meaningful and actionable guidance and advice. So, thank you.
If you missed any of our five-part series focusing on a single indicator of signs that a transition to professional memory care, for you ease of reference, here are the links to those blog posts:
We understand these are difficult and frightening conditions to consider. This is even more reason why we are warmed by your feedback and trust to turn to us for thoughts and advise on the subjects. As we’re sure that you are aware, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. Our warmest best wishes to you all, and again, thanks for your feedback!
22 June 2022

If you are one of our blog fans, you know that we pride ourselves here at Gateway Gardens Assisted Living & Memory Care (Winder) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Winder who lovingly provide at-home assisted living care and/or memory care support to your loved ones. Today we’re going to discuss how fundamentally important it is for you to love yourselves first before you can be truly loving to your senior loved one with assisted living or memory care needs.
A necessary part of searching for happiness in life is practicing self-love. But why is self-love so important for everyone, but especially important for those of you providing assisted living or memory care support to a loved one?
Some mistakenly believe it is a “good” thing to be hard on yourself. According to STANFORD MEDICINE, self-compassion and self-love have a multitude of benefits.
Other benefits of self-love include feeling optimistic, lowering the risk of anxiety and depression, and healthy behaviors. There are three main components to self-love and with older loved ones, they may need to be gently reminded of one (or all three) of these aspects.
Treat Yourself
The first aspect of “treat yourself” is an inner, emotional response to your own actions and thoughts. Even when you make a mistake, instead of being harsh, try to be patient with yourself. If a friend or family member makes an error, would you yell at them for their mistake? Often, we will reach out to a helping hand to those close to us, but when it comes to self-evaluation, we can be extremely tough on ourselves.
Practice Mindfulness
As we age, it can be easy to become set in our ways. Being mindful is being generally curious and open to new ideas; having a child-like wonder as some may call it. Practicing mindfulness is also related to having a non-judgmental attitude. When you practice mindfulness, with self-love, it can translate into not fixating on negative events or stories about yourself.
We Are Only Human
“To err is human, to forgive divine.” – Alexander Pope
You need to remind yourself every now and then that you are human. You are going to make mistakes, and that’s okay! Accepting that you are not perfect is part of being human. Forgiving yourself when you do make a mistake is an act of self-love, not weakness.
If you are patient with yourself, you can enhance your senior living experience.
At some point, all the love in the world may not be enough to carry the day for severe senior assisted living and/or memory care challenges. Gateway Gardens Assisted Living & Memory Care here in Winder offers a wide range of care options that can help alleviate some of the stress, anxiety, and fatigue that come with caregiving on one’s own. We offer senior assisted living and professional memory care services here in Winder and we will work with you to determine what is right for you and your loved ones.
20 June 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. This is the fifth and final blog post within our five-part series focusing on a single indicator of signs that a transition to professional memory care will be in the best interest of your loved one.
Here are the links to our prior posts on this subject:
As dementia progresses, a senior's ability to maintain relationships also changes. They will need people around them who understand dementia and can provide a gentle form of company that does not demand consistent memory continuity. Most seniors in assisted living are not experiencing dementia and are not trained in supporting relationships with a dementia patient.
However, every caregiver within our memory care community is professionally trained in providing memory care, understands dementia, and can help residents maintain relationships with both staff and other residents. Furthermore, memory care staff can help coach family and friends on how to communicate with their loved ones to produce happy and rewarding interactions. If your loved one is having difficulty maintaining relationships or seems to be withdrawing from their friends in assisted living, or even forgetting their friends in assisted living, it may be time to make the transition to memory care.
We understand these are difficult and frightening subjects to consider. With that said, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
13 June 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. This is the fourth blog post within our five-part series with each post focusing on a single indicator of signs that a transition to professional memory care will be in the best interest of your loved on.
Here are the links to our prior posts on this subject:
As dementia progresses, a senior's ability to maintain relationships also changes. They will need people around them who understand dementia and can provide a gentle form of company that does not demand consistent memory continuity. Most seniors in assisted living are not experiencing dementia and are not trained in supporting relationships with a dementia patient.
However, every caregiver within our memory care community is professionally trained in providing memory care, understands dementia, and can help residents maintain relationships with both staff and other residents. Furthermore, memory care staff can help coach family and friends on how to communicate with their loved ones to produce happy and rewarding interactions. If your loved one is having difficulty maintaining relationships or seems to be withdrawing from their friends in assisted living, or even forgetting their friends in assisted living, it may be time to make the transition to memory care.
We understand these are difficult and frightening subjects to consider. With that said, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
6 June 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. This is the third blog post within our five-part series with each post focusing on a single indicator of signs that a transition to professional memory care will be in the best interest of your loved on.
Here are the links to our prior posts on this subject:
Mental continuity is a serious concern when a loved one has dementia. While you may be used to your loved one being a little confused sometimes or forgetting a few things, these signs can develop into a growing lack of independence. If your loved one is confused often, to the point that they are having trouble keeping track of their personal affairs or community activities, then it may be time to consider moving from home care, or an assisted living community, to memory care.
Signs that dementia care may be necessary include increased confusion, piles of unopened mail, inability to understand their current medications or health care treatment plan, and regularly misplaced items. Extreme forgetfulness, like forgetting your visits or the friends they have made in the assisted living community, is also a sign that memory care might better support your loved one.
We understand these are difficult and frightening subjects to consider. With that said, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
1 June 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. This is the second blog post within our five-part series with each post focusing on a single indicator of signs that a transition to professional memory care will be in the best interest of your loved on.
Here are links to our prior posts as well as topic definitions for future posts on this subject:
One of the early signs that memory care may be necessary is whether your loved one is no longer an active part of the assisted living community. Assisted living is designed to give seniors as much independence as possible, only stepping in to provide care services and support when a senior needs assistance. Restaurant-style dining and housekeeping, for example, remove most of the constant physical strain from one's lifestyle, while community and social activities provide ample opportunity to socialize and stay engaged.
Have you noticed your loved one stop participating in community events? Do they no longer take advantage of meals in the dining room without prompting, or seem disinterested in activities? These changes may be a result of their dementia making these things more challenging. Memory care will help them by providing a more guided experience that ensures they are still finding enjoyment, getting enough to eat, and remaining appropriately stimulated.
If you find yourself providing more special care than you expected, or if your loved one is always in need of familiar companionship, this is another sign that a transition to memory care may be approaching. Assisted living is a living option meant to allow friends and family respite from constant care, yet the freedom to visit and socialize whenever they can. However, families starting to find that assisted living does not provide the care needs or depth of support needed by a loved one due to dementia should consider memory care as the next step. Your loved one may begin calling more frequently, asking you to stay longer, or just needing more during your visits.
Memory care is designed to help seniors not only live comfortably but also experience their senior living in a more guided and supported way. This includes helping them avoid overstimulation and situations that they have come to find upsetting, helping them to feel supported and safe, and helping loved ones to keep their visits more fun.
We understand these are difficult and frightening subjects to consider. With that said, here at Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
30 May 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. We hope you had a loving and memorable Memorial Day Holiday. We are certain that those who invested the ultimate sacrifice look down upon us in celebration of the enabling role that they played in securing our freedom. We hope your Holiday weekend was truly rewarding.
This is going to be a very busy week for us here at Gateway Gardens Assisted Living and Memory Care because, well, the week after Memorial Day always is. From experience, we know that in the days after an extended Holiday break, families across the nation reflect upon the extended time with their senior loved ones and the new concerning observations about their mental acuity. Our phones will ring all week with voices on the other end asking variations of the same question: “When is the right time to move from assisted living to memory care”?
This question is one that is both foundationally important and very difficult to answer due to the unique personal variables involved. So, given the public’s high focus upon this question, we thought we’d cover the next few blog posts on individual discussion items regarding how to determine when your loved one have become strong candidates for professional memory care.
In our next blog post, we’ll continue upon this same subject but specialize upon a few factors that directly relate to indicators regarding when a transition from assisted living to memory care living should strongly be considered. Just for your reference, here are the future subjects and back-links to them once posted:
The answer is, it depends. Everyone experiences dementia differently. Some loved ones can fully and comfortably live out their diagnosis in an assisted living community, even as they progress through the early stages of dementia. However, as the stages of Alzheimer's progress, a better quality of life may necessitate moving your loved one from assisted living to a memory care community. That decision can be difficult, especially because you must make it on behalf of your loved one. And it may be even harder if they believe they're doing just fine at home with you or within their existing assisted living community. But transitioning to a memory care community can offer significant benefits and safety that often improve the quality of life for a loved one affected by dementia.
Memory care is a special variation of assisted living designed to provide a greater level of care for seniors living with some form of dementia. Since assisted living and memory care communities are similar, seniors transitioning from independent living to memory care still have the benefit of a senior living community, activities, 24-hour full-time staff members, meals, and assistance with activities of daily living. But the environment, care options, and lifestyle provided are carefully shaped to help seniors living with a memory loss disease, like Alzheimer's disease. These aspects help seniors by reducing confusion, keeping them engaged, and encouraging a life filled with happy moments, all while remaining safe. The transition from assisted living to memory care is generally the easiest when transitioning within communities offering both assisted living and memory care.
We understand these are difficult and frightening subjects to consider. With that said, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
23 May 2022

Here at Winder's Gateway Gardens Assisted Living and Memory Care, we take great pride in our holistic approach to managed care. We invest heartfelt time and energy managing this senior care blog for the purpose of assisting those of you at-home senior care providers to help you deliver the best care possible. We want all of you to consider us a ready resource for information and advice that is intended to help improve your quality of life as well.
With steadily rising outdoor temperatures, we thought it smart to cover the VERY important topic of hydration. Every bit of advice listed below should be considered advice for both you and your senior loved one. So here you go, seven tips to stay hydrated this summer:
[Bonus for you parents out there!]
Our bodies are made up nearly 60% of water and kids are an even greater percentage. Every cell, tissue and organ in our body relies on water. For example, our bodies rely on water to regulate temperature, remove toxins, and keep our joints lubricated. When we talk about hydration, it means keeping our water levels in our bodies in a healthy range so we can function at our best.
You should drink half your body weight in ounces of water each day. (Ex: If you weigh 120lbs, you should drink 60 ounces of water each day.). One of the simplest ways to know if you’re drinking enough water is the color of your urine. In most cases, a well-hydrated person will have colorless or light yellow urine. If it is dark yellow or amber, it may be a sign of dehydration. Another telltale sign you’re dehydrated? You’re thirsty. If you’re thirsty, you’re already dehydrated and you need to pick it up!
We’re glad to have you here on our assisted living and memory care blog and hope you find it useful. Refer back to the above links to our four chiropractic clinics and call us anytime you have questions regarding how we can help you manage pain.
16 May 2022

We pride ourselves here at Gateway Gardens Assisted Living & Memory Care (Winder) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Winder who lovingly provide at-home assisted living care and/or memory care support to your loved ones. Today we’re going to discuss some things that you caregivers can do to take the stress out transitioning to professional care sometime in the future.
Preparing for your future.
Everyone can benefit from a bit of downsizing. Over the years we accumulate so many useful things as well as clutter. Letting go of things we’ve acquired seems like an especially daunting process for seniors, but it can be very simple, therapeutic, and rewarding. A big part of senior living is enjoying peace of mind and having less stuff will give you exactly that.
Start early and start small.
Downsizing is an easy task if you start chipping away at unwanted things little by little. Don’t start with big projects that may discourage you from continuing.
Getting rid of a few things a week like duplicate kitchen utensils and pans are a great place to start. Consider rooms that you won’t have at your new residence and find creative ways to eliminate their clutter. Turning your home office into one desk’s worth of essentials or organizing tools into one toolbox makes for a smooth transition.
Garages and attics usually require the most attention. Holiday decorations, temporary hobby items and things that just don’t fit anywhere else usually end up here. Make a goal to pack what you need over a few weeks or months from those areas. Whatever’s left over can be sold, donated or discarded. Have a plan for where items will go and avoid “maybe” piles.
We encourage you to bring your hobbies, culture and accomplishments to your new home. The things that will bring you joy and meet basic needs are important to have. At Gateway Gardens Assisted Living and Memory Care, we accommodate independent living, assisted living, respite care and memory care.
Take into consideration all of the included services like meals, housekeeping and maintenance you’ll receive at a Manor Lake. Factor those into what you won’t need in your new home.
What will I NOT need at a senior living community?
Our community has a lot of things you’ll need. Items that are a part of your hobbies and interests or cherished memories will be important to keep.
We hope you find this useful. As always, thanks for reading and if you have any questions, contact us anytime.
9 May 2022

If you’ve ever flown on a commercial flight, you were briefed that “in the event of an emergency, secure your oxygen mask first”. This clearly makes sense because you can’t serve those dependent upon you unless you take care of yourself first. One of the things we take seriously here at Winder's Gateway Gardens Assisted Living and Memory Care is a commitment to all of you out there providing at-home assisted living services and/or memory care services.
You too, at some point in your life may find yourself taking care of aging parents or elderly members in your family, in the same way, they cared for you. Never forget that it’s not easy for your elders, who were once independent, to become dependent on you or on others for their basic care. You can never say what turn life may take. God forbid if a parent has a sudden accident or slips in the bathroom – would you really be in a state to handle such a situation?
You can’t be a full-time and fully focused at-home senior care provider. You must address your professional obligations, your home, and your family. Add in senior care responsibilities and life can surely become overwhelming. This is the primary reason why people opt for professional assisted living services and professional memory care services. No matter how much we love our parents and elders, at some point our cumulative responsibilities will render us all unable to meet the ever-increasing challenges of senior care.
Until that time arrives, for the sake of your loved ones, take care of yourself first. Maybe that means seeking periodic relief via short term “respite” senior care services. There is a volume of clinical study that reveal that those who take care of elders are at risk for anxiety, depression, stress, and musculoskeletal disorder. We understand and can advise. It’s what we do and here at Winder's Gateway Gardens Assisted Living and Memory Care, we’re here for you!
2 May 2022

Today we look to educate all our Winder-area assisted living and our Winder memory care community residents, family, neighbors, and friends on the subject of arthritis, an ailment common to so many.
Any chronic health condition can impact day-to-day life, and arthritis comes with its own set of challenges. So, what is arthritis? Understanding the nature of the disorder will empower you to make changes to enhance your wellbeing.
The most common form of arthritis – Osteoarthritis – causes deterioration of protective joints over time, and commonly affects the knees, hips, spine, and hands. Rheumatoid arthritis is an autoimmune disorder that can affect the joints and attack body tissues. The condition can lead to joint deformity and bone erosion. While arthritis can create difficulties, you can take steps to manage pain and improve your quality of life. Be sure to consult with your doctor before considering any of the suggestions that follow.
While your doctor may prescribe medication as a way to manage arthritis, these home remedies can act as natural treatments to help alleviate pain and inflammation.
Heat and Cold
An electric blanket or hot shower can diminish discomfort and alleviate stiffness. Cold application works best to relieve swelling, joint pain, or inflammation. You can freeze or microwave gel packs to apply cold or heat to your liking.
Lemongrass Essential Oil
Essential oils are known for their soothing scents, and they have other beneficial properties too. A 2017 study found that lemongrass essential oil can reduce pain from rheumatoid arthritis. For safe application, dilute essential oils and test them in a small area to check for sensitivity or allergic reactions.
The following tips can enhance your overall health and help you manage arthritis.
Weight Management
The degeneration of cartilage can put strain on your joints and carrying around extra weight can put pressure on your feet, knees, and hips. Talk to your doctor about a weight loss plan to prevent future damage and improve your mobility.
Exercise
Staying active is an excellent way to engage and strengthen vital muscles around your joints. Low-impact exercises like walking, water aerobics, or swimming are a great way to build strength. Exercises to improve balance also help combat aches and pains. Getting social is a wonderful way to stay motivated, so check out the engaging activities in your senior living community.
A Healthy Diet
A nutritious diet loaded with fresh fruits and vegetables affects every aspect of your health, from the glow of your skin to the strength of your bones. A diet full of saturated fat and processed foods not only contributes to obesity – thereby accelerating degeneration of the joints – but can also aggravate inflammation. Try the following foods that are rich in antioxidants to remove free radicals from the body:
Flare-ups can be par for the course with arthritis. Luckily, there are simple methods you can use to reduce stress and enhance arthritis pain relief.
Stretching when you get out of bed is a gentle way to get in tune with your body and can also boost your mobility. A simple knee hug or torso twist can make all the difference during arthritis flare-ups.
Lift Your Mood with Calming Music
If arthritis pain has you feeling low, your favorite upbeat tune can be an instant way to shift your thoughts. Audio therapy can also help if you’re having trouble sleeping, and binaural beats in instruments such as the piano or organ can increase relaxation and lower stress.
If you or your loved one struggle with arthritis, talking with your doctor is most definitely your first place to start. Bring the aforementioned ideas to him/her knowing that our assisted living and memory care community here in Winder is designed to support our senior residents which includes assisting in prescribed arthritis treatment.
25 April 2022

Welcome back to our blog page for our Winder-area assisted living and our Winder memory care community. No matter what stage of care need your elderly loved one is at, you can trust that you have proven professionals right around the corner here at Gateway Gardens Assisted Living & Memory Care to deliver genuine quality of life improvement to you both. Today, we feel it is important to educate you on the differences between Alzheimer’s and dementia. They are related but clearly unique subjects.
Many people outside of healthcare mistakenly confuse dementia with Alzheimer’s, yet the two are very different conditions. While both can affect memory, there are clear distinctions. What follows is a look at what these differences can mean for patient symptoms, long-term outlook, and patient memory care need.
The confusion many people have between Alzheimer’s and dementia is understandable, as Alzheimer’s is both the most common cause of dementia and one (but not the only) form of dementia. Dementia is the name for a group of brain disorders that make it hard to remember, think clearly, make decisions, or control one’s emotions. Dementia is not a normal part of aging. It is caused by damage to brain cells that affects thinking, behavior, and feelings.
While Alzheimer’s makes up an estimated 60 to 80 percent of overall dementia cases, it’s not the only form of dementia. Alzheimer’s is a specific disease, while dementia is not. There are many other forms of dementia with different causes. The symptoms for those forms of dementia may or may not overlap with the symptoms of Alzheimer’s. For example, vascular dementia is typically caused by a stroke. While later symptoms often include memory problems, initial symptoms are more likely to include things such as poor judgment and trouble planning. Dementia With Lewy bodies (DWB) occurs when Lewy bodies — microscopic protein deposits in the brain—form and impair cognitive function. Along with the memory loss and decision-making challenges found in Alzheimer’s and vascular dementia, DWB can also cause hallucinations, daytime sleepiness, and physical movement issues, such as trembling or slowness. Those suffering from Parkinson’s disease have a 50 to 80 percent chance of developing Parkinson’s disease dementia, which is similar to DWB.
Why are facts about Alzheimer’s AND dementia important? Memory care involves taking steps to mitigate the impacts of dementia in patients as possible. While some forms of dementia have the potential to be reversed if identified early enough, there is currently no cure or reversal available for Alzheimer’s specifically. Memory care therefore often involves cognitive exercises to help slow the progression of dementia or at least help patients better cope with its impacts.
We understand these are difficult and frightening subjects to consider. With that said, here at Winder's Gateway Gardens Assisted Living and Memory Care, we are highly trained and skilled subject matter experts on the two subjects. And we can help you whether you are a resident, resident family member, or a non-associated care giver simply doing their best to serve another. We salute you and want you to know that we are always open and ready to talk.
18 April 2022

Hello and welcome back to our Gateway Gardens Assisted Living & Memory Care blog. Today’s focus is fully upon all of you at-home care givers who looking for inspiration and strength to carry on in your assisted living care giving and/or your memory care support services. Family caregivers play a crucial part in keeping our families strong and healthy. More than 30 million Americans have reported caring for an elderly loved one in the past 12 months, and that number is expected to rise as our population grows and ages. We’re here for you and today offer five ways that can help you cope and deliver even higher levels of loving care for a loved one.
When we take on the responsibility of caring for a loved one, we may feel confident that our duties are clear and that we can handle it all. As we continue to care for them and the stresses and anxieties build-up, though, we may isolate ourselves from our friends and family and feel trapped, potentially leading to anxiety disorders and depression.
Book a coffee date with someone you trust and take the time to express any anxieties or frustrations you may be feeling. This won’t just help you relieve the stress that’s been building up inside of you but will also let you know that you are not alone in this situation.
It can be hard to ask for help from others when you’re already a caretaker for a loved one, but if you have siblings, cousins, nieces, or nephews, you do have a whole network of family members who can alleviate some of the stress.
Even if it’s just getting a cousin to take your loved one to their appointments, that’s one less task for you to do and a chance to stop and calm your mind.
If you’re taking care of a loved one, especially if they’re living with you, it can be difficult to find a time in your day to step away from your responsibilities and take care of yourself.
Even if you take a moment to stand outside in the fresh air for 10 minutes and to take little breaks throughout the day to ground yourself and breathe. This will help you put everything in perspective and avoid emotional burnout.
With all the tasks you might have to handle, including medication, medical appointments, and preparing healthy meals, it can be easy to be overwhelmed by everything around you. This is where a schedule can come in very handy.
Take care of yourself and your health by making time to get a proper amount of sleep every night, enjoy mealtimes to keep yourself fueled, and times when you can step away from your loved one to handle your own errands.
Many of us think that we must shoulder all the burdens associated with caring for a loved one. It’s never a bad thing to be educated on your loved one’s needs, but it can lead us to feel like we’re not doing enough or, worst of all, failing to take care of our family members or friends.
You are doing a selfless thing by taking care of your loved one and you should be proud of that, but you should also realize that there is only so much you can do. Taking the time to understand this can help you relax and focus on the things you can do for your loved one, instead of the things you struggle with.
Gateway Gardens Assisted Living & Memory Care here in Winder does everything we can to make sure seniors and their families feel comfortable, happy, and at ease as a cherished member of our community. Give our team of senior care and memory care professionals a call today or schedule a tour anytime!
11 April 2022

For elderly and seniors, the month of April is national “Stress Awareness Month” and a good time to take stock of your mental health. Well, allow us to customize that introduction if you may. For all of us, the month of April is national “Stress Awareness Month”. We talking to you all of you who could use at-home assisted living advice and/or at-home memory care service advice. Care stress is real, unavoidable, but can be successfully managed. Recall that every time you fly, the flight attendant briefs you and tells you to place the oxygen mask on yourself first before assisting others? To maximize the effectiveness of your caring love, you must take care of yourself first.
A person’s mental health centers around their emotional, psychological, and social well-being. Elderly people and seniors are like everyone else whose mental health affects how they feel, act, think, make decisions, and interact with other people. Having good mental health is vital to a person’s good overall health and enjoyment of their life.
The World Health Organization (WHO) estimates that about 15% of all adults over age 60 have a mental health problem. Those numbers may have increased during the COVID-19 pandemic, health experts say. Experts identify several common mental health issues for the elderly and senior population. These include:
Depression: Seniors and elderly who are depressed may feel consistently “low.” This can happen to caregivers as well. Enjoyment in life is hard for them. They may struggle with guilt, anger, shame, emptiness, hopelessness, and other similar feelings. It’s important to recognize chronic depression. If you or someone you know is thinking about suicide, call the National Suicide Prevention Lifeline at 1-800-273-8255.
Post-traumatic stress disorder (PTSD): Many people in the senior and elderly population have experienced loss, a dangerous event, and even shock. They may still struggle with their feelings around those events and be triggered by something that helps them recall those moments. Even in the safe and loving environment here at Winder's Gateway Gardens Assisted Living & Memory Care, your and our loved one’s can struggle with PTSD. We can help you deal with that.
Bipolar disorder: Symptoms include changes in a person’s mood and behavior. They may have manic episodes, which could be felling really good or depressive episodes in which they’re overcome by sadness, helplessness, or a general “down” feeling. They may struggle to do daily activities.
Addiction: It might be hard for you at-home caregivers to diagnose addiction or addictive behaviors. We are trained to identify signs of addiction and how to professionally respond. However, addiction is often overlooked by friends, family, or caregivers.
Anxiety disorders: These are ongoing continuous struggles with anxiety that may grow worse over time. For seniors and the elderly, common forms of anxiety include social anxiety disorder, depression, panic disorder, and obsessive-compulsive disorder.
Dementia: Forms of dementia can cause memory deterioration and lead to other symptoms. These include personality changes, difficulty communicating, erratic behavior, and personality changes. Dementia can have a detrimental effect on a person’s quality of life. We are highly trained and experienced in serving those with dementia (and their families too).
By getting professional help, seniors and the elderly can treat and manage these conditions. They’re nothing to be ashamed of and none of them are considered to be “normal” parts of aging. Contact us at Winder's Gateway Gardens Assisted Living & Memory Care anytime!
4 April 2022

On Easter, people of all ages spend time with their loved ones and celebrate spring. For many older adults, this holiday brings back wonderful memories of their childhood. It is also a great time to involve seniors with dementia in some exciting activities. If your elderly loved one has been diagnosed with dementia, know that all of us here at Gateway Gardens Assisted Living & Memory Care here in Winder send our deepest respect and send our best wishes for strength, wisdom, love, and peace.
One way we do this is by managing this senior living and memory care blog on the behalf of people just like you. All of us have deep passion for caring for our seniors and those requiring memory care. That is the sole reason we choose senior care as our full-time profession.
Easter season is a particularly beautiful period here at Manor Lake for all the same reasons it’s likely one of yours as well. But it is particularly heartwarming because the entire community rallies around our dear memory care residents in thoughtful and selfless ways. When we see our dear senior assisted living residents rallying around their memory care friends, it is truly a site to behold.
So, today we simply offer some ideas for you to chew on and possibly adapt to help make your memory care loved one’s life just a tad bit brighter.
The multiple steps involved in dyeing Easter eggs can be difficult for seniors with dementia. However, they can still have fun decorating the eggs with a little prep work from their caregivers. Before starting the activity, use a white crayon to draw fun shapes on eggs, such as bunnies and butterflies. Give your loved one some watercolors and encourage him or her to paint the eggs. The white crayon will resist the paint and the image will be revealed to your loved one.
For many seniors, Easter is about the new life that begins in spring, and growing a small garden is a wonderful way to celebrate the season. Help your loved one plant a small windowsill herb garden. This activity can be stimulating for seniors at various levels, beginning with your loved one watering the plants each day and eventually tasting the delicious results of his or her efforts.
Scents can stimulate memory in seniors with dementia, and lavender can help soothe anxiety. Help your loved one make a lavender sachet by providing small, colorful fabric pouches he or she can fill with lavender seeds. Once your loved one has filled the pouch, help seal it by either sewing or gluing the edges shut. Encourage your loved one to find a special drawer for the sachet so he or she can enjoy a lovely burst of scent while getting dressed.
Seniors with dementia can even participate in the main Easter event by stuffing and hiding the eggs. Set out plastic eggs and trinkets, and let your loved one stuff them. Help him or her hide the eggs before the hunt, and keep track of the number of eggs you lay out. Your senior loved one is likely to get a thrill out of watching younger family members searching for the hidden eggs.
Involving your loved one in these activities can enhance his or her physical and emotional wellbeing. However, sometimes family caregivers find it challenging to support their loved ones and involve them in family events, because of other pressing commitments. Caring for a senior loved one can be overwhelming at times, which puts family caregivers at risk for burnout. However, professional senior living and memory care services will empower you to focus not only on them, but to empower you to focus on your own health, maintain a full-time job, care for other needy members of your family, and a host of other reasons.
Thinking about loved ones and practicing writing can help bolster a senior’s memory. Set out different colored pieces of paper, markers, and spring-themed stickers, and encourage your loved one to get creative. Once the cards are made, help your loved one mail them to the recipients. He or she can also deliver the cards by hand at an Easter family event. Either way, your loved one may feel a sense of purpose by bringing joy to someone else this spring season.
If you are the primary assisted living or memory care service provider and need ideas and assistance of any kind, know that we’re here for you. Contact us anytime!
21 March 2022

Spring is in the air! Staff and cherished residents alike here at Winder's Gateway Gardens Assisted Living and Memory Care are taking moments to smell the roses. Well, roses aren’t in bloom just yet, but you get our drift. Whether your loved one resides within our senior assisted living community or our memory care community, it’s time to think about engaging with your loved one in some form of healthy and fun outdoor activity. We have some ideas for you that fit perfectly with what we try to accomplish here in our senior living and memory care blog. Of course, that is to promote a celebratory quality of life.
These recommendations of course go out to you at-home care givers because few, if anyone, understand and appreciate your labor of love and commitment to our cherished seniors out there across the country. So here goes.
Gardening: Spending time in the garden is an excellent physical exercise and many people find it relaxing and fulfilling. Gardening is a great way to spend time in the natural light, fresh air, and greenery. In addition, recent studies have uncovered the many benefits of getting your hands dirty. According to J E Public Health, “Earthing (or grounding) refers to the discovery of benefits—including better sleep and reduced pain—from walking barefoot [or having your hands in the dirt] outside.”
Walking: Some light walking in the evening or early morning can be refreshing. Walking also keeps the body fit and active in older adults. A leisurely stroll after dinner can help keep your digestive system running smoothly, too. Doctors are quick to recommend walking as an outdoor activity to many seniors because of the many benefits.
Golfing: Now, we’re not necessarily recommending buying new clubs for your senior loved one, but if you golf, consider having senior ride along with you out on the course. The game is played in a beautiful setting with abundant fresh air. Riding along while you and your friends play golf will provide both physical and mental health benefits.
Fishing: This kind of goes along with the notion of “playing” golf as described above. You don’t need to put your Mom or Dad in an off-shore fighting chair, but how about a chair next to you and their grandchildren while you fish for a few perch or two.
Photography: Capturing beautiful photos of nature is a wonderful way to spend time outdoors. Photography can be a relaxing activity for seniors. It is a great way to get outside and enjoy natural sunlight and the serenity of nature. Photography can help you appreciate the smallest details of nature, too. It is said to stimulate the brain and improve cognitive and emotional health.
Picnic: Picnicking with your family or friends is a great way to spend time outdoors. A nice meal and lots of natural Vitamin D are both great health-boosters for people of all ages, but especially seniors. As a bonus, arrange for some games post-meal, such as horseshoes, cornhole, or croquet. And remember, you don’t have to set the playing field up at regulation. Shorten the field for them.
Oh, and while you do these things, don’t forget to smell the roses! And never forget, here at Gateway Gardens Assisted Living & Memory Care, we deliver senior assisted living and memory care services in a loving environment as if you all are our own biological family.
14 March 2022

Have you ever “drawn a blank” trying to figure out something fun to do while visiting your loved one within our Senior Assisted Living community here in Winder or within our Memory Care Community also in Winder? Well, rest assured you are not alone.
We all tend to over-complicate things when it comes to spending time with our senior loved ones. They really don’t have high expectations. The fact that you are there for them sends all the message they need. But understanding full well that you’ll still struggle to come up with a new activity, we’ll just throw something as food for thought. Bookmark this website: NationalDayCalendar.com
How easy might it be to simply go there and choose any one from the long list of “National Days”. You don’t have to match the exact National Day event to the calendar day of your visit. Use it to simply give you ideas. For instance, the 15th is “National Pears Helene Day”. Huh? Well, when you and your loved one discover this is the day to combine warm poached pears, vanilla ice cream, and chocolate sauce, you both have something to look forward to. March 19 is “National Certified Nurses Day”, so why not discuss with your loved one how to express your appreciation for the dedicated Manor Lake Assisted Living & Memory Care staff who provide loving support each and every day. Why not add your own personal touch to the day by extending appreciation to every member of the staff, not just those with “RN” on their name tag. There’s a lot of love doled out by the cleaning staff, the culinary staff, maintenance staff, drivers, administrators, and every contributor not mentioned there.
Happy “Whatever day it is today” day! And enjoy your day with your loved ones as we do every day here at Gateway Gardens Assisted Living & Memory Care!
7 March 2022

Getting the news that your parent, in-law, or spouse has dementia is devastating. There’s no other way to put it. Hopefully this is the most sobering challenge of your lifetime. Here at Gateway Gardens Assisted Living and Memory Care here in Winder, we will be honored to help you every step along the way. Whether that help to you is direct in the form of you and your loved one joining our memory care community or by simply offering free education via this memory care blog, rest assured our hearts go out to you because very few can directly relate to what you are going through.
So, take one long and deep breath and make a commitment to yourself that you are going to remain calm and that you are going to get educated on the subject of memory care to the absolute best of your ability. For some of you reading this, that first deep breath comes now!
First of all, what are your parent’s or relative’s daily needs? If your loved one needs help with activities of daily living (ADL) then you’ll need to find a facility that helps with bathing, dressing, and eating. If this is the case, then you’ll want to talk with memory care communities across your area. Why do we recommend this? First, because you are researching one of the most meaningful investments of your life, that being entrusting others to full-time care of your loved one. Second, we are certain that the more you know about others, the more you will come to appreciate Gateway Gardens Assisted Living & Memory Care as your future care giver of choice.
Here are some questions to consider that will help determine the level of care your relative needs:
Sometimes seniors diagnosed with dementia can get angry, resist care or display other signs of aggression or distress. You’ll want to ask the memory care communities under consideration how their staff reacts when residents with dementia occasionally get angry, resist care or show other signs of aggression or distress. You’ll want a closer look at memory care communities that say their team redirects residents who show signs of anger or distress. It’s important to find out the staff’s reactions to your relative’s anger or distress. Are they caring and considerate or are they numb or bothered? It’s also key to know whether staff seems interested in getting to know your relative. Do they seem genuinely attentive and sincere? Or are they treating your relative like a number or like he or she doesn’t matter? The type of staff you want around your loved one are those that are pleasant, well-trained, involved and understand that your relative is more than their condition or disease.
You’ll want to look for an easy-to-navigate but spacious facility that boasts plenty of common areas, 24×7 care team support, eye-catching courtyards, activity rooms, stunning private suites, attractive semi-private suites, and a gourmet meal plan with snacks in between. Ask about daily activities as there should be a mix of activities, therapeutic sessions that encourage movement, socialization, and healthy behaviors. There’s no doubt you’ll want vibrant memory care home where your loved one will thrive. You’ll want to see a state-of-the-art facility that’s in a league of its own. At Gateway Gardens Assisted Living & Memory Care, we offer premier home environment care in a loving family atmosphere for your loved one. We facilitate the ability of your loved one to continue living with dignity, respect, freedom, and choice. Our home environment enables seniors with Alzheimer’s, Dementia, and other memory impairments to maintain the highest quality of life while providing peace of mind to their family and friends.
28 February 2022

We realize that the high percentage of our Gateway Gardens Assisted Living & Memory Care blog know that we invest time and energy as a service to our community. We understand that all of you providing at-home senior assisted living care and/or memory care services to your loved one is a labor of love that most simply can’t begin to understand. To ease your burden in any way refreshes us in knowing that our seniors, the ones who’ve provided for us all through the years, enjoy loving reward for all that they have done.
Today we’re going to focus on just some very simple support tips that we trust will enrich both you and the loved ones that you care for.
According to the United States Census Bureau, seniors are on track to outnumber children for the first time in U.S. history in coming years. As the country’s older population continues to increase in number, the generation coming behind them—their adult children—are often taking on a role as supporter and caregiver.
As your loved one ages, he or she may not always let you know when help is needed. That’s why it’s important to pay attention to signs that his or her level of independence isn’t what it used to be––such as problems completing daily tasks, bills piling up, or changes in behavior.
While at times it can be difficult to know how to best support your aging parent, the good news is there are more resources and care options available than ever before, like us here at Gateway Gardens Assisted Living and Memory Care here in Winder. Use these four tips to make sure you’re ready to provide your loved one with the support he or she needs.
According to a study by Merrill Lynch and Age Wave, nearly three out of four adult children have not had a detailed conversation with their aging parent about long-term care, living arrangements, or net worth. However, these discussions are invaluable to helping you support your loved one. Find a time to sit down with your parent and siblings so that you’re all on the same page about future needs. By getting everyone involved, it will make transitions smoother when additional long-term care is needed.
As your parent ages, it’s important for you to be an advocate for his or her health. Support your loved one by keeping up with health conditions, doctor’s appointments, medications, and changes in behavior. Communicate often with family members or others who know your parent well to take note of his or her overall well-being. Be sure your parent has completed a Living Will, Power of Attorney, and Health Care Power of Attorney so there is a clear designee if your loved one becomes unable to make decisions due to dementia, behavioral conditions, or other medical concerns.
Finances are often one of the most difficult topics for adult children to discuss with an aging parent. However, it’s essential to have a full financial picture before making any long-term care decisions. Initially, the only support needed may be smaller tasks like helping make sure the bills are paid on time, reviewing accounts, or going to a meeting with a financial planner. By addressing finances early, you’ll be prepared to support your loved one later and make care decisions that fit his or her financial situation.
Sometimes supporting your aging parent is as simple as routinely asking how you can help. If you notice your parent has been complaining about a new ache or pain, ask if you can help by taking your loved one to his or her next doctor’s appointment. If your parent is considering an assisted living community, ask if you can help by going along on a tour. If he or she has questions about a financial question, ask if you can help find the answer. By tackling concerns together, you’ll continue to foster a relationship based on open communication and support.
Gateway Gardens Assisted Living & Memory Care here in Winder offers a wide range of care options that can help alleviate some of the stress, anxiety, and fatigue that come with caregiving on one’s own. We understand that taking care of aging loved ones can progress from slightly challenging to completely overwhelming in a matter of days, but we are here to support your family every step of the way. We offer senior assisted living and professional memory care services here in Winder and we will work with you to determine what is right for you and your loved ones.
21 February 2022
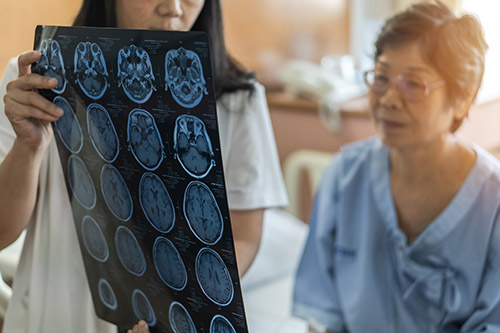
As promised, today we follow last week’s blog post with some guidance for those of you who feel some form of formal cognitive evaluation is required for you or a family member. But first, once again warm winter greetings to you, our faithful assisted living and memory care blog readers, cherished assisted living residents, memory care residents, family members. And for the record, we send a special shout-out to all of you angels out there providing at-home care to a senior loved one in need.
The diagnosis of Alzheimer’s can be done through an entire set of tools that are specifically designed to determine and detect dementia and to figure out whether the cause of it is Alzheimer’s or not.
To start with, it is highly essential to self-assess the symptoms first hand while encountering this disease. These assessments can be specifically noted as well as reported by a close family member as well who deals with the patient daily.
A person can easily perform the basic physical tests at home to see whether the response of their mind towards different tasks is effective or not. Apart from this, there are many tests that doctors opt for to know the exact root of the cause of these signs and symptoms of Alzheimer’s.
If the patient visits a doctor who suspects him/her to have Alzheimer’s disease, the doctor may refer the patient to Geriatricians, Geriatric Psychiatrists, or Neuropsychologists that will further the examination. That likely will include:
Physical Testing
During this testing, the doctor examines your reflexes, coordination between the patient’s mind and body, hearing and sight senses, ability to do simple tasks as walking or reading, and many more. This is the first stage of testing and is generally the foundation of further complex tests.
Neuropsychological Testing
This is where the doctor will assess the patient’s memory and other mental functions. During this test, the doctor can figure out timelines at which the symptoms may progress in the future. These tests provide additional details of the functioning and processing of your brain activities.
Brain imaging
This can be done with the help of MRI scans i.e. magnetic resonance imaging that uses radio waves and magnetic field to produce images of the brain. This method is effectively used to monitor brain shrinkage and to rule out other possibilities. Another way of brain imaging is through a Computerized Tomography or a CT Scan, that uses X-Ray technology to find tumors or any head injuries in the brains.
Of course, if you have questions don’t wait a single moment. Know that the caring professionals at Gateway Gardens Assisted Living and Memory Care here in Winder are ready to address any need or concern.
14 February 2022

Warm winter greetings to you, our faithful assisted living and memory care blog readers, cherished assisted living residents, memory care residents, family members, and a special shout-out to all of you angels out there providing at-home care to a senior loved one in need.
A funny thing happened at a memory care resident’s family home while having dinner with their dear friends. They entertain this couple often for dinner and consider them best friends. While telling a story about a funny moment the four of them had in the past, this family member drew a blank and momentarily forgot their dear friends’s first name. “And that’s when, ugh, you know…what’s your name again?” of course drew chuckles from all and the story went on.
The point here is that a perfectly healthy brain routinely hits speed bumps along the way. The fact that this person in the emotion of the moment forgot a dear friends name is nothing other than a source for laughter and some future good-natured ribbing. That is unless it’s not. Which brings us to the purpose of today’s blog. What exactly are the signs that one might be transitioning into some stage of significant cognitive decline? Today we answer that.
During the early Alzheimer’s disease stages, the patient might experience very mild symptoms broadening it to general forgetfulness. These signs and symptoms of Alzheimer’s may include planning troubles, forgetting the placement of daily use items, problems in managing financial decisions, troubles in performing tasks at work, and inability to recollect as well as judge places and distances. The time span of this stage is between 2 years to 4 years.
Before Alzheimer’s disease symptoms appear, there are changes in the brain related to Alzheimer which are noticeable. This begins 10-15 years before the onset of Alzheimer which is referred to the pre-clinical Alzheimer disease. It is important to notice any minor signs of forgetfulness.
During this stage, the patient’s condition might start looking a bit more prominent such as the patient can experience forgetfulness of personal past, unable to remember the address or phone number, personality changes and might not even be able to recall the day it is. The duration of this stage can be anywhere between 2 years to 10 years.
A person’s routine is disrupted, and they are unable to do simple tasks on their own and require assistance. This stage can last many years and goes beyond memory loss and affects the cognition outside the memory including language and calculations. This makes it more problematic to complete daily tasks. This stage would also include them forgetting minute details of who they are married to and who their family members are.
The memory from the distant past tends to be better than recent memory of day-to-day tasks, whom they met and what they spoke about. They could experience restlessness and experience changes in sleeping patterns including sleeping during the day and staying awake at night. They might experience personality changes and act suspicious or feel lost in gatherings amongst familiar people. Read on to know more about Everything You Need to Know about Alzheimer's Disease.
During this stage, the symptoms are regular and highly significant. The Alzheimer’s symptoms during this stage include apparent and sudden behavior changes, inability to carry a conversation, eating and swallowing can be difficult, inability to control the bladder, Vulnerability to infections, difficulties in sitting, walking as well as swallowing.
The increased dependence on people starts at this stage where performing day to day tasks is an issue, but they forget people who are important to them. they might not know what to do when the doorbell rings, when the phone rings or if there is a fire and a fire alarm goes off.
Leaving them alone becomes dangerous and it is best they have assistance as they are communicating but not in a specific context to have a conversation or are unable to communicate what they are experiencing. The brain cells deteriorate considerably, and motor skills are not properly functional.
So, there you have it. This should put that story-telling family member’s mind at ease because occasional forgetfulness is a common human trait and most often not associated with cognitive decline. But if anything in this blog post raises more questions than answers, stay tuned for next week’s blog post where we’ll talk about diagnosing Alzheimer’s and other forms of dementia. Of course, if you have questions don’t wait a single moment. Know that the caring professionals at Gateway Gardens Assisted Living and Memory Care here in Winder are ready to address any need or concern.
7 February 2022

The therapeutic nature of music is something for all of us to consider. Today’s blog post will primarily focus on the therapeutic effect that music can offer your loved one living here in our senior assisted living community or our memory care community. We’ll touch on the scientific evidence of this in a moment, but first a practical testimony from the laymen’s perspective.
We were talking with a resident’s daughter this morning who shared the story about how her son hosted a couple of his college buddies at her house over the weekend. She loves the boys and lovingly welcomes them repeatedly to stay at her house. But their college kids. Loud, fast, funny, and stay up way too late. She loves them and their youthful energy. She does not drink alcohol, but she envisions how she feels this morning to that of a hangover after a long weekend of partying. Her remedy you ask? She reprograms “Alexa” away from the rock and roll channel of the past few days and asks her to play “soft classical”. She sits and listens with eyes closed and decompresses. Better than aspirin she says.
So now we transition away from simple feelings about the benefits of music to the science of it all. We covered this story of scientific research regarding music but feel it is more than worthy of a revisit. Modern researchers have discovered that music soothes those suffering from dementia, and/or Alzheimer’s disease. Researchers at The University of Utah Health recently tested whether they could alleviate anxiety in seniors suffering from dementia by playing familiar music to them using headphones and a hand-held music device. Anxiety and agitation are two of the most disruptive aspects of living with dementia and Alzheimer’s disease for both patients and caregivers.
After the researchers helped the patients pick meaningful music, they used a functional MRI to record the changes in the brain while the music played. The brain images showed that music helped the areas of the brain known as the salience network, the visual network, the executive network, and the cerebellar and corticocerebellar networks all work with better connectivity. These areas of the brain activate language and memory, according to the study’s authors.
“When you put headphones on dementia patients and play familiar music, they come alive,” Jace King, lead author of the study, said in a press release. “Music is like an anchor grounding the patient back in reality.”
Music and movement are the last things to go in the brain.
It’s almost miraculous what music can do for Alzheimer’s patients and the research about the benefits is there.
Patients Respond
Health care providers have seen firsthand how much music helps dementia patients. with the clients there.
Play songs from their era that they might recognize. Patriotic songs are also popular.
Music touches people on so many levels.
The reaction by dementia patients to music was also dramatically demonstrated in the 2014 documentary, Alive Inside. Elderly care professionals can set up personalized playlists on iPods for their patients. The music helps the patients access the deep memories not lost to dementia. It also helps them converse and socialize in ways they weren’t doing before the familiar music became a part of their daily life.
For more information on professional senior assisted living services or memory care services here in Winder, contact us here at Gateway Gardens Assisted Living and Memory Care .
24 January 2022

Greetings once again to all of our Winder-area assisted living and our Winder memory care community residents, family, neighbors, and friends. Today we’re going to share with you today some insights into an increasingly popular concept called “Self-Care”. This topic can benefit everyone whether you are a member of our staff, a cherished member of our assisted living or memory care community, or if you are an independent living senior or an at-home senior care provider. The benefits associated with focusing on your physical, mental, and emotional well-being each day are numerous. Better overall health, improved mood, and reduced stress have all been linked to a consistent self-care routine. Taking care of yourself is important for everyone, and it doesn’t need to be complicated or expensive. Read on to learn more, including how you can start a self-care routine today.
Before we dive into learning more about self-care and how you can create your own routine, it is important to take a step back and address why you should. As the pace of life continues to accelerate, with increasing demands being made on your time, it feels selfish to set aside "me" time. However, if you are a primary caregiver – a parent, healthcare worker, first responder, or someone who cares for an elderly loved one – self-care is a must. Simply put, you cannot care for others without seeing to your own needs first. Developing a routine that addresses your physical, mental and emotional health, and leaves you feeling refreshed and recharged, will better prepare you to focus on the needs of others. For more information on the importance of self-care check out the Harvard Health Blog.
Self-care is any activity that impacts your physical, mental or emotional health in a positive way. Since we are all unique, the possibilities are endless – so don’t be afraid to experiment until you find what works best for you. Once you do, try your best to be consistent. The benefits of self-care only happen when it is done regularly – either daily, weekly, or monthly. Following are some suggestions for activities that can help improve your physical, mental, and emotional well-being.
Physical Self-Care
Self-care that focuses on your physical health doesn’t have to involve kale or extended sweat sessions at the gym – unless you want it to. Following are some simple activities that you can include in your self-care regimen. The key is to find an activity that you love and will want to do on a regular basis.
Mental Self-Care
A glance at the evening news, or your smart phone’s calendar, will confirm there is no shortage of stressors in today’s world. Self-care strategies that promote relaxation and a calm mind are a great way to improve your mental health. Try adding one of these activities to your self-care routine:
Emotional Self-Care
In an article for Psychology Today, psychiatrist Abigail Brenner, M.D. describes the importance of emotional self-care. “Mastering your emotions is not only your personal responsibility but also is a positive strategy for getting through life in the best possible way you can. When you have a healthy attitude about your feelings and how to express them, you are better equipped to get through events well, rather than feeling each time strong emotion hits that you are overwhelmed and incapable of handling the situation.” Strategies for emotional self-care can include learning to set boundaries or forming a strong support network. Following are some simple ways to begin:
Finding a self-care routine that works best for you requires some work, but the long-term benefits are worth the effort involved. Focus on finding what works best for you and being consistent, so you can offer the best version of yourself to your loved ones!
Gateway Gardens Assisted Living & Memory Care here in Winder offers a wide range of care options that can support self-care program initiation and sustainment. We understand that taking care of aging loved ones can progress from slightly challenging to completely overwhelming in a matter of days, but we are here to support your family every step of the way and that includes us helping you take care of yourself at home. We offer senior assisted living and professional memory care services here in Winder and we will work with you to determine what is right for you and your loved ones.
17 January 2022

It comes as no surprise to us that our most frequently asked question from those researching professional assisted living options here in Winder is, “What Exactly is Assisted Living”. The reason is simple this question is asked so often. It is because assisted living has no single definition. It differs from community to community, state to state, family to family. So today, we’re going to share with you the way we answer this frequently asked question.
Here’s how we define it. Assisted living is “a combining of housing, personalized supportive services and health care designed to meet the individual needs of persons who need help with the activities of daily living, but do not need the skilled medical care provided in a nursing home.”
This level of care can cover a wide variety of resident needs, including dressing, bathing, using the bathroom, eating, mobility, and getting in and out of bed. While assisted living is a healthcare-type environment, assisted living is different than a nursing home. Typical assisted living residents are able to live independently for some or most daily activities, and simply require help for certain non-medical issues.
Assisted living communities go by many names, including adult congregate living facilities, rest homes, homes for the aging, personal care homes, residential care, retirement homes, retirement communities, adult foster care, and community residences, but they all point to the same type of care provided.
Those residents who require more intensive care or medical supervision (such as our dear residents within our memory care community) are typically not residents of assisted living facilities, but rather find better-suited care in a nursing home or more medically oriented facility.
Choosing an assisted living community for your loved one is never an easy choice, and you should be very comfortable with the level of care provided by the community. At the very least, assisted living facilities should offer the following services:
Assisted living is meant to provide your loved one with the care they need to live happy and healthy in a supportive environment. If you have any questions about the services we provide here at Winder's Gateway Gardens Assisted Living and Memory Care, please do not hesitate to contact us. We will be happy to answer your questions and give you a tour of our community.
10 January 2022

First and foremost, stop and realize that you are not alone and that you are loved. Consider all of us here at Winder's Gateway Gardens Assisted Living & Memory Care to be a ready, empathetic, loving, and professionally experienced resource for you.
Being diagnosed with Alzheimer’s, no doubt, is a life changing event. For many, it will seem like the end of the world. However, rest assured that is it not. So where are you and where are you going?
You understand something is not quite right. You’ve known for a while because you recognized the gaps in memory. You struggled to remember conversations you just had. People reminded you of things they told you only previously that day, and sometimes you couldn’t put a name to the face, even for a close family member or friend you’ve known most of your life. You see your doctor and she confirms your suspicions. Make no mistake, your doctor should be considered one of your most trusted advisor. Consider your family caregivers and/or special friend(s) right up there as well.
Alzheimer’s is a frightening diagnosis. When you or somebody you love has been diagnosed with this form of dementia, it’s important to not get caught up in what you are still capable of doing right now and ignoring what the future may hold.
You might not want to think about assisted living at this moment, but it is a topic to discuss as early as you can. Keep in mind, though, that whether this is you, a spouse, a parent, or somebody else you love who has been diagnosed with Alzheimer’s, it might take a while for them or you to absorb this new diagnosis.
Even though you may have realized something wasn’t quite right and worried that could be Alzheimer’s or something similar, receiving that formal diagnosis can be a shock to your life. Now what?
Don’t rush them through the process. Everyone goes through different stages of grief at different times. When you realize what the future will hold and that there is no cure for Alzheimer’s at this moment, it can feel like a loss already.
Yet, it doesn’t have to be a loss. Not for a long, long time still to come.
This should include memory care assisted living. When an elderly person who has been diagnosed with Alzheimer’s or another form of dementia looks into memory care assisted living communities like ours, they’re looking into adequate support in the years ahead.
Their spouse, their adult children, their friends, their neighbors, and others might be more than willing to support them so they can remain home, but as the disease progresses it will steal more memory, more mental function, and eventually cause more health issues and limited mobility.
This will place a tremendous amount of pressure on that caregiver support system at home. Plus, a lot of things can and often are missed when people have no prior experience supporting an elderly person through the different stages of Alzheimer’s.
A memory care assisted living facility — will have properly trained and experienced staff ready to support you or that person you love through the advancing stages of Alzheimer’s. They can offer comfort, be the buffer between the memory loss and family members who can get caught up in the verbal or even physical outbursts from the individual. They will understand what comes next, how to remain calm and rational, and how to best support that elderly person as they face this long and difficult road ahead.
If you or an aging loved-one is considering a move to a memory care community in and around Winder, Georgia, please contact our caring staff today!
3 January 2022

New Year’s Greetings from all of us here at Winder's Gateway Gardens Assisted Living and Memory Care! We are now a couple of days into the calendar year 2022. Many of us authored our traditional “New Year’s Resolutions” and are working through the details of strategic self-improvement. But if you provide daily assistance to a senior loved one, then we warmly suggest that you include delivering “improved health” to your senior loved one.
Like so many of you loving family members out there caring for a loved one, you might assume that professional assisted living is a last resort for an aging loved one. But is that really the case? Many people simply have the wrong idea about what assisted living is and what it offers.
It’s easy to overlook just how beneficial assisted living can be, but the more you investigate a quality assisted living community, you will start to understand why seniors tend to actually be healthier (mentally and physically) at assisted living.
We outline just a few of the reasons why this could very well be the case, and why you should sit down and discuss the professional senior assisted living option with an aging parent or other loved one.
In life, that is. Being withdrawn, wanting to give up, or hiding out in your room isn’t going to offer a great emotional benefit. But having friends, staff, and others enticing you to get out and connect on a personal level and taking part in various entertainment options or activities is a wonderful way to help someone stay (and feel) more connected. That connection taps into our nature, our human nature. We were designed to be with others and when we have that engagement with others, it can lift us up emotionally, which has a direct impact on our physical wellness, too.
Not all assisted living communities are the same, so it’s important not to conflate one with others. The average assisted living community will have decent dining options for elderly residents, but here at Manor Lake we offer an outstanding (even celebrated) dining experience!
This is directly linked to high quality healthy food choices which tends to improve overall health. While a senior may not eat healthy at home, especially when living alone, we ensure that they enjoy healthy meals for breakfast, lunch, and dinner.
Again, not all assisted living communities offer the same benefits, but there is somewhere safe that elderly residents can get some much-needed exercise. Just walking down a broad corridor with hand rails or strolling along carefully manicured and maintained grounds can offer wonderful exercise options.
In short, professional assisted living offers many options that can help seniors be healthier, but you and they must take that first step and look into it for yourselves. Contact us here at Winder's Gateway Gardens Assisted Living and Memory Care to learn more.
13 December 2021

In the past year, Americans across the nation experienced toilet paper, food, hand sanitizer, and paper towel shortages. Some industries were put at extraordinary risk due to short supply of vital staples. The Assisted Living and Memory Care support providers were arguable at the top of the list for the supply shortages. But our stubbornly dedicated staff here at Gateway Gardens Assisted Living and Memory Care here in Winder went above and beyond to prioritize and deliver the level of comfort and safety that our beloved community members deserve.
It was humbling to see the entire staff work steadfast to keep morale high when some residents were feeling isolated from their family and loved ones. We’d like to thank and congratulate our entire heroic team as 2020 revealed far more triumphs than struggles. From creative ideas for programs that kept our resident family socially engaged to our COVID-19 testing protocols and safety strategies, the team deserves a standing ovation for their incredible work over the past year.
Throughout the year, Gateway Gardens kept both our Assisted Living activity calendar and our Memory Care activity calendar filled with safe and fun activities that kept our community engaged and content through the difficult (and sometimes isolated) times. They were quick on their feet when it came to implementing the latest safety guidance. They were always one step ahead and making sure the community didn’t run out of critical supplies like masks, toilet paper, and other hard-to-find PPE and supplies. We implemented rigorous testing strategies and screening questions for the team and community that helped keep the virus in check within our walls.
Our amazing team did all of this with a smile while remaining calm, cool, and collected.
Along with the rest of the world, we became familiar with video conferencing technology. Our activities team was quick to get residents set up to engage with their families and loved ones when visits became impossible to arrange. Additionally, the team kept residents active with fun indoor games and fitness activities.
As the COVID-19 vaccine became available, our team rolled up their sleeves to make our first clinic happen as quickly and seamlessly as possible. Our resident family and team received their first round in January and the second set in February. We are so grateful to have had the opportunity to add an extra layer of protection for our community and we are hopeful for the future!
As busy as we were here in 2021, we’ve already rolled up our sleeves in anticipation of 2022 and the privilege of finding new and creative ways to deliver a genuine and ever-improving quality of life experience here at Gateway Gardens. Our warmest Holiday greetings to you all!
6 December 2021

This post cites Alzheimer’s research that publishes some very uplifting findings! Whether you are a beloved senior assisted living resident here at Gateway Gardens (Winder), a loving family member of a memory care service resident, or an at home care provider, the subject of dementia touches almost all of us in some form or fashion. It is our pleasure to bring positive news on the subject as often as we can. Today is one of those days!
Researchers at the University of California have discovered a very strong link to exercise as having a direct effect upon thwarting Alzheimer’s. Here’s the link to the entire story. The UC researchers conclude that exercise positively effects a process called “autophagy”. Autophagy is the body’s process of clearing spent or defective proteins from cells. Defective proteins have long been known contributors to dementia.
This is just one reason why we place such a high emphasis on exercise and active lifestyles here at Winder's Gateway Gardens Assisted Living and Memory Care. We invite you all to come see it for yourself!
29 November 2021

Very warm Christmas season’s greetings from all of us at Gateway Gardens Assisted Living & Memory Care here in Winder. We fully realize that life’s conflicts get in the way of being with family over the Holidays. For all of you with family members serving our country overseas and unable to return home, our most sincere thanks for your sacrifice. So today, we offer a few ideas for celebrating remotely with your loved ones here at Manor Lake.
Sharing laughter, joy, and praise is what the holidays are all about. There are lots of ways to reach out and include your loved ones in the celebration. Here at Gateway Gardens Assisted Living & Memory Care we celebrate every person’s unique traits and help them maintain as much independence as possible. Have a warm and blessed Holiday season!
22 November 2021

Very warm Thanksgiving greetings from all of us at Gateway Gardens Assisted Living & Memory Care here in Winder. As business owners, clients, prospective clients, friends and family, and suppliers our sense of appreciation for all of you has never been higher.
Like us, each of you have had unique and serious challenges during the last couple of years, most likely both professionally and personally. We are reflecting upon these challenging times with a “glass half-full” perspective and we hope that you all are doing the same. Each and every one of you has delivered a positive and enduring effect on us and our business as well as on those around you. We hope that in some way we’ve done the same for you.
Wishing you sincere peace and joy this Thanksgiving holiday. While surrounded by family and friends, we take time for positive reflection upon all of life’s blessings, we hope that you do as well.
Happy Thanksgiving from everyone here at Gateway Gardens.
15 November 2021

Today’s blog post is targeted for our entire blog reading community. Whether you are a beloved senior assisted living resident here at Gateway Gardens, a loving family member of a memory care service resident, or one of the many providing loving care of a senior loved one within your own home, we hope you take this advice to heart. Simply give the gift of focused time this Holiday season to your senior loved one(s).
Backed-up ports and the corresponding lack of goods going through the supply chain could become a real-life "Grinch," making for a disappointing Christmas holiday for millions. Hundreds of huge cargo ships, stacked high with thousands of containers filled with clothing, electronics, toys and staple goods, are circling U.S. ports on both coasts with no slip to dock and unload. The massive gridlock is delaying what is usually at this point in the year a cresting apex for stocking store shelves for the holiday season, a make-or-break time of year for many retailers.
Consider telling your loved ones today, that you simply don’t expect them to stress out trying to find you Holiday gifts. Tell them that your plan, this year, with all things considered, you’re going to replace wrapped gifts for hours and minutes of loving fellowship. So many of you are going to (or already have) order that perfect gift that will not be delivered on time and thus adding to Holiday stress.
Sure, find some simple things commonly found at your local store to wrap and deliver, but communicate to your senior loved one that you look to take an overnight trip somewhere with them or even that you plan to take a simple drive around town. It’s a plan that will surely pay emotional dividends.
As always, if you have any questions regarding professional senior assisted living or memory care services, contact us anytime.
1 November 2021

Today’s blog post is authored for all of you at-home care providers providing your loved one with senior assisted living or memory care services. This is our way of giving back to the community so that your beloved senior has the best chance of living a safe and happy life.
Home is meant to be a space where we’re at our most comfortable. There’s a lot that goes into making a comfy home: the right amount of room to move around, decor that reflects your personality, and of course, a space that’s safe and secure. For seniors, safety in the home should be a priority, especially because reports have shown that at-home accidents are among the leading causes of fatalities in the U.S.— and that number only increases with age. Luckily, there are some simple tips that can make a space more senior-safe and friendly. Find some of the best ones and make sure safety is always a priority in your home.
Falls are the most common accidents for seniors at home. No one can predict when they’re going to have a dizzy spell, but making sure your home is clear of clutter, stray cords and debris is a great place to start when trying to prevent an accidental fall. Look out for rugs with rubberized backing to help avoid tripping up, wear non-slip footwear and make sure all entryways and high-traffic walkways are completely clear. And make sure you’re familiar with tips for falling more safely.
Whether you like to hold onto things or prefer a minimalist space, how you store things can make a world of difference. Items that get daily use should be in an easy-to-access area that doesn’t require uncomfortable lifting or bending. Try to give them designated spaces so you don’t have to tumble around looking for things that you might need on the spot. It’s also wise to have a special spot for important documents, IDs and health records.
The most common place for senior accidents in the home is the bathroom. From slipping in the tub to getting burned by hot water, a lot can go wrong in a bathroom. Installing grab bars near the toilet and shower, placing rubber mats in the tub, even including a bathing chair for seated showers can help prevent accidents. A toilet seat with handlebars can also make sitting and standing much easier.
A poorly lit space can make accidents more likely, especially for seniors who have a habit of waking in the night to use the bathroom or get a glass of water. Motion-detection lighting or automatic night-lights in the hallway help with nighttime light. In the daytime, incandescent light bulbs are helpful to create a bright space. Having a reading lamp or other lamps near commonly used spaces can help, too.
Candles can create a nice ambience at home, but it can be easy to forget when you have one lit. Opt for flameless battery candles to achieve the same atmosphere without the fire hazard. For electronics, keep all areas near outlets and cords clutter-free and limit the number or cords plugged into power strips. Make sure smoke and carbon monoxide detectors are always working and replace batteries in a timely manner. During colder months, avoid the use of space heaters and heated blankets, as they’re easy to forget about and can be a fire hazard. If you have to use a space heater, keep them far away from curtains, blankets and bedding.
Thanks for reading, and as always, if you have any questions, contact us anytime.
25 October 2021

Sometimes the most beautiful moments with your senior loved one starts right outside your front door and in your driveway. Whether you are an at-home care provider or currently trust us with your senior assisted living or memory care services, consider going for a therapeutic drive with the ones you love and care for!
You may not know this, but according to Travel and Leisure, several of the top 15 most beautiful fall drives are very close by in North Carolina, Virginia, and Tennessee! According to Travel and Leisure, the colors are in full swing by mid-October on the East coast. So, head on out!
Just for your information, here are 15 must-see places to drive through this fall:
So, what if getting out for a ride is simply not practical or possible. Consider taking a virtual tour of these great places on the internet. Either way, take some pictures of the quality time spent together and consider sharing your stories with us. Enjoy your trip and as always, if you have any questions, contact us anytime.
18 October 2021

By now, most of you know that we manage our Gateway Gardens Assisted Living & Memory Care blog for the benefit of all of you at home in the Winder area caring for your loved one with senior assisted living needs and/or memory care challenges. We do this because you are neighbors and friends, but most importantly, because we view you as heroes. As professional care givers, we know the challenges that you face. And we want to do our part to help. Today we’re going to focus on the very real challenge of pandemic-related caregiver fatigue.
Caring for our loved ones as they age is never easy. There are tons of factors that can make it taxing physically, mentally, financially, and more for both the caregiver and the one receiving care. This has always been the case, but with the emergence of COVID-19, things have only gotten more difficult. Many of us, especially caregivers for older adults, are feeling a real sense of burnout due to Coronavirus, also referred to as pandemic fatigue. Today we will be covering pandemic fatigue in more detail, recommending coping strategies, and discussing care options.
When we began seeing increased COVID-19 rates in the United States, many people stayed home as much as possible to slow the spread and protect those they live with, especially those in vulnerable populations like older adults. Seven months later, it often feels less urgent to stay home, despite higher rates of COVID-19 than ever in the U.S. People are coping with the loss of their loved ones, jobs, or housing, and many live in a constant state of anxiety about getting sick. One group of people that are hit especially hard by Coronavirus spikes are caregivers of older adults, as they risk their lives, and the lives of their aging loved ones, every time they have to leave the home while COVID-19 rages on. Many of these caregivers still have to go to work to support their own kids, and relief has been hard to come by in recent months.
The combination of all of these fears, frustrations, and losses contribute to what we now refer to as pandemic fatigue. Pandemic fatigue can also be thought of as burnout from being pulled in all different directions while also feeling isolated from the outside world. Pandemic fatigue can put our mental and physical health at risk, affecting the quality of our work, caregiving, and lifestyle.
Fortunately, there are steps you can take to overcome pandemic fatigue, empowering you to stay as relaxed, calm, and collected as possible.
Stay Connected
Letter writing and virtual hangouts are ways to stay connected with loved ones.
One major reason why pandemic fatigue has grabbed a hold of so many of us is the lingering feeling of isolation and loneliness. We may not be able to host or attend gatherings like many of us used to, but that doesn’t mean we cannot stay connected with friends and family members.
Staying connected not only helps us preserve our mental health, talking to friends and family can help us express built up feelings and work through our struggles. Even if you don’t explicitly talk about your problems, feeling connected and supported is just as important too.
Try the following to get in touch with friends and family during the pandemic:
Take Care of Yourself
Maintain a balanced diet with plenty of fruits, vegetables, and whole grains.
When we put so much time and effort into taking care of others or simply trying to make ends meet, it can feel impossible to take care of ourselves and our needs, too. Setting aside just a few minutes of the day to dedicate to yourself can make a huge difference in your mental state. If you’re feeling burned out, it will only make it harder to provide quality care to your loved one or maintain a household.
Try incorporating more of the following to take care of yourself:
Most caregivers go through their entire days without rest or doing things they enjoy, and this can lead to burnout faster than anything else. Self-care can look a bit different for everyone but doing enough of it pays off when it comes to your physical and mental health, as well as your caregiving ability.
Get Help
Many are feeling stuck and overwhelmed to the point where they feel like they are drowning in their responsibilities as a caregiver, especially with pandemic fatigue thrown in the mix. If you feel this way, see if you can find a local or virtual support group or if you have access to counseling through your workplace or insurance.
Gateway Gardens Assisted Living & Memory Care here in Winder offers a wide range of care options that can help alleviate some of the stress, anxiety, and fatigue that come with caregiving on one’s own. We understand that taking care of aging loved ones can progress from slightly challenging to completely overwhelming in a matter of days, but we are here to support your family every step of the way. We offer senior assisted living and professional memory care services here in Winder and we will work with you to determine what is right for you and your loved ones.
Now may be the time to have that discussion. Contact us today.
11 October 2021

This blog post if for you angels out there taking care of a loved one at home suffering from Alzheimer’s. Although it’s a longstanding tradition here at Gateway Gardens Assisted Living & Memory Care here in Winder to celebrate Halloween with both our assisted living and our memory care residents, we celebrate a bit differently within our two unique care communities. The scary and ghoulish themes of Halloween can serve a detrimental effect on memory care patients. So we have some things for you to consider in advance of the upcoming holiday.
Halloween is one of the most celebrated days in the American calendar. It is a day rich in history that everyone should celebrate. For decades now, it’s been known to be a favorite day for the kids who would feel their pockets or even bags with candy, fully dressed in a ghoulish costume.
Halloween is characterized by scary costumes and decors which can greatly frighten individuals with Alzheimer’s. It is therefore important to organize Halloween parties that suite people with Alzheimer’s for them to feel loved an included. How can we organize Halloween for seniors? Here are few tips to make this Halloween happy and safe for everyone:
Halloween is all about decorations and costumes. Halloween wouldn’t be the same without them. But extreme decorations don’t go well with people who suffer from Alzheimer’s. Keep decorations to the minimum. Even though it may not guarantee that the patient will not get confused or stressed, maintaining the outlook of the house by decorating minimally celebrates the holiday without causing too much confusion or disorientation. In order to accomplish this, there are some things that one should do or avoid.
It’s always fun for kids to watch ghosts and goblins at the park during Halloween festival. The same cannot be said about people with Alzheimer’s. This might cause the patient to avoid the place again due to scary memories. The best thing is to take them to a less public and elaborate celebrations.
There is no Halloween without candy. In the culture of celebrating Halloween, most families, if not all share candy with other kids. It is therefore difficult to keep candy away. Nutritionally, sugary foods have been known to heighten the condition. Many patients won’t control themselves from taking candy. It is therefore important to monitor them or even keep the candy away in a safe place.
Although this may prove to be a hard option, it is important to try and explain to your loved one that there will be some commotion around. If you are someone who has stayed with the patient for long, you will have a good chance of getting them to understand. Even so, this won’t guarantee you success because patients with Alzheimer’s lose memory very quickly. Therefore, try to create distractions and carefully and patiently explain any questions that they may have.
Halloween can be a fun filled time for everyone. Just as we take safety measures to protect children during the holiday, we can provide the same precautions for our elderly and those who may suffer from memory conditions.
All of us here at Gateway Gardens Assisted Living & Memory Care wish you the very best for a joyful Halloween celebration.
4 October 2021

Our team of professional memory care and assisted living care providers here at Gateway Gardens Winder are there for all of you, young and seasoned alike. Today’s blog offers “food for thought” pertaining to senior nutrition. Your senior Mom or Dad’s dietary requirement is significantly different than your senior in high school. Across the nation, without even realizing it, well intentioned senior care givers are denying their senior loved one of a healthy diet. Add in the fact that as the coronavirus pandemic persists, researchers continue to say a weakened immune system can increase an older adult’s risk for the virus. A poor diet can often result in decreased immunity. In addition, there are other health issues linked to malnutrition:
Learning what puts older adults at risk for a poor diet or malnutrition will help you learn how to detect a problem and address it.
Research from the Mayo Clinic report that physical, social, and psychological factors contribute to poor dietary conditions within our senior community:
Once you pinpoint the cause of a senior loved one’s poor nutrition, it will be easier to address those concerns. Whether it is having groceries delivered or exploring meal delivery services, there are a variety of solutions to consider.
If you are considering a senior living community for yourself or a loved here in Winder, we invite you to come visit and see the thriving senior assisted living community here at Gateway Gardens Winder and/or our loving memory care community here in Winder as well!
27 September 2021
Greetings once again to all of our Winder-area assisted living and our Winder memory care community residents, family, neighbors, and friends. We had a family member call us and ask if we could repost our recommendations for preparing loved ones for the upcoming flu season. She asked us this because she believes there are instances within her caregiver circle of people forgetting about the very real threat that the flu presents to our senior loved ones. We share the same concern, so, here goes.
As people around the world continue focusing on the COVID-19 crisis, the time of year when the seasonal flu begins to make its rounds is approaching. It’s important not to overlook the safety measures designed to protect us all from the influenza virus. Compared to the severity of the coronavirus, the flu may not seem as serious of a health risk. The reality, however, is that the seasonal flu can still be deadly for seniors. In fact, seniors comprise nearly 85 percent of influenza-related deaths and up to 70 percent of hospitalizations in a typical year.
The annual flu vaccine is considered to be the gold standard when it comes to prevention, but it’s not the only one. Lifestyle also plays a key role in determining who will—and who won’t—get bitten by the flu bug.
These last few recommendations are likely ones you’ve heard frequently since the COVID-19 pandemic began, but they bear repeating:
Finally, contact your physician at the first sign of the flu. There are prescription antiviral drugs that help lessen the severity of flu symptoms and may even be able to shorten the length of time you are sick. But these medications must be taken before the flu progresses too far.
We exist to add quality of life to both you and your beloved. People turn to us daily for advice and consult. We’re here for you! Contact us today to schedule a tour!
20 September 2021

Welcome back to our assisted living and memory care blog. We’ve covered the first seven of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those seven blog posts are conveniently linked for you in the topic list below:
Congratulations! If you’ve accomplished all of the above, now it is time to make the transition. Yes, there will be stress involved, but take comfort that you are nearing a sharp increase in both your loved ones and your quality of life! So, let’s get moving!
Now that you’ve finalized the community, it’s time to make a smooth transition. Once you’ve gone through the terms and conditions and proceeded with the payment, you can help set-up rooms, get involved in activities, and help your parents settle in. It’s recommended to meet the care and administrative staff to build a bond with the caregivers who play an important role in the wellbeing of residents.
Display patience towards your aging parents as they settle in a new environment. If possible, show a genuine interest in the activities and you can even participate in one of the activities to make parents feel at home. It’s important to stay connected with staff and parents during this phase. Once the parents settle in, they will soon start to enjoy all the benefits being offered by assisted living and like their new home.
Important Points for Moving a Person with Dementia into an Assisted Living Community.
At times, it may take one to three months for your parents to adjust to this new environment and lifestyle. Your patience and support is vital in making this move successful.
We sincerely hope that you’ve discovered this eight-part blog series to be both useful and actionable. When the time comes for you to seek a consult regarding professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder is here for you. We’re ready to discuss some or all the topics listed above. Call us!
13 September 2021

Welcome back to our assisted living and memory care blog. We’ve covered the first six of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those six blog posts are conveniently linked for you in the topic list below:
In today’s seventh blog post of the series, we encourage you to take personal tours of every community under consideration.
Now that your basic research is completed, it’s time to pay a visit to shortlisted communities. But start with us though. I think you all understand by now that through this blog and other support services, our intent is to serve the entire general public not just our dear residents and family members. The more you know, the more you will come to appreciate us here at Manor Lake! Schedule a trip to the community to understand their environment. If possible, plan the visit along with your parents. It’s recommended to understand the community culture, know the meal preparations being offered, and take a tour of the premises.
Ask about:
When Visiting Communities, Here Are Few Items To Look For:
Discuss with family members about available options. Narrow down your choice once you have a general feel of the place, and know what to expect once your parents start living there. You can check on assisted living’s violations and citations with your state licensing records website. Most family members can also visit their loved ones anytime, but it is best to check with the service provider. During these trying Covid times, regulatory agencies can and do downward direct changing visitation management policy.
Once all the tours are done, all the questions answered, you gut will tell you that there is something special about our Gateway Gardens assisted living community and our memory care community. We’re ready to discuss some or all the topics listed above. Call us!
6 September 2021

Welcome back to our assisted living and memory care blog. We’ve covered the first five of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those five blog posts are conveniently linked for you in the topic list below:
In today’s sixth blog post of the series, our intent is to encourage you to do the obvious. You need to evaluate your options.
You may wonder why we recommend that you evaluate options. We are confident that the more you know about other local assisted living and memory care providers the more that you will appreciate and value us here at Gateway Gardens Assisted Living and Memory Care! Now that you’ve conducted due diligence regarding your needs, finances, requirements, and other considerations, it’s now time to investigate what’s out there for you.
Assisted Living communities come in various formats. Every community has its own look and feel. One of your most valuable resource resides right there inside you…you very own gut! We will never disparage any of your other options out there, but we do know this. Once all the tours are done, all the questions answered, you gut will tell you that there is something special about our Gateway Gardens assisted living community and our memory care community. We’re ready to discuss some or all the topics listed above. Call us!
30 August 2021

Welcome back to our assisted living and memory care blog. We’ve covered the first four of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those four blog posts are conveniently linked for you in the topic list below:
In today’s fifth blog post of the series, our intent is to help you learn how to research well. We are confident that the more you research, the more you will come to learn that we stand alone as your professional assisted living and memory care consultants and care providers. While every situation is unique, and each and every one of you have unique expectations, we are confident that we stand ready and more than able to address each and every one of your needs and concerns. So, let’s get started with how to research well.
Make a checklist of all your requirements based on the points mentioned above. Use these checklists to understand the offerings. A checklist helps you drill down to your requirements to pick the right community. If your parents need specialized memory care, then ensure your service provider has the right set of professionals. Assisted living communities that offer dementia care trained staff on the premises also have their residential areas catering to the needs of such residents. For example, facilities include doors with alarms or outdoor spaces that are enclosed with walking pathways.
We’ll help you add to your checklist of requirements. There are things you should expect from your care providers that you haven’t even thought of. The more you know, the more that, together, your loved one will enjoy the quality of care and quality of life that they deserve. So, we trust that it is becoming clear to you that when the time comes for you to seek a consult regarding professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder is here for you. We’re ready to discuss some or all the topics listed above. Call us!
23 August 2021

Welcome back to our assisted living and memory care blog. We’re here for you dear residents, resident’s family, and the entire local community. We’ve covered the first three of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those three blog posts are conveniently linked for you in the topic list below:
In today’s fourth blog post of the series, our intent is to help you define and understand your own limitations as it pertains to providing assisted living support. Simply to remind you all, as professional assisted living and memory care providers, we field calls every week regarding the financial considerations regarding professional health care. While every situation is unique, there are recurring considerations common for all of you. So, let’s get started with helping you know your own limitations.
When parents need assisted living, it’s often adult children that may also be in denial. However, you, as a primary caregiver for your aging parents, need to be aware of your own limitations in terms of time and physical presence you can offer. Those adults who commute frequently will be unavailable for their aging parents’ needs. Most importantly, aging parents also need fun and recreation - both of which are difficult to handle daily. It’s important for you to:
There comes a time when professional assisted living or memory care services are a safer and better choice compared to keeping your aging parents at home and alone. Dear friends, when that time comes it is not a comfortable period in anyone’s life. Even more difficult for most is the act of admitting to themselves that the time has actually come. We can’t determine that for you, but what we can do is help you through the analytical process that will aid you in making your own decisions. So, we hope you understand that when the time comes for you to seek a consult regarding professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder is here for you. We’re ready to discuss some or all the topics listed above. Call us!
16 August 2021

Welcome back to our assisted living and memory care blog. We’re here for you dear residents, resident’s family, and the entire local community. We’ve covered the first two of this eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. Those two blog posts are conveniently linked for you in the topic list below:
In today’s third blog post of the series, our intent is to help you understand your parent’s (or any other loved one’s) needs and issues. Simply to remind you all, as professional assisted living and memory care providers, we field calls every week regarding the financial considerations regarding professional health care. While every situation is unique, there are recurring considerations common for all of you. So, let’s get started with helping you understand your loved one’s needs and issues.
Determining your parent’s or other loved one’s needs empowers you with a better understanding of how moving in to assisted living community supports them in having a higher quality of life:
But what if the questions above leave you with more questions than answers? OK, stop for a moment and understand this. There are more people out there just like you who stress when addressing what only appear to be rather straight forward questions. These questions are in fact complicated and multifaceted questions that often require a professional support provider to help you break the challenge down into manageable parts.
We can help break all this down for you. We don’t promise to have all the answers, but what we can promise you is that we’ve guided people like you through this process countless times over the years. People describe our conversations as being a “refreshing breath of fresh air”. That warms our hearts and we welcome those conversations. So, when the time comes for you to seek a consult regarding professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder is here for you. We’re ready to discuss some or all the topics listed above. Call us!
8 August 2021

Welcome back to our assisted living and memory care blog. We’re here for you dear residents, resident’s family, and the entire local community. Last week we posted the first of an eight-part series on the subject of “When and How to Seek Professional Assisted Living or Memory Care”. That blog post is conveniently linked for you in the topic list below:
In this second of eight posts, our intent is to help you address how to determine your budget when the time comes. As we pointed out last week, as professional assisted living and memory care providers, we field calls every week regarding the financial considerations regarding professional health care. While every situation is unique, there are recurring considerations common for all of you. So, let’s get started on determining your budget.
Arriving at a reasonable monthly budget is often one of key criteria in the decision-making process. The cost of assisted living varies for each community. Some assisted living communities have an all-inclusive rate while others may have a base rate plus level of care charge.
Assisted living expenditures often fall under bracket of “private pay”. Some long-term care insurance plans may include support for this category. However, an individual can opt for an assisted living waiver if the beneficiary meets the clinical eligibility for the said waiver.
One cannot solely depend on Social Security benefits to pay for assisted living. While it is an important source of income for senior members, the fee for assisted living may go higher than the amount received through Social Security.
Veteran’s Administration (VA) also offers support for assisted living provided the eligibility criteria are met. Enrollment at the VA assisted living centers is as per availability and eligibility.
Depending upon your health insurance plan, Medicare may offer certain services not covered by assisted living. In recent times, state government offers support for assisted living through Medicaid programs. But, it may not cover the entire cost of the program. You will need a deep understanding to know if your parents are eligible to apply for certain Medicare or Medicaid benefits. We can help you with this!
When the time comes for you to seek a consult regarding professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder is here for you. We’re ready to discuss some or all the topics listed above. Call us!
2 August 2021

Hello dear residents, resident’s family, and the entire local community who are struggling through providing in-home assisted living or memory care services. This goes out to you whether you are or are not actively searching for professional care services in and around Winder. As professional assisted living and memory care providers, we field countless calls every week from people just like you who sometimes find it overwhelming to care for a loved one in need. Know that you are not alone! Those of you who follow our assisted living and memory care blog know that we invest in all of you by offering the lessons learned of our entire highly trained, skilled, and loving staff.
One of THE most common concerns we hear from people just like you is the comment, “This is all so overwhelming. I’m not sure what to do”. We’ve decided to not overload you here via a lengthy dissertation, rather, we’re going to begin today with the start of a short eight-part series to help you determine your future life care path for your aging parents. The eight-part series will consist of the following topics:
So, let’s get started by “Opening the Communication Channels”.
Your aging parents may consider themselves to be independent so you may face resistance to the suggestion of an assisted living community. You need to understand their needs and convey the situation in the best way possible.
We hope you benefit, are encouraged, educated, and enjoy our blogging efforts. When the time comes for you to seek a consult regarding caring for your loved one’s professional assisted living or professional memory care services, please know that Gateway Gardens Assisted Living & Memory Care Winder stands ready to improve the quality of both you and your loved one’s lives. Call us!
26 July 2021

In our last blog post, we discussed five benefits of chiropractic care for the elderly. That blog post hopefully got you thinking about a different way to manage pain. Today, we’re going to talk about something equally (or more) important than managing pain. We’re going to talk about managing heart disease.
Did you know that according to the Center for Disease Control and Prevention, seniors supported by professional assisted living professionals realize a statistically significant decrease in hospitalization for heart disease? This positive report is attributed to the professional support provided by assisted living and memory care communities such as ours at Gateway Gardens Assisted Living & Memory Care here in Winder, GA that deliver quality of life support programs as well as regular and reassuring professional health consultation.
The following items are primary goals of our assisted living and memory care community and our memory care community in an effort to reduce the rate of senior patients developing heart illnesses.
Provide Fitness and Relaxation
Keeping seniors active and relaxed improves heart health. Workout programs that range from low to moderate impact exercises are managed based on fitness levels and health status. Regular exercise helps lower stress levels and improve quality of sleep. When these two vital factors are achieved and stabilized, a healthier heart is guaranteed.
Promote Nutrition and Healthy Diet
Assisted living communities pay close attention to the nutrition and diet of their senior residents. They make sure that the food served to senior residents are both appetizing and healthy to improve food intake and facilitates consumption of important nutrients that can strengthen the heart. Also, taking note of food that must be taken moderately. Low-salt, low-fat, low-sugar diet are usually the dietary recommendation for these people.
Provide Smoke-Free Environment
We know for a fact that a smoker has a higher risk of developing chronic heart disorders including atherosclerosis and coronary heart disease. Gateway Gardens Assisted Living & Memory Care offers a designated outdoor area for smokers separated from non-smokers so that non-smokers will not be exposed to smoke-filled air. This is also a way to encourage current smokers to break the habit. Medical advises are also given to those smokers to support them to give up smoking.
For more information about assisted living and memory care services in and around Winder, contact Gateway Gardens today!
12 July 2021

Summer greetings to you, our faithful blog readers, cherished assisted living residents, memory care residents, and family members all! A common goal within our entire care team is to leave work each day and reflect that “I made someone smile today”. It is the goal of this blog post to educate you all regarding how chiropractic care can help increase mobility and decrease pain within our senior community. Less pain equals more smiles.
Before we get to it, we remind everyone to consult your primary care provider before implementing any of the ideas here. While it is true that American medical doctors increasingly embrace the drug-free and non-invasive nature of chiropractic care, each and every individual has unique challenges and concerns. So run all this through your doctor and together you two can make an educated decision. OK, so off we go!
Did you know that by 2030, it is estimated that approximately 20% of the US population will be 65 or older. As we age, we are more prone to aches and pains as well as balance and mobility issues that can result in falls. According to the CDC, falls are one of the 10 leading causes of nonfatal emergency department visits in the United States. Adults aged 65 and older have the highest incidence of unintentional falls with 3,143,536 falls in 2018.
As healthcare costs continue to rise (since 1999 it has more than doubled), many people are growing concerned about how they will be able to afford their medical care when they are older. Currently, annual healthcare costs are $11,300 per person in the U.S. This leaves many people wondering what they will do, how they will get the care they need during their golden years.
What is extraordinary is that chiropractic care has been shown to decrease healthcare spending in the over 65 segments of the population. More than 16% of a person’s healthcare spending occurs in the last year of life. Healthcare spending in those over 65 is 5 times more than children and 3 times more than adults (under 65). Regular chiropractic care has a significant impact on those expenses.
So, the answer, at least in part, is to get regular chiropractic care. Right?
Well, we have a way to go there. Only about 14% of older adults currently use chiropractic even though it has been shown to reduce the risk of arthritis, improve balance and mobility, reduce the likelihood of requiring the care of a nursing home, and even decrease the incidences of hospital stays.
Chiropractic for the elderly can be a great asset to their existing medical care.
Many people think of chiropractic care and think of a treatment for their aching back. The truth is, it has numerous applications and is a great treatment for many conditions. Even healthy people, seniors included, can benefit from regular chiropractic care.
Prevent Falls
Chiropractic care helps improve coordination and balance which helps to prevent falls. It makes the communication pathways throughout the spine more effective so that you have a better sense of where and how your body moves through space. This cuts down on falls as well as bumping into things.
Manage Pain
There have been many studies on how chiropractic is an effective pain management treatment – and not just for your back. It is a very effective treatment for several age-related conditions such as spinal compression fractions and osteoarthritis. Regular chiropractic care eases the pressure off of the joints which decreases pain or in some cases eliminates it.
Improve Balance
There are small receptors at the base of your neck (your cervical spine). These receptors give your brain messages that help it understand where your body and limbs are functioning in the space you are in. Aging decreases these receptors’ ability to function properly, and many older people begin to have balance problems as a result. Chiropractic care helps improve the communication between the spine and brain by stimulating the receptors and making them function more effectively.
Increase Range of Motion
Several studies, including an Australian study in 2001, have provided powerful evidence that chiropractic care greatly improves a person’s flexibility and range of motion. By bringing the spine back into alignment and the body back into balance, patients experience a greater range of motions and can move with much more ease.
Boost Immunity
A properly aligned spine allows for proper circulation which helps to move toxins through and out of the body. At the same time, the brain is better able to communicate with all parts of your body and organs. This allows it to better monitor the body, identify problems, and provide more efficient repairs. In one study, adults who received regular chiropractic care over a five-year period experienced a 200% increase in immune system function.
The evidence speaks for itself. Chiropractic care works and it is a great treatment for seniors. You don’t have to give in to age-related conditions! Chiropractic care can help to improve many so you can enjoy a better, richer quality of life.
So that’s it for today. Go out and make someone smile today. And for information on assisted living or memory care services here in Bethlehem, contact Gateway Gardens Assisted Living and Memory Care anytime.
2 July 2021

The 4th of July is a favorite summer holiday for Americans across the country. Whether you’re enjoying a barbecue with your dear loved ones here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care, or with them at home with you, we all relish the opportunity to celebrate freedom with those that we love and to welcome in the summer season.
Independence Day is considered one of our most important national holidays and a symbol of patriotism. The tradition of celebrating the 4th of July dates all the way back to the 18th century and the American Revolution. However, Independence Day didn’t actually become a federal holiday until 1941.
Fun Facts and History of 4th of July
From all of us here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem, we wish you a safe and happy 4th of July!
21 June 2021

At Gateway Gardens Assisted Living and Memory Care here in Bethlehem, we celebrate our residents and their spirit of independence not only on July 4th, but every day of the year. Our dedicated and loving staff is here to accommodate the unique lifestyle our residents choose so that they can enjoy the freedom to do what makes them happy. The flexibility afforded by this lifestyle option often has our dear assisted living residents wondering why they didn’t make the decision to move sooner!
We believe the key to a positive independent living experience lies in having a well-trained and dedicated service staff to anticipate the wants and needs of our residents. One of our top priorities here at Gateway Gardens is to empower our team of professionals to deliver the highest standards in hospitality services. We support your loved one’s independent streak! When wants and needs change, we help our senior residents navigate the senior living journey by having open conversations with senior family members that focus on long-term needs and maintaining a level of independence that fits those needs. When changes need to happen, family members can also focus on the positive aspects of those changes.
Our senior living options are designed to promote optimum levels of independence for our residents along with the freedom to enjoy the lifestyle they deserve! To learn more about our senior assisted living services and the quality of life you and your loved ones can enjoy here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem, contact us.
7 June 2021

We pride ourselves here at Gateway Gardens Assisted Living & Memory Care (Bethlehem) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Bethlehem who lovingly provide at-home assisted living and/or memory care services to your loved ones. Trust us, we know your challenges and consider you all heroes for your selfless and loving investment to family. Since we’ve officially entered the summer season, let’s address senior safety during periods of high heat.
Seniors are especially at risk in high heat situations. Large stretches of the USA are experiencing extreme temperatures at the moment. Caregivers need to check on the elderly. If you live in another city, lovingly devise a plan for a relative or other local person to check on your loved one.
Does an elderly person live in your neighborhood? Go knock on the door and ask how things are going. Do NOT accept the first answer. We all want to say, “OH, I’m ok, don’t worry.” The person may not realize they are suffering from heat exhaustion. Invite them into air conditioning, offer to take them to some air-conditioned setting. Sit in a hospital waiting room. Anything to get out of the heat for a while. Ask a senior to become an overnight guest.
Seniors need and deserve your special attention. We pride ourselves in pampering our dear residents with the special care and love they so rightfully deserve. To learn more about our approach to professional assisted living and professional memory care services, call us anytime!
24 May 2021

With raising spirits all around, we send our greetings to you, our faithful blog readers, cherished assisted living residents, memory care residents, and family members all! We are celebrating a degree of return to normalcy from pandemic-related lock downs. Family members are enjoying safely and personally celebrating life with all of our cherished residents. Families across our community are once again are prioritizing their summer vacation around their senior family member(s) under our assisted living care or memory care support services.
We’ve covered this subject before, but feel it is so important to revisit some considerations for your upcoming visits to your loved ones here at Gateway Gardens. Some of the things offered here might seem intuitive, others we bet you’ll find insightful and actionable.
So here you go, some things to consider when planning your summer vacation with your loved one:
First, it is always good to stop and remember those things that cannot be changed: aging, the effects of some illnesses, the progress of dementia, and other factors. “Old age,” as Betty Davis said, “is not for sissies.” Sometimes we see families whose holidays would improve if they paused briefly to realize that a parent will never again have the health and energy of past times. However, treasured memories can still be created with person before you. Honor that person; try to make him or her comfortable; ask to hear a story, or tell one yourself. Even in advanced stages of illness, holiday experiences can be joyous if accepted for what they are. It is good advice for life in general, and especially with aging loved ones.
Especially for elders who are not used to being active and have their own hopes for a vacation experience “like old times”, the temptation to try to keep too fast a pace during a holiday can lead to exhaustion. Be sure that every day someone is prepared to stay at home or leave an event early; your elder will be happier not trying to keep up with the most energetic members of the family. Try to rotate this responsibility so no one misses too much. It can be an adult child, a younger family member, family friend, or regular caregiver. This is simple, but easy to forget.
Whether it is security scans at airports or long car rides, the pace and distractions that many of us take in stride as part of travel can be exhausting, confusing, or frightening for elders. If you are in a rush, the problem is exacerbated. Plan ahead, allow for a slow pace and leisurely pace, and explain what is going on. This can relieve pressure on everyone.
People who visit home after an absence of several months sometimes can see the signs of decline in the condition of the home or the elder. It is important to be on the lookout for these, especially if family is not regularly present. Signs include a poorly- stocked kitchen, plumbing or appliances that do not function and have not been repaired, clutter that may be the initial stages of hoarding, or poor hygiene. Rarely to our elders call and say, “I cannot manage alone and I need help to continue living here.” Far more often, the signs appear without a request for help. If you have concerns about whether someone is safe at home, an assessment by a geriatric care manager or local senior citizens’ service center is called for.
Vacations with aging parents can be bittersweet. But with proper planning and the right attitude, the emphasis can be on the sweet. Do not try to do too much; find ways to enjoy the person as he or she is today, and to help him or her enjoy the day as much as possible. Grieve if it is called for, laugh when you can, ask for help when you need it. It is all part of life.
For information on assisted living or memory care services here in Bethlehem, contact Gateway Gardens anytime.
17 May 2021

We are warmed by your feedback and appreciation for the fact that our blog contributors here at Bethlehem’s Gateway Gardens Assisted Living and Memory Care provide meaningful and educational material. As you might imagine, a frequently discussed topic with phone callers and walk-in visitors centers upon how those on fixed income can cover the expense of senior assisted living professional care and/or professional memory care services. Today’s blog covers three of the financial avenues that are often tapped to cover or assist in covering the cost of professional care.
Many people don’t realize a senior’s life insurance policy — or that of a family member — can be used to pay for assisted living. You can sell a policy to a third party for market value and use the proceeds to fund a long-term care benefit plan while retaining some death benefits. Another option is “surrendering” a life insurance policy to the life insurance company for cash value. In this case, you give up ownership and won’t receive any benefits upon death.
If your loved one owns a home or other property, they may be able to cover assisted living costs with home equity. Some ways to leverage home ownership to pay for assisted living include:
If your loved one served in the military, worked for the government, or was a railroad employee, they may be eligible for a stipend to cover some assisted living costs.
Wartime veterans or spouses may qualify for a pension program through the Department of Veterans Affairs (VA) to offset the cost of senior care. Federal and Postal employees and annuitants, as well as qualified relatives, can apply for Federal Long Term Care Insurance (FLTCI), which helps pay for future long term care expenses. Employees have to apply for FLTCI before retirement, and certain medical conditions may prevent approval.
There are multiple other avenues that we are ready and eagerly welcome the opportunity to discuss with you. When we serve to increase your knowledge of how to best research your options, we are all warmed by so doing. Contact us here at Bethlehem’s Gateway Gardens Assisted Living and Memory Care to learn more!
3 May 2021

Greetings to our faithful blog readers, cherished assisted living residents, memory care residents, and family members all! It occurred to us that many of you may not realize the constant dedicated efforts of your support team in continuing education. The quality of all our caregivers is humbling to us and should serve as comfort to you. We’d like to make that point with you today by simply bringing to your attention just one of the countless subjects our staff invests their time and energy upon: Parkinson's and End of Life Care.
We are promoting continuing education regarding Parkinson’s and End of Life Care at no cost to our administrators and nurses. Parkinson's and End of Life Care is a 1-hour continuing education program approved for administrators, and nurses. We will examine clinical characteristics of Parkinson's disease in its later stages as well as special care considerations and issues that might arise. Also discussed are end of life care concerns among individuals with late stage Parkinson's disease and the introduction of hospice services.
Many seniors in residential care are diagnosed with Parkinson's disease and many other forms of dementia. Most will receive end of life care. It is important to look at the many care needs of the resident during their final stage of life.
Again, this is just for your information to remind you that those administrators and nurses that you see on a regular basis here at Gateway Gardens Assisted Living and Memory Care here in Bethlehem work hard each and every day, both within our care community and within the classroom. We thank them all here, and if you can, maybe you can thank them as well.
26 April 2021

Celebrating Memorial Day is both a solemn and joyous celebratory American tradition. First and foremost, it is a day of remembrance for those who have died in military service for their country. So, there is an inherent solemn presence throughout the holiday weekend. But it is safe to say that most (if not all) of those we honor on Memorial Day would want us to celebrate their sacrifice and to offer a positive energy to those who survive them. So that’s what we encourage all of you to do.
The big take away in this blog post is to remind all of you who provide senior assisted living care services and or senior memory care support services to a loved one that Memorial Day can be taxing on the heart of our beloved seniors. To some, the holiday is a reminder of a cherished loved one that has passed and who is sorely missed. We caregivers need to be prepared to guide our loved ones toward positivity of memories. You will provide your loved ones with a gift of love by investing some thought on specifically how you are going to deliver positivity to those loved ones who tend to get down during holiday events.
As this day is also seen as the beginning of summer, many people choose to decide to celebrate this day by having BBQ’s, going on vacation to summer destinations, or going camping in the mountains. These things are fun and a great time to get together with family and friends; however, maybe we could each spend a little time remembering those who have lost their lives. Spend time talking about family members you might have lost and the memories you have with them. Talk to your children and explain the significance of this day to them and why we get to take time off from work and school. Visit a cemetery where your loved ones are buried and take time to honor them. Go to Memorial Day events in your community, at schools, or city parks. Remember the families of those who have lost loved ones; find ways to let them know they are also being honored.
Here at Gateway Gardens Assisted Living & Memory Care in Bethlehem, we are forever grateful for those that have served our country and their families. We would not be where we are today without each of the men and women who have served. Let’s celebrate them together!
12 April 2021

Spring is finally here, and that means warmer weather has begun! Let’s hope it’s here to stay! After a cold winter, a spring celebration is almost necessary. Here are some fun ways to welcome the new season with your loved one who requires senior assisted living help or for your loved ones requiring memory care support services.
It is obvious that flowers are associated with spring – this is the season that flowers start to grow and flourish. At this time, flowers are bountiful and available and therefore less expensive. Why not bring some fresh ones into your home? Not only do flowers bring a wonderful scent (for those of you that like floral smells) into an environment, but a study done at Harvard has also found a few other positive effects: 1) Feelings of compassion and kindness for others are increased for people who have fresh cut flowers in their homes for only a week. 2) Negative feelings, such as anxiety, worrying, and sadness are decreased after being in a home with flowers. 3) Living with fresh cut flowers can increase energy, happiness, and enthusiasm at work. For those who enjoy creating, make pastel drawings or watercolors of the flower arrangement.
Gardening is a good way to get away from everyday worries for a little bit. It has been shown to be good for your health in a number of ways: 1) Time away from electronic devices by focusing attention on nature can relieve stress. 2) Gardening decreases symptoms of depression. 3) It is a form of exercise that gets the blood moving. 4) The increase in physical activity associated with gardening has been shown to decrease risks for dementia. Start seeds indoors if it is a cold, rainy day.
After birds’ migration to warmer weather during the winter months, hanging a bird feeder in the spring is a great way to welcome our feathered friends back for the spring and summer months. Bird feeders can promote education and learning about birds and can also be a way to connect with nature. Early risers can watch the birds feed in the early morning if a bird feeder is near the breakfast table, or you and your older adult are able to venture outside.
Why not switch up the daily routine and take a meal outside? Picnicking allows you to slow down and enjoy what you’re eating. It can also improve your mood and connect you with your surroundings and the people around you. The fresh air that you get while picnicking can revive your body and clear your mind. If the person you’re caring for is able to walk to the picnic spot, s/he will get a little exercise in, too.
While cleaning isn’t always everyone’s favorite thing to do, it is a great way to start a new season, especially spring. Cleaning for the spring, or any time, offers many benefits including having a clean and organized home, ridding your home environment of mold, mildew, dust, and bugs, decreasing clutter, prolonging the life of your appliances, and an overall sense of well-being and accomplishment. Dusting and straightening objects, even folding laundry, can be soothing tasks for people with low focus and restless energy. Everyone needs a sense of purpose and to know they can contribute.
After being “cooped up” in socks and warm shoes all winter, your feet are probably itching to be free. What might surprise you are the many benefits that walking around barefoot can have. Choosing to forego socks and shoes can give you greater balance, strength, and healthier feet, which decreases the number of foot conditions. It can also give you greater circulation, better posture, decreased blood pressure, and reduced inflammation (shown to be the number one cause of disease in the 21st century). Who would have known our bare feet could be so beneficial!
If the thought of being barefoot seems silly to the senior you’re caring for, or makes them chuckle, encourage them to talk about the time they were barefoot as a child, teenager, or as a young parent raising barefoot children.
These are just a few ways to embrace the warmer weather and the benefits that come with spring, but even simply appreciating the sun and outdoors (even from inside) can be a celebration and bring a new sense of purpose to life.
At Gateway Gardens Assisted Living & Memory Care here in Bethlehem, we know caring for an older adult brings joys and challenges. Our mission is to change the way the world ages. We provide seniors with quality care that enables them to live happier and healthier lives. Our services are distinguished by the caliber of our caregivers, the responsiveness of our staff and our expertise in Live-In care. We embrace a positive, balanced approach to aging centered on the evolving needs of older adults. For more information, contact us here at Gateway Gardens anytime!
5 April 2021

Well, Easter 2021 has come and gone. Hopefully, all of you out there shared precious and memorable moments celebrating Easter with your family. Now it is time to celebrate Spring and a systematic return to more pleasant weather. As most of you know, here at Bethlehem’s Gateway Gardens Assisted Living and Memory Care we offer regular and recurring advice via this blog to educate our residents, their family, caregivers, and friends.
Over the weekend, a neighbor who cares for her senior father confided that her Dad didn’t celebrate her traditional Easter meal as he normally does. It was just a passing comment and in no way meant to be critical. It gave me pause to share with her a few things to keep in mind about the aging process, one of them being about aging and its effect upon the sense of taste. More on that in a moment.
When you think of the aging process, you may think of wrinkles, diminishing vision, hearing impairment, or muscle loss. These are obvious signs of growing old, and they happen to almost everyone. However, there are effects of aging that many people overlook. These concerns may go undetected for some time, so it is important to know how our bodies are continually changing. The following are four results of growing older that you may not have considered.
Growing old is something no one can avoid. Remember to be aware of the ways your body may change so that you will know if or when they happen. At Gateway Gardens Assisted Living & Memory Care here in Bethlehem it is our privilege to keep your loved one loved, healthy, and cared for.
22 March 2021

It is probably never going to feel like the right time to have “The Talk” about a memory care facility with a parent who is the caregiver of a spouse with dementia. Many adult children avoid bringing it up because it’s such a complicated and sensitive topic. Here at Gateway Gardens Assisted Living & Memory Care (Bethlehem), we’ve helped countless people like you prepare for this most difficult conversation whether your need is for professional assisted living care services and professional memory care services. Today, we’re going to focus on those of you facing memory care needs, but much of this advice applies to transitioning to assisted living as well.
But the best time to approach this tough issue is right after the initial diagnosis. As dementia progresses, it’s possible that your parent could have specialized needs that can’t be met at home. Being proactive in having the talk about your parent’s plan of care as the disease progresses ensures a plan is in place that allows your caregiving parent to get the support they need to provide quality care.
If your parent is the caregiver of a spouse with dementia, it may take some time to process and identify where the line is between being able to provide quality care at home versus when the support of trained, specialized care providers should be sought. Through regular conversations where you show that you’re genuinely concerned about both of your parents’ well-being, you can be instrumental in identifying potential future problems and instigating change.
Before you bring anything up, do your homework so you problem-solve with your parent, not dictate the solution or convince through arguments. Learn about how the disease will progress and how it could impact your parent’s ability to stay at home.
The Alzheimer's Association website is a great resource for information about how to help your loved one remain as independent as possible, how behaviors change as the disease progresses, strategies caregivers can use to manage stress and how to decide which care options may be the best fit.
Research the memory care facilities in your parents’ community so you can come to the table with some options that are available in your area.
Test the waters before you broach the subject. Give your caregiving parent a call to see how they’re doing and to get a sense for how they might react when you bring up the topic of a memory care facility. Caring for a loved one with dementia can take its toll, so say something like, “How's your health? The doctor say anything new?" If your parent responds openly, show that you’re ready to be a helpful resource by saying something like, “Is there some way I can be helpful?"
Avoid the temptation to plan a family meeting. Family meetings can feel threatening and overbearing and more like an “intervention” than family support. Instead, have the conversation in a more natural way, such as at the kitchen table over a cup of coffee. After relaxing and enjoying each other’s company for a little while, look for an opening when you can move into a more serious conversation.
Depending on your relationship with your parent, you might want to take the more direct approach by saying something like, “I noticed that you’ve been more tired than normal and that you were so busy last week that you forgot your own doctor’s appointment. Are you getting enough time to take care of yourself?”
If your parent is more self-conscious or private, consider taking a more indirect approach by saying something like: “I read in the paper about a husband who was taking care of his wife with dementia. He got so worn out that he had a heart attack, even though he had no history of heart disease. It made me think about you taking care of Dad and how hard that can be for one person to do.”
No matter which approach you take, be gentle. Talk in a calm tone of voice, offer a reassuring touch and follow your parent’s cues.
Adult children can be eager to solve their parents’ problems, but your parents are just as committed to maintaining a sense of control. Additionally, caregiver grief and guilt are common reactions to moving a spouse to a memory care facility. Yes, you want your parents to be safe and secure, but your parents need to feel heard, respected and valued, too.
If there is resistance or conflict, pay close attention to the feelings being expressed, and recognize and respond to the things that matter to your parent. Make sure they feel supported and understood by using reflective listening. Say something like, “I hear you saying ... but it's also worth thinking about this … ”
Remind them that they won’t always be able to safely take care of their spouse with dementia at home alone and that they can be a better partner if they aren’t totally exhausted by all of their care needs. Find ways to be reassuring, and frame the discussion as a place where everyone’s opinions can be heard.
It’s important to understand that “The Talk” really isn’t a one-time conversation. It’s simply the first in a series of discussions over time. After some time passes and your parent has had a chance to think about it, look for other opportunities to raise the issue again.
If your parent shows signs of warming up to the topic, show them that you are trying to be their advocate, and offer to go with them for a tour of memory care facilities. If they say something negative, be patient, but don’t give up. Connect them with a caregiver support group, which might help them come to terms with the idea that sometimes the best decision for the health and happiness of everyone is to consider moving the spouse with dementia into a memory care facility.
Remember that, ultimately, this is your parent’s decision. The best thing you can do is remain positive and supportive throughout the ongoing discussions about a potential move. And remember, whether you need guidance related to senior assisted living or memory care support services, we’re here for you. Let’s talk.
15 March 2021

Our blog posts are syndicated to various social media sites in the interest of educating and keeping our residents and their family informed. GOOD NEWS! The visitation policy update is posted on our home page, but we feel important to place it here in our blog to facilitate maximum exposure.
We are pleased to announce that the in accordance with the Executive Order for Long Term Care the community is allowing Family Visitations. The recent decline in Covid-19 cases in the County allows us to safely have visitors in the community. Each of our properties has specific guidelines for the families to follow and currently visitation is by appointment. Please feel free to contact the community directly for hours and schedule. Additionally, communities are open for Dining and Activity Programing. We are also pursing or have opened our Hair Salons depending on each community’s specific plan for reopening.
8 March 2021

Today we dedicate our discussion to those of you wondering if the senior loved ones under you care are safely served by being online and active in social media circles. For reasons you can likely conclude on your own, your concerns for your loved one who requires memory care support is much greater than those receiving senior assisted living support. Regardless of the type of care you provide, all of us here who deliver professional assisted living and memory care support services understand, respect, and value the quality of life enhancing results that healthy online living delivers. So let’s get to it.
Ten years ago, few people would have predicted that seniors would become some of social media’s most passionate users. But a study last year by Pew Research Center found that 62% of online seniors are on Facebook. Other studies show that social media use among seniors is rising at a rapid rate. As more and more seniors use social media, there are growing concerns. With that said, most research indicates that social media improves quality of life for elderly adults. But some senior care professionals are increasingly worried about the dangers that social media could pose to seniors’ well-being.
On the whole, social media seems to have a positive effect on seniors’ well-being. Internet use has been shown to reduce seniors’ risk of depression by as much as 33%. One study found that seniors who use Facebook show marked improvements in cognitive function. Another study found similar results when seniors were trained to use email, Skype, and Facebook.
Social media also opens new avenues for seniors separated from children and grandchildren by long distances. Facebook makes it easy to keep in touch with family members. Video-calling is particularly popular with seniors, who use services like Skype to connect with their grandchildren.
So why are some people concerned about the dangers of social media for elderly well-being?
One common concern is that social media could, over time, make seniors more depressed. When researchers have surveyed social media users of all ages, they’ve found instances where social media use is linked with higher risk of depression. However, this concern might be overblown among the elderly — after all, research has found that online seniors are less depressed than others.
A study out of the University of Missouri might explain why. In that study, researchers found that the risk of depression only rose in social media users who were using sites like Facebook to compare themselves to others. Depression was tied to an increase of jealous feelings and lower self-esteem. If users were using social media primarily to keep in contact with others, their risk of depression did not increase. Since most seniors use social media for keeping in contact with family and friends, it makes sense that most seniors aren’t at high risk of depression due to social media use.
A much bigger concern is how social media affects seniors’ in-person interactions. Senior isolation is a serious problem among the elderly, one with devastating health effects. Social media use can alleviate some of these effects, but it’s not enough. Seniors need to regularly spend time in the physical presence of others to avoid the emotional, mental, and physical effects of senior isolation.
If seniors and their families start to treat social media as a replacement for in-person interaction, that could put a greater percentage of seniors at risk for feelings of isolation and loneliness. “There are obvious benefits to social media use among seniors,” says Larry Meigs, CEO and President of Visiting Angels. “If social media is used to augment in-person contact, that’s fantastic. But there’s a real concern that seniors and their family members might have less of these interactions the more they rely on social media.”
Ultimately, social media is a positive tool for seniors, families, and senior care providers. But it’s something that should be approached with a degree of caution. If social media is your loved one’s main avenue for social interaction, or if you’ve noticed they’re spending less time with others now that they’re on Facebook, it may be time to consider a change.
Spending more time with your loved one is always a welcome solution. But it might not be enough. If you live far away or have a busy schedule, frequent visits aren’t always practical. When it’s time for you to seek help from a team of proven senior living or memory care professionals in and around Bethlehem, we’re there for you. Always.
1 March 2021

From all of us here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care, we appreciate the positive feedback from our blog readers regarding the practical utility of our blog posts. Many of our readers are at home taking care of their loved one’s Assisted Living support needs and/or their Memory Care support requirements. We are honored and humbled to lend a hand via our weekly blog posts. Today, let’s try to find a laugh in it all with some help from our friends at DailyCaring.com.
“I was kneeling beside Mom’s bed last night when she was saying her bedtime prayer. This night she prayed, ‘Now I lay me down to sleep, I pray the LORD my soul to keep. If I should die before I wake, I pray he takes me like an earthquake.’ Instead of …my soul to take. I said ‘what?’ Mom laughed and said, ‘well, I couldn’t remember the rest and …well, it rhymed!’ ~ Amen!”
Funny moments happen while you’re caring for an older adult. Look to recognize and celebrate them. Of course, chronic illnesses or diseases like Alzheimer’s are certainly no laughing matter. But even in the middle of the worst day, there’s still room for laughter.
Let’s talk about why it’s good for both you and your senior to find humor in caregiving and why you shouldn’t feel guilty about it.
Even if you’re caring for an older adult with a debilitating illness or in declining health, the world doesn’t have to be dark, gray, and depressing all the time. It might sound counter-intuitive, but these are the times when a dose of humor is most needed.
Besides, being angry, miserable, and tense won’t change a bad situation or make your senior’s life more pleasant. So why not try to look at the funny or positive side of things whenever possible? Like we do here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care, look for ways to engage the creative spirt! Your certain to find reward and humor in it all.
It turns out that humor is a very effective way of coping with the difficult emotions that come with caregiving and aging.
In research studies, over 75% of recurrent cancer patients and those facing terminal illness said that maintaining a sense of humor was very important. It was right up there with being pain-free. That’s a pretty big endorsement.
A common reason why caregivers resist looking for humor is that they feel guilty about seeming mean or disrespectful of their senior. In truth, part of being a wonderful caregiver is to let yourself laugh and to encourage laughter in your older adult.
After all, you’re not laughing at the person you love and care for. You’re laughing at a funny, ridiculous, or ironic situation. Best of all are the times when your older adult laughs even harder than you do.
“I came home yesterday from work and Mom came out to the kitchen to greet me. I said, ‘Mom, you have on my sweat pants!’ We each have a pair of soft, comfy pea green sweats. Hers are a size 14 and mine are a few sizes bigger! She says, ‘I thought I had lost a lot of weight!’ Then she pulls up her shirt to show me she had them pinned to her bra to keep them up! We had a good laugh!”
No caregiver and no older adult will feel like laughing all the time. But giving yourself permission to notice when funny things do happen and encouraging your senior to laugh eases the burden and makes life more positive for both you.
Are you at home providing assisted living and/or memory care services of a loved one. Know that you are never alone. Contact Gateway Gardens Assisted Living and Memory Care anytime. We know your challenges and can help!
22 February 2021

This is the third of a three-part blog series designed to help those of you considering a transition to professional senior assisted living care here in Bethlehem. So far, we’ve covered when is the right time to move and how to prepare for a move. Today, we’ll cover what to expect after the move.
It’s important to remember that it can take a while to adjust to your new environment after any move. After a move is complete, everything will be new: new place, new people, and new routines. Here are our recommendations for making your move as smooth as possible:
The right moves for seniors are often made with ample research and planning. We recommend evaluating your situation carefully. Maybe the simplest advice is to lean on us here at Gateway Gardens Assisted Living and Memory Care every step of the way. We are honored and confident in our ability to help you achieve the smoothest transition possible. Contact us!
15 February 2021

Last week we discussed when is the right time to move into a managed senior living community. This blog post is targeted for those of you who have decided that now is the right time to transition to assisted living care here in Bethlehem. Today, we’ll discuss how to prepare for you or your loved one’s move.
Moving can be challenging for seniors and their families both emotionally and logistically, even if the move is ultimately the right decision. In order to make helping seniors move as easy as possible, here are our top tips to help make sure you’re prepared:
When the time comes for you to seek a consult regarding caring for your loved one’s senior assisted living care needs, please know that Gateway Gardens Assisted Living & Memory Care here in Bethlehem stands ready to help you every step of the way! Contact Us anytime to learn how we do this!
8 February 2021

While there are countless benefits that come with managed senior care, all of us here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem understand that it can be a stressful topic for individuals and families. Transitioning to managed care means saying goodbye to a home that’s comfortable, familiar, but may no longer be safe. A high percentage of new residents and their family members here within our senior assisted living community contemplated moving for months. They did this for good reasons. Transitioning from independent living is without doubt one of the most difficult decisions anyone will ever make.
Our advice is to acknowledge these feelings but to also focus on the positive aspects of moving. It’s also important to seriously evaluate and consider your current and future needs. Some reasons why considering a move might be the right choice include:
1 February 2021

We’d like to share some keen insight with you from Dr. Elizabeth Galik (Phd, CRNP) and Dr. Richard Stefanacci (MD, DO) regarding their views on improving care for patients with dementia. It is a professional obligation for the staff here at Gateway Gardens Assisted Living & Memory Care (Bethlehem) to exercise continuing education on the subjects of professional assisted living care services and professional memory care services. The big takeaway here is the need for those of you caring for a loved one with any form of dementia to be honest and proactive to position both you and your loved one from suffering avoidable (and sometimes unrecoverable) quality of life crisis.
With over 5.8 million individuals living with dementia, and after failures of all the recent attempts for treatment or cure, there is no better time to get back to basics in the geriatric management of dementia. As in most geriatrics care, providing quality dementia care requires a caring collaborative for the best clinical, psychosocial, and financial outcomes.
Most think of dementia care in the long-term care (LTC) setting as occurring in the late stages of the disease within the confines of the LTC units of a skilled nursing facility. However, an increasingly large number of early-stage dementia patients are coursing through the subacute units of skilled memory care communities. So in addition to addressing acute medical comorbidities and rehabilitative goals of traumatic injuries, these subacute stays often signal a major change in cognition, function, or behavior for individuals with dementia.
These changes in condition will require a reassessment of the plan of care for these patients, regardless of whether they return home, move in with their family, or transition to professional memory care on a permanent basis. The subacute stay provides an excellent opportunity to modify the plan of care for patients with dementia and their families.
Dementia — a chronic or persistent disorder of cognitive processes and functional impairment — is predominately progressive in nature. With a known trajectory of decline in cognition, language, motor function, and perceptual abilities, proactive planning for future care is important to minimize negative outcomes and optimize person-centered care approaches. All too often, this planning is put off for far too long.
In most situations, advance planning for eventualities such as the inability to drive or take medications safely or the need for increasing support to maintain activities of daily living is not addressed until a crisis occurs. As clinicians, we can all play a role in addressing these issues sooner rather than later. One benefit in addressing care and safety needs sooner is that it may be easier for the patient to adjust to a change in routine, a new caregiver, or a new supportive environment early in the course of dementia.
Moving to a more supportive and supervised environment early, when the symptoms are less severe, can actually improve the individual’s and caregiver’s health and well-being. If the move to a new setting occurs later, after the patient’s dementia has progressed to the moderate to severe stages, an accelerated decline may occur afterward.
Often there is a small window for the change to be beneficial. Once that window closes — and if the individual’s needs for increased supervision, assistance, and care, potentially with LTC services, have not been addressed — both caregivers and clinicians must prepare for a rescue mission. They may be confronted by an impending crisis that arrives in the form of a traumatic fall, motor vehicle accident, getting lost, or other major catastrophic event.
The post-acute and long-term care (PALTC) interdisciplinary team frequently works together with individuals with dementia and their families to address realistic care and rehabilitative goals. They may deprescribe unnecessary or inappropriate medications, optimize quality of life, and assess and manage the complicating medical comorbidities and behavioral and psychological symptoms of dementia.
If you live in or around the Bethlehem area and ever have questions about the challenges of creating a 24/7 safe and loving atmosphere for your senior loved on, we’re here to help. We want to develop a relationship with you based on trust and a common love for our ageing loved ones. We trust that when the time comes, you’ll team with us for your professional senior assisted living or memory care support services. Together, we’ll provide the best loving care possible. Give us a call. Let’s talk.
25 January 2021

Deciding on how to best care for your loved one with Alzheimer’s or dementia can be overwhelming. As professional assisted living and memory care service providers here in Bethlehem, we know this all too well. Whether you’re here with us now, or struggling at home to care for a loved one, education, relief, and comfort are just a phone call away.
In the early stages, many people prefer to try to keep their loved one at home, either with the help of family or part-time caregivers. However, caring for someone in the advanced stages of dementia can be a full-time job. Most family caregivers are simply not able to dedicate 100% of their time. Also, in the long run, the family home is often not the most suitable environment, mostly due to safety concerns.
Professional Memory Care communities like ours here at Gateway Gardens are designed with Alzheimer’s and dementia care residents in mind. From the physical structure of our building, our grounds, specially trained staff, personal attention, and carefully planned activities, all aspects of Gateway Gardens living is tailor-made to meet the particular needs of residents in all stages of dementia with a variety of other health issues.
Safety & Security: Injuries are the single biggest risk to folks with Alzheimer’s or dementia. Wandering is a common behavior and can be a source of many problems. Residents are lovingly monitored 24 hours a day.
Personalized Care: Each resident has a customized care plan based on his/her particular needs. Our low staff to resident ratio allows for each resident to receive the best possible care and frequent contact with staff.
Staying Engaged & Socializing: Isolation can be very detrimental to the health and wellbeing of folks with dementia. We strive to help residents stay engaged and socially active. Residents are encouraged to spend much of their time with other residents in the dining and common areas.
Staying Active: The programs and staff are focused on helping residents stay as physically active as possible throughout the day. While residents have their own apartment, the communities are designed to encourage residents to move about the community. There are also secure outdoor walking paths for residents to enjoy.
Maintaining Independence: Although memory care residents often need help and care with many basic daily activities, we encourage residents to maintain a healthy level of independence, allowing them to age in place with dignity and grace.
Having Fun: Throughout each day, there are a variety of programs that offer residents the opportunity to have fun and enjoy themselves. Some of these enriching activities include games, gardening, field trips and outings, music and art therapy, and spiritual programs.
We hope you benefit, are encouraged, educated, and enjoy our blogging efforts. When the time comes for you to seek a consult regarding caring for your loved one’s memory care needs, please know that Gateway Gardens Assisted Living & Memory Care Bethlehem stands ready to improve the quality of both you and your loved one’s lives. Call us!
11 January 2021

The difference between simple entrepreneurial and genuinely loving professional senior assisted living care and truly loving professional memory care services is volunteer investment in our residents, their families, and the local community. This blog here at Gateway Gardens Assisted Living and Memory Care here in Bethlehem is a perfect example. We publish topics that we know benefits a much wider community than our Manor Lake family and we take great professional reward in so doing. Today’s blog is duly credited to our friends at Elmcroft who earn our respect as like-minded community servants.
Everyone is forgetful sometimes. Forgetting an item while grocery shopping, misplacing your keys, missing your exit while driving or not remembering an appointment every so often are no real causes for concern. Forgetfulness can seem to get worse when you’re experiencing stress, are especially busy, have taken on a new challenge, or haven’t been getting enough sleep. Occasional memory lapses are apart of the normal aging process, and there is probably no cause for alarm if forgetfulness or absentmindedness are not getting significantly worse or accompanied by other problems like personality changes, disorientation, frequent struggles to find the right words or difficulty completing familiar tasks.
The difference between normal forgetfulness and dementia is that dementia causes memory loss and other issues that disrupt daily life and become disabling.
Unlike normal age-related changes in memory and thinking, which may be occasionally bothersome or frustrating but don’t significantly disrupt a person’s life, dementia is not part of the normal aging process. Dementia is defined by the Centers for Disease Control and Prevention (CDC) as the impaired ability to remember, think or make decisions that interferes with doing everyday activities. Alzheimer’s disease is the most common type of dementia, but there are several other forms of the disease.
According to the CDC, symptoms of dementia can vary widely from person to person. People with dementia often have problems with memory, attention, communication, reasoning, judgment, task completion, problem-solving, mood, behavior, and spatial and visual perception.
Early signs a loved one may be developing dementia include:
These signs do not necessarily mean someone is developing dementia. Many of these symptoms can also stem from emotional stress or grief, mental health issues like anxiety or depression, reactions to a new medication, and medical problems like head injuries, vitamin deficiencies, thyroid disorders, infections, stroke and tumors. That’s why it’s important to consult a medical professional if your loved one has several of these symptoms, or if the symptoms seem to linger after a stressful event.
According to the National Institute on Aging, some seniors can also develop a condition known as mild cognitive impairment, or MCI. This means they have more memory or other thinking problems than other people their age, but they can usually care for themselves and participate in normal daily activities. MCI can be a precursor to Alzheimer’s disease or dementia, but not everyone diagnosed with MCI will progress to the more severe diagnosis. The Mayo Clinic says that while about 1% to 3% of older adults develop dementia every year, studies suggest that around 10% to 15% of individuals with MCI go on to develop dementia each year.
If you or your loved one is having trouble remembering, thinking, concentrating or participating in familiar activities and everyday tasks, it’s important to see a doctor. A thorough examination will include blood tests (and other diagnostic tests, as needed), a review of prescription medications, cognitive and mental health evaluations, and discussions about recent stressors and lifestyle choices. The results of that examination may help a doctor uncover a treatable and even reversible cause of the symptoms.
Dementia-like symptoms caused by depression, pharmaceutical side effects, drug or alcohol abuse, tumors and other structural problems in the brain, metabolic or endocrine conditions, and nutritional deficiencies can be reversible.
If the doctor suspects dementia after the examination, a course of management and treatment can be recommended. Neurodegenerative dementias, like Alzheimer’s disease, have no cure, but medications are available that can help slow their progression or reduce symptoms like disorientation, anxiety, delusions or behavioral changes. Research is underway for more effective treatments.
A healthy diet, active lifestyle, memory/brain games, strong social support and community involvement can offer some protection from memory loss and may slow the progression of Alzheimer’s disease or related forms of dementia. Environmental modifications and breaking down tasks into simpler steps can help increase independence and safety and reduce frustration and confusion. Non-medical treatments may also help lessen symptoms and improve the quality of life for people with dementia. These include:
If you or your loved one struggle with sleep issues, talking with your doctor is a good place to start. Our assisted living and memory care community here in Bethlehem is designed to support our senior residents by providing a safe, secure environment where their everyday needs are met. We not only offer comfortable housing accommodations but also indoor and outdoor amenities, events, and fitness programs to keep you physically and mentally active during your senior years. We are proud to deliver professional assisted living and memory care services that measurably improve quality of life.
We welcome your call and/or visit to learn more. Contact us today!
4 January 2021

Here at Gateway Gardens Assisted Living & Memory Care, our team of professional memory care and assisted living care providers constantly seek ways to improve the quality of life of our residents, their family, and their friends. Today’s blog addresses one of the most prolific thieves of quality of life, untreated hearing loss. There are many different causes of hearing loss, and in many cases, hearing loss is something that happens steadily over time. This can make it difficult to notice. For many of us, the idea of getting our hearing checked can be frightening.
If you think a loved one might be suffering from hearing loss, however, it is important to get it checked out, as being hard of hearing without seeking help can be quite isolating. Here are four signs to look out for in your loved ones that you suspect might be hard of hearing.
1. They often complain that other people are mumbling.
If your loved one is suffering some hearing loss, to them, it does sound like others are mumbling. Try speaking a little slower, making sure to clearly enunciate your words, and see if that helps them. Louder is not always better — be sure you are looking at them so they can also see your mouth and lips moving as you speak. If your family member is still struggling to understand what you are saying, the problem likely is their hearing, not your speaking style.
2. They have a difficult time hearing women’s or children’s voices.
The pitch range of most women and children’s voices is a higher frequency than that of most men, and women and children tend to speak more softly than men, as well. High-frequency hearing loss is the most common type of hearing loss. If your loved one is having trouble hearing women and children when speaking, it might be time to suggest an appointment with a specialist.
3. They answer inappropriately to questions or seem to be answering another question.
If such odd answers are an increasingly common occurrence, try asking the same question again, looking your loved one directly in the eye and speaking a little more slowly. If they can understand and answer the right question when you take extra steps, it might be time to consider a checkup.
4. They avoid social situations or frequently miss phone calls or a ringing doorbell.
It is common for people experiencing hearing loss to withdraw because they are worried about not being able to hear conversations, whether in person or on the phone. Talk to your loved one, either in person in a quieter setting or even via email if they use that and see if there might be other reasons for their isolation. If not, it could be time to talk to them about hearing loss options.
If you have any questions regarding your loved one’s real or suspected hearing loss here at Gateway Gardens, contact us anytime. We will be glad to consult you regarding how to address the subject with your loved one and the local options that you have for professional hearing treatment services.
21 December 2020

Manor Lake Assisted Living Communities are Considered 1-A Long Term Care Facilities by the Georgia Department of Public Health. With the 1-A status our residents and Staffs will be among the first to be offered the Vaccine. We have already contacted the two approved providers for the Vaccine Walgreens and CVS pharmacies to ensure our staff and residents are scheduled for Vaccination Clinic dates as soon as possible.
Get more information from Gateway Gardens here.
To learn more about the Covid-19 Vaccine Distribution plan from the Georgia Department of Community Health follow the link below to the Plan Document.
Manor Lake Assisted Living & Memory Care is Accepting New Residents. For many of our seniors Assisted Living or Memory Care at Manor Lake is currently the best option. Considering the enhanced safety measures that Manor Lake is taking, moving into a senior community may make more sense than living isolated alone at home and not getting adequate care.
Maintaining the health, wellness, and safety of our residents is our number one priority. Due to the COVID-19 situation, effective immediately we are restricting visitors to our community. This is in cooperation with federal mandates regarding this situation. Letters regarding specific details are being sent to the responsible parties for our residents to provide them with more detailed information. In addition to restricting visits, our staff will be screened prior to the starting of their shifts and have been trained on the symptoms of COVID-19 as well as infection prevention techniques. This is a fluid situation and we will keep you informed as the situation changes. We appreciate your cooperation and patience. If you have any questions, please don’t hesitate to contact us.
14 December 2020

Our team of professional memory care and assisted living care providers here at Gateway Gardens in Bethlehem are there for all of you, young and seasoned alike. Today’s blog offers numerous “brain exercises” that we all can to do improve memory and focus. Again, these exercises are not directed at our assisted living and our memory care residents, but to their families and indeed, all members and family members of the staff here at Gateway Gardens here in Bethlehem. We send due credit to “Healthline”, who authored these superb ideas.
The brain is involved in everything we do and, like any other part of the body, it needs to be cared for too.
Exercising the brain to improve memory, focus, or daily functionality is a top priority for many people, especially as they get older. That said, people of all ages can benefit from incorporating a few simple brain exercises into their daily life, which we’ll explore in more detail in this article.
Research has shown that there are many ways you can hone your mental sharpness and help your brain stay healthy, no matter what age you are. Doing certain brain exercises to help boost your memory, concentration, and focus can make daily tasks quicker and easier to do, and keep your brain sharp as you get older.
Let’s take a deeper dive into 13 evidence-based exercises that offer the best brain-boosting benefits.
1. Have fun with a jigsaw puzzle
Whether you’re putting together a 1,000-piece image of the Eiffel Tower or joining 100 pieces to make Mickey Mouse, working on a jigsaw puzzle is an excellent way to strengthen your brain.
Research has shown that doing jigsaw puzzles recruits multiple cognitive abilities and is a protective factor for visuospatial cognitive aging. In other words, when putting together a jigsaw puzzle, you have to look at different pieces and figure out where they fit within the larger picture. This can be a great way to challenge and exercise your brain.
2. Try your hand at cards
When’s the last time you played a game of cards? Researchers who conducted a study in 2015Trusted Source on mentally stimulating activities for adults, say a quick card game can lead to greater brain volume in several regions of the brain. The same study also found that a game of cards could improve memory and thinking skills.
Try learning one of these tried-and-true card games:
3. Build your vocabulary
A rich vocabulary has a way of making you sound smart. But did you know you can also turn a quick vocab lesson into a stimulating brain game?
Research shows that many more regions of the brain are involved in vocabulary tasks, particularly in areas that are important for visual and auditory processing. To test this theory, try this cognitive-boosting activity:
4. Dance your heart out
The Centers for Disease Prevention and Control notes that learning new dance moves can increase your brain’s processing speed and memory. In other words, bust a move on the dance floor and your brain will thank you.
Want to test it out? Give one of these dance activities a try:
5. Use all your senses
A 2015 research report suggests that using all your senses may help strengthen your brain.
To give your senses and your brain a workout, try doing activities that simultaneously engage all five of your senses. You could try baking a batch of cookies, visiting a farmer’s market, or trying a new restaurant while you focus on smelling, touching, tasting, seeing, and hearing all at the same time.
6. Learn a new skill
Learning a new skill is not only fun and interesting, but it may also help strengthen the connections in your brain.
Research from 2014 also shows that learning a new skill can help improve memory function in older adults.
Is there something you’ve always wanted to learn how to do? Perhaps you’d like to know how to repair your car, use a particular software program, or ride a horse? You now have one more good reason to learn that new skill.
7. Teach a new skill to someone else
One of the best ways to expand your learning is to teach a skill to another person.
After you learn a new skill, you need to practice it. Teaching it to someone else requires you to explain the concept and correct any mistakes you make. For example, learn to swing a golf club, then teach the steps to a friend.
8. Listen to or play music
Do you want an easy way to increase your creative brain power? The answer may lie in turning on some music.
Listening to happy tunes helps generate more innovative solutions compared to being in silence. Which means, cranking up some feel-good music can help boost your creative thinking and brain power.
And if you want to learn how to play music, now is a great time to start because your brain is capable of learning new skills at any point in your life. That’s why you’re never too old to start playing an instrument like the piano, guitar, or even the drums.
9. Take a new route
Don’t get stuck in a rut when it comes to your daily tasks. Instead, be willing to try new ways to do the same things.
Choose a different route to get to work each week or try a different mode of transport, like biking or using public transport instead of driving. Your brain can benefit from this simple change, and you might be surprised by how easy it is to change your thinking.
10. Meditate
Daily meditation can calm your body, slow your breathing, and reduce stress and anxiety.
But did you know that it may also help fine-tune your memory and increase your brain’s ability to process information? Find a quiet spot, close your eyes, and spend five minutes meditating each day.
11. Learn a new language
A 2012 review of research has overwhelmingly proven the many cognitive benefits of being able to speak more than one language.
According to numerous studies, bilingualism can contribute to better memory, improved visual-spatial skills, and higher levels of creativity. Being fluent in more than one language may also help you switch more easily between different tasks, and delay the onset of age-related mental decline.
The good news is that it’s never too late to reap the rewards of learning a new language. According to researchers, you can boost your memory and improve other mental functions by becoming a student of a new language at any time in your life.
12. Take up tai chi
It’s no secret that tai chi can benefit your health in many ways, including your mental health. Plus, it can also help center you when life seems out of balance.
Taking up a regular practice of tai chi can help reduce stress, enhance sleep quality, and improve memory. A 2013 study found that long-term tai chi practice could induce structural changes in the brain, resulting in an increase in brain volume.
Beginners do best by taking a class to learn the different movements. But once you know the basics, you can practice tai chi anywhere, anytime.
13. Focus on another person
The next time you interact with someone, take note of four things about them. Maybe you observe the color of their shirt or pants. Are they wearing glasses? Do they have a hat on, and if so, what kind of hat? What color is their hair?
Once you decide on four things to remember, make a mental note, and come back to it later in the day. Write down what you remember about those four details.
Focusing on your brain health is one of the best things you can do to improve your concentration, focus, memory, and mental agility, no matter what age you are.
By incorporating brain exercises into your everyday life, you’ll get to challenge your mind, sharpen your cognitive skills, and possibly learn something new and enriching along the way, too.
If you have any questions regarding professional, safe, and loving assisted living care or professional memory care services here in Bethlehem, contact Gateway Gardens Assisted Living and Memory Care today.
7 December 2020

We found the following educational and uplifting story from the University of Utah and feel compelled to share it with you. As professional senior assisted living, memory care, and respite care support providers, we know that music has always been a therapeutical tool to enrich our dear resident’s lives. The month of December is comparatively the most music intensive month for residents and staff alike. So, we’d like to share this story with you and encourage all of you to involve music in the loving care of your family. So, now off to the wisdom of the fine folks at the Univ of Utah.
Ever get chills listening to a particularly moving piece of music? You can thank the salience network of the brain for that emotional joint. Surprisingly, this region also remains an island of remembrance that is spared from the ravages of Alzheimer’s disease. Researchers at the University of Utah Health are looking to this region of the brain to develop music-based treatments to help alleviate anxiety in patients with dementia.
“People with dementia are confronted by a world that is unfamiliar to them, which causes disorientation and anxiety,” said Jeff Anderson, MD, PhD, associate professor in Radiology at U of U Health and contributing author on the study. “We believe music will tap into the salience network of the brain that is still relatively functioning.”
Previous work demonstrated the effect of a personalized music program on mood for dementia patients. This study set out to examine a mechanism that activates the attentional network in the salience region of the brain. The results offer a new way to approach anxiety, depression, and agitation in patients with dementia. Activation of neighboring regions of the brain may also offer opportunities to delay the continued decline caused by the disease. For three weeks, the researchers helped participants select meaningful songs and trained the patient and caregiver on how to use a portable media player loaded with the self-selected collection of music.
“When you put headphones on dementia patients and play familiar music, they come alive,” said Jace King, a graduate student in the Brain Network Lab and first author on the paper. “Music is like an anchor, grounding the patient back in reality.”
Using a functional MRI, the researchers scanned the patients to image the regions of the brain that lit up when they listened to 20-second clips of music versus silence. The researchers played eight clips of music from the patient’s music collection, eight clips of the same music played in reverse and eight blocks of silence. The researchers compared the images from each scan.
The researchers found that music activates the brain, causing whole regions to communicate. By listening to the personal soundtrack, the visual network, the salience network, the executive network and the cerebellar and corticocerebellar network pairs all showed significantly higher functional connectivity.
“This is objective evidence from brain imaging that shows personally meaningful music is an alternative route for communicating with patients who have Alzheimer’s disease,” said Norman Foster, MD, Director of the Center for Alzheimer's Care and Imaging Research at U of U Health and senior author on the paper. “Language and visual memory pathways are damaged early as the disease progresses, but personalized music programs can activate the brain, especially for patients who are losing contact with their environment.”
However, these results are by no means conclusive. The researchers note the small sample size (17 participants) for this study. In addition, the study only included a single imaging session for each patient. It is remains unclear whether the effects identified in this study persist beyond a brief period of stimulation or whether other areas of memory or mood are enhanced by changes in neural activation and connectivity for the long term.
“In our society, the diagnoses of dementia are snowballing and are taxing resources to the max,” Anderson said. “No one says playing music will be a cure for Alzheimer’s disease, but it might make the symptoms more manageable, decrease the cost of care and improve a patient’s quality of life.”
As always, we remind you that for anyone out there with questions regarding professional senior assisted living care here in Bethlehem, memory care services, or respite care services here in Bethlehem, reach out to us anytime!
Credit for this work goes to: The University of Utah’s K.G. Jones, M. Rollins, K. Macnamee, C. Moffit, S.R. Naidu, E. Garcia-Leavitt, R.K. Gurgel, J. Amaro and K.R. Breitenbach at U of U Health and University of Utah, E. Goldberg from the Jewish Family Services of Utah, J.M. Watson from University of Colorado and M.A. Ferguson from Massachusetts General Hospital also contributed to this project. This work received support from A. Scott Anderson and the American Ontological Society.
30 November 2020

Whether you’re a cherished resident at Gateway Gardens Assisted Living & Memory Care here in Bethlehem, a family member, or a valued fan of our blog, we trust you had a great Thanksgiving Holiday and are looking forward to the magic of the entire Christmas Holiday season. But it is winter, and winter can be a challenging time to remain physically active. We’re going to address this challenge in today’s blog post.
In winter, staying active becomes increasingly hard to do. Between preparing for the Holidays and the higher likelihood of severe weather, our walking groups tend to part ways until the next spring season. As the opportunities to get outside grow limited, unless you are an avid fan of the cold, the amount of exercise you get can plummet. However, there are several easy and fun ways we can remain active during the upcoming colder months!
Chair yoga is a fun and easy way to stay active indoors. Never tried yoga? No problem! Chair Yoga adapts many of the more complex positions into accessible movements for beginners. Yoga has many health benefits, such as improved balance, mindfulness, and agility. As we are gearing up for winter, chair yoga is the perfect routine to help stay warm in the cold months ahead.
Exercise doesn’t always have to be accomplished in workout clothes. Dancing is an excellent form of exercise as it builds muscle strength, balance and coordination as well as heart health! The best part is that dancing can be done on your own or with a group of friends. All you need are a few of your favorite tunes and some dancing shoes. Did you know that in addition to being a great form of cardio, dancing can even improve your memory? A recent study in the New England Journal of Medicine cited that dancing could prevent the development of dementia as we age.
With so many great reasons it’s hard not to want to move those couches to the wall and hang up the disco ball!
Before you head outdoors this winter, remember to do a few quick arm and leg stretches. Snow and ice can obviously be slippery but warming up your muscles before you head out in the elements can do wonders for your balance as you walk across the icy bits. You should also take water with you. Unpredictable weather and increased exertion against wind and snow increase the likelihood that you are outside for longer than expected.
The extra layers we put on to keep warm make us sweat, which means we need to up the intake of water we drink in the day. Drinking cold water in cold weather isn’t enticing, so keep a few water bottles out until they become room temperature!
No matter what kind of activity you choose, it is important to remember that safety should always come first. Staying hydrated during the winter is particularly essential since all the extra layers can make your body sweat more than usual. Also, stretching before heading outdoors will decrease your likelihood of falling on the icy sidewalks.
Managed healthy and safe activities within our assisted living community here in Bethlehem, our memory care community, and within our respite care services is a source of great pride for us here at Gateway Gardens. Come see it for yourself. Contact us anytime!
9 November 2020

When it comes to happiness later in life, there is one factor that countless studies show is key for most people: Social connection. More important than money or one’s past career success, research from around the world shows people need social activity to genuinely enjoy their “golden years.”
Keeping active and engaged is important at any age, but for seniors, it is vital. When it is time to think about living arrangements for the latter part of one’s life, it’s so important to consider how various communities do or don’t foster those social connections. We’re certain you’ll find that Gateway Gardens Assisted Living & Memory Care here in Bethlehem will pass all your tests.
Happiness and connection are tied to physical health as well. For example, one study looked at 1,110 seniors without dementia. Their social activity levels and cognitive functioning were measured over 12 years, and the results were amazing. Those seniors with a higher level of social activity had a rate of cognitive decline that was 70% lower than those with less social activity. Studies also show that happier senior citizens live longer.
The problem is that many seniors find themselves without those social connections. Over the years, family and friends move away and pass away, and opportunities for connection dwindle as people retire from jobs and their children leave home. Lives that once bustled with business and social activity can become quiet and lonely.
Fortunately, there are senior assisted living communities like ours that foster social connections and help keep seniors engaged, connected and happy. Whether you or a loved one seek professional assisted living services here in Bethlehem, professional memory care services for a loved one in or around Bethlehem, or professional respite care services here in Bethlehem, Gateway Gardens is here for you.
We provide living arrangements that give seniors both the level of autonomy they want and the support they may need. Amenities like chef-quality meals served three times a day and weekly housekeeping services mean there is more time to engage in activities, develop new friendships and spend time with family. An array of activities and opportunities promotes an active lifestyle and lets seniors pursue their passions and explore new interests.
For more information, please browse our Gateway Gardens Assisted Living & Memory Care website.
2 November 2020

Getting swept up on a great television series can make us laugh, provide a shared interest with others, or simply forget our worries for a little while. Streaming services, like Netflix, Hulu, Amazon and Disney+, offer an enormous variety of options for television (as well as movies) but it might seem like these services target only younger people. In fact, seniors are likely to find many shows they enjoy. We’re here to help by recommending a few streaming TV shows for older adults.
Note that some of these shows air on network television or cable, but can be watched using streaming services for more choice and flexibility.
For our assisted living community residents here in Bethlehem, the need for readily accessible entertainment, like a streaming service, is important, especially when:
Unlike “regular” television, streaming services allow someone to watch an episode or two whenever it’s convenient. Many seniors like the ability to pause for short breaks or rewind if they miss something. They can even make plans to watch a show at the same time as a friend or family member, to share the experience.
There’s also evidence that our memory care residents here at Gateway Gardens Bethlehem can benefit from the social context of watching TV with people who are close to them.
The term “scripted television” came into fashion to differentiate shows that tell stories from reality shows. Scripted shows include comedies or dramas or, increasingly, a mix of the two. Comedies are an especially good choice for when it’s time to unwind. A 2014 research study even concluded that “laughter therapy” improves the general health of seniors.
One of the biggest changes streaming television has brought to the industry is diversification of stories and characters. There is more representation than ever of different ages, abilities, ethnicities, gender identities and other traits. Gone are the days when most senior citizens on television were caricatures — the overbearing mother-in-law or the cranky next-door neighbor, for example. Senior adults are more often portrayed on TV as having rich inner lives with hopes and dreams as well as flaws. The following are just a few examples.
Many popular streaming series are set during different time periods, often with no expense spared with regard to sets, costumes and music.
Game shows and reality competition shows can provide excitement, humor and insight into different hobbies and interests. These are some popular ones.
Sometimes the “best” television shows are the ones from our youth. From I Love Lucy (Hulu) to Star Trek (Netflix), any classic show you ever loved probably lives on a streaming service now. Watch it again in its entirety or just your favorite episodes.
You can always talk to friends and family for additional show recommendations, but we think some of these will give you a starting point to find your new favorite streaming TV series. Here at Gateway Gardens, our goal is to meet the needs of all our residents, from their medical care to the little things they enjoy doing each day. Get in touch to learn more about life here at Gateway Gardens Assisted Living and Memory Care here in Bethlehem.
26 October 2020

Today we hope to educate all our Bethlehem-area assisted living and our Bethlehem memory care community residents, family, neighbors, and friends on the subject of healthy sleep. Sleep disorders affect people of all ages, but they become more prevalent during your senior years, putting you at risk for a range of other mental and physical health issues. Today’s blog is intended to educate and provide some things to consider, but with that said, we need to make something clear. As it pertains to any and all health-related topics, your medical team is (and always should be) your final source for guidance.
While occasional sleep problems are common, insomnia or other abnormal sleep behaviors are a cause for concern. You can help combat them by identifying the root cause and implementing various natural remedies and routine changes.
It is common knowledge that a chronic lack of quality sleep can negatively affect your physical, mental, and emotional health. During sleep, the body has a chance to repair cell damage and refresh the immune system, subsequently building up your defense against disease and sickness.
For older adults, insufficient sleep puts them at higher risk of depression, anxiety, and memory problems. Additionally, you or your loved one may become more susceptible to daytime sleepiness and nighttime falls. Other more serious conditions that may result from insomnia and other sleep disorders include an increased risk of diabetes, cardiovascular disease, and breast cancer.
In order to improve your quality of life, it’s important to get a good night’s rest on a consistent basis. If you are struggling to get a good night’s sleep, then consult your doctor. You, your doctor, and your family should team together to identify the underlying problem and then applying the appropriate treatment.
In general, adults function best when they get an average of seven to eight hours of sleep each night. It is normal for your body’s internal clock to evolve as you age, causing you to feel sleepy earlier in the evening or to wake up earlier in the morning. Additionally, lower levels of growth hormone production lead to a decrease of slow-wave or deep sleep, resulting in less melatonin and more fragmented sleep.
However, there are a variety of more severe sleep disorders that can negatively impact your ability to feel truly rested. Insomnia, or difficult falling and staying asleep, is the most common, but seniors can also suffer from other sleep-related issues. Some of the main causes of sleep disturbances or insomnia in older adults include:
If you want to improve the amount and/or quality of sleep you are getting, you must treat the underlying problem. For certain root causes—such as pain, medical conditions, or your medications—you should speak to your physician about making changes to your treatment plan. They may also recommend specific solutions to your sleep disorder.
In general, however, there are several preventative measures and routine changes that may help counteract the common causes of insomnia or sleep impairment in seniors:
If you or your loved one struggle with sleep issues, talking with your doctor is a good place to start. Our assisted living and memory care community here in Bethlehem is designed to support our senior residents by providing a safe, secure environment where their everyday needs are met. We not only offer comfortable housing accommodations but also indoor and outdoor amenities, events, and fitness programs to keep you physically and mentally active during your senior years. We are proud to deliver professional assisted living and memory care services that measurably improve quality of life.
We welcome your call and/or visit to learn more. Contact us today!
12 October 2020

Greetings once again to all of our Bethlehem-area assisted living and our Bethlehem memory care community residents, family, neighbors, and friends. We’re entering flu season here in Bethlehem, and while most focus today is rightfully centered on COVID, you simply must address the dangers of flu season and what you need to do now!
As people around the world continue focusing on the COVID-19 crisis, the time of year when the seasonal flu begins to make its rounds is approaching. It’s important not to overlook the safety measures designed to protect us all from the influenza virus. Compared to the severity of the coronavirus, the flu may not seem as serious of a health risk. The reality, however, is that the seasonal flu can still be deadly for seniors. In fact, seniors comprise nearly 85 percent of influenza-related deaths and up to 70 percent of hospitalizations in a typical year.
The annual flu vaccine is considered to be the gold standard when it comes to prevention, but it’s not the only one. Lifestyle also plays a key role in determining who will—and who won’t—get bitten by the flu bug.
These last few recommendations are likely ones you’ve heard frequently since the COVID-19 pandemic began, but they bear repeating:
Finally, contact your physician at the first sign of the flu. There are prescription antiviral drugs that help lessen the severity of flu symptoms and may even be able to shorten the length of time you are sick. But these medications must be taken before the flu progresses too far.
We exist to add quality of life to both you and your beloved. People turn to us daily for advice and consult. We’re here for you! Contact us today to schedule a tour!
28 September 2020

Welcome back to our blog page for our Bethlehem-area assisted living and our Bethlehem memory care community. No matter what stage of care need your elderly loved one is at, you can trust that you have proven professionals right around the corner here at Gateway Gardens Assisted Living & Memory Care to deliver genuine quality of life improvement to you both. Today, let’s visit the subject of heart health.
The heart is obviously a foundational muscle and the moment its integrity is compromised, or it starts to fail in some way, our bodies react. Just like with the brain, there are so many smart ways that we can go about keeping our hearts healthier as we age. We’re going to look at proactive heart health, why it’s important, and the best ways to keep our tickers going strong.
According to the heart foundation, heart disease is the number-one killer of Americans and each year, it claims more lives than every form of cancer combined. Heart disease, including all forms of strokes and cardiovascular diseases, kills hundreds of thousands of people every year. With so many deaths annually, it’s important to note the most common reasons our hearts give out on us.
When it comes to the health of our hearts, some habits are better than others. According to Harvard Medical School, there are five habits that can be extremely destructive to the heart. They are:
If any of these things apply to you, you could be doing your heart a huge disservice, but it’s never too late to make valuable changes to your health! Reach out to us to learn more about our proactively managed heart health activities!
In the meantime, check out our community’s accommodations and reach out to us if you’d like to learn more about assisted living and/or memory care services here in Bethlehem. We exist to make your life easier, your elderly loved one’s existence better, and your family’s quality of life the best it’s ever been. Contact us today to schedule a tour!
21 September 2020

Helping your parent or a loved one make the move to professional assisted living care here in Bethlehem or professional memory care here in Bethlehem can be overwhelming for all involved. However, there are steps you can take to make the transition as easy and comfortable as possible. The key is thinking ahead and taking a little extra time to plan. Here are five essential tips to keep in mind as you prepare.
Once a community is selected, it’s time to create a road map for the move itself, including what items will be stored or sold and identifying logistics and costs for moving day. Gather important personal information such as Social Security and Medicare information and legal and financial records, so that all critical information is at your fingertips. If you have time, it’s also a good idea to schedule visits to the community with your loved one in advance of the move so that their new home starts to become familiar and comfortable even before they move in. Schedule a lunch or check out the community’s daily calendar for special programs or events to help break the ice and get to know residents and staff members.
During all that has to be done, keep in mind that this is a big change for your parent or loved one. Approach the discussion with dignity and respect, and with the understanding that your loved one will be a primary decision maker during this transition. Read the signs and ask thoughtful questions to explore concerns or fears that may lead to a larger and more honest discussion. If your loved one is asking pointed questions, then find out what the underlying concern may be. Gently enter the discussion so that you can discover how best to provide support in a way that is comfortable for them.
Sorting through treasured items can be a serious undertaking. As you go through a lifetime of belongings, we recommend familiarizing yourself with their new accommodations. You’ll want to pack the essentials, but also look for ways to make their new space feel like home. Help your loved one identify some key items that are emotionally significant to them, like a favorite art piece, family photos, or a treasured keepsake. Carefully consider which rooms your family member regularly occupies and the items they touch most to gauge what their needs will be in their new place. For example, if they are no longer entertaining regularly in their home, then they can probably leave the china cabinet behind, but may want to bring a favorite teapot or coffee mugs for cozier encounters. Most importantly, include your loved one during each step of the process – choosing things for the new place will help them feel more at home when they arrive.
Any move can be difficult, especially if you are managing it by yourself. Gather a support team of family and friends. If someone offers to help, let them! Identify a team leader and key decision maker, then delegate tasks such as canceling utilities, scheduling movers and packing boxes. If you find yourself in a bind, don’t hesitate to talk with the staff at the community – they’ve helped lots of families in the same situation and can offer advice and support, along with helpful resources for the big move.
Although it is important to support your loved one through this significant transition, it is equally important to give them time and space to adjust to their lifestyle change. Independent living can offer seniors more opportunities to remain self-sufficient by providing services like transportation, an on-site fitness center and salon, daily social activities and delicious dining options. Assisted living provides the added security of licensed nurses and a well-trained staff around the clock, while also helping your loved one to be more socially active by offering activities and outings that may not have been available to them at home. Here at Gateway Gardens Assisted Living & Memory Care (Bethlehem), we ask families to provide a life story upon move-in so that we can get to know new residents and their interests more quickly and introduce them to activities and people they might enjoy. Our team can offer guidance to help you find the right balance of support and independence for your loved one at their new community.
If you have specific questions or need help in planning your loved one’s move, get in touch with a member of our highly trained staff for more information on how to prepare your loved one for their new home.
14 September 2020

We routinely receive finance-related questions while providing professional assisted living services here in Bethlehem and loving memory care services in Bethlehem as well. A commonly asked question pertains to whether or not establishing joint bank accounts between seniors and their family. We want to recognize “A Place For Mom” who authored great guidance on this subject that we share with you today.
So, are you considering opening a joint bank account with an aging parent? While it may seem like a convenient way to pay the bills, a joint account has drawbacks that could be financially damaging to you both. Weigh the pros and cons here before heading to the bank.
A joint bank account is an easy way to assist your aging parent with managing day-to-day finances. Having a joint checking account can help you:
Depending on your financial situation, the decision to combine accounts could be detrimental to both you and your parent. Here are some risks to consider before opening a joint account with your elderly loved one:
Money is the main reason adult siblings fight over their parent’s care, and joint bank accounts can lead to disputes. If one sibling is a primary caregiver, or helps their aging loved one pay bills, it may seem sensible for them to take over an elderly parent’s finances or to set up a joint account.
But siblings could question how and why money is being spent, says Mike Travers, a certified financial planner in Ontario, Canada. They may accuse the joint account holder of financial abuse, especially if the funds appear to be misappropriated. “Parents need to be mindful of what they may set their children up for,” says Travers.
In families with multiple children, a joint checking account with one child has consequences regarding inheritance. “In most states, upon the parent’s death, the money in the account automatically goes to the child whose name is on the account, thereby disinheriting the other children,” writes Takacs. This is because joint accounts are usually held with rights of survivorship, which means ownership passes automatically from the deceased to their survivor.
A joint account can preclude a will in the case of your loved one’s death, no matter when the account was established. This means the child on the shared account would receive all the money in the account.
The FDIC guide to joint bank accounts provides a potential solution: “While most joint accounts are held with rights of survivorship, in rare instances joint account owners are ‘tenants in common,’ which means ownership does not necessarily pass from decedent to survivor. Instead, each co-owner can bequeath his or her share of the account to whomever he or she chooses.” With this provision, the aging parent could assign their share of the account to a separate child, ensuring it’s split evenly. Consult a financial advisor to see if this provision could apply to your family.
If the risks of a joint bank account outweigh the benefits in your family’s circumstances, consider these alternatives:
Every family’s financial situation is different. Consider consulting a certified financial advisor to understand how to best help your elderly parents. Visit the Certified Financial Planner Board of Standards to search for one by city, state, or ZIP code. Certified elder law attorneys are often also experts in financial issues related to aging. Visit the National Academy of Elder Law Attorneys to find one in your area.
Before selecting an advisor, ask about their experience with elderly finances. Registered financial gerontologists have extra training in providing financial advice to aging adults and their families. In addition, some geriatric care managers offer financial advising or can link you with an advisor who specializes in elder-care finance.
Please know that our professional expertise is in providing assisted living and memory care services. We are not financial advisors, however, we view this as prudent guidance that helps your formulate questions and concerns that you can direct to a qualified financial consultant. As always, we stand ready to answer any and all questions you might have regarding the benefits of professional care services. Call anytime!
31 August 2020
We witness and understand that there are certain stresses involved in visiting the doctor and the dentist. We discovered some very practical advice provided by Dr. John Voytas, M.D., a Doctor of Geriatric Medicine. He focuses on preparation for the visit and how it can make things go so much more comfortable and effective for the patient, family, and providers alike. All of us here at Gateway Gardens Assisted Living & Memory Care (Bethlehem) thank Dr. Voytas and the great folks at Graceful Aging for putting together this short presentation that we trust you will find useful.
Please know that we manage this blog as a free service to help all of you, like us, who provide loving assisted living and/or memory care services for a loved one. Also know that we stand ready to answer any and all questions you might have regarding the benefits of professional care services. Call anytime!
24 August 2020

Our team of professional memory care and assisted living care providers here at Gateway Gardens here in Bethlehem are there for all of you at home care providers. Much of our blog is dedicated to works designed to assist you in your selfless commitment to your senior loved ones. Unfortunately, there will come a day when solo home care or professionally assisted home care is no longer enough. For those of you who have arrived that moment, please know that your friends here at Gateway Gardens Assisted Living & Memory Care are ready with open arms to provide the loving care necessary to deliver the quality of life that both you and your challenged loved one(s) deserve. So let’s start with the basics.
Everyone ages differently. While some age-related changes are inevitable, such as slower reflexes and vision challenges, other issues can vary greatly from person to person. Lifestyle and to a lessor degree, genetics, are key determinants in how healthy you are at every age.
This is important information to keep in mind as you search for a senior living community, whether for yourself, a spouse or aging parents. It might be that a senior is active and independent at the time of a move, but what happens when needs change?
Moving is tough at every age, but more so for older adults. This is why making a second move during the retirement years is something to avoid if possible. Understanding what types of care a senior community offers and what happens if care needs change over time are important issues to address before making a decision to relocate. This includes if one parent needs more or different care than another.
If you aren’t familiar with different types of senior care, this quick overview might be helpful:
At each community you visit, ask the staff about how they handle changes in needs after a senior becomes a resident. Are different types of care available on the same campus? Can residents move from one to another seamlessly?
When you are weighing options for yourself or your parents, choosing a community that offers multiple levels of care is something to consider. If one person develops different care needs, a couple can still remain a part of the same senior community. Even if these changes require separate living arrangements, they will still be in an environment that is familiar to them surrounded by team members they know.
Now is the time for you to seek a consult regarding how Gateway Gardens Assisted Living & Memory Care here in Bethlehem can improve the quality of both you and your loved one’s lives. Call us!
17 August 2020

We often hear horrible stories from families concerning an elderly loved one who was short-changed or downright scammed, financially or otherwise. Our caring professionals here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care focus this blog post on the topic of con-artists and scammers of all stripes. While this blog post is geared towards the senior community, it is certainly germane and relevant to folks of all ages. It certainly applies to all of our faithful blog readers whether your providing assisted living and/or memory care support. So let’s discuss the very real risks out there.
Safeguarding your money, your assets and your identity from theft and fraud.
Con-artists come in different shapes and disguises, but the objective is always the same!
This clever actor charms elderly victims by phone with an affable “nice guy” approach. Deceptive and dishonest, this tele-trickster is the last person you would want to invite into your home! You’re right if you guessed… he’s a con artist!
According to the U.S. Congress, Americans lose an estimated $40 billion each year due to the unethical activities of fraudulent “salespeople.” Con artists will try to take money as well as property and other valuable assets. Sweepstakes tend to be the most prevalent of all con artist scams but they might also be disguised as home improvement deals, real estate investments, inventions, or even false charities. Knowing how to spot these scams will help you identify a con artist and may someday save you from heartache and financial disaster.
Most people are not likely to fall for a scam if it actually sounds like one, so these phony deals are usually disguised as something else:
Most con artists use key words and phrases to make you feel important or to pressure you to act quickly. For example:
“You have been selected as one of ten finalists for our sweepstakes offer.”
“As a senior citizen, you have already been pre-approved.”
“This is not for every one, so keep it a secret.”
“Cash or credit card only, no checks.”
“You must decide now. If you hang up, you will lose this opportunity.”
The object of any con game is to get you to part with your money. Most of these scams are initiated by people who approach you on the street or call you at home. Be suspicious of ANY plan, idea, scheme, or so-called business deal that requires you to give money – or access to your money – to a stranger. Here are some of the more common scams:
The Bank Examiner
Someone calls you claiming to be a bank examiner or police investigator who needs your help to catch a “dishonest” bank employee. He usually asks for your account number and account balance. He may tell you that the bank records show a much smaller balance and that he suspects a teller must be stealing the money. He asks you to withdraw a large sum of money from your account and give it to him so he can do an audit or check serial numbers, after which the money will be re-deposited. Of course, you never see him or your money again.
Door-To-Door Sales
Often times con artists will try to get you to subscribe to a magazine or offer a cure for a medical condition. They may also offer a free inspection of your home for problems with your furnace, hot water tank, appliance, or garage door. Whatever the con artist has to offer, simply say no and report them to your local police. More than likely they need to have a solicitor or business license of some type from your local city hall in order to conduct such door-to-door business. The con may even have an I.D. that appears to have been issued by your local government office. Check it carefully.
The Fake Lottery Ticket
Someone with a foreign accent approaches you on the street and tells you he has a winning lottery ticket, worth $100,000 or more, but he cannot cash it in because he is not a U.S. citizen. He even verifies the winning numbers by calling a number and letting you listen to a phony recording of winning lottery numbers. He offers to sell you the ticket for just a few thousand dollars. You jump at the chance to make such easy money and help someone out at the same time. Of course the lottery ticket is worthless and you have lost your money. (Someone close to me actually fell prey to a similar scheme.)
Home Improvement Scheme
A man drives up to your house in a commercial van or pickup truck, dressed in workman’s clothing. He tells you he has just finished a large roofing job (or driveway resurfacing, etc.) and has some materials left over. He tells you he will use the leftover materials to repair your roof, driveway, or other repair work, at a large discount. If you agree, he will do a quick, shoddy job with cheap material.
The Phony C.O.D. Scam
The con artist will scout a neighborhood to find an unoccupied home, then check a city directory to find out the homeowner’s name. Armed with this information, he will fill out a phony shipping label and apply it to a box of rocks or other junk. Returning to the house dressed as a delivery man, he will knock or ring the bell, properly setting the stage for his next act. Getting no answer, he will go to a neighbor, you, and ask that you accept the package and pay the C.O.D. fee.
Credit Card Fraud and Stolen Identities
These days you have to be especially diligent in safeguarding not just your credit cards, but your identity as well. It is very easy for a criminal to steal your good name and then proceed to destroy it, leaving you with a pile of debts and scores of angry creditors. Identity thieves often search through people’s garbage to find what they need to assume your identity. Even something as innocent as old discarded phone or utility bills can put you at risk. Con artists use these documents to obtain a phony ID with your name and their picture. Then, they can go all over town applying for credit cards in your name and running up big bills. Thieves also steal from mailboxes. New checks and credit cards are favorite targets. Also, if you leave bill payments out for the mailman to pick up, this mail can be stolen and your checks “washed” to remove dollar amounts and payee information. Your signature is left untouched. The crook then makes the check out to a phony name for a much higher amount and cashes it.
The Funeral Chaser
Shortly after a relative dies, someone delivers a product to your door that the deceased allegedly ordered before his or her death. You may even get a bill for an expensive item along with a request to make the final few payments. This scam artist uses newspaper obituaries to prey on bereaved families. Please understand that you are not responsible for anyone else’s purchases. If a claim is legitimate, the estate will settle the matter.
Medicare Number Theft
Since many seniors rely on their Medicare health insurance, it’s no surprise that many elder fraud scams originate from that source. Often, fraudulent medical equipment companies offer free supplies to unsuspecting seniors in return for their Medicare numbers. However, the patient’s doctor is required to order and sign for all equipment and products before Medicare will pay for them. The most important tips when it comes to spotting health insurance fraud include:
You do have choices
If the sweepstakes offer, deal or business opportunity sounds too good to be true, your instincts are probably correct. If you’re not interested, hang up the phone! However, if you believe an offer is legitimate, take steps to protect yourself and those close to you:
If you have any questions or concerns regarding how to provide fraud free loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Bethlehem.
3 August 2020

We appreciate the positive feedback from all of us here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care regarding the practical utility of our blog. It is now August and the increasing heat index can be deadly for the young and senior alike. The safety of our cherished residents in our top concern, and it should be for all of you at-home care givers as well. We feel a heartfelt responsibility to freely share our professional knowledge regarding professional assisted living , memory care, and respite care services. So today, we’ll talk about the uber-importance of senior hydration and leave you with some ideas of how to keep your loved one safe.
Summer provides opportunities to enjoy the great outdoors. After a long winter stuck inside, a lot of people look forward to it. From picnics and barbecues to outdoor concerts and beach trips, many people spend summer largely outside. For older adults, however, summer presents unique health risks. One is dehydration. While heat and humidity can be a dehydration or heat stroke threat to people of all ages, older adults are especially vulnerable.
Sometimes the increased risk is caused by a medical condition that weakens a senior’s sense of thirst. Other older adults have problems adjusting to temperature changes. Their bodies don’t produce the sweat they need to cool down. Taking extra steps to stay hydrated during the summer is important.
The Centers for Disease Control recommends adults consume 48–64 ounces of fluid each day. If you are outdoors in the heat, you should consume even more. Fluid can come in the form of fruit and vegetable juices, soup, water, and milk. While sodas and coffee are liquids, many health professionals say they shouldn’t be counted in your daily total. If they contain caffeine, which is a diuretic, they can increase the risk for dehydration.
These tips can help seniors stay hydrated:
Our final tip is to limit consumption of alcohol on hot days or when spending time outdoors. Like caffeine, it can cause fluid loss that increases the chance for dehydration.
It’s also important to learn warning signs that could indicate the early stages of dehydration. They include:
If a senior you are the caregiver for is exhibiting these symptoms, call the doctor or seek treatment at an urgent care center or a hospital emergency room. The older adult might need IV therapy to restore fluid levels.
If you have any questions or concerns regarding how to provide both loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Bethlehem.
13 July 2020

Hello once again from our team of Bethlehem-area assisted living and Bethlehem-area memory care professionals. Since it is dangerously hot outside these days, you all are probably looking for things to do inside to have some fun and beat the heat. Today we thought it might be inspiring to consider our list of “Inspiration Women over 60” to introduce to you some uplifting introductions and to inspire you to research further about any of these inspirational women that you find particularly interesting.
So, here you go. Twenty inspirational women over 60:
Many of these women have been pioneers in their careers. Some are less well known, while some have made it into the history books. Some of them are no longer with us, while others continue to make incredible strides. All of them, however, inspire us to live our best lives.
1. Iris Apfel, 97
She’s been called unique, iconoclastic and a “rare bird.” The subject of a brand-new documentary entitled “Iris,” Iris Apfel has spent the last 60-odd years as a legendary designer of jewelry and clothing, as well as an interior designer who has consulted for nine presidents at the White House. At age 84, she and her designs were the subject of an exhibition at the Costume Institute of the Metropolitan Museum of Art, and at age 90 — just a few years ago — she inspired a line of MAC cosmetics.
2. Ruth Bader Ginsburg, 85
Supreme Court Justice Ruth Bader Ginsburg was, of course, only the second female justice in United States history, nominated in 1993 at the age of 60. She continues to serve on the Supreme Court and influence key decisions furthering the rights of women, and she has been on the Forbes list of “100 Most Powerful Women” as well as the subject of the popular Tumblr blog Notorious RBG celebrating her judicial accomplishments as well as her status as an inspirational part of women’s history.
3. Debbie Allen, 68
Debbie Allen will be a familiar face to anyone versed in the world of dance and choreography over the past several decades. Though this former Broadway star and member of the President’s Committee on the Arts and Humanities is best known for her work on Fame — not only the original film but the TV series and 2009 remake — she’s also been a TV and stage producer, a judge since 2007 for So You Think You Can Dance, and founder of the Debbie Allen Dance Academy for youth in Los Angeles, California.
4. Joan Rivers, 1933-2014
This sharp-tongued icon of comedy was the first woman to host a late-night talk show on network TV, “The Late Show with Joan Rivers,” which debuted in 1986 when she was already 53 years old. In 1989, she went on to host a daytime talk show, which would run for four more years, and appeared on a number of other cable TV shows on fashion and entertainment. She wrote 12 books, received a Grammy nomination, and contributed to a number of philanthropic causes. By the time she died in 2014, she was known as one of the greatest trailblazers for female comedians.
5. Joan Ganz Cooney, 88
Joan Ganz Cooney might not be a household name, but her accomplishments have definitely reached countless households: as the founder of Children’s Television Workshop, which produced “Sesame Street” and “The Electric Company,” Cooney has received numerous Emmy Awards, including the Emmy for Lifetime Achievement in 1989. She has received the Presidential Medal of Freedom, she’s been inducted into the Academy of Television Arts & Sciences Hall of Fame, and in recent years, her innovations in children’s programming have inspired various literacy and learning programs named in her honor.
6. Georgia O’Keeffe, 1887-1986
Georgia O’Keeffe is one of the 20th century’s best-known painters, famous for her lush close-up depictions of plants and flowers as well as her images of Southwestern landscapes. The wife of pioneering photographer Alfred Stieglitz, O’Keeffe continued producing art in various media, including drawing, painting, and later, sculpture, until two years before her death at age 98.
7. Tao Porchon-Lynch, 100
Tao Porchon-Lynch has been an actress, a model, a dancer, a wine expert and she’s set a Guinness World Record for the oldest yoga instructor. Born in India, this sometime winner of the title “Best Legs in Europe” has traveled the world, meeting luminaries like Mahatma Gandhi, Charles de Gaulle, and Martin Luther King, Jr. She became a full-time professional yogi in 1967, and has continued to do yoga (and dance) throughout her life, releasing a yoga DVD as recently as 2013. In “The Imperfect Environmentalist” by Sara Gilbert, Porchon-Lynch was quoted as saying, “I’m going to teach yoga until I can’t breathe anymore.”
8. Dr. Ruth Westheimer, 90
Although Dr. Ruth Westheimer has long been an advocate for safe, healthy and enjoyable sex, it wasn’t until she reached her mid-50s that she became known for her frank, down-to-earth advice via her radio show: “Sexually Speaking.” Since then, she has continued to educate the public through television, magazine and newspaper columns, books, teaching college classes, and providing advice on her website — and she continues to operate a private practice in sex therapy. She has won countless awards, including Honorary President of the Council on Sexuality and Aging.
9. Jacquie “Tajah” Murdock, 87
This former Apollo Theater dancer and Harlem native is not only smart and educated (she holds a master’s degree from NYU), she continues to be a fashion icon well into her 80s. She’s always had a love of fashion, and the glamour of movie stars like Marlena Dietrich and Lena Horne inspired her to create a unique style of her own. She was recently featured in the documentary Advanced Style, about older New York City women who still rock the fashion world. In a recent interview with Soul Train, she said, “I want older women to know that there is life after the ages of 50 and 60. I want them to know that you must be active — you cannot just sit there and twiddle your thumbs. They should keep active, do something they like and get involved because life is for the living.”
10. Aung San Suu Kyi, 73
Suu Kyi is Burma’s best known opposition politician, and the chair of the National League for Democracy, working tirelessly over the last 25 plus years on behalf of non-violence, peace, human rights and democratic rule in Burma, despite spending almost 15 of those years under house arrest by the existing government. She has received numerous international accolades for her efforts, including the Nobel Peace Prize and the Presidential Medal of Freedom, and as of 2014 was listed by Forbes as the 61st most powerful woman in the world.
11. Beatrice Wood, 1893-1998
Wood, a ceramic sculptor and sometime actress, died at the astonishing age of 105 after becoming known as the “Mama of Dada” and a compatriot of many of the key figures of modernist art. Anais Nin, Man Ray and Marcel Duchamp are just a few of the avant-garde artists in her circle of friends. At the age of 90, she added “writer” to her list of artistic accomplishments, publishing her autobiography entitled: “I Shock Myself,” in 1985. Regarding her longevity, she said, “I owe it all to chocolate and young men.”
12. Alice Waters, 74
Alice Waters is the founder of one of America’s most renowned restaurants, Chez Panisse, and is credited for inspiring California cuisine as well as being the first woman to win the James Beard Foundation’s Best Chef in America award. After pioneering the use of fresh, organic, and local ingredients in her Berkeley, California, restaurant (founded in 1971), Waters went on to write several cookbooks, consult on school lunch reform, and train many younger chefs to celebrate healthy food ideals.
13. Annie Leibovitz, 68
This well-known entertainment photographer has taken many of the last century’s — and the current century’s — most iconic pictures of celebrities, including the famous photograph of John Lennon and Yoko Ono in a bed, taken on the day Lennon was murdered in 1981. She’s photographed everyone from Lady Gaga to Queen Elizabeth II to Benedict Cumberbatch.
14. Bernadette Peters, 70
Another showbiz great, Bernadette Peters has starred in musicals, films, and television shows since the 1960s, and is still going strong — just one of her recent accomplishments was a Grammy Award for Best Musical Theatre Album in 2004. While my own generation might know her best as Lily St. Regis from the 1982 movie Annie, it was her role in 1974’s musical Mack and Mabel that catapulted her into the spotlight. Most recently, in addition to continuing her performances on stage and screen, she’s also begun writing children’s books, and contributes to many charitable causes.
15. Jane Goodall, 84
After 55 years of studying chimpanzees in the Gombe Stream National Park, Tanzania, Jane Goodall is considered to be the world’s leading chimpanzee expert. She’s been the subject of films and books for both children and adults, the recipient of dozens of awards, and in her later years, continues to be an activist on behalf of animals and the environment. Oh — and she’s even been the grand marshal of the Tournament of Roses Parade, in 2013.
16. Katharine Graham, 1917-2001
A pioneering journalist who President George W. Bush called “the beloved first lady of Washington and American journalism,” Graham led the Washington Post newspaper to prominence during the publication of the Pentagon Papers in 1971 and the Watergate scandal in 1974. She took over the company in 1963 at the age of 46 and didn’t leave until 1993; during that time, she became the first woman to lead a Fortune 500 company and to serve as director of the Associated Press. Her memoir, written in 1997, went on to win a Pulitzer Prize for biography.
17. Sister Madonna, 88
It isn’t surprising to hear that someone who has earned the moniker “the Iron Nun” wouldn’t show any signs of slowing down even at age 84. Spokane nun Sister Madonna Buder competed in her first triathlon at age 52 and since then, has competed in nearly 50 Ironman events and over 325 triathlons worldwide. Just this past month, she was dubbed the Ironman All World Athlete Champion for her age group — of course, because of her age, the Ironman organization keeps having to create new age brackets for her to compete in!
18. Olga Kotelko, 1919-2014
Another star runner, Canadian athlete Olga Kotelko‘s real athletic career began after her retirement from a 30-year teaching career. A baseball player in her youth, she took up slow-pitch softball and, in her 70s, started training in track and field, eventually earning the distinction of oldest female high jumper in history. She’s broken world records and won dozens of awards. Scientists have even studied her amazing physical fitness levels, the results of which inspired the 2014 book: “What Makes Olga Run?: The Mystery of the 90-Something Track Star and What She Can Teach Us About Living Longer, Happier Lives.”
19. Vivienne Westwood, 77
English fashion designer Vivienne Westwood is perhaps most famous as the co-creator (along with Malcolm McLaren) of the punk and new wave style, including all those safety pins, spiked collars, and bike chains. She continues to design clothing for the catwalk and for notable entertainment clients including Pharrell Williams, whose iconic hat was in one of her 1980s collections. She is also an activist for a number of civil rights and environmental causes.
20. Maya Angelou, 1928-2014
A prolific, influential writer and the author of internationally recognized autobiography I Know Why the Caged Bird Sings, Maya Angelou has been known and respected as a spokesperson for women and people of color throughout her life, giving lectures and readings well into her 80s. She published poetry, essays, and an impressive seven autobiographies, the most recent of which was published in 2013. In 1993, she recited a poem at Bill Clinton’s presidential inauguration, and during the later 1990s and 2000s, she continued to be active by collaborating with R&B artists, creating a line of Hallmark cards, and campaigning for the Democratic party.
As always, if you have any questions or concerns regarding how to provide both loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Bethlehem.
6 July 2020

In our continuing effort to support those of you who lovingly support your senior loved ones, our team of Bethlehem-area assisted living and Bethlehem-area memory care professionals thought it would be wise to share eight facts you should know about summer and senior care. We want all of you at-home care providers to fully understand that older adults are especially susceptible to heat-related injuries and heat stroke.
So, please consider and take heed knowing that:
If you have any questions or concerns regarding how to provide both loving and safe care for your senior loved one, contact Gateway Gardens Assisted Living and Memory Care here in Bethlehem.
22 June 2020

Whether you spent Father’s Day with Dad here at Gateway Gardens Assisted Living & Memory Care (here in Bethlehem) or not, start thinking about your next tribute to remind him of how special he is to you and your family. If life got in the way and you could not be with Dad this past weekend, it’s not too late to make next weekend something very special.
It is our pleasure to share our professional experiences and lessons learned regarding assisted living, memory care, and respite care support services. One lesson learned is that paying tribute to your aging Dad should not be a Father’s Day only affair. Look deep into your creative self and do something more from the heart than the wallet.
Here are four particularly rewarding tributes that Dads of all ages will enjoy:
1. A Handmade Family Tree
Even if you think your father isn’t nostalgic about the past, people do change as they get older. Some discover, in their senior years, a sudden passion for genealogy. Others simply want to talk about the past more often than they ever used to do.
Either way, a thoughtful gift might be a handmade family tree from you.
There are templates you can use which merely require you to fill in the names of the generations by hand. Then, you can take your finished product to a copy store and have it printed out for framing.
Choose good quality paper and you’ve created a real family heirloom.
2. Top-of-the-Line Gourmet Food
Some seniors become picky eaters as they age. What used to taste great may now be undesirable. It could be because dietary needs change as we get older. Sometimes it is the side effect of a medication.
One way to jump-start an older father or grandfather’s appetite is to offer up something irresistible.
3. A Photo Printer
Fathers these days tend to have a lot of digital pictures stored away on hard drives. Whether its pictures of grandchildren or places they’ve traveled to, the images are stored digitally and therefore viewable only on a device.
If your father is like most in his generation, he may yearn for the days when photos were printed and easily accessible in a shoebox. One thoughtful present would be to give him a photo printer.
That way, he can print out the photos he loves and have them in the format he’s used to.
4. A Digital Transformation of His Old Slides & Movies
This one is the opposite of the idea above. Seniors also tend to have lots of slides and movies tucked away, too. Just think: their child-rearing days coincided with the first home movie cameras. Going back even further, they may also have slides of their early days before you were even around.
The trouble is slide projectors and old reel-to-reel projectors have a funny way of failing after several decades of lying around in storage in a closet. That means all those great memories are locked away on outdated media formats.
There are companies who specialize in this. You give them your old slides or reel tapes. The company returns them along with a CD that contains everything in digital format.
The best part about this special gift is that you get to share it together. In fact, viewing the old memories can become a family event. One that is truly a memorable and meaningful gift that is sure to warm the hearts of everyone. Prepare for tears!
To learn more about our approach to professional assisted living, professional memory care, and/or professional respite care services, call us anytime!
8 June 2020

We hope you realize by now that we pride ourselves here at Gateway Gardens Assisted Living & Memory Care (here in Bethlehem) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Bethlehem who lovingly provide at-home assisted living and/or memory care services to your loved ones. Trust us, we know your challenges and consider you all heroes for your selfless and loving investment to family.
An at-home care giver communicated that her mother is 81, her arthritis is painful, but she gets around with a walker. Her mind is okay for now, though she is sometimes forgetful. She feels lonely. Her care giver is worried about her safety and has been telling her for several years that she needs help. She hates the thought of her falling and not having help, There is a fantastic assisted living close by, but will she listen? No! She just stubbornly says that she’s fine so I should leave her alone.”
Well, she’s likely right that her mom would be safer if she had someone checking on her regularly. Also, depending on her mom’s personality, her mom might be happier with the easy availability of companionship that assisted living offers. Why the resistance?
Some possibilities:
We often forget that our parents are adults who have lived long, and in most cases, responsible lives. They may have been poor parents, ordinary parents, or stellar parents, but the fact that we are trying to help them at this stage implies that they most likely did raise us. While occasionally you’ll meet an elder who willingly turns over all decisions to others, most will continue to want their autonomy. They want to make the decisions that rule their lives.
So, when they need help, what do you do? You take a step back and then try a different approach.
When possible talk with your parents about all kinds of things, not just their health and impending frailty. In other words, have real conversations.
Within those conversations, you’ll likely see opportunities to discuss their ideal wishes. Even if they are already at a stage where they probably should make adjustments in how they are living, approach it by asking how they see their future. Let your parent or parents know that you want to follow their wishes if you can, and you will always do your best to care for them, but that you need information in order to do that.
Try this: Rather than “Mom, you aren’t safe alone and you need help,” say, “Mom, I’m wondering if you could benefit from some help around the house?”
Suggesting some housekeeping help could open the door to the idea. From there, you could move to help with showering, medications, and other daily needs.
If she says she doesn’t want people in her home (she probably will), you could bring up assisted living. Again, mention that she might be able to benefit from this arrangement.
Why does it matter how you present the issues? My mantra is put yourself in their place.
Sometimes it’s about fear. Other times it’s simply about saving face. Whatever the reason, ask yourself how you’d feel if someone decades younger than you suddenly started telling what you needed to do to “stay safe.”
Remember, YOU want them safe. They want to live their lives. Think about where they are rather than your fear for them.
To learn more about our approach to professional assisted living, professional memory care services, or professional respite services, call us anytime!
25 May 2020

For more information and/or for any concern, contact us anytime!
11 May 2020

In the months leading up to a senior loved one’s transition to an assisted living community like ours here at Gateway Gardens Assisted Living & Memory Care Bethlehem, family members are busy (often overwhelmed) juggling all of the details of the move. From helping your loved one to downsize and sell their home to figuring out a floor plan for their new suite or villa, the busy days often leave little time for much else.
Once your family elder has made the move, you may find yourself coping with a range of emotions. Guilt, worry, and sadness are common. Your role has changed in your family member’s life and that will be an adjustment. You might also be asking yourself what comes next. How can you stay connected to your loved one, while also giving them the space needed to get involved at the assisted living community?
Today we offer three simple suggestions that you we’re certain will help you with the transition.
1. Create a visitor’s calendar: After your relative is unpacked and settled, work with them to set up a schedule for visitors. Having people drop in during the first month or so following the move enables your loved one to have company on a consistent basis. Setting up a calendar can help to avoid prolonged periods of time where no one stops by. Planning visits can also give the older adult something to look forward to as they adjust to their new surroundings. Be sure to include extended family members and people your loved one is close to in these plans. Encourage visitors to ask the senior to show them around and introduce them to fellow residents and staff they’ve met.
2. Participate in resident activities: We take a holistic approach to wellness by offering residents an opportunity to participate in activities that nurture the mind, body, and spirit. There are events and activities designed to appeal to every hobby and interest. Sit down and review the current month’s calendar together. If your loved one is reluctant to take part in activities on their own, it may help to have you and other family members participate, too. At least until they’ve met some new friends and are comfortable attending alone.
3. Get to know the staff and some of our residents here at Manor Lake Assisted Living & Memory Care: When you’ve been intimately involved in an elder’s care, it can be tough to turn those tasks over to someone else after they move. You may worry if the senior will get the attention they need. It will likely give you peace of mind if you get to know your assisted living team here in Hiram. We’re here to care for you as well with a wealth of knowledge that is certain to give you peace.
Call us anytime as we're here for you!
4 May 2020

We pride ourselves here at Gateway Gardens Assisted Living & Memory Care (here in Bethlehem) for helping more than our residents and their families. We take great pride in helping you, our neighbors here in Bethlehem who lovingly provide at-home assisted living and/or memory care services to your loved ones. Trust us, we know your challenges and consider you all heroes for your selfless and loving investment to family.
Today we give full credit to the professionals at “Caring.com” for a wonderful work regarding smart things to do regarding managing the finances of your loved one. More than four in 10 family caregivers spend $5,000 or more annually on caregiving, according to a new Caring.com survey of 2,767 family caregivers. Close to half rely on family funds to cover costs. And with nearly 40% of respondents also spending more than 30 hours per week on caregiving, caring for a loved one has become a full-time, unpaid job for many — one that leaves little time for a caregiver to plan for their own financial future.
“Quite often caregivers find themselves dipping into their own pockets to pay for caregiving expenses,” said Tim Sullivan, Vice President at Caring.com. “Without a plan in place, savings can be depleted, and retirement delayed. It’s so important to make the time to speak with your loved ones about finances, eldercare and planning for the future,” Sullivan added.
Caregivers who seek to educate themselves about their options can avoid the unnecessary stress of common financial mistakes. This guide can help you discover the tax advantages, professional services and investment strategies that can lessen caregiving-related financial strain.
Financial Questions to Ask your Aging Loved Ones
Managing your own money isn’t easy under the best of circumstances, so it’s not surprising that most people feel overwhelmed when it’s time to step in and take over the management of their parents’ finances. The first step is to accept that you won’t know what kind of shape their finances are in until you ask. Money is always a sticky topic, especially for adults who are beginning to lose their independence, so it is best to approach the discussion fully prepared to ask the right questions.
Finding answers to the following questions will put you on the path to becoming a more confident, and more capable guardian of your loved ones’ financial future.
1. “Do you have a durable power of attorney?”
The durable power of attorney (DPOA) is considered one of the most important personal legal documents for any older adult to have. Along with a healthcare proxy, it will give whomever your parent designates — whether it be you, one of your siblings or someone else — the power to make financial and legal decisions (or, in the case of a healthcare proxy, to make medical decisions) if your parent is incapacitated.
Without a durable power of attorney in place, you’ll have to go to court to get appointed as your parent’s guardian. That’s the last thing you’ll want to have to think about in a time of crisis, and it’s a notoriously complicated and messy legal process. With a durable power of attorney and healthcare proxy in place, you can seamlessly make decisions and access accounts on your parent’s behalf without getting the courts involved.
2. “Have you updated your will, insurance and retirement account information recently?”
Many people never take another look at their insurance policies or investment account beneficiary designations after they sign the initial papers, but both should be reviewed every year. Beneficiary designations — of who will receive the proceeds from an account if the policy or account holder dies — can be affected by any change in family circumstance, like the birth of a new child, a death or a divorce.
A yearly financial and insurance review also provides a good moment for your parent to review his asset allocation and evaluate whether he has enough, or too much life insurance. If, for example, his children are grown and his spouse has other funds on which to live after he’s gone, your parent could think about cutting back on the amount of life insurance he carries to save money on annual premiums.
3. “Do you have plans or insurance in place to pay for long-term care if it’s needed?”
Even if your parent is in good health today, eventually, he’ll likely need some type of long-term care — and the costs are staggering. A year in a nursing home costs more than $50,000 on average, and much more in some states. Usually, neither health insurance nor Medicare cover any of these expenses, so your parent should have some type of plan in place to pay for such care should it be needed. Long-term care insurance is a good option and can be added to existing life insurance policies, possibly at a discounted rate.
Medicaid also covers some nursing home costs, but your parent should consult an elder-law attorney now to find out if he qualifies for Medicaid. If not, the attorney may advise spending down assets – literally, the process of spending money without gifting or transferring assets until your parent meets the strict income requirements necessary to qualify for Medicaid. Without a plan in place to pay for long-term care, you and your siblings will be on the hook to pick up the cost unless your parent has very deep pockets.
4. “Who’s advising you?”
Although most adults are fiercely private about their finances and want to maintain their independence, it’s important in case of an emergency that you know how to contact your parent’s attorney, financial advisor, accountant and insurance agent. At the same time, as your parent ages, you can keep an eye on whether his financial and legal advisers are scrupulous, objective and well-versed in elder financial issues, with no vested interest in selling specific products. Getting the details on exactly who is advising your parent is a good way to protect him from scams, as well as to ensure that he has funds in case of an emergency.
5. “Where is all this stuff?”
If your parent has a stroke or heart attack, the last thing you’re going to want to worry about is what his Social Security number is, what health insurance he has or whether the mortgage has been paid. That’s why it’s important to sit down with him before a crisis hits and find out what kind of bill-paying system he has in place, what insurance he has and where all his important papers are located.
Although some may balk at sharing this kind of personal information, reassure him that you don’t have to see any of his private papers now; you only need to know where they are to ensure his financial well-being in the event that he’s not able to take care of it himself.
To learn more about our approach to professional assisted living, professional memory care services, or professional respite services, call us anytime!
20 April 2020

If you ever watched a comedic sitcom or movie on television, you likely seen this common scene. An elderly person loses their hearing aid, causing them to mishear certain lines from another character. As a result, a comedic situation is played out. However, it’s only a satirization of a subject that we take very seriously here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem. Approximately 10,000 Americans become sixty-five every day, so the need for recognizing, understanding, and treating hearing loss is increasingly important.
Due to misconceptions of hearing loss, most people don’t know the truth and facts about the subject. The reality is that we will all experience some form of hearing loss at some point of our life. It will also be in varying degrees. The reason why is because of the biological change a person experiences as they grow older. However, because of public perception, people don’t realize the facts about this ongoing health issue for seniors. Here’s what people should know about hearing loss.
Aside for the medical issues that hearing loss can bring, it can also bring on several emotional problems for seniors. Due to most seniors feeling embarrassed by their conditions, they tend to resort to defensive mechanisms and deny their conditions publicly. For example, an assisted living resident here at Gateway Gardens might begin to avoid social gatherings because of their hearing loss. But our caring assisted living professionals are trained and attentive to both the tell-tale signs of diminished hearing and related behavioral changes like new tendencies to isolate themselves from others.
It’s powerfully rewarding providing loving assistance to our cherished residents. Helping residents and their families recognize the need for initial or recurring hearing treatment is an important aspect of enriching the quality of life of those we serve. To learn more about our approach to professional assisted living, professional memory care services, or professional respite services, call us anytime!
13 April 2020

Greetings all. Your caring staff here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem are fully aware that this is the third pandemic-related blog post in a row. Rest assured we’ll move on soon enough to more uplifting messaging, but we can’t turn our head to the fact that defending against this pandemic is our number one priority.
Below, we offer a number of insights for you at-home care givers, some of which most of us by now are fully aware of and implementing, other things that maybe you haven’t given thought to do. Rest assured that these are things being implemented within both our assisted living and memory care communities. Regardless whether you’re a Manor Lake resident, family member, or neither, you’re all precious members of our community and we will always do our part to help out in any way we can. So here you go:
Caring for a Senior at Home During a Pandemic
1. Frequent handwashing: One of the best ways to prevent getting sick is to wash your hands in hot, soapy water throughout the day. This guide from the Centers for Disease Control and Prevention outlines a 5-step process for proper handwashing.
2. Use hand sanitizer: While hot water and soap will always be the best option, hand sanitizer can help when you are out in public and don’t have access to a restroom. Choose one that contains at least 60 percent alcohol.
3. Don’t touch your face: Most people don’t realize how many times an hour they touch their face until they try not to do so. A quick rub of the eye or a scratch on the nose happens more often than you think. If you’ve been exposed to a virus and have it on your hands, touching your face can easily transfer the bug.
4. Take good care: A healthy diet combined with exercise and a good night’s sleep help keep your immune system strong. That’s vital for fighting off viruses of all kinds.
5. Limit public activity: Social distancing is another important step in protecting a senior family member from COVID-19 and other viruses. To the extent that you can, avoid going out in public while viruses are spreading. Utilize services like home delivered meals, drive-through pharmacies, and online shopping wherever possible.
6. Screen all visitors: Be vigilant about limiting who can visit your home or the home of your loved one during this time. People who are out in public may be carrying the virus and not showing any symptoms. By allowing others into your home, you are placing yourself and your loved one at risk.
7. Explore virtual physician visits: If a senior has a routine medical appointment scheduled, call the physician’s office. Many doctors are moving to virtual visits until the pandemic is under control.
Supporting a Loved One When You Can’t Be There
If your aging parent or another senior loved one resides in an assisted living community, you may not be able to visit during an outbreak of the flu or a pandemic emergency. This can be stressful for all involved. Finding ways to stay connected can help keep everyone’s spirits up.
Here are a few suggestions for doing so:
Dementia and COVID-19
According to the Alzheimer’s Association, having dementia doesn’t increase a person’s risk for contracting COVID-19. However, some behavior-related issues linked to dementia might. Also, because people with dementia are typically older, their odds of getting the virus are higher.
One risk for those who experience memory loss is that they may forget to wash their hands or refrain from touching their face. Both are known risk factors for viruses of all types.
Another complicating factor is if a senior with dementia has lost or impaired verbal skills. They may be unable to communicate that they have a headache or are experiencing chest pain, two symptoms of COVID-19.
Here are a few suggestions that may help you lower your family members risk for the illness:
Stay Updated on the COVID-19 Pandemic
Finally, learning more about COVID-19 and staying informed about changes in the state of the pandemic is important. While it’s not necessary to watch the news stations around the clock, staying updated on new information is a method of self-protection.
Here are two resources you can turn to for novel coronavirus education and updates:
Most states and local governments also share frequent updates on the pandemic. Call your local officials to learn more.
If you or a family member is a resident of Gateway Gardens Assisted Living and Memory Care here in Bethlehem, please know that we actively welcome your calls so that we can personally reassure you of the steps we are taking to keep residents and team members safe.
6 April 2020

Today we offer you an outstanding article written by Linda Dono, a featured writer with AARP. We believe all readers can take something away from this. To protect the most vulnerable residents against COVID-19, assisted living, memory care, and respite care communities (like ours here at Gateway Gardens here in Bethlehem) are raising the bar for casual visits — following federal and health care industry recommendations as coronavirus infections spread across the country.
So, what can you do to keep a loved one engaged and not socially isolated? Here are ideas to show you are still there in spirit and still care.
1. Send snail mail
Handwritten cards and letters are more special than ever, perhaps because electronic communication is increasingly supplanting them. Recipients can display the cards and re-read correspondence to remind themselves that you care.
2. Share a virtual meal
Plan a long-distance date. Order what your loved one likes — and pay for it — via a meal delivery service such as DoorDash or Grubhub and make sure the meal gets there at the appropriate time. Then call to talk during the meal, making sure that your resident knows how to use a speakerphone feature on her cellphone or landline phone.
3. Use other delivery services
You know the snacks your loved likes. Since you can't bring a few packages of treats during a visit, arrange for a bulk delivery.
For those in assisted living or independent living who still like to cook, you can get their grocery lists and do the shopping for them or use a shopping service such as Instacart. Deliver the food as close in as you're allowed and make sure to put the name and address or room number of the recipient on the boxes or bags.
4. Create your own FaceTime book club
If your kids are at an age where they love being read to, make sure Grandma or Grandpa has some kids’ books they can read aloud — if they don't, order some online — using the video-calling feature on their digital device.
Among the most popular video calling apps is Apple's FaceTime, but that's for iPhones, iPads and Macintosh computers only. Amazon Alexa, Facebook Messenger, Google Duo, IMO, Skype, Viber and WhatsApp also work on Google Android, Microsoft Windows and other devices.
Be sure to coordinate so that everybody is on the same platform. This way, grandkids of different siblings can be on the same story time call.
Older kids can make the call more like adults’ book clubs. Both grandparent and grandchild can read a couple of chapters of the same book and talk about their impressions or what they learned.
Watching the same TV show, such as a documentary on Netflix or Amazon Prime, also can help spark discussion that spans generations.
And if reading a book or watching a documentary isn't an option, perhaps because of your loved one's memory loss, help the kids in a sing-along. Singing old, familiar songs — “Happy Birthday,” classic hymns if they're religious — can bring back memories and is a skill that often remains even if speech is difficult.
5. Order a jigsaw puzzle — of your family
Mail-order companies specialize in custom puzzles from photographs or perhaps your child's artwork.
If your care recipient is a puzzle lover, you can have a puzzle delivered that contains 2,000 or more pieces. But also available are those with as few as 15 pieces, which might work well for people with dementia or less dexterity.
While you're at it, order a coffee mug with the favorite family photo, too.
6. Play a board game
Think about the games your family loved growing up, such as Clue, Monopoly, Life, Scrabble or Sorry, or if you have young kids, children's classics such as Candyland or Chutes and Ladders. Familiarity with the rules is important.
Backgammon, bingo and chess also will work if you've played those in the past and both sides know the lingo of the game. Make sure identical game boards are set up at your house and your loved one's home. You and your family then can play the game over the telephone, talking about how the dice landed and what moves your game piece is making.
A cellphone set on speaker will work well for this because games sometimes take hours. A video call also will add dimension but isn't necessary if everyone commits to narrating their actions.
7. Assemble a hobby box
This is the time to find a nice box at a craft store, perhaps decorate it and fill it with items that your loved ones can come back to again and again.
Put in items that will work with their existing hobbies or ask what they've always wanted to try. Think crossword puzzle books for those who like a brain challenge, paints and suitable paper for those who have been artistic in the craft room, squishy balls and miniature Slinkys or other toys for those with a silly streak, yarn and hooks for crocheters.
You can rest assured that maintaining the health, wellness, and safety of our residents remains our uninterrupted number one priority. We want you to know that we are here to help. Contact Gateway Gardens Assisted Living and Memory Care in Bethlehem anytime with questions and/or concerns.
31 March 2020

All of us here at Gateway Gardens Assisted Living and Memory Care here in Bethlehem are adjusting dialing to the unprecedented challenges to providing professional assisted living and memory care services. One of the most rewarding services that we conduct is group exercise classes which of course are both disallowed and unadvised during the COVID-19 outbreak. But it is important to encourage older adults to stay active and maintain gains in strength, balance, and flexibility that reduce fall risk, strengthen the immune system, and improve quality of life.
Older adults may be concerned about their safety as they prepare to exercise within their personal space, but research has shown that the risks of solo exercise is no greater than exercising in a group setting. Use these tips and resources when communicating with older adults about the importance of staying active during this time.
Rest assured that maintaining the health, wellness, and safety of our residents and staff is our number one priority. We want you to know that we are here to help. Contact Gateway Gardens Assisted Living and Memory Care in Bethlehem anytime with questions and/or concerns.
Credit: Jennifer Tripken, EdD, ncoa.org
17 March 2020

Maintaining the health, wellness, and safety of our residents is our number one priority. Due to the COVID-19 situation, effective immediately we are restricting visitors to our community. This is in cooperation with federal mandates regarding this situation. Letters regarding specific details are being sent to the responsible parties for our residents to provide them with more detailed information. In addition to restricting visits, our staff will be screened prior to the starting of their shifts and have been trained on the symptoms of COVID-19 as well as infection prevention techniques. This is a fluid situation and we will keep you informed as the situation changes.
Again, maintaining the health, wellness, and safety of our residents and staff is our number one priority. We want you to know that we are here to help. Contact Gateway Gardens Assisted Living and Memory Care in Bethlehem today with any questions and/or concerns.
2 March 2020

We have a lot in common with those of you out there providing at-home assisted living services or memory care services in and around Bethlehem. For instance, the challenges related to loss of appetite within our aging loved ones is common to both professional and at-home care givers alike. We believe you’ll find this blog post both educational and actionable in addressing the loss of appetite within the loved one under your care.
A Loss of Appetite in a Parent or Senior Loved One
A loss and changes in appetite are a natural part of aging. Although poor appetite doesn’t necessarily indicate a serious health problem such as dementia in the elderly, it is still critical to make sure seniors get enough nutrients. Along with some warning signs to be mindful of, there are some easy ways you can help your senior loved ones get the right nutrition.
Although it’s normal for our appetites to change with age, several different factors can also cause a loss of appetite in the elderly:
“I remind my clients often that a loss of appetite (and thirst) is a normal part of aging and doesn’t always mean something is wrong,” says Heather Schwartz, RD, at Stanford Hospital and Clinics. “However, minimizing the detrimental effects of poor nutrient intake is always important, no matter from where the low appetite stems.”
It is also critical to rule out any underlying health problems or symptoms. If your loved ones aren’t eating well, a good first step is always to consult a physician.
What Should I Be Concerned About?
The aging process brings with it many perceptual, physiological and other changes that can lead to decreased appetite in the elderly patient, including:
However, if your parents or senior loved ones are making poor food choices because of their changing tastes, or if they aren’t getting enough to eat, then that’s cause for concern. Seniors must get the right nutrition for their changing dietary needs. Vitamin or nutrient deficiencies can cause significant health problems for vulnerable groups, especially the elderly. Changes to taste or appetite also occur in conjunction with some serious illnesses, including:
Any unexplained changes to your loved ones’ dietary health, including unexpected weight gain, loss or general malaise, should be checked out with a physician so you can rule out or confirm symptoms of dementia.
How Can I Stimulate an Appetite in the Elderly?
If you’re concerned about a lack of appetite in your elderly loved ones, whether dementia is a concern or not, there are a few practical things you can do to help them get enough nutrition:
Be aware of medication side effects.
If the problem is dry mouth, Schwartz says, “Chewing sugarless gum, brushing often or using an oral rinse before meals can improve taste sensation, and ultimately nutrient intake.” If meat is tasting “off” — and a common complaint is that some medications make foods taste metallic — then try other sources of protein like dairy or beans. If water doesn’t taste right, try adding herbs, or sliced fruits or veggies like lemon or cucumber.
Consider using an appetite stimulant.
Some seniors have had success with prescription appetite stimulants. A healthcare provider must be consulted to inform the patient and caregiver of the side effects of the stimulant and to also make sure it is appropriate for your loved one.
Encourage social meals.
People of all ages may experience a reduced appetite when the thought of eating alone comes to mind. For seniors, accessibility and availability of social contact can be even more of a problem, especially if they suffer from dementia. Schwartz suggests checking out the meal options at senior centers, temples or churches, and community centers. Additionally, meal “dates” with friends, family or caregivers and even meal delivery services can help.
Increase nutrient density, not portion size.
“I ask caregivers not to increase the volume of food they serve to seniors who may have low appetites,” says Schwartz. “Rather, increase the nutrient density of the foods they serve.” In other words, don’t intimidate them with a huge helping. Alternatively, add healthy extra calories in the form of avocado, olive oil or a little peanut butter.
Set a regular eating schedule.
“Our bodies tend to thrive off regularity, as do our hunger and thirst signals, so when we stray from our usual patterns, so does our appetite,” says Schwartz. She suggests starting slowly by adding a small beverage and/or snack during a normal mealtime. This can help stimulate the body’s hunger signals.
Eating to Encourage a Good Night’s Sleep
In addition to experiencing serious changes in appetite, older adults and individuals with dementia often experience changes in their sleeping patterns. Such changes may be as a result of sleep disorders, such as insomnia or sleep apnea.3 They may also be related to pain or discomfort. It is not uncommon for people to be uncertain when addressing their elderly loved ones’ lack of eating and sleeping. However, both adequate sleep and nutrient consumption are critical for promoting optimal health.
Not eating during the day and feeling hungry at night can make sleeping even more difficult. Such unhealthy patterns increase the frequency of night awakenings. If dementia is involved, this can be very disorienting. Alternatively, chronic fatigue can make elderly adults less likely to finish meals. Consistent sleep deprivation can contribute to feelings of depression and a lack of physical activity, which can also negatively impact the senior’s appetite.
Foods To Eat for Better Sleep
In addition to getting enough to eat throughout the day, it is important that caregivers pay special attention to what is on a senior’s plate during the hours directly preceding bedtime. Try encouraging the following items for dinner and nighttime snacks:
Make sure to limit meal sizes late at night and avoid overly greasy or spicy foods. Such foods may irritate the stomach and cause difficulty falling asleep. As a result, the patient might avoid future evening meals. Also, older adults should avoid alcohol before bed since it affects normal sleeping patterns.
We want you to know that we are here to help. Contact Gateway Gardens Assisted Living and Memory Care in Bethlehem today.
Credit: Heather Schwartz, RD
24 February 2020

As professional assisted living and memory care support providers here in Bethlehem, we know it is often times intimidating when providing care for senior living, assisted living, memory care, or respite care loved ones. Today we’re asking all of you in this loving struggle to take a moment and reflect if you might unknowingly make some simple mistakes that make it harder on both you and the loved one under your care. The keyword there is “unknowingly” and if we connect with just one of you out there and motivate some new degree of peace and happiness, well, we celebrate mission accomplished.
Today’s due credit is provided to Health Central, an award-winning non-profit dedicated to improving the mental and physical health of both the young and old.
Please realize that this list is only a start. While reading, when/if you discover “that’s me”, then consider avoiding or rewording these questions and statements may improve your caregiving partnership. Also, realize this blog post really is a call for you to take a moment to dedicate a few moments of your time to honest reflection. You can be your own best asset regarding constructive criticism, and when you are and you react accordingly, both you and your loved ones can enter a happier space. So, off we go.
1. “Do you remember?”
It seems natural to ask your dad who is living with Alzheimer’s (or simply the very natural memory recall decay associated with aging) about events from his past. However, doing so directly can be a problem. Why? Because he may not remember the event, but the expectation that he should remember could make him anxious. Instead, when you want to engage him in conversation about the past, leave the topic open. You can say, “Dad, I’d love to hear about what your favorite thing to do was when you were growing up.” He can then take you along on any adventure that comes to mind.
2. Don’t argue.
If your wife says that she used to live in a house that you’ve never heard of or seen, you can say “Really? I’d forgotten that.” Being right doesn’t matter and correcting or arguing will get you nowhere good. Go along for the ride. You might learn something interesting. If not, no harm done.
3. “You’re embarrassing me!”
A reminder for us all is that people living with dementia (or non-dementia memory decay) aren’t giving us a hard time – they are having a hard time. If you are at the store with your husband and he becomes anxious which causes him to become belligerent, soothe him by holding his arm in a comforting manner, use a calm voice and put the “blame” on yourself. Tell him that you forgot something and really need him to help you by going back home. Do not tell him that his behavior embarrasses you. He can’t help it.
4. “Why are you doing that?”
If your husband is pulling on the fringe around a couch cushion, he isn’t being purposefully destructive. People living with Alzheimer’s often have a need for tactile feedback. Additionally, they may have a compulsion for their fingers to be doing something. Some people will pick at their skin and cause sores. Others will spend hours tearing up pieces of paper or tissues. Your husband won’t know why he is doing this, but you can help him by buying him a lap pad or “fiddle pad.” These products, now widely available, provide both tactile stimulation and keep fingers busy.
5. “What shirt do you want to wear?”
People living with dementia have a hard-enough time navigating this confusing world without being asked open-ended questions. Preserve dignity by offering choices, which is a vital part of care, but simplify the choices by holding up two shirts and asking which she’d like to wear. He may mention the color of one shirt, but point at another, so go with the one he points to and say, “This one?” Then he’ll say yes or no, or else nod. You can say, “Great choice! Let’s put that on,” and then help him dress.
6. “That’s an orange, not an apple!”
It doesn’t matter, it doesn’t matter, it doesn’t matter. It’s up to you to remember that the person living with dementia may have a hard time with words. Don’t make your mom feel worse by criticizing her words. If you ask her if she’d like an orange and she says yes but digs for an apple, let it go. If she has what she wants, then everyone should be happy.
7. “You are home!”
No one approach will work every time, but what is consistent is that your loved one is looking for a feeling of safety and comfort when she asks this question. If you can distract her by asking her to snuggle on the couch under a blanket and watch a DVD, that may work. Or you may ask her if she misses home a lot. If she says yes, ask what she misses about it. Engage her in a conversation and, eventually, the anxiety that causes her to want to ‘go home’ should subside. There are many guides for dealing with this common issue.
8. “You just ate!”
People living with dementia often don’t remember if they ate so they may want to eat again. Often, keeping snack foods around can help. Instead of scolding your dad for asking to eat again when he just ate, when he wants to eat again you can suggest some treat that he likes and then offer a small amount. That snack may be enough to satisfy without arguing about the fact that he just had supper.
9. “We need to hurry!”
Your dad has an appointment to see the doctor and you’ve waited a month for this, but he is stuck in a fearful mode and becomes angry and throws things rather than getting dressed. Obviously, he is stressed and trying to hurry him won’t help. Calm yourself down first and offer support by agreeing that this is a stressful situation. Take time to sit and comfort him. If you began preparing early, this may work. If not, you may have to cancel the appointment. Sometimes you must just let it go and hope for a better day.
10. “Here, let me do that!”
Your husband who is living with dementia will become easily confused, and stress just makes the confusion worse. Trying to get a button in a buttonhole can be a massive frustration, yet he may not want help. Sometimes, you can distract him from the task at hand and later do it yourself, but when possible, have patience and let him finish. Note: When it comes to getting dressed, adaptive clothing can be helpful. An ingenious shirt with magnets instead of buttons can look dressy yet be easy to put on. With some digging, you may find shortcuts for other tasks, as well. The idea is that your patience is gold. Allow room for slowness and mistakes. None of this is worth a blowup on your part. Your anger or anxiety only accelerates his anxiety and can ruin what could be an otherwise decent day.
When interacting with a person living with any type of dementia it's generally better to use statements rather than questions unless you are offering a simple, obvious choice. Say, “It’s cold so we need jackets,” rather than “Do you think you need a jacket?” As your loved one’s disease progresses, words will become increasingly hard to process and decisions can be impossible to make. Watch for this progression and adjust your speech so that you have a slower cadence. Use short sentences but speak with a smile. Sometimes your body language can say it all.
You’ll never stop learning in your journey of loving care. If we helped you learn one thing here today, then we both win! When the time comes for you to seek a consult regarding how Gateway Gardens Assisted Living & Memory Care Bethlehem can improve the quality of both you and your loved one’s lives, call us!
17 February 2020

Prologue: All professional memory care and assisted living care providers like us here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem understand and respect those of you who so lovingly carry the burden of care for your loved ones. Part of our community service campaign is to educate via this blog so that you can enjoy the maximum time at home with your loved ones. However, statistics show that unfortunately there will come a day when solo home care or professionally assisted home care is no longer enough. To every extent possible, we’ll be here for you via this assisted living and memory care blog, week in, and week out with insights that hopefully helps ease your loving burden. When that burden becomes too heavy to bear, know that your friends here at Gateway Gardens Assisted Living & Memory Care are ready with open arms to provide the loving care necessary to deliver the quality of life that both you and your challenged loved one(s) deserve.
(Due credit for this blog post and its insights is provided to Ms. Carol Bursack, of agingcare.com. We think you’ll value her work and insight as much as we do.)
Family caregivers are now better able to take advantage of services offered by home care companies. I certainly took advantage of these services throughout my time caring for multiple seniors, including my parents and an elderly neighbor.
The biggest challenge I faced, though, was when I hired professional caregivers for loved ones who had dementia. The caregivers were not always sure how to handle unusual behaviors associated with Alzheimer’s or the tricky situations they created. Thankfully, due to increased awareness of the unique challenges that Alzheimer’s disease and other forms of dementia present, reputable home care companies across the country are providing their employees with proper training in dementia care. Experienced and informed caregivers can provide benefits to both seniors and their family members that make in-home care well worth considering.
Dementia Care in a Familiar Environment
The biggest value that home care offers is that it allows elders to remain in their own homes for as long as possible. This option is far less disorienting for a dementia patient than a move to an assisted living facility, a memory care unit or a nursing home. Familiar environments offer a great deal of security and peace of mind for individuals with dementia. If a company’s caregivers are well versed in dementia care, in-home care can be the ideal starting point for families who need extra help with their loved ones but want to prevent or delay placement in a long-term care facility.
Dementia Patients Benefit from Routines
Just as familiar surroundings are safe and soothing, the same can be said for daily routines. Maintaining a schedule like the one a senior followed pre-dementia can help reduce anxiety and confusion. For example, an elder who watched the nightly news after dinner each evening for years may feel a sense of normalcy when it’s switched on, even if they don’t completely understand what they are seeing and hearing.
A fundamental aspect of home care is that services are provided for all clients (with and without dementia) according to personalized scheduling tools called care plans. This organizational technique easily translates into a set routine for dementia patients who thrive on familiarity and repetition. Professional caregivers are trained to facilitate daily activities, including chores and personal care tasks, at the appropriate times and provide assistance as needed. Humans are creatures of habit and preserving these very personal and deeply ingrained routines can help elders retain a sense of control and understanding of what is going on around them.
Specialized Training in Dementia Care
Home care companies aid with activities of daily living (ADLs), companionship and many other core services. In addition, many companies offer professional training in dementia care for their employees. Common aspects of this training include methods for staying engaged with the senior, managing often unpredictable behaviors through validation and redirection, communicating effectively, and breaking down activities into smaller steps that are easier to manage. There are several training programs and schools of thought when it comes to dementia care, so be sure to inquire about the particular education a home care company provides to or requires of its caregivers.
Safety training is also part of professional caregivers’ initial and ongoing education, since seniors with dementia may be prone to wandering and other risky behaviors. A 2013 study published in the Journal of the American Geriatrics Society found that 90 percent of community-residing persons with dementia had unmet safety needs, particularly for fall risk and wander risk management and home safety evaluations. Increased supervision and assistance from both informal and formal caregivers are crucial components in helping elders reduce safety risks while they continue living in their own homes.
Meaningful Activities for Dementia Patients
Knowledge of the clinical aspects of dementia allows professionals to better serve their clients and enrich their lives with social interactions and activities. Perceptive caregivers can provide a positive environment for dementia patients by learning about a senior’s interests before they developed the disease and adapting the way they engage in these meaningful hobbies both in the home and in the community. For example, if golf is something an elder enjoyed, they may visit a golf course for a walk or to watch others play the game.
Sensory stimulation is another crucial component of dementia care, especially in the later stages of cognitive impairment. Studies show that participating in music therapy, dance or other creative outlets has a positive effect on mental health, physical health and social functioning in older adults. An experienced caregiver will work to engage clients in activities even as their interests and abilities change.
Care That Evolves with the Client
In-home care can be customized to provide as much or as little assistance as a family requires, and changes can be made as often as necessary. Services can be unskilled (companion care and homemaker services) or skilled (personal care and nursing care) in nature and can be provided occasionally for respite, on an around-the-clock basis or anywhere in between. This flexibility is a significant advantage for caregivers and seniors who are dealing with progressive diseases such as dementia. As a loved one’s condition declines, professional caregivers offer the adaptability necessary in caring for an individual with Alzheimer’s and related dementias.
When Home Care Is No Longer Enough
In-home services can help dementia patients delay the move to long-term care, but their growing needs will eventually necessitate higher levels of care and around-the-clock supervision. Without a robust team of informal caregivers to share the burden, it becomes necessary to look elsewhere for assistance. While it is possible to receive these services in the home, the cost of 24/7 home care is often too much for the average family to pay for privately over the long term.
The time for thinking about a move to assisted living, a memory care unit or a nursing home is different for everyone. The decision depends on whether family members and hired caregivers can continue to cope with changes in a senior’s condition at home. A competent home care company will closely monitor their ability to provide the best care for their patients. Should a client’s needs surpass what is noted in their current care plan, the company will let the family know that additional services or a change in setting is needed.
We hope you enjoyed, are encouraged, educated, and benefit from this and all our blogging efforts. When the time comes for you to seek a consult regarding how Gateway Gardens Assisted Living & Memory Care here in Bethlehem can improve the quality of both you and your loved one’s lives, call us!
10 February 2020

Valentine’s Day reserves special space in the hearts of many of the assisted living and/or memory care loved one’s that we support. Professional assisted living caregivers such as us here at Gateway Gardens Assisted Living & Memory Care in Bethlehem have long recognized that this Holiday can become a solemn one for many of our loved ones if the Holiday is ignored by caregivers. The reason is completely understandable when cherished Valentine’s Day memories of a deceased spouse often turn to solemn reflection.
Valentine’s Day is a perfect occasion to show the special people in your life just how much you care. Whether your Valentine’s Day plans include celebrating Valentine’s Day there at home or while visiting your aging parent or loved one residing within a professional assisted living community like Bethlehem’s Gateway Gardens, try out some of these ideas to celebrate the holiday:
Research a Special Valentine’s Day Memory
Search your photo archives of Valentine’s Day memories of both your loved one and their loving spouse who has passed. Your time and effort will bring joy to them and to you as well. Do this early in the day so that you both can move on to other activities that are likely to bring smiles to their face. The goal is to maximize positive moments at the expense of solemn reflection.
Spread the love
The “day of love” gives us all an excuse to spoil our loved ones and spread some cheer with a thoughtful gift. While the traditional Valentine’s Day presents of flowers and chocolates are always a hit, some other gift ideas for the senior in your life include things like cozy socks, a no-fuss houseplant, framed photographs or even a gift card to their favorite restaurant. At the end of the day, the best gift you can give your loved one is the gift of your time and presence.
Create DIY Valentines
Crafting is a fun activity that people of all ages enjoy. For senior adults, arts and crafts can be particularly helpful in improving hand-eye coordination and keeping their cognitive skills sharp. When you visit your older loved one in assisted living, bring along supplies to make handmade Valentine’s Day cards for friends, family members, and the caregivers at the assisted living community. Making a craft together is also a great way to keep grandchildren involved and ensure they have a lasting memory of the visit.
Take a trip down memory lane
Valentine’s Day is a wonderful opportunity to share fond memories and stories with our older loved ones. Learning about an older family member’s life and experiences firsthand is not only a powerful way to connect, but it also helps us understand who we are and where we came from. Once again, try looking at favorite family photos and letters or listening to familiar music to spark memories and prompt meaningful conversations about the past.
Here at Gateway Gardens, we encourage you to celebrate Valentine’s Day with your aging parent or loved one, whether they still live at home or within a professional assisted living community. Simply visiting your loved one and spending quality time with them is the best way to demonstrate your appreciation and make the holiday one to remember. Happy Valentine’s Day from all of us here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care!
5 February 2020
Come and Join us! Fun and More! Feat. Elvis, dancing, raffle, and treats for your sweets!

3 February 2020

In our continued support of you angels out there engaged in the loving sacrifice in providing senior assisted living or memory care support, today we’re going to share a fantastic discussion of one of the single most frustrating conditions that caregivers like you often deal with, your loved one’s paranoia. While most of this article deals with dementia-related paranoia, this article is very relevant to you senior living care providers as you will learn that paranoia is common within non-dementia inflicted seniors. So for all of you who provide assisted living or memory care support to loved ones in and around Bethlehem, know that you can lean on us here at Gateway Gardens Assisted Living and Memory Care.
Brain changes from dementia can cause hallucinations, delusions or paranoia. According to Heathman, MD, a Houston psychiatrist, “paranoia, or having false beliefs, is a common trait of later stage dementia. However, it can occur in all stages of dementia.”
What Do We Mean By Paranoia?
Sometimes our loved one living with dementia will believe something we do not. When this results in undesirable emotions such as fear, jealousy or anger, we call it paranoia. It is generally the secondary emotions we are upset by. With the term, paranoia, comes an implicit judgment and the implications that, “My reality is real, your reality and your feelings are not.”
The best thing we can do to alleviate ‘paranoia’ is to discard this judgment. Start from a place of “our realities are real and different.” For the person experiencing paranoia, their reality is as real to them as yours is to you and mine is to me. For the sake of understanding in this article, I will use the term ‘paranoia’. My hope is that after reading it you, like me, will not find a use for the word anymore.
How to Help Soothe Paranoia in Dementia
We can provide reassurance and support so those experiencing paranoia feel safe and loved. Do not fall into the trap of detailed explanations or logical arguments. Try these behavioral techniques to calm someone living with dementia, who is experiencing paranoia.
What we call paranoia in dementia feels very real for the person living with it. It is their reality. Susan London, LMSW, Director of Social Work at Shore View Nursing and Rehabilitation says that, “There is often no evidence that will convince them otherwise.” Try the following in response to your loved one:
Summary – Do’s and Don’ts for Paranoia in Dementia
Do:
Don’t:
When it’s time for you to seek help from a team of proven memory care professionals in and around Bethlehem, contact us. Anytime.
Source: Homecareassistance.com
28 January 2020

Regular readers of our Gateway Gardens Assisted Living & Memory Care blog know that we provide loving care to their assisted living or memory care dependent loved one. Today, we offer due credit to “BrightFocus Foundation” as the primary source for this blog post and for their genuine professionalism in funding research related to Alzheimer’s disease, macular degeneration, and glaucoma.
Today we chronicle the experiences of three caregivers of Alzheimer’s and dementia loved ones. They were asked what “best lessons” they could share with a friend who is new to Alzheimer’s or dementia caregiving. Below are their responses. But before reading further, all the professional assisted living and memory care staff here at Bethlehem’s Gateway Gardens stand ready to share our experiences and lessons learned as well.
Eileen - Years of Grieving. Then Respite. Then Clarity.
Eileen’s husband was diagnosed with Alzheimer’s four years ago. Their adult children and young grandchildren live out of state. While the children are very supportive from a distance, the daily caregiving role is all on Eileen. Through these four years, she has continued to work full time, at a job she loves.
Her husband remains mostly lucid, but increasingly there have been frustrating and scary moments, threatening behavior, and showering and bathing battles. With these episodes, and with her children’s encouragement, Eileen identified a memory care facility in her area, and reluctantly moved him there. The facility instructed her to not visit for two weeks so that he could acclimate. At the end of the two weeks, she went to see him. He was so mad at her, at first, he couldn’t even speak. But that lasted only briefly.
Marie - A Newer Caregiver Learning to Accept
Marie is newer to being an Alzheimer’s caregiver as her father was diagnosed with mid-stage Alzheimer’s just within the last year. He and Marie’s mother live with Marie, her husband and their school-age daughter. Marie and her husband both work fulltime – her workday starts at 6 am, his at 2 pm and Marie’s mother works part time. These schedules allow one of them to always be with her father, which became necessary following his recent wandering incident.
Through tears, Marie expressed her overwhelming feelings of guilt - guilt for being angry with him for having this disease, guilt for being angry that his behavior makes their life more difficult, and guilt when she wishes things were the way they used to be. She has taken classes to better understand the disease, and says she sometimes reads online caregiver comments, identifying with the guilty feelings people express. So far though, she has not been able to resolve these feelings of guilt. She remains frustrated, angry and tired, and feels bad about not yet being able to accept things as they are. She was not sure she had a “lesson” to offer. I reminded her that guilt is normal, and by doing what she is doing—taking classes and reading the online forums, she is doing all she can right now to accept it.
Edgar - Protecting His Wife
Edgar has been his wife’s primary caregiver for ten years. She has dementia, and when I asked him his best lesson as a caregiver, he was not sure he had one. “I am still learning,” he said, adding “I don’t know if I have adapted.” Then, he told me the story of his wife’s fall several years ago. She broke her femur, and then a few weeks later, fell again, and was hospitalized with three broken vertebrae. She had tremendous sciatica pain. She was prescribed pain medication that changed her behavior. From the hospital she went to rehab. Her personality remained changed as a result of the opioid medication. Because of this, Edgar then learned all about the side effects of opioids, and feels strongly that before accepting the use of these drugs, patients and/or families should consult with a second physician. Also, be diligent in weaning someone from them as soon as possible and, ideally, limiting their use to no more than 7 days.
Having said that, Edgar was quick to say that he sees many situations, in his wife’s memory care facility, with different degrees of difficulty. He cannot say his approach would be the right answer for others. His primary message, though, is to send a big caution on the use of medications in this population. He has been successful in minimizing his wife’s use of any drugs, and she has remained stable for several years during the years since recovering from the falls. If she ever has the need for more medication, he will definitely question her physicians about side effects and possible alternatives.
There is Hope and There is Help for all of You
Whether you provide your loved one assisted living support or memory care services, no matter where you are in the caregiving journey, as these stories show, there are struggles and lessons. But through research, we are learning more, and through education and awareness, caregivers can better manage the questions and stresses of caregiving. With more and more resources for caregivers, local community services, and education and sharing, each and every time someone shares a tip or a resource, someone else benefits. And that’s why we offer this story and manage this blog.
When it’s time for you to seek help from a team of proven memory care professionals in and around Bethlehem, contact us. Anytime.
21 January 2020

Suppose your elderly mother or father is struggling with day-to-day activities like laundry, cleaning and cooking. But he or she is not truly ill and doesn’t need a high level of daily health care. You worry about him or her walking up and down stairs or carrying a bag of groceries. An assisted community like ours here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care can serve as the perfect protective measure and path to providing them the very best quality of life possible.
What Is Assisted Living?
Assisted Living is perfect for seniors who are mostly independent, yet need help managing medications and meals. But there’s much more to Assisted Living than that. Bethlehem’s Gateway Gardens Assisted Living and Memory Care’s assisted living services include housekeeping, laundry, and a host of activities that our residents love. Hot and delicious meals are served three times a day and snacks are available all day. Assisted living is a type of communal living that seniors and their families choose when they are healthy but need a bit of extra help. Assisted living is a great intermediate step on the continuum of elderly care.
Assisted living is commonly paid for by individuals’ long-term care insurance. However, long-term care insurance coverage varies widely, and you need to know the details of your policy. In general, long-term care insurance is flexible along the continuum of care. It can pay for both assisted living and memory care services. Some policies allow you to tap long-term care policies for in-home services, but most are written to cover professional services such as ours.
If you live in or around the Bethlehem area and ever have questions about the challenges of creating a 24/7 safe and loving atmosphere for your senior loved on, we’re here to help. We want to develop a relationship with you based on trust and a common love for our ageing loved ones. We trust that when the time comes, you’ll team with us for your professional senior assisted living support services. Together, we’ll provide the best loving care possible. Give us a call. Let’s talk.
13 January 2020

We want to thank in advance “Active Beat” who publishes insightful works on healthy lifestyles. They recently offered advice for senior care givers regarding nutritional health. Here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care, we gladly share the following with you today whether you’re providing senior assisted living support or any form of memory care support services to your beloved. Afterall, we’re all in this together.
If you provide senior assisted living care for a loved one, you may already include supplements in order to boost their memory and protect against age-related memory decline. If you care for an already diagnosed Alzheimer’s or related dementia condition you likely are administering physician prescribed supplements. Regardless, researchers at Yale University claim that the body doesn’t absorb nutritional supplements quite as effectively as it does natural foods.
Whether you’re preventing a family history of dementia and Alzheimer’s, or just looking to reduce risk in general, researchers recommend following the “MIND” diet which is short for Mediterranean-DASH Intervention for Neurodegenerative Delay. It touts eating a more plant-based diet with limited red meat, saturated fats and sweets, says Mayo Clinic. And when it comes to brain-boosting Alzheimer’s-fighting super foods, these 12 foods should be at the top of your shopping list.
Berries
You likely already know that berries—such as strawberries, blueberries, and raspberries—are considered superfoods. This is due to the fact that they deliver a boatload of antioxidants in each bite! Antioxidants have long been linked to enhance cognitive function in dementia and Alzheimer’s patients. However, a study published by the Journal of Alzheimer’s Disease discovered that high-antioxidant berries were able to reduce plaque in the brain, which is thought to cause Alzheimer’s.
Chatelaine writes that blueberries in particular are among the best. “They contain flavonoids, which activate brain pathways associated with less cellular aging,” writes the source. WebMD also points out that berries have been linked to slowing down the symptoms of Alzheimer’s. We suggest eating about 1/2 cup three times a week.
Super Spices
Do you know what spices like turmeric, cocoa, cinnamon, and nutmeg have in common? According to the journal Central Nervous Systems Agents in Medicinal Chemistry, these spices contain certain polyphenols and compounds with numerous cognitive advantages. The journal research outlines the many gluco-recovery, anti-inflammatory, and antioxidant properties in these spices and theorizes on their Alzheimer’s prevention connection.
MindBodyGreen also explains that “these spices can all help to break up brain plaque and reduce inflammation of the brain which can cause memory issues.” The foods on this list will not only help improve brain function, but fight off illnesses that cause our brains to age prematurely like obesity, heart disease, diabetes and hypertension.
Omega-3’s
Natural foods rich in omega-3 fatty acids—namely nuts, flaxseeds, and certain types of fish—have long been linked to Alzheimer’s prevention. And even though much speculation can be found, more research must be conducted for undeniable scientific proof. However, research in the Journal of Alzheimer’s Disease as well as the European Journal of Nutrition, details how omega-3-rich foods can help decrease the rate of cognitive decline in Alzheimer’s patients.
Fatty fish like salmon and trout are particularly good because the iodine and iron “help maintain cognitive function” and they contain “brain boosting omega-3 fatty acids.” You should be eating these types of fish at least two or three times a week.
Coconut Oil
I know, here we go about the coconut oil—yet again! But really, research from the Journal of the American Academy of Physician Assistants has found evidence of coconut’s oil’s effectiveness in the fight against dementia and Alzheimer’s disease.
Akin to olive oil, coconut oil is known for it’s rich polyphenol content. The same study credits unique phenols in coconut oil with neuro-protective abilities.
Leafy Greens
Dark, leafy green vegetables are among the best foods for us. No matter what, we should all be eating these veggies. But people who are at a high risk for dementia or Alzheimer’s should definitely be loading up on these. According to findings from the Journal of Nutritional Health and Aging, increasing your consumption of leafy greens will decrease the risk of Alzheimer’s and dementia—and they’re just plain good for you!
The best leafy greens are spinach, kale, and romaine. They are loaded with brain-boosting antioxidants and vitamin K, both of which act as brain shields when it comes to warding off age-related cognitive decline. It’s important to note that if you’re taking blood thinners, you should consult with a doctor before loading up on too much vitamin K.
Cruciferous Vegetables
Just like leafy greens, we should all be eating these veggies on a regular basis. They are just as important as leafy greens because like kale and spinach, broccoli, cauliflower and Brussel sprouts are all high in vitamin K. Chatelaine also notes that they are high in glucosinolates which have an antioxidant effect, as well as folate and carotenoids that lower homo-cysteine and fight cognitive impairment, says MindBodyGreen. The source recommends eating at least 1/2 cup every week.
Other vegetables that are important to eat when it comes to improving brain health are pumpkin, squash, asparagus, tomatoes, carrots and beets. MindBodyGreen says when these foods aren’t overcooked they contain lots of vitamin A, folate and iron which can help with cognition.
Beans and Legumes
Foods like beans, chickpeas, and lentils are all good for us, specifically our brain health because they are loaded with antioxidants, fiber, vitamins, and minerals. MindBodyGreen writes, “these foods contain more folate, iron, magnesium and potassium that can help with general body function and neuron firing.” The source also states that they contain choline, which is a B vitamin that boosts acetylcholine (a neuro transmitter critical for brain function).
We suggest swapping out red meat for 1/2 up of beans or legumes at least twice a week.
Nuts and Seeds
Nuts are one of those foods that can be really healthy for us if we eat them properly. Plus they make for a really easy go-to snack! Our first rule is that they need to be unsalted. The other golden rule with nuts and seeds is that they are to be enjoyed in moderation because they contain lots of healthy fats.
Chatelaine says walnuts are among the best nuts because they are high in “omega-3 fatty acid, a brain-protective nutrient” which also makes them great for fighting off Alzheimer’s disease. The source also suggests eating only 1/4 cup or two tablespoons of a nut butter daily.
Chicken
Unless you’re a vegetarian, you probably already eat chicken quite frequently throughout the week. Thankfully, it’s a great option and should be easily substituted for red or processed meat whenever possible. However, we suggest only eating one serving a day.
Of course, it’s important to note that we’re not talking about fried chicken or flash-frozen chicken like the boxed version you probably purchased at the grocery store. We’re talking about a nice lean, grilled piece of chicken.
Whole Grains
Whole grains play an important role in the “MIND” diet. “Choose fibre-rich whole grains like oats, brown rice, and whole-grain wheat to offset your intake of refined grains,” writes Chatelaine.
Olive Oil
Olive oil isn’t a food or snack per se, but it’s a common ingredient used in the kitchen and should be preferred over other popular oils. You should be using it when cooking and can even try it as a salad dressing because unlike other unhealthy options, it contains monounsaturated fats, vitamin E, and antioxidants. WebMD points out that olive oil has “been shown to improve brain function over the long term and protect against dementia.”
Red Wine
You might be wondering what wine is doing on this list, but red wine has actually been shown to improve brain health and protect against Alzheimer’s! WebMD explains that several studies have shown this to be true, however in order for it to work, the wine must be enjoyed in moderation. Women should only drink one glass a day and in the case of men, it can be up to two. It’s important to note, that if you drink too much red wine it could have the opposite affect and make you more likely to get dementia, says the source.
We hope you found this blog post both interesting and insightful as you care for your senior or memory challenged loved one. If you provide assisted living services to a loved one in or around the Bethlehem area, or if you provide memory care services to a loved one, please know that you are not alone in your support challenges. We’re here for you, anytime! Why not give us a call!
6 January 2020

Well, the new year is upon us. It’s early January and from experience, we here at Bethlehem’s Gateway Gardens Assisted Living and Memory Care know that many of you purposely (and understandably) chose to ignore the notion that your senior loved one is now fully dependent. That is something so many of us simply do not want to address during the Holidays. But now you feel you can no longer prolong the fact that you must prepare for a monumental life change, for everyone involved.
When a senior’s health begins to decline, an adult child or other loved one may take on a few tasks to help. Aiding with chores like grocery shopping and mowing the lawn can allow the older adult to remain in their home. As the senior’s needs worsen, loved ones often take on more responsibilities.
For some families, however, it is a crisis of some kind that causes them to assume the role of family caregiver. The senior might have experienced a fall or been diagnosed with a chronic illness. In these situations, a caregiver may find themselves struggling to juggle all their loved one’s needs. It can be an overwhelming transition for people to make.
If you are in this situation, we have some suggestions to help new family caregivers like you manage the role.
5 Tips for New Caregivers
Our Final Suggestion
Our final suggestion is to become acquainted with us before you need us. We understand what you’re going through and can help you. We want to develop a trust and understanding and when the time comes, we hope that you’ll team with us for your professional senior assisted living support services. Together, we’ll provide the best loving care possible.
Give us a call. Let’s talk.
23 December 2019

Christmas and Chanukah share a similar spiritual message: that it is possible to bring light and hope into the world. These two holidays occur together this year, which makes this an even more special holiday season.
This is a season to reflect upon how fortunate we are to have you as our customers: our friends and neighbors. During these holidays, we wish you, your family, and your friends a safe, joy-filled, and relaxing season.
Warm wishes for a Happy Hanukkah, a Merry Christmas, and a most Happy New Year! With peace, joy, and love this holiday season and beyond!
9 December 2019

Well, Thanksgiving has come and gone, and we are smack in the middle of the Christmas/Holiday season. Your loved one who’s now living with dementia or the multiple challenges of senior life have always been the cornerstone of family Holidays and traditions. The challenges increase for all caregivers to continue the tradition with each new passing Holiday season. So, your friends, memory care professionals , assisted living professionals, and respite care professionals here in Bethlehem are back to offer you all some advice as once again you negotiate the Holiday season as a primary care giver.
Shop from home. Shopping, while oftentimes a large part of the season, will most likely bring undue stress to both the person living with dementia and the family caregiver. Avoid the sensory overload, large crowds, and confusing environment by shopping online or through a catalogue with your loved one. They can still choose gifts for the family but will be able to do so in the comfort and safety of their own home.
Create a new take on old traditions. Holiday family outings, such as outdoor ice-skating, caroling, or seeing “The Nutcracker” at a local playhouse, hold fond memories — but may not be feasible in the wake of dementia. Revamp these holiday traditions by taking a snowy day walk, lighting a fire and listening to Christmas music, or finding a version of “The Nutcracker” on DVD for family movie night. Time spent with family is the most important thing during holidays — the ice-skating, caroling and theatre are simply activities.
Remember a few of your favorite things. While it may seem like this year is going to be different than all the rest, it’s important (for both the caregiver and the person with dementia) to reminisce holidays past. Take the time during a holiday family get-together to share photos from previous celebrations, to recall funny family bloopers, and to engage in activities that your loved one is still able to — like decorating the Christmas tree or helping bake holiday treats.
As you’re adjusting to how things will be this holiday season (and those to come) — instead of how things once were — it’s important to remember the good and to hold onto joyful past memories in the wake of holiday stress. Focusing on the positive, rather than becoming overwhelmed by the negative, will not only help you cope and celebrate, but also encourage your loved one to enjoy such a special time, and to be at peace.
For those of you selflessly exercising the labor of love caring for you memory challenged or physically challenged loved ones, all of us at Gateway Gardens Assisted Living & Memory Care in Bethlehem hold you in the highest regard. We wish you and your entire family warmth and peace throughout this holiday season and going forward into 2020.
18 November 2019

By now I think all of you realize that here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care, we invest in managing this blog as a service to our cherished residents, their families, and to the countless angels out there who lovingly provide self-help at-home senior care services. We feel a heartfelt responsibility to freely share our professional knowledge regarding professional assisted living, professional memory care support, and or respite care services. We are fully aware of the vast weight of the labor of love that all of you bear regardless of the level of professional support that you currently secure.
While this Thanksgiving-related blog post is heavily focused on those of you who care for a loved one with memory care issues, so much of this messaging can be directly applicable to those providing senior assisted living support to someone without memory issues.
Thanksgiving is a time for family and friends to gather to give thanks, catch up and share a special meal together. However, when a family member is diagnosed with a dementia, such as Alzheimer’s disease, the family dynamic changes dramatically. Nowhere is this more evident than at holiday gatherings. The hustle and bustle of a typical family Thanksgiving can cause extreme levels of anxiety for someone with dementia, turning a wonderful day into a confusing and agonizing ordeal. Consequently, for the family caregiver, it can become a day full of tension as they watch over their loved one with anxious eyes.
It doesn’t have to be that way. With advance planning and preparation, Thanksgiving can still be enjoyed by everyone, even the family member with dementia. To be successful, however, you do need to plan and structure the day for the best possible outcome.
Here are some tips we’ve gathered, contributed by individuals with dementia, families and caregivers:
If your loved one is one of our cherished memory care residents here at Gateway Gardens, consider bringing some of your Thanksgiving cheer to them, rather than disrupting their routine by transporting them to your gathering.
For more information about senior living or memory care services here in Bethlehem, contact us anytime.
13 November 2019

Today’s blog post is a tribute to our staff who work so hard each day to create the safe, clean, and genuinely attractive living environment that every resident deserves. We invite the followers of our blog to take a walk through our gallery page and see with your own eyes the physical layout of our warm and friendly community. We think you’ll be impressed, and we gladly welcome the opportunity to show it off to you personally.
For those of you who don’t know us well, we specialize in assisted living, memory care, and respite care services to the greater Bethlehem, Ga area and beyond. We freely welcome the opportunity to engage you and your questions regarding the nature and considerations of assisted living, memory care, and respite care services. To do that, contact Gateway Gardens Assisted Living & Memory Care here in Bethlehem.
6 November 2019

Today’s blog post is designed to help those of you out there trying to decide the strategic care plan for a loved one suffering from the early stages of Alzheimer’s or other dementia-related disease. It is very common for all of you care providers to be confused regarding exactly what type of professional care is best now, assisted living or memory care. We are proud to inform that we lovingly provide both services here at Manor Lake Assisted Living & Memory Care here in Bethlehem. We thought we’d share the following with you while crediting dementiacarecentral.com for insightful and informative narrative on this subject.
Even with help from community-based services and respite services, providing care for a loved one with Alzheimer’s disease (A/D) or dementia becomes more difficult with time. In later stages of the disease, many people will require more care and assistance than their family members can provide. Even for people who don’t need intensive hands-on care, safety may be an issue and they may not be able to stay home alone. Residential care options may be able to provide best for the needs of some individuals. However, these options are often considerations that caregivers and their families find difficult to plan for, or to even discuss.
Residential Care Options for Dementia
The natural progression of Alzheimer’s Disease, as well as other forms of dementia, will result in the need for care for loved ones. Depending on one’s stage of Alzheimer’s/dementia, and his/her ability to function, the level of care and supervision that is required varies. For most families, this means some form of residential care. This is where assisted living, “memory care” comes into play.
Assisted Living Communities
Assisted living residences, such as continuing care retirement communities, are especially suited for those individuals in the earlier stages of Alzheimer’s disease and dementia who do not have many medical problems, but who do need more intensive support for Instrumental Activities of Daily Living (IADLs). Many people with dementia will need help with IADLs. These are activities that we perform from day to day that add to our quality of life, but are not as basic to self-care as Activities of Daily Living (ADLs). ADLs are the basic activities that we must perform every day in order to take care of ourselves. Individuals with dementia may also need help with these tasks.
The following tasks are considered to be IADLs:
Typically, ADLs refers to the following tasks:
Those who are in the middle-stage of dementia require a greater amount of supervision and care than those in early-stage dementia, and for those in middle-stage dementia, assisted living is also a good option. In assisted living facilities, individuals generally live in a private studio, private apartment, or a shared apartment, and have staff available to assist them 24-hours / day. This type of living arrangement is ideal for those who are still able to live with some independence but do require assistance with ADLs. Transportation to and from doctor’s appointments and social activities are also offered at assisted living facilities. In addition, assisted living facilities have dining halls where residents gather to eat meals.
Memory Care
For individuals with dementia who require a higher level of skilled care and supervision, memory care units are an ideal option. These units offer both private and shared living spaces. Sometimes they exist as a wing within an assisted living facility or nursing home or they sometimes operate as stand-alone residences. Supervised care is provided twenty-four hours / day by staff trained to care for the specific needs and demands of dementia patients. Memory care units offer the same services as assisted living facilities, in addition to activities that are intended to stimulate the memory of those with Alzheimer’s and other dementias, and possibly slow the progression of the disease. Activities may involve music, arts and crafts, games, and more.
For more information, contact Gateway Gardens Assisted Living & Memory Care here in Bethlehem.
Source: dementiacarecentral.com
28 October 2019

We take great pride here at Gateway Gardens Assisted Living and Memory Care here in Bethlehem to share our knowledge and stories to help as many people as possible. For those of you struggling to care for loved ones in need of memory care support, we understand your challenges and the huge labor of love that you bear.
Today we’ll share with you the most common symptoms shared by Alzheimer’s and related dementia disorders. The symptoms include any combination of the following:
Helping People with Alzheimer’s Disease
Although there is no cure for Alzheimer’s disease, there are things you can do to slow its onset and to maximize your loved one’s quality of life. The ability to deliver positive effect is especially enhanced if the disease is still in its early stages.
While you may be able to care for an Alzheimer’s patient in the early stages of the disease, you need to realize that the challenges will become increasingly difficult. Your loved one can present a danger to themselves by wandering off or forgetting to turn off the stove. If this is the case it may be time to consider professional memory care services like those we provide here at our Gateway Gardens Assisted Living and Memory Care community. For more information about memory care services here in Bethlehem, contact us anytime.
21 October 2019

Many people who are in need of assisted living services in and around Bethlehem or memory care services in and around Bethlehem put off looking for care for fear of how they will pay for it. We are fully committed to providing the highest quality and most affordable assisted living services across the Bethlehem Georgia area. We fully realize that assisted living services, for some, can be cost prohibitive. However, we are fully committed to assisting you with potential sources of financial aid so that you and or your loved ones can secure the care that you deserve.
Check the Veteran’s Aid & Attendance Program
Check eligibility for the Veteran’s Aid & Attendance Pension, a program which can provide financial help to those who require assistance with activities of daily living such as eating, bathing, dressing and undressing or taking care of the needs of nature.
It can pay up to $1,830 per month to a veteran, $1,176 per month to a surviving spouse, or $2,170 per month to a couple for veterans and surviving spouses (as of 2017). Certain income and asset limits also apply.
This program allows you to keep more assets than most state aid programs, and it provides a higher level of assistance. You cannot receive benefits from both the Veterans program and a state aid program, so you may want to evaluate both to determine which provides the highest level of assistance for you or your loved one.
Check with your state’s medicaid office
Find your state Medicaid office and check on their available resources. To qualify for Medicaid you'll need to have assets and income that are below the federal poverty levels.
Many state programs offer assistance with assisted living costs for those who have no financial resources. Qualifying for such assistance usually means you have less than $2,000 in assets, although exact program requirements can vary from state-to-state.
Find non-profit resources for assisted living and elderly care
With a little digging you may find a non-profit organization that can help. If they can't help they may direct you to additional sources of assistance. Start with these two organizations:
Ask for family support
One home health company has created a free personalized way to stay in touch with those who need in-home care or assisted living through a feature they call CareTogether. It functions like a customized form of Facebook designed just for a senior who needs care, allowing the family to stay updated on what their needs may be.
You could use a feature like this, or a Facebook page, to explain your or your loved one’s needs to extended family and then ask family members if they would be willing to contribute a small monthly amount to provide in-home or assisted living care for this family member.
We want you to know that we are here to help. Contact Gateway Gardens Assisted Living and Memory Care in Bethlehem today.
Source: thebalance.com
18 October 2019

We’re establishing a tradition here at Gateway Gardens Assisted Living & Memory Care here in Bethlehem to celebrate Halloween with our assisted living residents as well as our memory care residents. Each year we research new and exciting ideas to smile, laugh, and share our love for our treasured residents. This year we found this article from SeniorAdvisor.com with a laundry list of ideas which we are not mulling over. We thought we’d share the same ideas we the followers of our blog in the hope that it navigates all of you to some special moments during Halloween.
Halloween Crafts for Seniors
Halloween crafts can be completed early in October so you can use them as decorations throughout the rest of the month.
(Mostly) Healthy Halloween Recipes for Seniors
You can find loads of cute Halloween recipes on the web, but most of them are laden with sugar. Since many seniors have health concerns, we tried to pick out a few of the healthier options that still fit the theme.
Other Halloween Activities for Seniors
If you want to pack Halloween week with more fun, interactive activities that you might consider include:
Halloween’s not for everybody, so you’ll probably have those uninterested in participating in some of these activities, but those that enjoy the season will be happy to have the opportunity to celebrate it in a variety of ways.
All of us here at Bethlehem’s Gateway Gardens Assisted Living & Memory Care wish you the very best for a joyful Halloween celebration.
14 October 2019

Caring for your loved ones that require significant assisted living support here in Bethlehem or memory care support here in Bethlehem is an exhaustive yet fulfilling labor of love. Without doubt it is very stressful as well. At some point this labor of love becomes an unhealthy tax on both the mental and physical state of the caregiver(s). It is at this point where guilt sets in when we recognize our inability to keep pace with the ever-increasing challenge of providing assisted living care support services. This guilt is natural but fortunately it is usually short-lived once we come to accept the realities of life that, at some point, we must turn to assisted living professionals to help us carry the load.
The key word there is “professionals”. We are programmed to believe that no one outside the family can provide the same level of loving care that a family member can. But that is simply not true. When you enlist the support of assisted living or memory care professionals in and around Bethlehem you are empowering you and your family with the power of scientific research and professional expertise that will enhance the quality of life of your loved one in ways that the non-professional family simply cannot. No offense of course.
So take the step to research your transition to professional assisted living care with confidence (not guilt) that you are about to increase the quality of life of both your loved one AND yourself. Conduct thorough research of the assisted living and memory care communities near you to experience the campus, assess the skill and attentive nature of the staff, and to simply get a feel for the memory care community as a whole. Trust your instinct, it will guide you well.
If you think it's time to move your parent or loved one to an assisted living care community, contact the assisted living and memory care professionals at Gateway Gardens here in Bethlehem. Our team is available to help guide you through this difficult process and answer any questions that may arise.
11 October 2019
According to the Center for Disease Control and Prevention, seniors supported by professional assisted living professionals realize a statistically significant decrease in hospitalization for heart disease. This positive report is attributed to the professional support provided by assisted living and memory care communities such as ours at Gateway Gardens Assisted Living & Memory Care here in Bethlehem GA that deliver quality of life support programs as well as regular and reassuring professional health consultation.
What We Do?
The following items are primary goals of our assisted living and memory care community and our memory care community in an effort to reduce the rate of senior patients developing heart illnesses.
Provide Fitness and Relaxation
Keeping seniors active and relaxed improves heart health. Workout programs that range from low to moderate impact exercises are managed based on fitness levels and health status. Regular exercise helps lower stress levels and improve quality of sleep. When these two vital factors are achieved and stabilized, a healthier heart is guaranteed.
Promote Nutrition and Healthy Diet
Assisted living communities pay close attention to the nutrition and diet of their senior residents. They make sure that the food served to senior residents are both appetizing and healthy to improve food intake and facilitates consumption of important nutrients that can strengthen the heart. Also, taking note of food that must be taken moderately. Low-salt, low-fat, low-sugar diet are usually the dietary recommendation for these people.
Provide Smoke-Free Environment
We know for a fact that a smoker has a higher risk of developing chronic heart disorders including atherosclerosis and coronary heart disease. Gateway Gardens Assisted Living & Memory Care offers a designated outdoor area for smokers separated from non-smokers so that non-smokers will not be exposed to smoke-filled air. This is also a way to encourage current smokers to break the habit. Medical advises are also given to those smokers to support them to give up smoking.
For more information about assisted living and memory care services in and around Bethlehem, contact Gateway Gardens today.
7 October 2019

Modern researchers have discovered that music soothes those suffering from advanced age, dementia, and/or Alzheimer’s disease.
Researchers at The University of Utah Health recently tested whether they could alleviate anxiety in seniors (with and without dementia) by playing familiar music to them using headphones and a hand-held music device. Anxiety and agitation are two of the most disruptive aspects of living with dementia and Alzheimer’s disease for both patients and caregivers.
After the researchers helped the patients pick meaningful music, they used a functional MRI to record the changes in the brain while the music played. The brain images showed that music helped the areas of the brain known as the salience network, the visual network, the executive network, and the cerebellar and corticocerebellar networks all work with better connectivity. These areas of the brain activate language and memory, according to the study’s authors.
“When you put headphones on dementia patients and play familiar music, they come alive,” Jace King, lead author of the study, said in a press release. “Music is like an anchor grounding the patient back in reality.”
Music and movement are the last things to go in the brain.
It’s almost miraculous what music can do for Alzheimer’s patients and the research about the benefits is there.
Patients Respond
Health care providers have seen firsthand how much music helps dementia patients. with the clients there.
Play songs from their era that they might recognize. Patriotic songs are also popular.
Music touches people on so many levels.
The reaction by dementia patients to music was also dramatically demonstrated in the 2014 documentary, Alive Inside. Elderly care professionals can set up personalized playlists on iPods for their patients. The music helps the patients access the deep memories not lost to dementia. It also helps them converse and socialize in ways they weren’t doing before the familiar music became a part of their daily life.
For more information regarding senior assisted living services or memory care services in Bethlehem, contact Gateway Gardens today.
4 October 2019

When it comes time to begin the most difficult task of choosing a Bethlehem-area senior living or memory care community take a deep breath and accept the fact that you are about to take on very serious responsibility. We want to help you in that endeavor by offering some guidance on how to move forward. Please know that we are here for you to help and expand upon the following advice.
At the very core of best practices to find the perfect senior living or assisted living community in Bethlehem is to speak with as many staff members and current residents as possible.
Questions to ask
Obviously, you can't just rely on facility tours or promotional brochures to make this crucial decision. First, get your ducks in a row. When you're ready to visit in person, turn to administrators, staff members and residents for answers to pivotal questions.
Consider Before You Visit:
Is the location realistic? Lengthy drives, not to mention flights, will affect visits and add barriers to relationships with friends and family members, including spouses still living at home.
Many families face a tough conundrum. Sometimes it's a matter of choosing between top-ranked but distant facilities versus more accessible locations for loved ones to visit regularly and monitor care.
Ask Administrators and Nursing Directors:
What are the staffing ratios? Bolster your question with research.
What is your staff turnover? Stable staffing is a good sign. In addition, consistent assignment – when the same caregivers are assigned to the same residents on a daily basis – is critically important. That way, staff members really get to know residents, anticipate their needs and can recognize and address problems early.
Which services do you offer? If you're undergoing rehab to recover from a hip fracture, you'll need a higher level of care than some nursing homes can offer. With medical conditions like chronic obstructive pulmonary disease, or COPD, residents may need help managing supplemental oxygen.
Do you provide special care for people with dementia? Memory care means much more than just a locked unit to prevent residents from wandering. Staffing ratios should be no more than five residents per caregiver, including nurses and aides, around the clock. Caregivers should have special training in dementia care, and the awareness and sensitivity to best address these needs.
Ask Dietitians:
What kind of food do you serve? Residents rely entirely on nursing homes to meet their nutritional needs. Healthy, tasty food improves everyone's quality of life.
How do you satisfy cultural and individual food preferences? People in nursing homes still want to enjoy meals that evoke family traditions and tastes they've developed over their lives.
Do you accommodate special diets? Residents come in with their own dietary preferences and restrictions. Some also may have medical orders for soft or puréed diets, for example.
Can residents eat when they want? Some people prefer to eat outside routine schedules.
Ask Residents:
After the formal tour, explain that you'd like a chance to speak with several residents. Drop in at the activities room or a lounge, introduce yourself, say you're considering a move there and ask what it's like for them.
Are you happy here? "Do you enjoy living here?" "What do you like best about living here?" and "If you could change one thing, what would that be?" are positive ways to frame your questions and make residents more likely to respond.
Do you have freedom of choice? Does the facility offer resident-centered care? Are you able to get up when you want? Do you go to bed at the time you want?
When you ask for help, how long do you have to wait? If you always have to wait beyond five minutes for help, you're likely to try doing things on your own, which could set you up for falls.
Ask Activity Directors:
What about activities? How do you keep residents engaged? Ask to see monthly activity calendars. Offerings should be varied and appealing.
Does the facility have a resident or family council? These self-determined groups can provide a strong voice for quality care.
Is reliable transportation available? Sometimes nursing homes only provide transportation for certain medical appointments – and they don't provide transportation for social purposes. Is there staff to help residents get to a granddaughter's play?
Can residents easily spend time outdoors? Attractive courtyards are sometimes the first thing visitors notice. But how often can residents, particularly those with mobility issues, actually go outdoors? Does staff encourage and help them to do so?
For more information on senior assisted living services here in Bethlehem or memory care services here in Bethlehem, contact Gateway Gardens anytime!
© 2026 Gateway Gardens at Bethlehem
Web/Marketing Solution Developed and Maintained by WSI Pro Marketing.